Abstract
In the lung, exposure to chronic hypoxia (CH) causes pulmonary hypertension, a debilitating disease. Development of this condition arises from increased muscularity and contraction of pulmonary vessels, associated with increases in pulmonary arterial smooth muscle cell (PASMC) intracellular pH (pHi) and Ca2+ concentration ([Ca2+]i). In this study, we explored the interaction between pHi and [Ca2+]i in PASMCs from rats exposed to normoxia or CH (3 weeks, 10% O2). PASMC pHi and [Ca2+]i were measured with fluorescent microscopy and the dyes BCECF and Fura-2. Both pHi and [Ca2+]i levels were elevated in PASMCs from hypoxic rats. Exposure to KCl increased [Ca2+]i and pHi to a similar extent in normoxic and hypoxic PASMCs. Conversely, removal of extracellular Ca2+ or blockade of Ca2+ entry with NiCl2 or SKF 96365 decreased [Ca2+]i and pHi only in hypoxic cells. Neither increasing pHi with NH4Cl nor decreasing pHi by removal of bicarbonate impacted PASMC [Ca2+]i. We also examined the roles of Na+/Ca2+ exchange (NCX) and Na+/H+ exchange (NHE) in mediating the elevated basal [Ca2+]i and Ca2+-dependent changes in PASMC pHi. Bepridil, dichlorobenzamil, and KB-R7943, which are NCX inhibitors, decreased resting [Ca2+]i and pHi only in hypoxic PASMCs and blocked the changes in pHi induced by altering [Ca2+]i. Exposure to ethyl isopropyl amiloride, an NHE inhibitor, decreased resting pHi and prevented changes in pHi due to changing [Ca2+]i. Our findings indicate that, during CH, the elevation in basal [Ca2+]i may contribute to the alkaline shift in pHi in PASMCs, likely via mechanisms involving reverse-mode NCX and NHE.
Keywords
Many chronic lung diseases are characterized by prolonged exposure to hypoxic conditions, with resulting development of pulmonary hypertension. The pathogenesis of hypoxic pulmonary hypertension is associated with changes in the pulmonary vasculature that include both contraction and growth of pulmonary arterial smooth muscle cells (PASMCs). The exact mechanisms underlying these changes are incompletely understood, although it is becoming apparent that these changes may be related to alterations in intracellular Ca2+ or pH homeostasis.
Our previous studies have revealed that exposure to chronic hypoxia (CH) increased the expression of Na+/H+ exchanger isoform 1 (NHE1), enhanced the activity of Na+/H+ exchange, and created an alkaline shift in intracellular pH (pHi) in PASMCs.1,2 Increased pHi is associated with PASMC proliferation in response to growth factors3,4 and, under some conditions, with enhanced smooth muscle contraction.5–8 A role for Na+/H+ exchange in modulating PASMC growth during CH was initially suggested by studies indicating that inhibitors of Na+/H+ exchange attenuated pulmonary vascular remodeling in chronically hypoxic rats. 9 Moreover, an absence of alkalinization correlated with reduced remodeling in a murine model of hypoxic pulmonary hypertension. 2 Later studies demonstrated that genetic loss of NHE1 prevented CH-induced pulmonary vascular remodeling 10 and attenuated hypoxia-induced proliferation and migration in vitro. 11
Prolonged hypoxic conditions have also been shown to cause influx of Ca2+ into PASMCs through store-operated12,13 or voltage-gated 14 Ca2+ channels, resulting in increased intracellular calcium concentration ([Ca2+]i). [Ca2+]i is well known to contribute to a variety of cell functions, with increased [Ca2+]i contributing to PASMC contraction13,15–19 and playing a role in smooth muscle cell proliferation20–23 and migration. 24
Interactions between pHi and [Ca2+]i have been demonstrated in smooth muscle under normoxic conditions.25,26 For example, although increasing [Ca2+]i alone was not sufficient to alter pHi,27,28 certain agonists that increased [Ca2+]i, including thrombin and angiotensin II, were found to also cause acidification.26,28,29 Others found that increasing or decreasing pHi resulted in an increase in Ca2+ influx.6,8,30–32 These studies suggest that the regulation of [Ca2+]i and pHi could be interdependent. Both [Ca2+]i and pHi increase in PASMCs during CH; however, it is not known whether these changes in pH and Ca2+ homeostasis are related or occur via completely independent mechanisms. Thus, the goals of this study were to determine (i) the relationship between pHi and [Ca2+]i in PASMCs during normoxia, (ii) whether this relationship is altered following exposure to CH, and, if so, (iii) the mechanisms involved. We used fluorescent microcopy with the Ca2+-senstive dye, Fura-2, and the pH-sensitive dye, BCECF, in transiently cultured PASMCs isolated from normoxic and chronically hypoxic rats to determine the effects of changing [Ca2+]i on pHi and vice versa.
METHODS
Hypoxic exposure
All protocols were approved by the Johns Hopkins Animal Care and Use Committee. Adult male Wistar rats (250-350 g) were placed in a hypoxic chamber for 3 weeks as described elsewhere. 13 The chamber was continuously gassed with a mixture of room air and 100% N2 to maintain 10% + 0.5% O2 and low CO2 concentrations (<0.5%). O2 levels inside the chamber were continuously monitored (PRO-OX, RCI Hudson, Anaheim, CA), and this value was used by a servo controller to adjust N2 inflow. Animals were allowed free access to food and water and were removed from the chamber for less than 5 minutes twice a week to replenish food and water supplies and to clean the cages. Normoxic animals were kept next to the chamber in room air and were thus exposed to similar temperatures and a similar light/dark cycle.
A total of 3,846 cells were analyzed for this study. The methods for obtaining primary cultures of rat PASMCs have been previously described. 15 Briefly, animals were deeply anesthetized with sodium pentobarbital (130 mg/kg via intraperitoneal injection) and the heart and lungs were removed en bloc. Intrapulmonary arteries (200600 μm outer diameter) were dissected and cleaned of connective tissue in ice-cold HEPES-buffered saline solution (HBSS) containing 130 mM NaCl, 5 mM KCl, 1.2 mM MgCl2, 10 mM HEPES, and 10 mM glucose with pH adjusted to 7.2 with 5 M NaOH. The arteries were opened and the lumen gently scraped to remove endothelial cells. The arteries were allowed to recover for 30 minutes in cold (4°C) HBSS followed by 20 minutes in reduced-Ca2+ HBSS (20 μM CaCl2) at room temperature. The tissue was enzymatically digested for 20-25 minutes at 37°C in reduced-Ca2+ HBSS containing collagenase (type I; 1,750 U/mL), papain (9.5 U/mL), bovine serum albumin (2 mg/mL), and dithiothreitol (1 mM). After digestion, single smooth muscle cells were dispersed by gentle trituration in Ca2+-free HBSS and were plated on 25-mm glass coverslips. PASMCs were cultured in Ham's F-12 media containing 0.5% fetal calf serum and 1% penicillin/streptomycin for 24–48 hours.
