Abstract
Abstract
Pediatric oncology patients often experience fatigue and physical and mental deconditioning during and following chemotherapy treatments, contributing to diminished quality of life. Patient empowerment is a core principle of patient-centered care and reflects one's ability to positively affect his or her own health behavior and health status. Empowerment interventions may enhance patients' internal locus of control, resilience, coping skills, and self-management of symptoms related to disease and therapy. Clinical and technological advancements in therapeutic videogames and mobile medical applications (mobile health) can facilitate delivery of the empowerment interventions for medical purposes. This review summarizes clinical strategies for empowering pediatric cancer patients, as well as their relationship with developing a “fighting spirit” in physical and mental health. To better understand physiological aspects of empowerment and to elucidate videogame-based intervention strategies, brain neuronal circuits and neurotransmitters during stress, fear, and resilience are also discussed. Neuroimaging studies point to the role of the reward system pathways in resilience and empowerment in patients. Taken together, videogames and mobile health applications open translational research opportunities to develop and deliver empowerment interventions to pediatric cancer patients and also to those with other chronic diseases.
Introduction
E
Empowerment Interventions in Pediatric Oncology
Although childhood cancer-directed medical interventions have been extensively studied, children's psychological experiences and quality of life (QOL) associated with childhood cancer have received comparatively limited attention. Research aimed at understanding and improving psychosocial outcome of children with cancer and their families is essential. Children diagnosed with cancer are significantly more likely to experience compromised mental health and QOL compared with siblings and peers. 8 Omnipresent patient and parent stresses include prolonged hospitalization, altered body image and sense of vitality, and fear of death. Treatment usually involves surgery, chemotherapy, and radiation therapy and is oftentimes arduous, invasive, and lengthy. Related stress experiences involve the actual event, the child's making sense of the event, the search for coping strategies, both behavioral and cognitive, and finally implementation of these strategies.9,10 Adolescent cancer patients may feel a sense of inadequacy, loss of control, and frustration, resulting in compliance issues. 11
Optimal adjustment to such uncontrollable stressors often requires adjusting oneself to the stressors rather than one being able to change the stressors (i.e., adjusting one's perceptions and reactions to a situation when one cannot alter the situation). Children with a wide range of coping strategies feel more in control and thus experience less anxiety than those with a narrow range of coping strategies.8,12,13 Current strategies addressing these comorbidities include counseling, physical therapy, and pharmacological therapies, alone or in combination.14–19 A key feature shared by all of these approaches is that they are externally administered to the individual.
A complementary approach to addressing patient depression, fear, generalized deconditioning, and fatigue involves the concept of empowerment—an enhanced mental ability to understand and positively influence one's own health status by patient engagement in his or her health management.1–6 As illustrated in Figure 1, empowerment can be defined in clinical terms as a process that accelerates and enhances improvements of both mental and physical health. Current empowerment-centered interventions include printed documents, conferences for cancer survivors, cancer camps, group sessions, and exercise programs (Table 1). Addressing patient and parental concerns with one-on-one education regarding diagnosis, treatment plan, and potential side effects, as well as providing emotional and social support directed at increasing confidence, can reduce anxiety and help patients feel in control of their health situation.14–16 Beneficial results of empowerment-centered interventions have already been demonstrated in patients with diabetes and attention deficit hyperactivity disorder.26–29
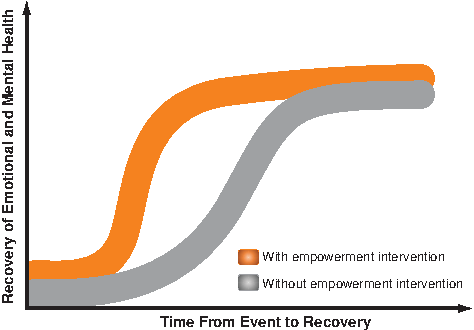
Empowerment accelerated improvements in physical and mental health of a patient, as shown by two possible recovery trajectories. Effectiveness of patient empowerment can be monitored by time dependence of health-related quality of life metric tools. (Color graphics available at www.liebertonline.com/g4h)
It is interesting that although interventions directed at increasing patient empowerment in diverse healthcare settings are becoming more prevalent, designing meaningful metric tools to specifically assess intervention efficacy remains challenging. Such interventions were initially developed for use in mental health populations and more recently expanded to assess other patient populations, including those with diabetes, cancer, and other chronic diseases, as described in Table 2. Although some of these studies have used validated tools, other studies have used simple, brief, nonvalidated questionnaires aimed at determining intervention efficacy.
