Abstract
In patients with pulmonary arterial hypertension (PAH), chest pain is most likely due to right ventricular demand ischemia. We report a patient with idiopathic PAH who developed severe angina due to extrinsic compression of the left main coronary artery (LMCA) from a dilated pulmonary artery trunk. The diagnosis was verified by electrocardiogram after exercise, coronary angiography including intravascular ultrasound, and cardiac multidetector computed tomography (MDCT). The origin of the LMCA was high in the left coronary sinus, facilitating extrinsic compression. The patient was successfully treated by percutaneous coronary intervention with stent implantation in the LMCA. Extrinsic compression of the LMCA is a severe and potentially fatal complication that should be considered in all patients with PAH and angina. MDCT is the method of choice for first-line diagnosis.
CASE DESCRIPTION
Idiopathic pulmonary arterial hypertension (IPAH) was diagnosed in a 49-year-old woman 6 years ago. She was classified as World Health Organization (WHO) functional class (FC) III at the time of diagnosis, but during treatment with an endothelin receptor antagonist (ambrisentan), she improved considerably and became stable in WHO FC II, with a 6-minute walk test distance of ≥400 m. She was seen at regular intervals of 4–6 months in our outpatient pulmonary hypertension (PH) clinic. During the latest visit, the patient reported increasing dyspnea and tightening chest pain during physical activity. She had no family history or other risk factors for coronary artery disease. On suspicion of worsening PAH, she was admitted to our PH ward for further evaluation.