Measurement of [Ca2+]i
[Ca2+]i was measured in rat PASMCs as previously described. 13 Cells were incubated with 5 μM Fura-2 AM, a membrane permanent (acetoxymethyl ester) form of Fura-2, for 60 minutes at 37°C under an atmosphere of 16% O2 and 5% CO2. Following incubation, cells were placed in a laminar flow cell chamber perfused with modified Kreb's solution (KRB) containing 118.3 mM NaCl, 4.7 mM KCl, 1.2 mM MgSO4, 25 mM NaHCO3, 11 mM glucose, and 1.2 mM KH2PO4 and then gassed with 16% O2 and 5% CO2. Cells were washed for 15 minutes at 37°C to remove extracellular dye and allow complete de-esterification of cytosolic dye. Ratiometric measurement of Fura-2 fluorescence was performed in a workstation based on a Nikon TES 100 Ellipse inverted microscope with epi-fluoresence attachments. The collimated light beam from a xenon arc lamp was filtered by interference filters at 340 and 380 nm and focused onto PASMCs via a 20× fluorescence objective (Super Flour 20, Nikon). Light emitted from the cell was returned through the objective and detected by an imaging camera. An electronic shutter was used to minimize photobleaching of dye. Protocols were executed and data were collected online with InCyte software (Intracellular Imaging, Cincinnati, OH). [Ca2+]i values were calculated from an in vitro calibration curve and thus should be considered an estimate of true [Ca2+]i.
pHi measurements
pHi within PASMCs was monitored using the cell-permeant pH-sensitive dye 2′,7′-bis(carboxyethyl)-5(6)-carboxyflourescein (BCECF AM) as described elsewhere.1,2 Cells were placed in the perfusion chamber, perfused with KRB solution, and excited with light filtered at 490 and 440 nm. Light emitted from the cells was detected at 530 nm. The ratio of 490 to 440 nm emission was calculated and pHi was estimated from in situ calibration after each experiment. For calibration, PASMCs were perfused with a high K+ solution containing 105 mM KCl, 1 mM MgCl2, 1.5 mM CaCl2, 10 mM glucose, 20 mM HEPES-Tris, and 0.01 mM nigericin to allow pHi to equilibrate to external pH (42). A two-point calibration was created from fluorescence measured as pHi was adjusted with KOH from 6.5 to 7.5. Intracellular H+ ion concentration ([H+]i)wasdetermined from pHi using the formula pH = –log([H+]i). For both [Ca2+]i and pHi measurements, cells were perfused using a multi-input, single-output system connected to reservoirs containing control solutions or solutions containing various antagonists. Switching between reservoirs allowed for rapid exchange of the chamber solution.
Drugs and solutions
Ethyl isopropyl amiloride (EIPA), SKF-96365 (SKF), and bepridil (BPD) were made up as 10−2 M stock solutions in DMSO (for EIPA and BPD) or distilled water and refrigerated until use. KB-R7943 was made up as a 10−1 M stock solution in DMSO, aliquoted, and frozen until use. Dichlorobenzamil (DCB) was made as a 10-mM stock in de-ionized water, aliquoted, and stored at 4°C until use. All other drugs were solubilized in de-ionized water on the day of the experiment. Drugs were diluted to final working concentrations in perfusate solutions. Vehicle (DMSO 1:1,000 dilution) had no effect on either [Ca2+]i or pHi. KB-R7943 (KBR) was obtained from Tocris (Ellisville, MO). Fura-2 AM and BCECF AM were obtained from Molecular Probes (Eugene, Oregon). All other chemicals were from Sigma-Aldrich.
DATA ANALYSIS
All values are expressed as mean ± SEM; n refers to the number of cells. All experiments were performed a minimum of 3 times (1027 cells/experiment) using cells obtained from a minimum of 3 different animals. pH values were converted to [H+] values for statistical analysis. For agents that induced a change in pHi or [Ca2+]i, statistical analysis was performed by comparison of values before and after treatment using paired Student t test. The effect of chronic hypoxia or inhibitors on the response to agents that caused a change in [Ca2+]i or pHi was evaluated by comparing the change in pHi or [Ca2+]i induced in the presence and absence of inhibitors or between normoxia and hypoxia, as a group using ANOVA. A P value <0.05 was accepted as statistically significant.
RESULTS
Effect of CH on pHi and [Ca2+]i in PASMCs
Resting [Ca2+]i in PASMCs isolated from rats exposed to CH was significantly higher compared to resting [Ca2+]i measured in cells isolated from normoxic rats (Fig. 1A). Similarly, basal pHi in PASMCs from rats exposed to CH was increased compared to PASMCs isolated from normoxic rats (Fig. 1B). The baseline values of both [Ca2+]i and pHi are qualitatively and quantitatively similar to those observed in our previous studies.1,2,13,15
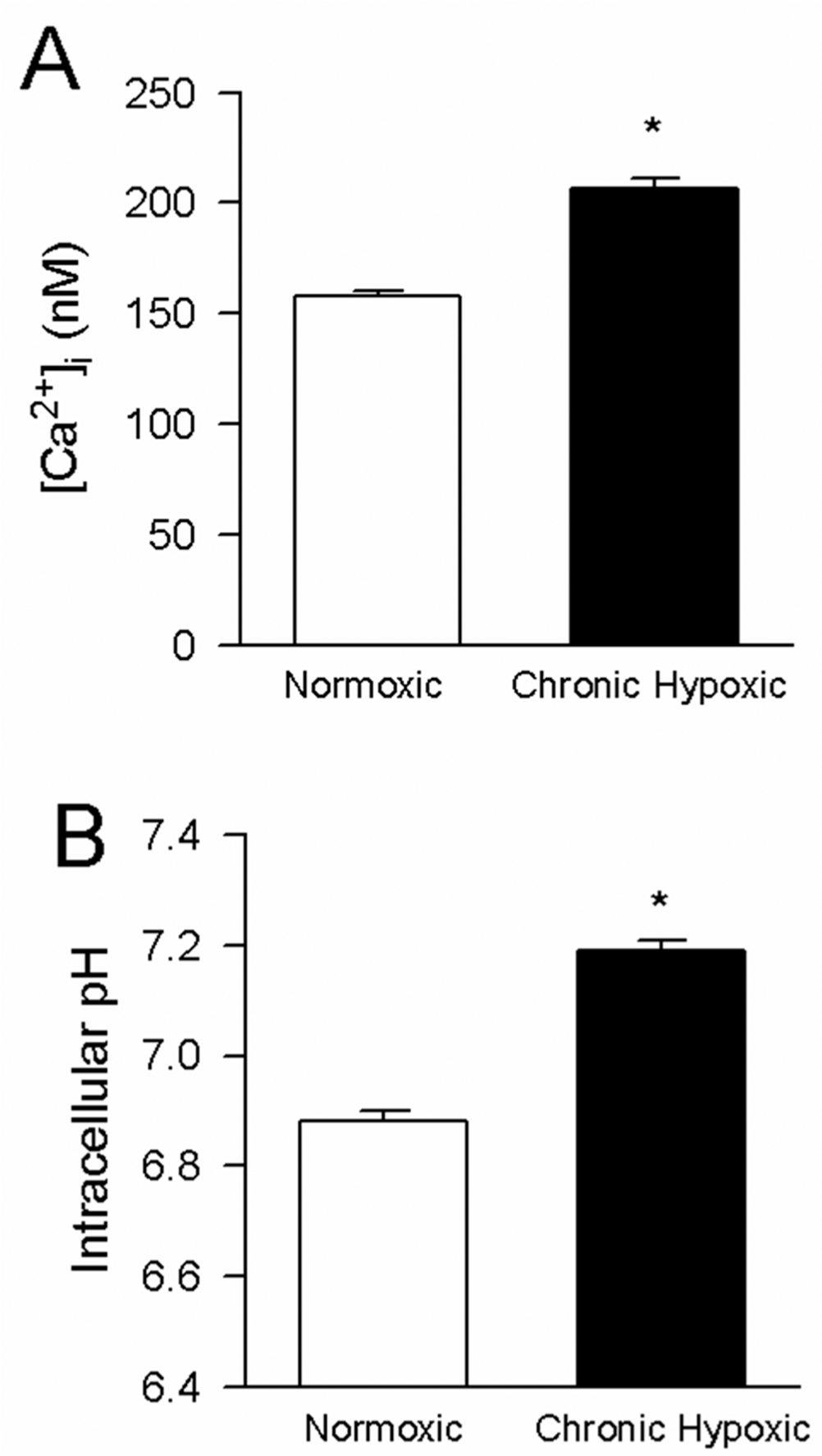
Bar graphs showing mean ± SEM values for resting intracellular Ca2+ concentration ([Ca2+]i; A) and basal intracellular pH (pHi; B) in pulmonary arterial smooth muscle cells isolated from rats exposed to normoxia (n = 204 for [Ca2+]i and n = 550 for pHi) and chronic hypoxia (n = 455 for [Ca2+]i and n = 934 for pHi). Asterisk indicates a significant difference from the normoxic value (P < 0:05).
