Abstract
Introduction:
Nasal reconstruction presents a formidable challenge to the surgeon. The unique 3D shape of the nose makes recreating the nasal pyramid a daunting task. Complicating the anatomy is the unpredictable nature of postoperative wound healing. Thus, accurate planning is essential to optimizing reconstructive outcomes. Existing techniques include using foil paper from suture packages to create a model of the defect on which to base the local or interpolated flap. 1 –3 However, these methods are limited in that they only create a 2D model of the defect and do not account for the 3D structure of the nose. Other methods of creating 3D nasal templates can be time-consuming, expensive, or require the use of custom imaging software. 4 –7 We present a technique that addresses these issues and accurately creates a 3D template of the nose.
Methods:
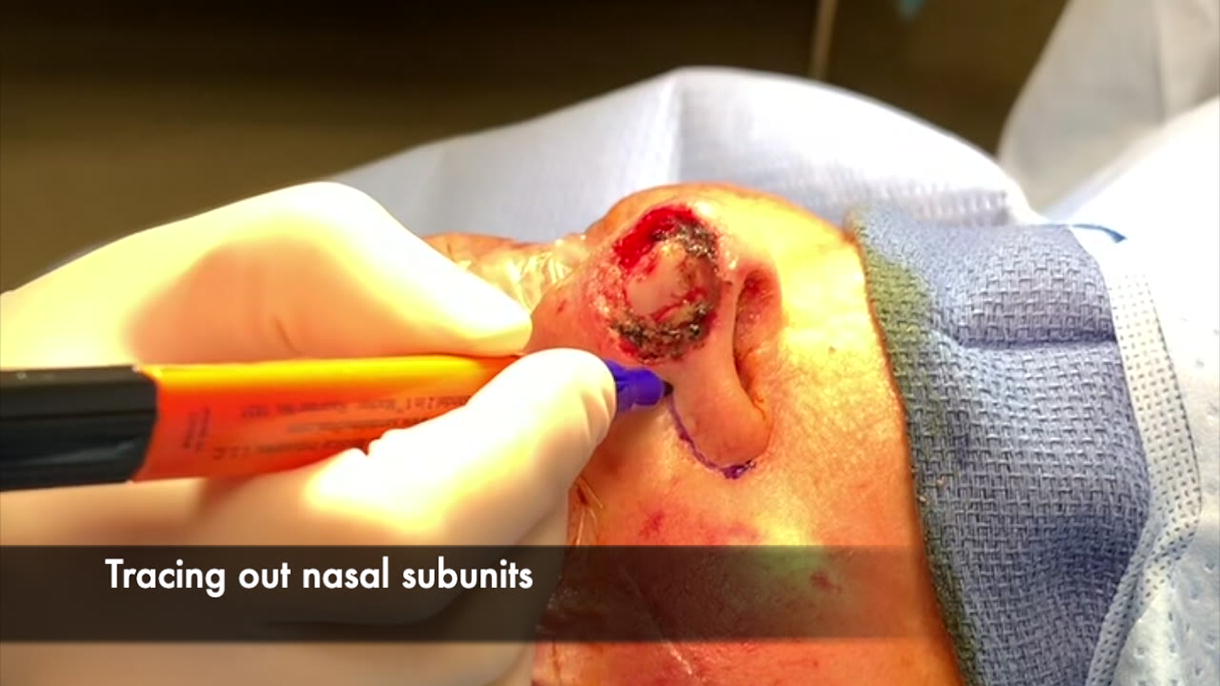
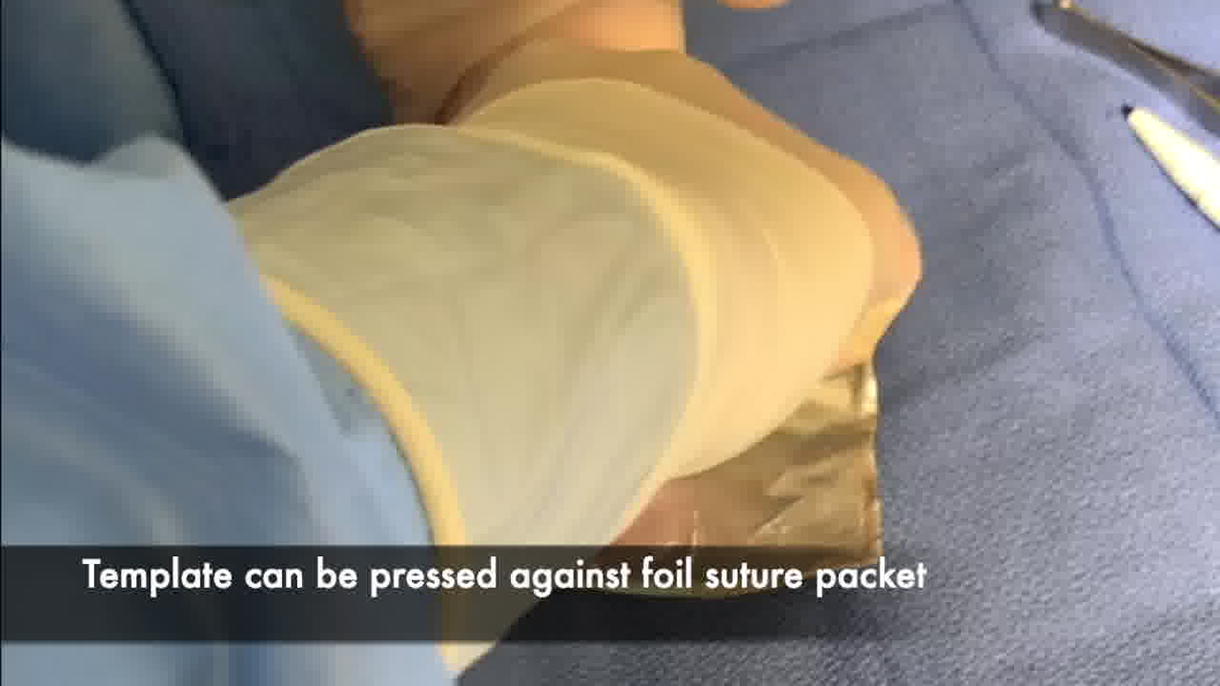
A marking pen is first used to outline the patient’s nasal subunits. With the ink still wet, a single layer of white Steri-Strips (3M) is placed over the nose and defect to cover all marked subunits. A Tegaderm (3M) transparent dressing is then placed over the Steri-Strips. After these two materials are adhered together, the entire dressing is removed from the nose as a single unit. When removed, the dressing will retain its original structure, and a 3D outline of the defect and nasal subunits will be seen. Another Tegaderm dressing is placed on the sticky undersurface of the Steri-Strips. A marking pen is then used to retrace the markings of the nasal subunits, which are visible underneath the Tegaderm. A complete template of the patient’s entire nose is created and set aside for later use. If desired, this 3D template can also be pressed against the foil of a suture package, leaving a blueprint of the nasal subunits and defect that can be cut into individual pieces. As the patient’s flap is raised, the template or foil pieces are brought back into the field to serve as a guide in accurately transcribing the 3D structure of the desired subunit(s) onto the 2D surface of the flap.