Physical examination revealed a normal blood pressure of 110/80 mmHg, heart rate of 80 beats/minute, and no sign of right- or left-sided heart failure. Transthoracic echocardiography revealed a moderately dilated right ventricle (RV) with an estimated systolic RV pressure of 100 mmHg and a tricuspid annular plane systolic excursion of 1.3 cm. The left ventricle (LV) was small (end-diastolic diameter: 2.8 cm) with a mildly depressed LV systolic function (LV ejection fraction: 50%). The main pulmonary artery (PA) was severely dilated (diameter: 42 mm) and later was visualized to be immediately adjacent to the takeoff of the left main coronary artery (LMCA). During a 6-minute walk test, the patient developed severe tightness around the chest after a 5-m walk and was unable to complete the test. An acute 12-lead electrocardiogram (ECG) showed ST segment depression in the inferior and the anterolateral leads compared with the resting 12-lead ECG (Fig. 1).
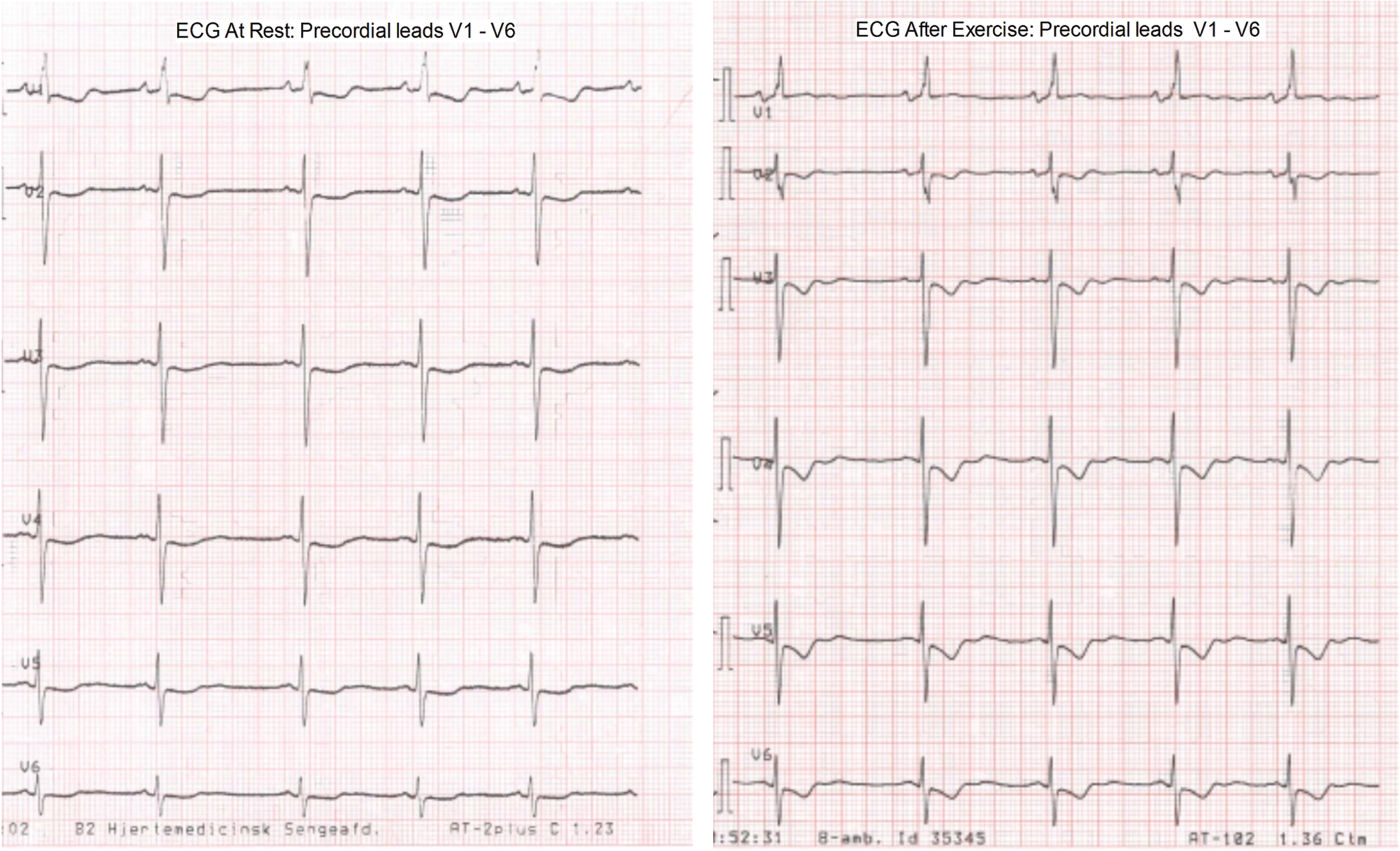
Twelve-lead electrocardiogram (ECG) at rest (
Coronary arteriography was performed from the right femoral artery and demonstrated a severe ostial LMCA stenosis (Fig. 2). The LMCA originated from a high position in the left sinus of the aortic root. There were no other atherosclerotic changes or stenosis of the coronary arteries. Intravascular ultrasound (IVUS) showed that the ostium of the LMCA was narrowed to a slit without evidence of underlying atherosclerosis. Cardiac computed tomography (ECG-gated multidetector computed tomography [MDCT]) confirmed a relatively high origin of the LMCA and a slit-like compression of the ostial part of the LMCA caused by a severely dilated PA trunk (Fig. 3).
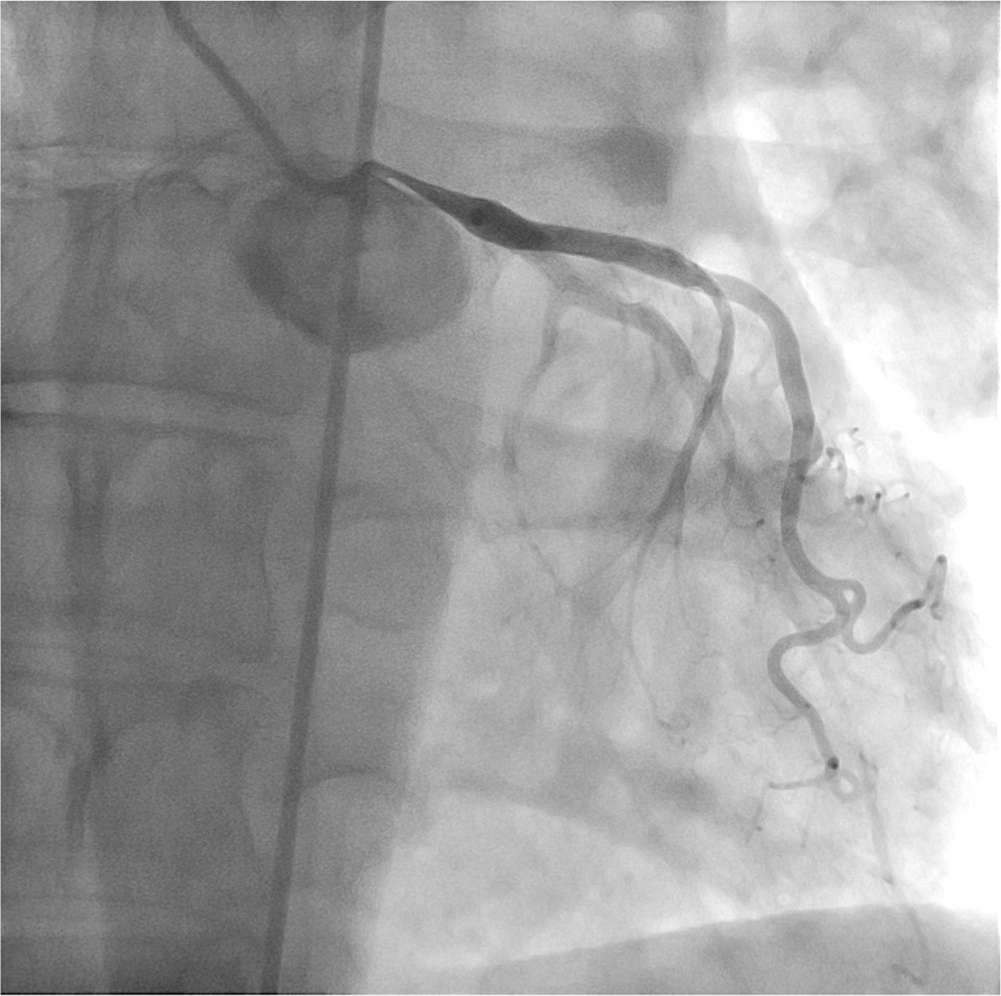
Coronary angiography demonstrating 90% stenosis of the ostium of the left main coronary artery (LMCA). Additionally, highly positioned LMCA from the left sinus of the aortic root was also observed, but no other atherosclerotic changes were found.