Effect of depolarization or Ca2+ channel blockers on [Ca2+]i
Exposure to KCl (80 mM), which causes depolarization and Ca2+ entry through voltage-dependent Ca2+ channels, increased [Ca2+]i in PASMCs from both normoxic and chronically hypoxic rats (Fig. 2A). In normoxic PASMCs, the increase in [Ca2+]i in response to KCl was slightly lower than that observed in hypoxic PASMCs. In normoxic cells, removal of extracellular Ca2+ or exposure to NiCl2 (500 nM), a nonspecific inhibitor of Ca2+ entry through nonselective cation channels (NSCCs), which includes store-operated Ca2+ channels, had no significant effect on basal [Ca2+]i. Somewhat surprisingly, application of SKF-96365 (10 μM), a more specific NSCC inhibitor, caused a slight, but statistically significant, increase in [Ca2+]i in normoxic cells. In contrast, in hypoxic PASMCs, removal of extracellular Ca2+ or application of NiCl2 or SKF-96365 decreased [Ca2+]i. These decreases in basal [Ca2+]i in PASMCs from chronically hypoxic rats in response to Ca2+-free conditions or inhibition of NSCCs are consistent with our previous observations. 13
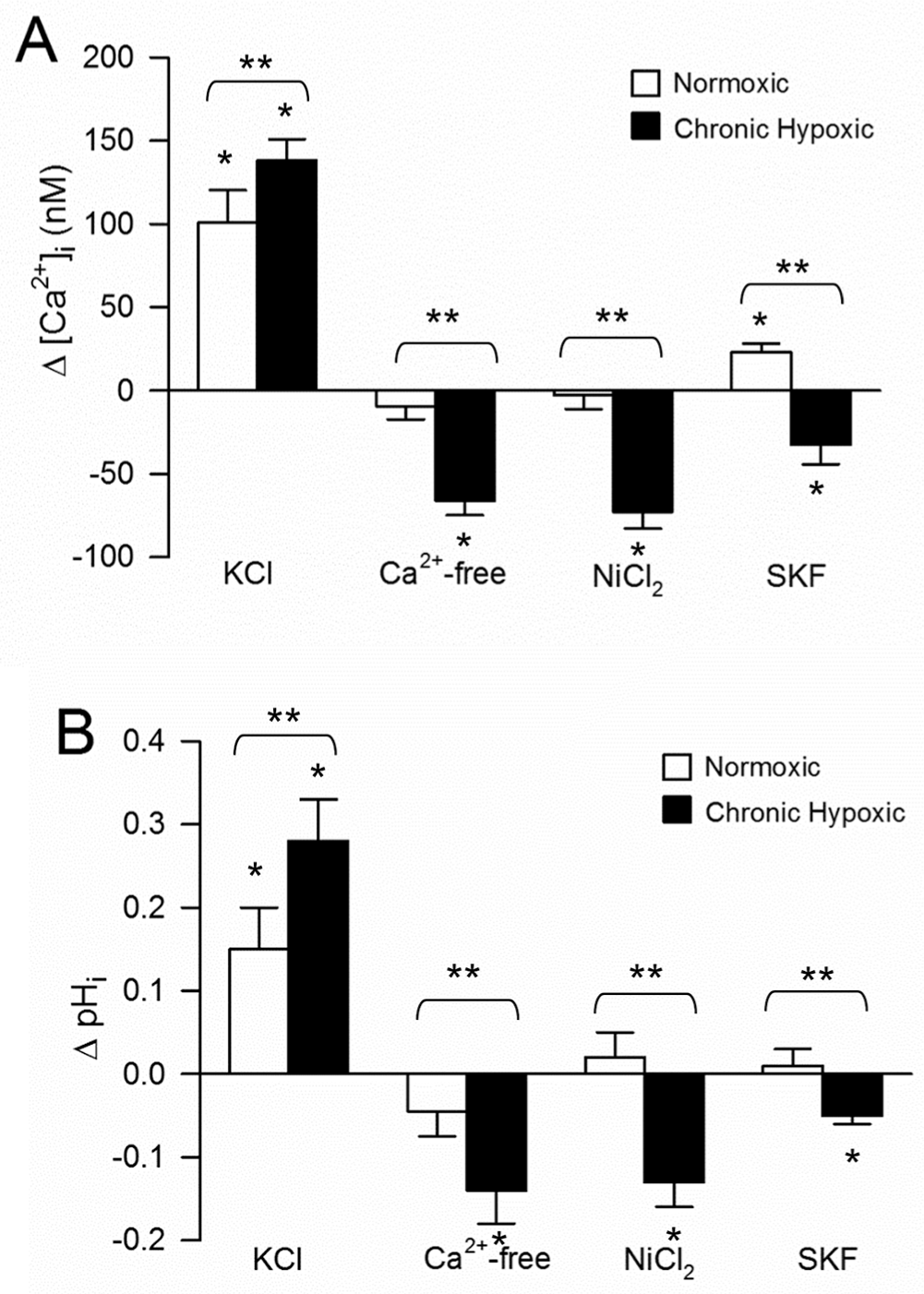
A, Effect of exposure to KCl (80 mM; n = 97 for normoxic and n = 138 for hypoxic); removal of extracellular Ca2+ (Ca2+-free; n = 83 for normoxic and n = 69 for hypoxic); treatment with NiCl2 (500 nM; n = 72 for normoxic and n = 79 for hypoxic) or treatment with SKF96365 (SKF; 10 μM; n = 79 for normoxic and n = 47 for hypoxic) on intracellular Ca2+ ([Ca2+]i) in rat pulmonary arterial smooth muscle cells (PASMCs). B, Change in intracellular pH (pHi) induced in PASMCs from normoxic and chronically hypoxic rats by exposure to KCl (n = 42 for normoxic and n = 37 for hypoxic); removal of extracellular Ca2+ (n = 92 for normoxic and n = 34 for hypoxic); treatment with NiCl2 (n = 89 for normoxic and n = 42 for hypoxic) or treatment with SKF (n = 55 for normoxic and n = 66 for hypoxic). Data are expressed as mean ± SEM change (Δ) in [Ca2+]i or pHi. Asterisk indicates significant difference from baseline; two asterisks indicate significant difference between normoxic and hypoxic values.