CEQ, Cancer Empowerment Questionnaire; HCEQ, Health Care Empowerment Questionnaire; heiQ, Health Education Impact Questionnaire' SCM, Shared Care Model.
Advances in Videogame Technology and Mobile Health Applications
With the advent of computers and multimedia, attention has been drawn to alternative sources of education and empowerment. Computer-based interventions in the form of compact disk read-only memory, Web/Internet-based interventions, and videogames, as detailed in Table 3, are increasingly being studied. These patient-centered, interactive modalities have a greater appeal to children and adults.42–49
Designing interactive videogames specifically for pediatric oncology patients is an exciting area of interest. A study involving virtual reality computer games on depressive symptoms in Hong Kong Chinese hospitalized children with cancer was recently conducted. Patients in the study group, which included videogame play therapy, had statistically significant fewer depressive symptom than those in the control group. 50 “Re-Mission™” is a sedentary interactive videogame created to change behavior and improve treatment medication adherence of children and young adults diagnosed with acute lymphoblastic leukemia.35,51 In a multicenter randomized control trial involving 375 patients 13–29 years of age, patients whose treatment included playing “Re-Mission” as well as standard therapy (treatment group) showed a statistically significant improvement in adherence to prescribed medication regimens compared with patients treated with standard therapy alone, despite suboptimal use of the intervention by most participants. 35 Playing “Re-Mission” also resulted in a significantly greater increase in cancer-related knowledge when compared with the control group, likely resulting from information integrated within the game or information-seeking behavior from the videogame therapy. 51 These studies provide important evidence that a judiciously designed videogame can enhance certain behavioral outcomes, potentially promote information seeking, and increase knowledge in adolescents and young adults with cancer.
Adapting existing commercially available videogames, including “Dance Dance Revolution” (Konami Digital Entertainment, El Segundo, CA), “Wii™ Bowling” and “Wii Boxing” (Nintendo, Kyoto, Japan), and “Circus Challenge” (Limbs Alive, Newcastle upon Tyne, United Kingdom), to promote physical exercise and weight loss and to improve neurologic function, has also become an important therapeutic approach.52–57 However, videogames specifically designed for particular population with a specific therapeutic goal are sparse and generally sedentary in nature.
The progression of videogames and mobile applications (apps) designed specifically for therapeutic benefit has focused on education and promotion of healthy life styles via diet, as well as fitness and exercise, in adults, and few are directed at children or specific diseases. However, one example of a child-focused game is “Zora,” a three-dimensional graphical virtual multiuser community designed for children undergoing chronic hemodialysis in the hospital setting, provided a safe and novel means for coping and sharing experiences in the creation of a virtual city/community support network. 48 “Zora” was subsequently found to be feasible, safe, and beneficial as an Internet-based psychosocial intervention in the home setting for adolescents following solid organ transplantation. 49
In a study focusing on clinical depression, patients were randomized to either receive videogame therapy (treatment group) or no videogame therapy (control group). Using the Patient Health Questionnaire, patients in the treatment group showed a statistically significant reduction of depressive symptoms at 1 month. 58 The same research group recently reported that playing casual videogames as a prescribed medical treatment also help in reducing anxiety. 59