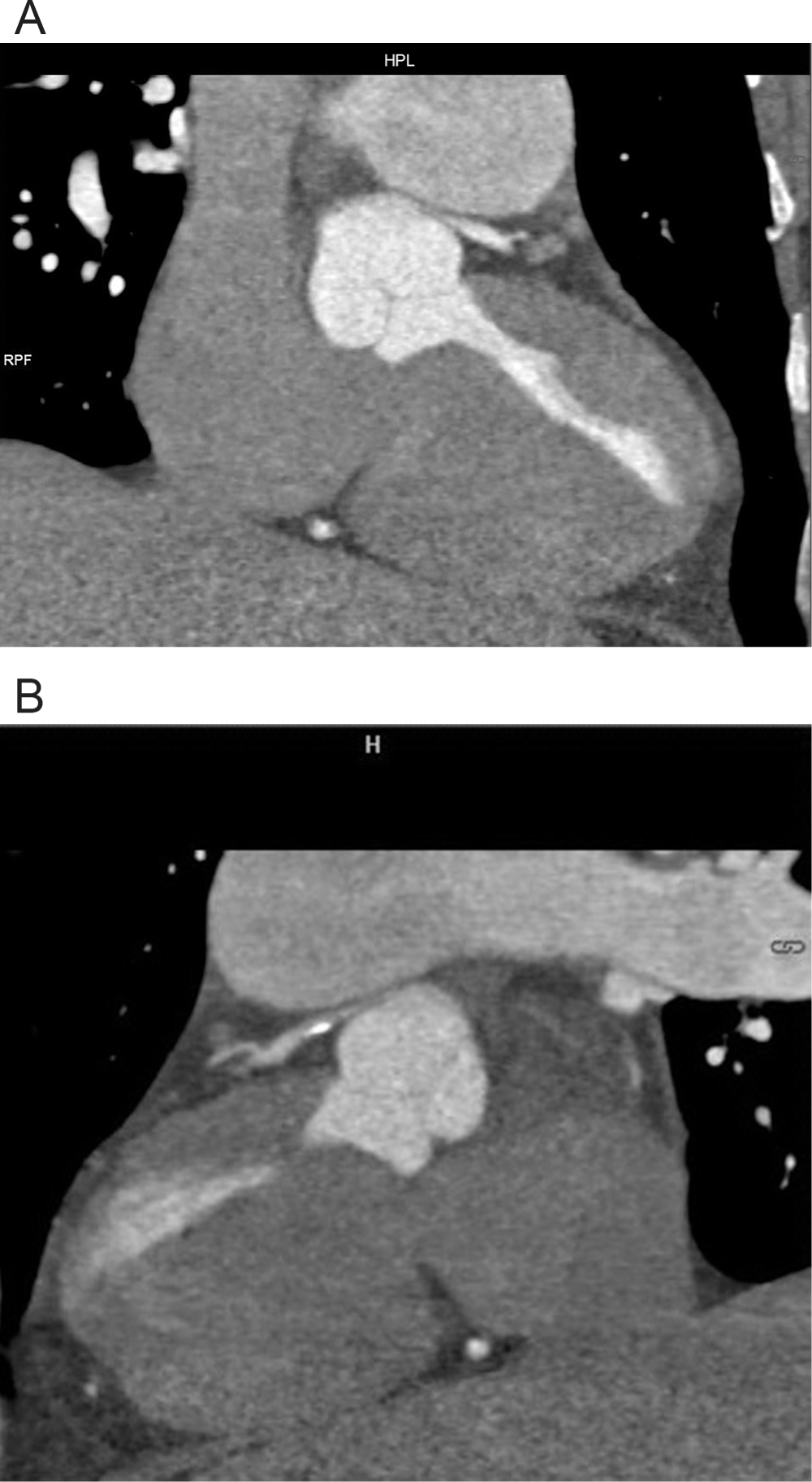
Computed tomography coronary angiography (
The patient underwent uncomplicated percutaneous coronary intervention (PCI) with implantation of a drug-eluting stent in the LMCA. Her symptoms completely resolved after the PCI. She performed a 6-minute walk test with a distance of 390 m 1 day after the PCI and did not experience any chest pain. Right-sided catheterization 1 day before discharge from the hospital confirmed the severity of the patient IPAH as diagnosed in 2008. It showed an atrial pressure of 5 mmHg, pulmonary capillary wedge pressure of 12 mmHg, mean pulmonary pressure of 58 mmHg, cardiac output of 3.8 L/minute, cardiac index of 1.95 L/minute/m2, and pulmonary vascular resistance of 15 Wood units.
DISCUSSION
Chest pain is one of the common manifestations in patients with PH. 1 The well-known explanation for chest pain in PH is RV hypertrophy and strain leading to demand ischemia. 2 Therefore, the development of chest pain in PH may often be a consequence of worsening PH and increased RV strain, as also initially suspected in this case. However, LMCA extrinsic compression due to a dilated main PA is another very important cause of exercise-related chest pain in PH, as finally concluded in our patient. Overlooking this mechanism of chest pain in PH may have serious consequences.
LMCA extrinsic compression due to a dilated PA has been reported previously. The clinical presentation may include exercise-related chest pain, cardiogenic shock, malignant arrhythmias due to myocardial ischemia, or sudden death. 3 The incidence of LMCA compression due to PA dilatation is not well known but ranges between 5% and 44%, according to different case series.4,5