Effect of changing [Ca2+]i on pHi
Increasing [Ca2+]i by exposure to KCl (80 mM) increased pHi in PASMCs from both normoxic and chronically hypoxic rats (Fig. 2B). Similar to the greater increase in [Ca2+]i induced by KCl in chronically hypoxic PASMCs, the magnitude of the KCl-induced increase in pHi was also greater in hypoxic PASMCs than in cells from normoxic rats. Although exposure to KCl increased pHi, the removal of extracellular Ca2+ using a Ca2+-free solution caused a significant decrease in pHi only in cells from chronically hypoxic rats. Qualitatively similar results were obtained with NiCl2 and SKF, which had no significant effect on pHi in normoxic cells but significantly decreased pHi in PASMCs isolated from chronically hypoxic rats. Interestingly, Ca2+-free solution and NiCl2 caused quantitatively similar reductions in both [Ca2+]i and pHi in PASMCs from hypoxic animals, whereas the effect of SKF was approximately 50% less in both cases.
Effect of removal of bicarbonate or exposure to NH4Cl on pHi
To alter pHi, PASMCs were exposed to HEPES-buffered extracellular solution, which removes the contribution of Cl-/HCO3-exchangers in pHi homeostasis, or to 3 or 10 mM NH4Cl, which causes alkalinization due to buffering of intracellular H+. As expected, based on our previous observations and studies in guinea pig pulmonary vascular smooth muscle,1–3 removal of bicarbonate caused a brief increase in pHi that subsided to a sustained reduction in pHi in cells from both normoxic and chronically hypoxic rats (Fig. 3A). Conversely, exposure to either 3 or 10 mM NH4Cl caused a significant increase in pHi in PASMCs from both normoxic and chronically hypoxic rats. Although 3 mM NH4Cl induced a change in pHi that was quantitatively similar in normoxic and hypoxic cells, the increase in pHi induced by 10 mM NH4Cl was substantially larger in cells from rats exposed to CH compared with normoxia. In most cells, the response to NH4Cl was a maintained increase in pHi, although in some cells, there was a transient large increase in pHi that then decreased to a sustained level that was below the peak but still above basal levels. In all experiments, pHi was measured after 10 minutes of exposure to either bicarbonate-free solution or NH4Cl, during the sustained phase of the response.
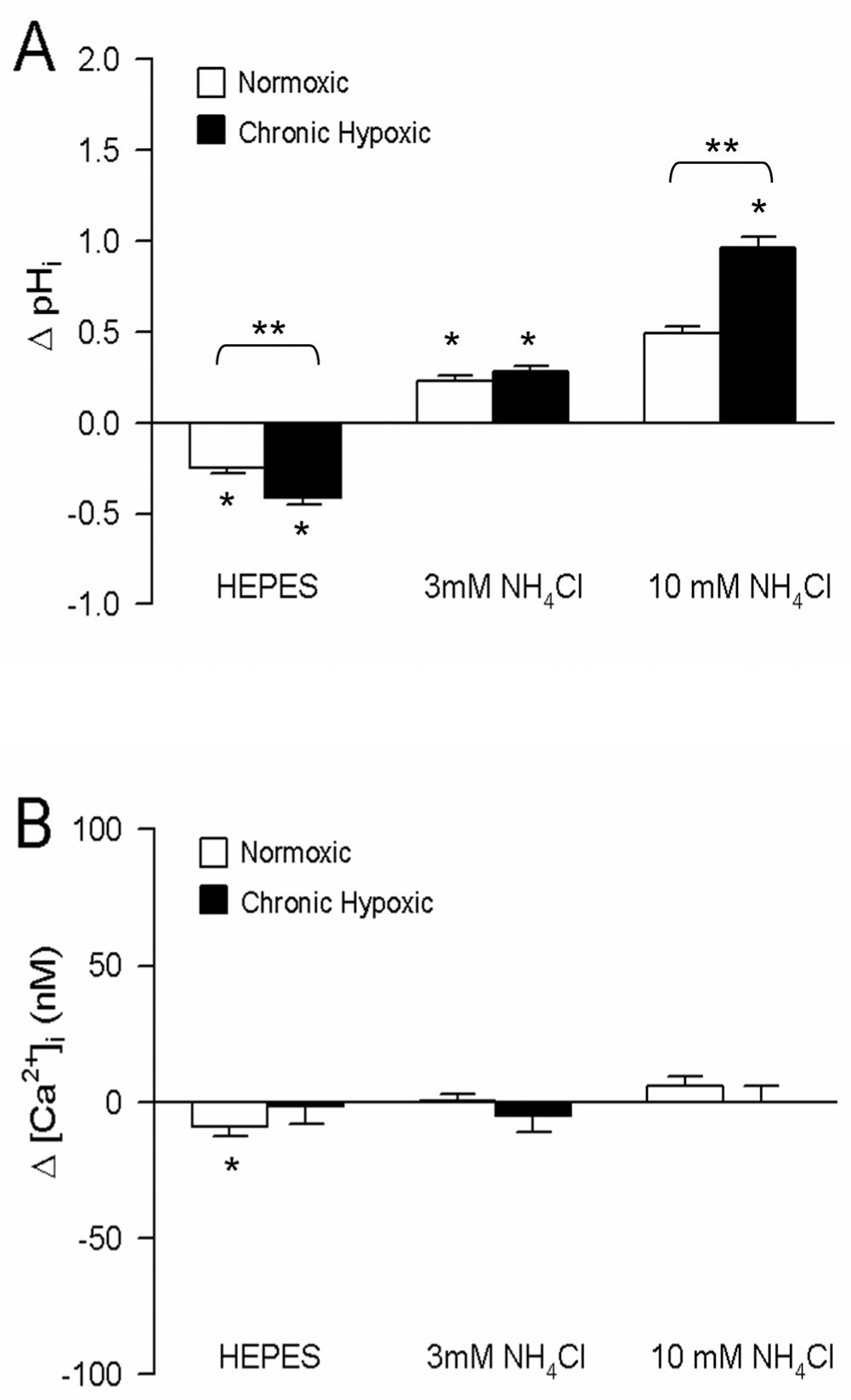
A, Effect of removal of extracellular bicarbonate (HEPES; n = 28 cells for normoxic and n = 32 cells for hypoxic) and exposure to 3 mM (n = 88 for normoxic and n = 77 for hypoxic) or 10 mM (n = 25 for normoxic and n = 32 for hypoxic) ammonium chloride (NH4Cl) on intracellular pH (pHi) in pulmonary arterial smooth muscle cells (PASMCs) from normoxic and chronically hypoxic rats. B, Changes in intracellular Ca2+ ([Ca2+]i) induced by exposure of PASMCs to HEPES-buffered extracellular solution (n = 85 for normoxic and n = 48 for hypoxic) or NH4Cl (3 mM: n = 69 for normoxic and n = 82 for hypoxic; 10 mM: n = 100 for normoxic and n = 48 for hypoxic). Asterisk indicates significant difference from baseline; two asterisks indicate significant difference between normoxic and hypoxic values.