In another study, traditional face-to-face cognitive counseling therapy for depression was compared with a computerized cognitive behavior therapy (SPARX) over 7 months; a statistically significant improvement in depression rating was demonstrated in the SPARX cohort compared with the traditional treatment cohort. 60 Commercially available videogames used as distraction therapy have also resulted in decreased conditioned nausea.61,62 Finally, in a randomized controlled trial involving pediatric burn patients, the average procedural pain scores, measured using the Faces Scale, were significantly less in the group where playing a virtual reality game was used in addition to traditional analgesia. 47
Creating hope, improving QOL, increasing one's sense of control, and reducing stress are also important parts of patient empowerment, especially in pediatric oncology. With these concepts in mind, the prototype “Patient Empowerment Exercise Videogame” (the PE Game) was developed. 63 The PE Game is an interactive videogame specifically designed for pediatric oncology patients during their chemotherapy treatment. 63 This videogame couples physical exercise with patient empowerment through several minigames that visualize metaphors for fighting cancer and provide positive reinforcement via physical activity. The nonviolent themes encourage safe physical exercise while avoiding repetitive stress and violence for the patient, who assumes the role of a superhero overcoming diverse obstacles.63,64 Patient- empowering videogames, such as the PE Game, offer a personalized support and improvement of disease self-management for patients of all ages with diverse chronic conditions. 65
Mobile health (m-health) is a rapid expansion from the growing electronic healthcare practices. Between 2002 and 2012 approximately 117 articles were published on the impact of mobile phones and smartphones in health care. 66 With the expansion of smartphone systems and cellular network technologies, novel biomedical sensors and communication paths continue to advance, creating room for m-health development. 67 The use of these devices in low- and middle-income countries is also of interest for healthcare maintenance and telemedicine. 68 Some smartphone applications promote healthier lifestyles and dietary choices, mental and behavioral health, obesity prevention, exercise monitoring, and blood glucose data analysis.69–71
The importance of mobile interventions is illustrated by development of “Re-Mission 2,” a mobile online game of Re-Mission, that promotes empowerment, self-efficacy and positive emotions, while also motivating pediatric and adolescent cancer patients to medication adherence. Another example is the U.S. Food and Drug Administration–approved BlueStar® (WellDoc, Baltimore, MD) mobile platform used for behavioral self-management in diabetic patients.72,73 For empowerment interventions, there are already available mobile apps for stress and anxiety management, including gamified mobile apps specifically focused on cognitive training or biofeedback-coupled music apps.74–76 Given increasing popularity of biofeedback-based wearables, mobile apps can bridge virtual and real worlds to empower patients.59,77 With clinical development and validation, therapeutic videogames and m-health have great promise of becoming personalized medicine tools in health care. 78
Neurological Mechanisms in Emotional Homeostasis