Results:
This technique serves as an efficient and inexpensive method for creating a template that matches the inherent curves and contours of a patient’s nasal anatomy. Common methods of nasal template creation are often time-consuming due to the challenge of transposing a 3D structure onto a 2D template. This template technique addresses this problem—allowing for accurate template creation in minutes. Furthermore, the template serves as a powerful tool in cases where the anatomy of the reconstructed side is distorted, such as complete alar subunit defects. By flipping the template inside-out, the normal side of the template is transposed onto the defect site and guides accurate placement of the alar base. The template is also valuable in cases of complex nasal reconstruction, where multiple subunits are missing.
Conclusion:
Template design in nasal reconstruction is often limited by time, cost, or accuracy. This template technique serves as an efficient, inexpensive, and accurate guide in nasal reconstruction.
Statement of Ethics:
This study was determined by the Loma Linda University Health Internal Review Board policies and procedures to be exempt. As no direct identifiers were included in the article and all data was deidentified, authorization for disclosure of protected health information was not required, according to the Loma Linda University Health Internal Review Board policies and procedures.
Conflict of Interest Statement:
The authors have no conflicts of interest to declare.
Author Disclosure Statement:
There are no author affiliations with commercial interests to disclosure. The abstract of this video was presented at the 2023 American Academy of Facial Plastic and Reconstructive Surgery Advances in Rhinoplasty & Facial Rejuvenation Meeting, April 2023, San Diego, CA.
Funding Sources:
This study was not supported by any sponsor or funder.
Runtime of video: 2 mins 40 secs.
Get full access to this article
View all access options for this article.