Increasing pHi by exposure to 3 or 10 mM NH4Cl had no significant effect on [Ca2+]i in PASMCs isolated from normoxic or chronically hypoxic rats (Fig. 3B), although a small subset of cells exposed to 10 mM NH4Cl (21 of 100 in normoxic; 7 of 48 in hypoxic) exhibited a transient increase in [Ca2+]i that rapidly returned to basal levels. Because pHi and [Ca2+]i were not measured simultaneously in the same cells, it is unclear whether the cells that exhibited a transient increase in [Ca2+]i also exhibited a transient overshoot in pHi in response to NH4Cl. Decreasing pHi by perfusing the cells with a HEPES-buffered solution caused a very small but statistically significant decrease in [Ca2+]i in PASMCs from normoxic rats, whereas no effect on [Ca2+]i was observed in PASMCs from chronically hypoxic rats.
Role of Na+/H+ exchange in mediating changes in pHi induced by changing [Ca2+]i
We1,2 and others3,33 have previously reported that Na+/H+ exchange contributes to regulation of pHi in PASMCs. To assess the contribution of Na+/H+ exchange in regulating pHi in PASMCs from normoxic and chronically hypoxic rats, cells were exposed to EIPA, a Na+/H+ exchange inhibitor. Blockade of Na+/H+ exchange with EIPA (10 μM) caused a significant decrease in pHi in PASMCs from normoxic animals (Fig. 4A). Consistent with our previously reported results, EIPA caused a decrease in pHi in PASMCs isolated from chronically hypoxic rats that was greater than the decrease observed in normoxic PASMCs. EIPA caused a small but statistically significant increase in baseline [Ca2+]i in PASMCs from normoxic animals (Fig. 4B) and a small but statistically significant decrease in [Ca2+]i in chronically hypoxic PASMCs. When PASMCs were pretreated with EIPA, the changes in pHi induced by KCl, removal of extracellular Ca2+, or exposure to NiCl were abolished (Fig. 4C).
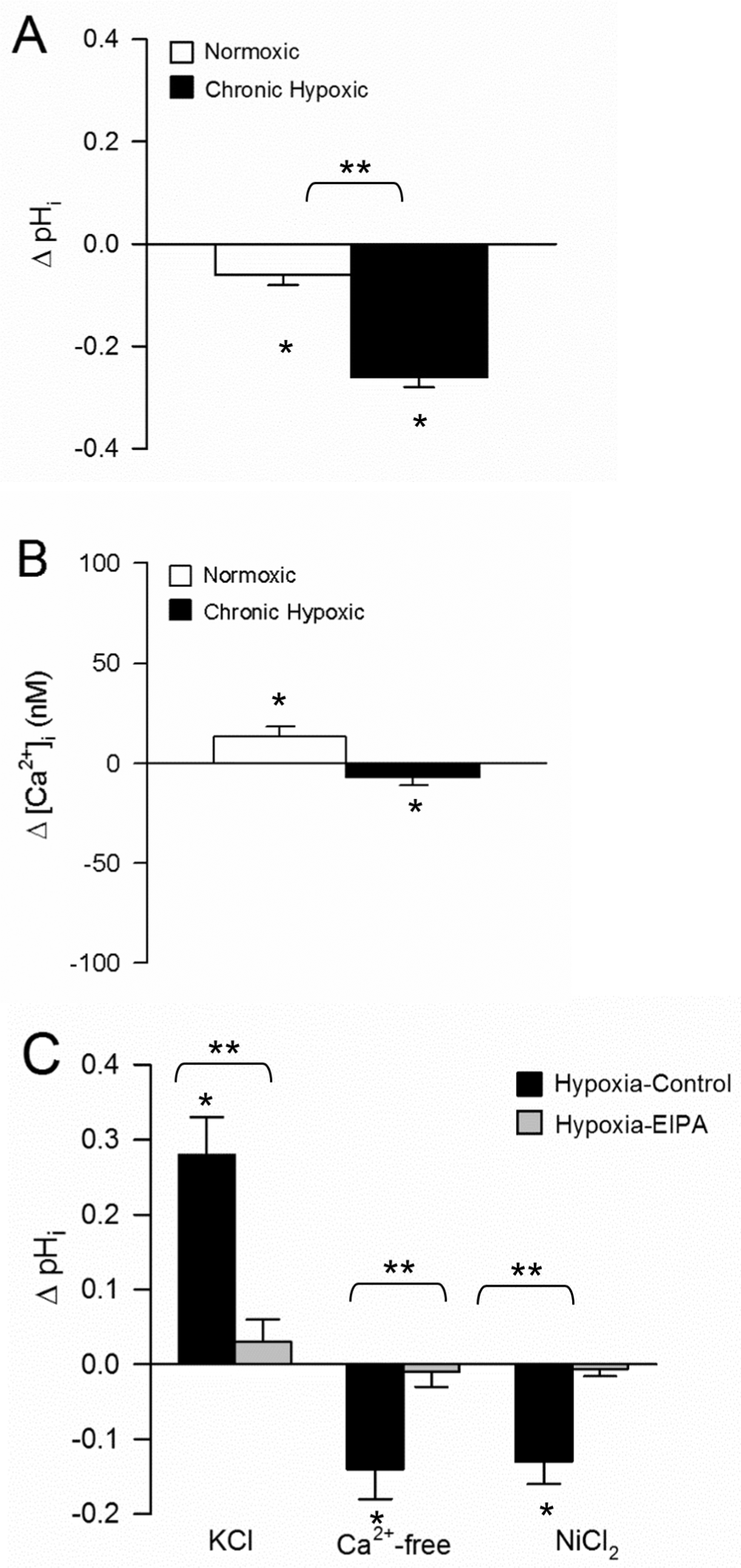
Role of Na+/H+ exchange in mediating Ca2+-dependent changes in intracellular pH (pHi). Effect of ethyl isopropyl amiloride (EIPA; 10 μM) on basal pHi (A) and intracellular Ca2+ ([Ca2+]i; B) in pulmonary arterial smooth muscle cells (PASMCs) from normoxic (n = 40 for pHi and n = 42 for [Ca2+]i) or chronically hypoxic (n = 49 for pHi and n = 100 for [Ca2+]i) rats. Asterisk indicates significant difference from baseline; two asterisks indicate significant difference between normoxic and hypoxic values. C, EIPA prevented the change in pHi induced by changing [Ca2+]i via perfusion with KCl (80 mM; n = 42 for untreated and n = 47 for EIPA), Ca2+-free solution (n = 92 for untreated and n = 35 for EIPA) or NiCl2 (500 nM; n = 89 for untreated and n = 31 for EIPA) in PASMCs from chronically hypoxic rats. Data are presented as mean ± SEM. Two asterisks indicate significant difference between values in the presence and absence of EIPA.
Is Na+/Ca2+ exchange involved in regulating pHi and [Ca2+]i?