In contrast to atherosclerotic coronary artery disease, which is more common in elderly males, extrinsic LMCA compression appears to affect younger people and may have a higher incidence in women. 6 Because of a low pretest probability for atherosclerotic coronary artery disease in young PH patients, coronary angiography is rarely performed. However, the extrinsic compression of the LMCA due to an enlarged PA is becoming increasingly recognizable and should always be considered in PH patients with exercise-induced chest pain, which is the most common clinical presentation of this problem.7,8 In one study, the origin of the LMCA from the right sinus of Valsalva was considered to convey a higher risk for extrinsic compression compared with the normal origin from the left sinus. 6 In another study, risk factors predisposing to LMCA compression in PAH were younger age, severe pulmonary trunk dilatation (>40 mm; normal: 25–30 mm), and a PA trunk/aorta ratio >1.2 (normal: 1.0). 5
Our case demonstrates that a high origin from the left coronary sinus may possibly be another risk factor for LMCA compression due to a steeper and more angled takeoff of the LMCA from the left sinus. In patients with known PAH who present with newly developed severe anginal pain during exercise, extrinsic LMCA compression from a dilated PA should be considered in the differential diagnosis. MDCT is excellent for confirming the diagnosis in such cases and may serve as the first-line diagnostic examination. Coronary angiography, IVUS, and myocardial perfusion methods to detect myocardial ischemia may play supplementary roles in the diagnostic evaluation. The treatment of LMCA extrinsic compression from a dilated PA in PAH is feasible and safe by PCI, and this has now become the most accepted treatment. 9