Emotional homeostasis and empowerment are intrinsically interconnected within an individual's neurobiology (Fig. 3). An intact reward system is central for preserving optimism and hope, qualities identified in empowered individuals, when confronted with adversity in everyday life, whether mild or extreme. 79 Two behavioral systems integral in normal human behavior include one motivating the pursuit of potential rewards and one motivating avoidance of potential losses. 79 The neural circuitries of stress, fear, and the mesolimbic dopamine pathway, also known as the reward system, are overlapping and interrelated in adaptive responses to fear and stress and in building resilience and empowerment.80–85 The predominant neurotransmitter of the reward system is dopamine, sometimes referred to as the pleasure chemical of the brain. Common brain regions with reciprocal interconnections include the hypothalamus, hippocampus, amygdala, prefrontal cortex, orbital frontal cortex, nucleus accumbens, the hippocampus, and the amygdala.86,87 The hippocampus and amygdala are central in emotional memory encoding and consolidation and in generating and regulating emotional reactions in response to stress, regulated in part by cortisol.86–89
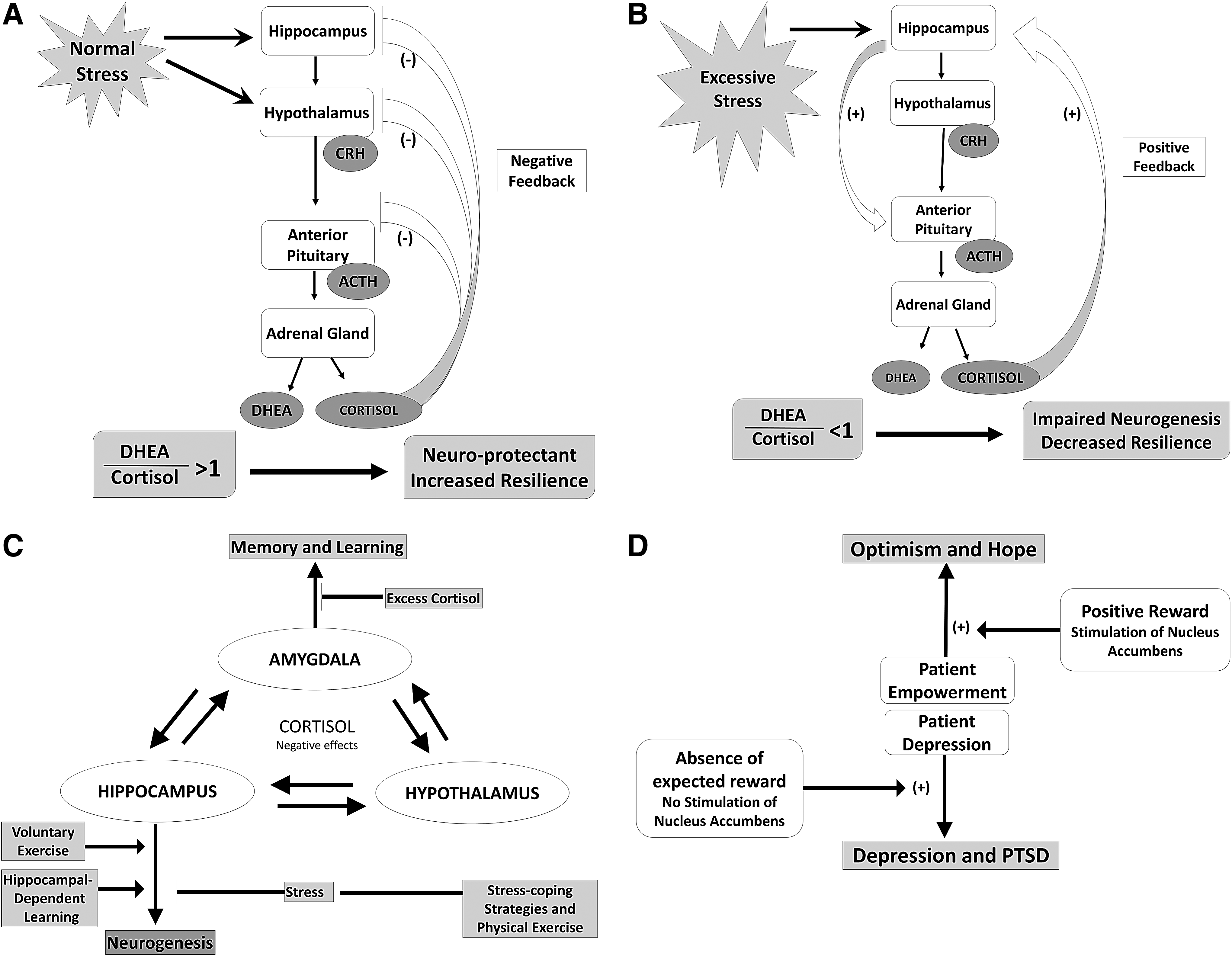
Overview of relationships among brain structures, hormone feedback systems, and psychosocial conditions following stress exposure.
The medial prefrontal cortex and the orbital frontal cortex are central in reward learning and guiding future behavior based on anticipated rewards or punishments.90–92 The orbital frontal cortex receives direct input from the taste, olfactory, visual, and somatosensory areas and is involved in integration of multiple stimuli and value assessment of stimuli.90,91 The medial prefrontal cortex is associated with visceral function in relation to emotion. 93 Lesions in these areas result in an inability to make reward-based decisions and to distinguish rewards from punishments. The inability to predict future rewards has been implicated in depression because it is thought to result in a hopeless and pessimistic outlook. 91 Decreased dopamine signaling, with resultant diminished striatal activation, has been documented in and associated with symptomatic depression and posttraumatic stress disorder in patients.79,81,82
Hormones important in maintaining emotional homeostasis in times of fear and stress include (1) corticotrophin-releasing hormone, which is anxiogenic when stimulating corticotrophin-releasing hormone 1 receptors but anxiolytic when stimulating corticotrophin-releasing hormone 2 receptors, (2) cortisol, which is important in restoration of homeostasis following stress, (3) neuropeptide Y, which is endogenously anxiolytic, and (4) dehydroepiandrosterone (DHEA), with neuroprotectant functions including promoting neurogenesis, establishing memory, and endorphin synthesis.84,88,89,94–97 The effect of neuropeptide Y as an endogenous anxiolytic has been compared with that of benzodiazepines.85,88,91,92 Neuropeptide Y, the level of which is known to increase with stress, was significantly increased from baseline following survival training, and chronic overexpression of neuropeptide Y has been associated with stress insensitivity. 88 Empowerment interventions that have the ability to stimulate the reward circuit while suppressing the fear, anxiety, and stress response could play a role in both treatment and prevention of depression and posttraumatic stress disorder in cancer survivors.80–84
Translational Research and Development of Empowerment Interventions
Understanding the effect that empowerment interventions have on neural systems facilitates the development of interventions that may alter the structure and functional brain changes associated with early life adversity. 85 Maintaining a properly functioning reward system when confronted with extreme adversity is crucial to preserving optimism and hope, both of which are qualities identified in empowered individuals. 79 Empowerment-promoting interventions targeting brain areas and circuitries described above, including interactive videogames designed to stimulate reward neural circuitry, have the potential to ameliorate the effects of chronic stress and improve resilience in patients with an increased risk of anxiety and depression, including those undergoing treatment for cancer.