A main mechanism regulating Ca2+ extrusion in PASMCs is the Na+/Ca2+ exchanger (NCX).34–36 This exchanger generally transports one Ca2+ ion out of the cell in exchange for 3 Na+ ions into the cell; however, under certain conditions the exchanger can reverse, resulting in Ca2+ influx. Although acute hypoxia has been suggested to alter NCX activity,35,36 it is not known whether either forward-mode (Ca2+ extrusion) or reverse-mode (Ca2+ entry) NCX contributes significantly to PASMC Ca2+ homeostasis during CH. The role of NCX in regulating resting [Ca2+]i levels in PASMCs was tested by addition of 50 μM BPD or 15 μM DCB, general NCX inhibitors. In normoxic cells, both BPD and DCB increased [Ca2+]i, consistent with blockade of Ca2+ extrusion (Fig. 5A). Addition of KB-R7943 (KBR; 10 μM), an inhibitor selective for reverse-mode (Ca2+ entry) NCX, to normoxic PASMCs had no significant effect on [Ca2+]i. In contrast, when chronically hypoxic PASMCs were treated with BPD, DCB, or KBR, basal [Ca2+]i decreased to a similar extent, presumably due to blockade of Ca2+ entry via reverse-mode Na+/Ca2+ exchange.
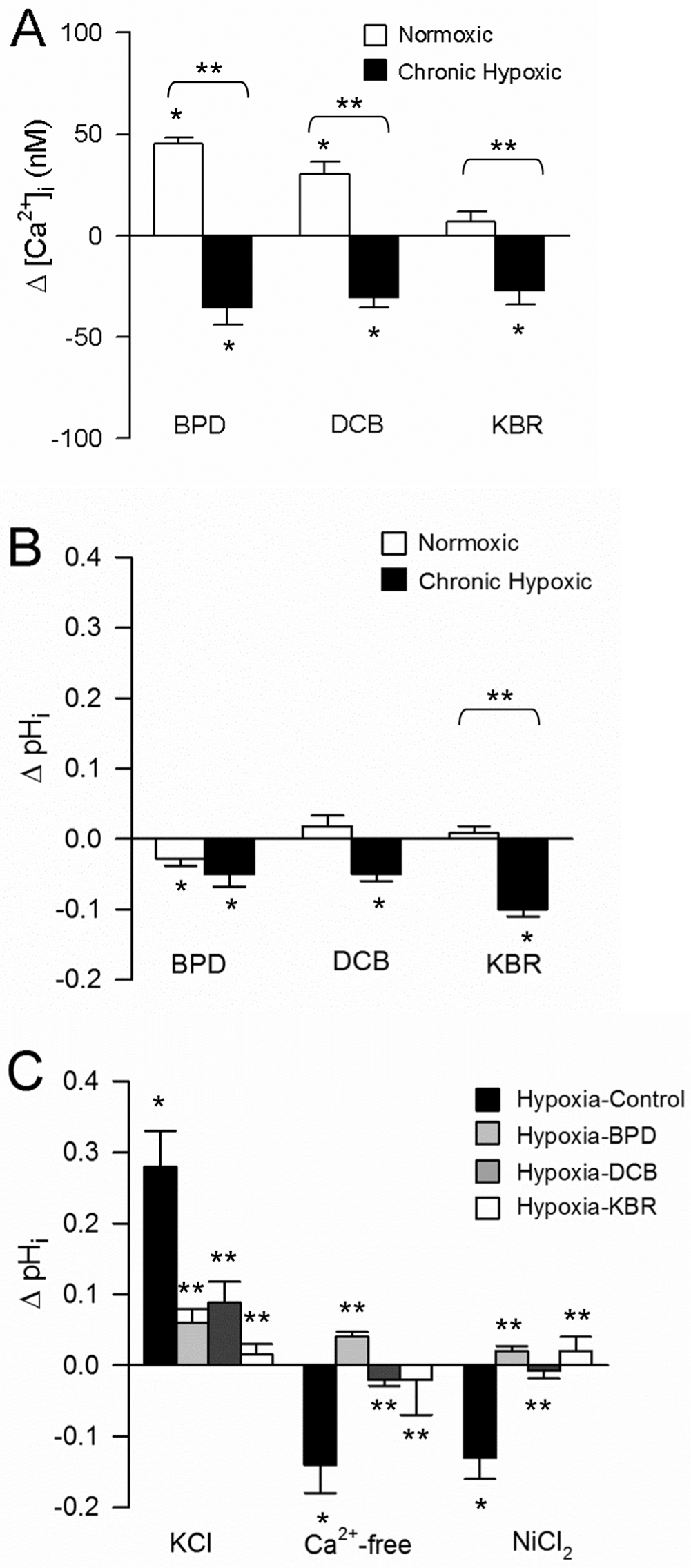
Role of Na+/Ca2+ exchange in mediating Ca2+-dependent changes in intracellular pH (pHi). All data are presented as mean ± SEM. A, Effect of bepridil (BPD; n = 119 for normoxic and n = 72 for hypoxic), dichlorobenzamil (DCB; n = 86 for normoxic and n = 68 for hypoxic), and KB-R7943 (KBR; n = 97 for normoxic and n = 127 for hypoxic) on basal intracellular Ca2+ ([Ca2+]i) in pulmonary arterial smooth muscle cells (PASMCs) from normoxic and chronically hypoxic rats. B, Effect of BPD (n = 90 for normoxic and n = 39 for hypoxic), DCB (n = 70 for normoxic and n = 70 for hypoxic), and KBR (n = 89 for normoxic and n = 83 for hypoxic) on basal pHi in PASMCs. A and B, asterisk indicates significant difference from baseline; two asterisks indicate significant difference between normoxic and hypoxic values. C, The effect of pretreating cells from chronically hypoxic rats with BPD, DCB, or KBR on the change in pHi induced by changing [Ca2+]i with 80 mM KCl (n = 37, 63, 111, and 37 for control, BPD, DCB, and KBR, respectively), Ca2+-free extracellular solution (n = 34, 74, 103, and 35 for control, BPD, DCB, and KBR, respectively), or 500 nM NiCl2 (n = 42, 89, 98, and 56 for control, BPD, DCB, and KBR, respectively). Asterisk indicates significant difference from baseline; two asterisks indicate significant difference between values in the absence (control hypoxic) and presence of Na+/Ca2+ exchange inhibitor.
Because reverse-mode NCX appeared to participate in regulation of [Ca2+]i levels in PASMCs from chronically hypoxic, but not normoxic, animals, we tested whether reverse-mode NCX was contributing to either basal pHi or changes in pHi during stimulation in PASMCs following exposure to CH. We found that, while DCB and KBR had no significant effect on basal pHi, BPD caused a slight but statistically significant decrease in basal pHi in PASMCs from normoxic rats (Fig. 5B). In cells from hypoxic rats, all three NCX inhibitors decreased pHi. When PASMCs from chronically hypoxic rats were pretreated with BPD, DCB, or KBR, changes in pHi observed when [Ca2+]i was increased by KCl or decreased by removal of extracellular Ca2+ or addition of NiCl2 were significantly attenuated (Fig. 5C).
DISCUSSION
During CH, PASMCs exhibit increases in both [Ca2+]i and pHi. Although our previous studies suggested that the elevation in [Ca2+]i and alkaline shift in pHi were associated with increased expression of NSCCs and Na+/H+ exchangers, respectively, it was unclear whether activation of these channels/transporters might also be altered and, if so, whether the changes were interdependent. Thus, the goal of the current study was to determine whether the elevation in basal [Ca2+]i contributed to the alkaline shift in pHi and vice versa. Our findings indicate that, during CH, changes in PASMC pHi do not significantly impact [Ca2+]i, whereas changes in basal [Ca2+]i may contribute to the elevation in pHi.
We found that KCl was able to increase [Ca2+]i in PASMCs from both normoxic and chronically hypoxic animals and that the effect of KCl appears to be enhanced in cells from hypoxic animals. This would be consistent with recent reports showing upregulation of voltage-gated Ca2+ channel expression and increased KCl-induced Ca2+-influx in PASMCs derived from chronically hypoxic mice. 37 In contrast, measures designed to reduce [Ca2+]i were only effective in PASMCs from chronically hypoxic animals, likely due to the low basal [Ca2+]i levels observed in normoxic cells. The lack of effect of Ca2+ channel blockers on basal [Ca2+]i in normoxic PASMCs is consistent with our previous results and those of other laboratories.12,13,15,38 Similar to our previous results, 39 blockade of NSCCs with SKF caused a small but statistically significant increase in basal [Ca2+] under normoxic conditions. A similar SKF-induced increase in [Ca2+]i has been noted in frog mesenteric endothelial cells 40 and a megakaryoblastic cell line, 41 as well as in endothelial cells at higher concentrations. 42 Although the exact mechanism underlying the increase in [Ca2+]i is unknown, SKF has been shown to depolarize smooth muscle 43 and, in endothelial cells, SKF can block K+ currents with an estimated 50% inhibitory concentration near the concentrations used to block NSCC. 42 Because of these uncertainties, we did not use SKF in the experiments designed to test the role of NCX and/or NHE in Ca2+-induced changes in pHi.
Interestingly, in cells isolated from chronically hypoxic animals, removal of extracellular Ca2+ and application of NiCl2 caused similar reductions in [Ca2+]i, whereas the effect of SKF was significantly less. One explanation for these differences is that, while SKF is considered a relatively selective inhibitor of Ca2+ entry through NSCCs, removal of extracellular Ca2+ and application of NiCl2 are less selective for specific Ca2+ channels/transporters. Indeed, both removal of Ca2+ and application of NiCl2 also would prevent Ca2+ entry through voltage-gated Ca2+ channels or reverse-mode Na+/Ca2+ exchange. 44 The lack of effect of nifedipine or verapamil on baseline [Ca2+]i in PASMCs from chronically hypoxic animals13,15 indicates that these channels do not contribute significantly to maintenance of elevated basal [Ca2+]i and thus would not be expected to contribute to the decrease in [Ca2+]i observed with Ca2+ removal. In contrast, application of BPD, DCB, or KBR, all of which can block reverse-mode NCX, reduced [Ca2+]i selectively in PASMCs isolated from chronically hypoxic animals. This finding is consistent with data demonstrating that reverse-mode NCX contributes to maintenance of elevated basal [Ca2+]i in myocytes from hypertensive rats 45 and influences PASMC proliferation. 46 Although the magnitude of the decrease in [Ca2+]i in response to NCX inhibitors was much less than that induced by extracellular Ca2+ removal, signifying a small role for Ca2+ entry through NCX in maintenance of basal [Ca2+]i, it was qualitatively similar to the difference between the effect of SKF and those of NiCl2 or removal of extracellular Ca2+, suggesting the contributions of NSCCs and NCX to maintenance of resting [Ca2+]i might be additive.
Regardless of whether increased by KCl or decreased by blockade of Ca2+ entry, changing [Ca2+]i induced similar directional changes in pHi. These results support other reports indicating that changes in [Ca2+]i can influence smooth muscle pHi regulation27,28,47–49 and indicate that the mechanisms involved in maintaining elevated basal [Ca2+]i may contribute to alkalination of basal pHi in PASMCs from chronically hypoxic animals. Interestingly, in rat aortic smooth muscle, changing Ca2+ was also found to change pHi, 26 but in the opposite direction, with increased [Ca2+]i causing a reduction in pHi mediated by Ca2+-ATPase. Whether the contrast between our study and the previous report is due to differences in vascular bed, presence of bicarbonate, or other factors remains to be determined.
As expected, removal of bicarbonate or inhibition of Na+/H+ exchange reduced pHi in PASMCs. In both cases, the magnitude of the reduction was greater in PASMCs from hypoxic rats, reflecting the role of Na+/H+ exchange in maintaining increased basal pHi during CH. In contrast, application of NH4Cl increased pHi, due to buffering of intracellular H+ ions. At the lower concentration, the effect of NH4Cl on pHi was similar in cells from normoxic and hypoxic animals and equal in magnitude to the effect of CH on pHi. At the higher concentration, the effect of NH4Cl was greater in PASMCs from hypoxic rats; the exact reason for this difference is not clear. Nonetheless, none of the methods employed to change pHi (removal of bicarbonate, application of NH4Cl, or inhibition of Na+/H+ exchange) significantly altered [Ca2+]i, suggesting that the alkaline shift in pHi observed in PASMCs from chronically hypoxic rats does not contribute to the elevation in basal [Ca2+]i. Although it is clear that none of the manipulations designed to change pHi had a significant impact on [Ca2+]i in our cells, our results stand in contrast to other reports in which changing pHi elicited changes in [Ca2+]i in ferret PASMCs, 8 rat aortic smooth muscle,6,25,30 canine kidney cells, 50 A7r5 cells, 31 endothelial cells, 51 and pancreatic acinar cells. 52 On the other hand, studies involving platelets53–55 also failed to show a change in [Ca2+]i when pHi was adjusted. The reason for the differences between studies remains to be determined, but variations in species, cell type, presence of bicarbonate, the methods used to alter pHi, and/or the magnitude of the change in pHi induced by interventions are likely contributing factors.6,30,52
One aspect that should be taken into consideration when measuring the effect of changes in pHi on [Ca2+]i is that the dissociation constant (K d ) for Fura-2 is pH-sensitive. Over the range of pHi from 7.0 to 7.5, K d will vary little, but with acidic pH (<6.5), K d can increase substantially. 56 For the range of basal pH values and changes in pHi reported in this study (average range of 6.8–7.2 and changes of −0.04 to 0.96 units), K d will vary slightly and does not significantly alter [Ca2+]i values, with a calculated difference of less than 20 nM between corrected and uncorrected values at the highest change in pHi that we observed (0.96 units). These modest changes in magnitude are consistent with those reported by others.30,52 Thus, it is unlikely that pH-induced alterations in K d obscured changes in [Ca2+]i.