One illustrative example is the above-described sedentary videogame “Re-Mission,” designed to improve disease self-knowledge and medicine compliance in teenagers with cancer. Functional magnetic resonance imaging (fMRI) was used to elucidate brain activity involved in active versus passive gameplay in healthy volunteer undergraduate students while they either played or observed someone else play “Re-Mission.” The fMRI results showed (1) active gameplay resulted in increased left parahippocampal cortex activation, (2) active gameplay, as opposed to passive observation, was necessary for activation of the mesolimbic reward system, and (3) there was a positive correlation between left parahippocampal activation and attitudes toward chemotherapy when assessed immediately following and then 1 month following gameplay.35,51,97
Because the hippocampus plays a role in emotional learning and memory consolidation, it is not surprising that they found a positive correlation between the degree of left parahippocampal activation and positive attitudes toward chemotherapy after playing the game and at the 1-month follow-up. Similarly, the role of enhanced reward system in building resilience has been shown in fMRI brain studies in Special Forces soldiers. 98 Finally, in patients with treatment-resistant depression, deep brain stimulation in the nucleus accumbens has been shown to improve symptoms of depression.81,83,99
Taken together, these data suggest that interventions directed at stimulating the complex reward circuitry and/or suppressing fear, anxiety, and stress responses can lead to improvements of core symptoms of depression. Interventions directed at decreasing the cortisol:DHEA ratio, by either decreasing cortisol or increasing DHEA levels, could promote resilience and serve as potential targets for therapeutic intervention, including carefully designed therapeutic videogames.84,99–101 Measurement of the cortisol:DHEA ratio could serve as a useful indicator of efficacy of such interventions. Such interventions could be exogenously administered pharmacologic compounds or disease-directed videogames specifically designed to stimulate and/or augment the reward neural circuitry, and thus decrease or prevent depression and stress disorders, and to promote empowerment in children and others with cancer.81–84,90,91 Of equal importance to understanding mechanisms of empowerment interventions are advancements in diagnostic tools that allow monitoring efficacy. There are new opportunities to correlate imaging and biomarkers with questionnaires assessing patient empowerment. Such questionnaires are being developed and validated for chronically ill patients.102,103
In addition to translational research, development of videogames as empowerment interventions may impact medical and regulatory practices. Both patients and healthcare providers will benefit from clinically validated games and apps that improve healthy habits, self-management, and QOL of chronically ill patients. “Re-Mission” and “Re-Mission 2” illustrate these benefits for pediatric oncology patients. Given that the U.S. Food and Drug Administration has been approving games and apps for medical uses (for example, BlueStar, the Jintronix [Montreal, QC, Canada] Rehabilitation System®, or MusicGlove® [Flint Rehabilitation Devices, Irvine, CA]), there are also new opportunities for pharmaceutical and biotech industries to integrate these digital technologies with specific drug-based treatments as innovative molecular–behavioral combination therapies. 104
Conclusions
Patient empowerment is a complex journey of personal change that results in gaining power over one's life. Traditionally, empowerment interventions have been externally administered, and efficacy of these interventions is determined largely by patient and provider feedback through the use of questionnaires. As therapeutic paradigms shift toward neurobiology-centered care, new interventions and outcome measures targeting specific neurocircuitry central to pleasure, reward, resilience, and empowerment can be developed, and efficacy can be measured using a combination of fMRI, neurochemical, and psychological tools.91,97–99,105 A well-designed videogame encompassing properties such as enhanced intrinsic motivation, active imagination, and attention to and engagement in intriguing “stories” focusing on a given health-related behavioral issue could actively capture one's full attention and thus promote health behavioral change. 106 Judiciously developed videogaming technology and mobile health are becoming valuable conduits of recruiting specific pathways and circuitry known to be involved in “positive” addiction into development of empowerment and resilience and promote optimal self-management. 107 Using technology to improve individual empowerment and resilience via strengthening stress and pleasure-sensitive neural processes and positive feedback of stress-buffering neurotransmitters is the next facet to developing empowerment in patients of diverse ages and disease processes.
Footnotes
Acknowledgments
C.S.B. and G.B. would like to thank the Department of Pediatrics for generous financial support of the PE Game project. The authors wish to acknowledge faculty and students from the Entertainment Arts and Engineering, Master Games Studio, University of Utah, for their respective roles in the design and development of the prototype Patient Empowerment Exercise Video Game, as well as students from the Lassonde Entrepreneurial program at the University of Utah for creating ![]() .
.
Author Disclosure Statement
G.B. and C.S.B. have a patent application pending for the Patient Empowerment Exercise videogame. G.B. and C.S.B. are scientific co-founders of Epicadence, Public Benefit Corporation, specialized in developing digital and mobile technologies as medical treatments. M.G., R.C.B., and M.L.G. declare no competing financial interests exist.
M.G., R.C.B., M.L.G., G.B., and C.S.B. all contributed to the literature review, interpretation of existing published information, and the technical writing of this manuscript. G.B. and C.S.B. contributed to the conception of this manuscript, as well as in the initial conception, design, and implementation of the PE Game.