In PASMCs from chronically hypoxic animals, all of the changes in pHi induced by changing [Ca2+]i were blocked by pretreatment with EIPA, indicating that the changes were mediated entirely via alterations in Na+/H+ exchange activity. Ca2+-dependent regulation of Na+/H+ exchange has been described in other cell types,27,48,49,57,58 and NHE1 has been demonstrated to complex with, and be activated by, calcium-calmodulin, perhaps providing a link between [Ca2+]i and Na+/H+ exchange activity. 59 Interestingly, an increase in [Ca2+]i was not requisite for calcium-calmodulin activation, which also occurred following tyrosine phosphorylation, 59 and other studies found that simply increasing [Ca2+]i was not sufficient to induce Na+/H+ exchange activation, but instead acted to modulate exchanger activity under certain conditions. 27 Moreover, Na+/H+ exchange activity is heavily influenced by the intracellular Na+ concentration ([Na+]i); reductions in [Na+]i enhance, whereas elevations in [Na+]i reduce, exchanger activity. Thus, in response to our manipulations, it was not clear whether the changes in pHi observed were directly related to the changes in [Ca2+]i or were secondary to changes in [Na+]i, as might occur with changes in NCX activation. The fact that the SKF-induced increase in [Ca2+]i observed in PASMCs from normoxic animals had no significant effect on pHi appeared to rule out a direct effect of increased [Ca2+]i and instead supported the latter possibility. Under normal resting conditions, NCX operates in forward, or Ca2+-extrusion, mode; however, when the cell is depolarized, such as during CH60–62 or exposure to high external [K+], the exchanger operates in reverse, or Ca2+-entry, mode. In this case, Na+ extrusion would be expected to enhance Na+/H+ exchange activity and increase pHi. Thus, inhibiting reverse-mode NCX would be expected to not only decrease Ca2+ entry and [Ca2+]i but also lead to accumulation of intracellular Na+, which would in turn serve to reduce Na+/H+ exchange activity and lower pHi. Indeed, blockade of reverse-mode NCX prevented the changes in pHi induced by KCl, Ca2+-free solution or NiCl2. A role for [Na+]i could also explain the effect of NSCC inhibition in chronically hypoxic PASMCs, as preliminary data suggest that these channels may contribute to depolarization of basal membrane potential in chronically hypoxic PASMCs (data not shown). Although alterations in NCX activity have been shown to modulate [Na+]i, 44 further experiments will be required to determine whether this indeed occurs in PASMCs from chronically hypoxic rats and whether changes in [Na+]i are responsible for mediating the NCX-dependent changes in Na+/H+ exchange activity.
One limitation in defining the role of NCX in mediating changes in [Ca2+]i and pHi in our study is the use of pharmacologic inhibitors, which could have off-target effects. We attempted to more selectively identify the role of NCX using small interfering RNA approaches; however, the long half-life of the protein, which has been reported at ~33 hours in cardiomyocytes, 63 prevented us from achieving adequate knockdown in PASMCs with this method. Similar difficulties have been noted using antisense oligionucleotides in vascular smooth muscle. 64 However, we believe the use of 3 different inhibitors, with different off-target effects, helps to offset concerns about the specificity of the pharmacological approach.
In summary, our findings indicate that, in PASMCs from chronically hypoxic rats, Ca2+ entry via NSCCs and reverse-mode NCX contributed to the sustained increase in basal [Ca2+]i observed in these cells (Fig. 6). Moreover, Na+ efflux through reverse-mode NCX may facilitate increased activation of Na+/H+ exchange activity, contributing to the alkaline shift in pHi. In contrast, the alkaline shift in pHi does not appear to contribute to the maintenance of elevated basal [Ca2+]i. Future studies will be required to elucidate whether the changes in pHi are due to the change in basal [Ca2+]i induced by hypoxia, or are secondary to other effects of the mechanisms involved in Ca2+ homeostasis (i.e., Na+ influx and/or membrane potential).
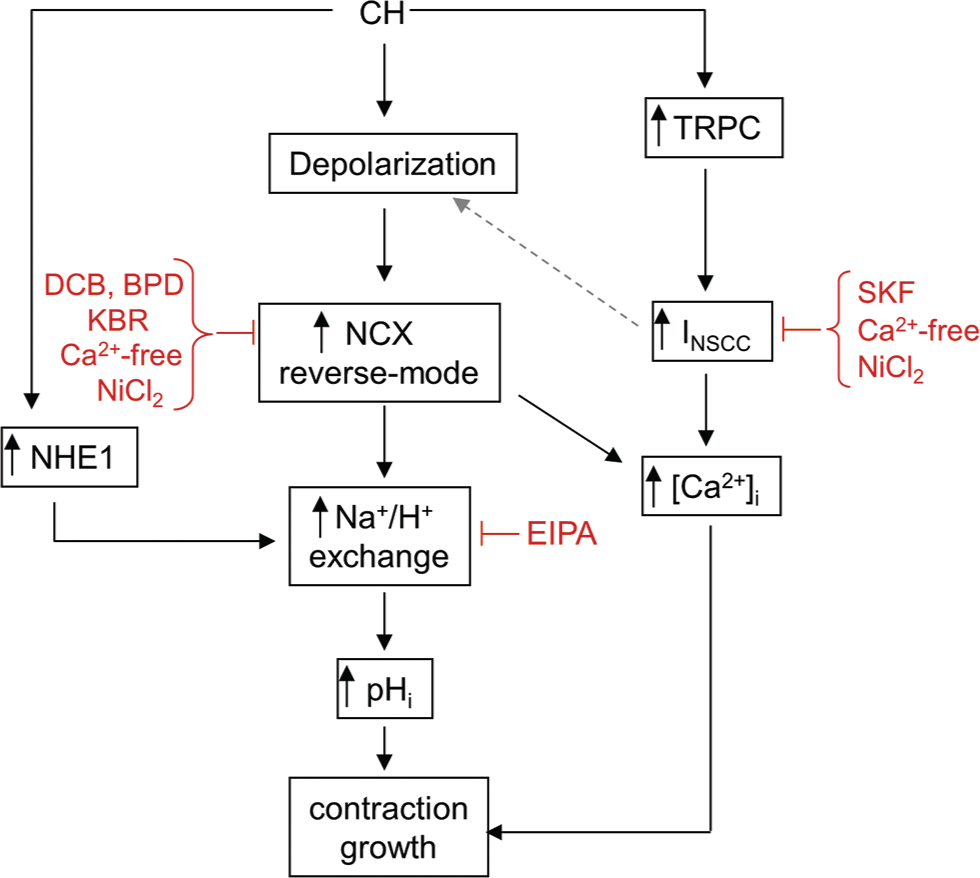
Schematic illustrating proposed mechanism by which changes in intracellular Ca2+ ([Ca2+]i) influence intracellular pH (pHi) in pulmonary arterial smooth muscle cells (PASMCs) during chronic hypoxia (CH). CH has been shown to upregulate the expression of canonical transient receptor potential (TRPC) proteins, leading to increased Ca2+ influx through nonselective cation channels (NSCC) and elevated intracellular Ca2+ concentrations ([Ca2+]i). Because these channels can also conduct Na+, activation may also contribute to depolarization. Depolarization during CH leads to Ca2+ influx through reverse-mode Na+/Ca2+ exchange (NCX), which, along with upregulation of Na+/H+ exchanger isoform 1 (NHE1) expression, leads to increased activation of Na+/H+ exchange and elevated intracellular pH (pHi). Both alkaline pHi and elevated [Ca2+]i have been associated with PASMC proliferation and contraction. Inhibitors are shown in red. Dashed gray line represents hypothesized pathway requiring additional confirmation. DCB: dichlorobenzamil; KBR: KB-R7943; SKF: SKF96365; BPD: bepridil; EIPA: ethylisoproplyamiloride.
