Abstract
Pulmonary artery dissection is a complication associated with pulmonary arterial hypertension. This complication is described as acute in onset and is frequently fatal without intervention. We describe a patient with idiopathic pulmonary arterial hypertension and chest pain found to have an unsuspected chronic pulmonary artery dissection on postmortem examination. Chronic pulmonary artery dissection should be considered in patients with chest pain and worsening dyspnea, as the frequency this condition may be underestimated.
Pulmonary artery hypertension (PAH) is a progressive, life-threatening condition associated with symptoms that become more prevalent with disease progression.1,2 In patients with PAH, the cause of chest pain is unclear but is commonly attributed to myocardial ischemia.3–6 However, acute pulmonary artery dissection is also associated with new-onset chest pain, often with fatal outcomes.7,8 We describe a patient who had progressively worsening idiopathic PAH and chest pain, which resolved after initiation of intravenous prostaglandin analog therapy, and was found to have had acute and chronic pulmonary artery dissections on postmortem examination.
CASE DESCRIPTION
A 56-year-old female with idiopathic PAH diagnosed 11 years earlier and treated with nifedipine, bosentan (Tracleer, Actelion, San Francisco), sildenafil (Revatio, Pfizer, New York), inhaled iloprost (Iloprost, Actelion, San Francisco), and warfarin presented with 2 weeks of severe, intermittent chest pain. Chest pain was sharp and nonradiating, located over the left anterior chest, lasting 20–60 minutes, and aggravated with exertion or deep inspiration. This pain was unrelieved by antacids and partially relieved by oxygen and rest. Physical examination revealed a pulse rate of 100/minute, blood pressure of 130/70 mmHg, and pulse oximetry of 96% (with oxygen administered at 2 L/min). Chest auscultation revealed clear lung fields, a 3/6 systolic murmur, and no pericardial rub. No chest wall tenderness was elicited. Ascites was absent, and lower-extremity edema was present. Initial and subsequent electrocardiographs during episodes of chest pain revealed tachycardia without ischemic changes. Concomitant serum troponin levels were normal. A single-photon emission computed tomography (CT) myocardial perfusion test with adenosine did not demonstrate perfusion defects. Echocardiography showed right ventricle enlargement, right ventricular systolic pressure of 60 mmHg, and a small pericardial effusion. Chest CT demonstrated no vascular filling defects, and the pulmonary artery diameter (6.8 cm) was greater than that from a chest CT obtained 1 year earlier (5.7 cm). Right heart catheterization was performed and, relative to earlier studies, demonstrated a declining hemodynamic profile (Table 1). The patient agreed to parenteral prostacyclin therapy, and intravenous treprostinil (Remodulin, United Therapeutics, Silver Spring, MD) was initiated. As the treprostinil infusion was increased, she experienced significant improvements in exercise tolerance and resolution of chest pain. Four months after treprostinil initiation, while receiving 35 ng/kg/min, her 6-minute walk distance improved by 200 feet, to 1,150 feet. Right heart catheterization demonstrated an improved hemodynamic profile (Table 1). Weeks later, while attending a family function, she and her spouse developed fever, cough, and myalgias after contact with a sick child. The spouse's symptoms resolved, but she was hospitalized for dyspnea. Chest CT revealed parenchymal infiltrates, pericardial effusion, and no pulmonary artery dissection. Echocardiography revealed a moderate-sized pericardial effusion with right ventricular collapse. Forty-eight hours later, atrial fibrillation developed, and respiratory failure progressed, requiring mechanical ventilation and vasopressors. Drainage of 800 mL of sterile, serous, pericardial fluid provided hemodynamic improvement. However, respiratory failure persisted, and after 7 days, her family requested withdrawal of care. Permission to perform an autopsy was granted.
Right heart catheter measurements
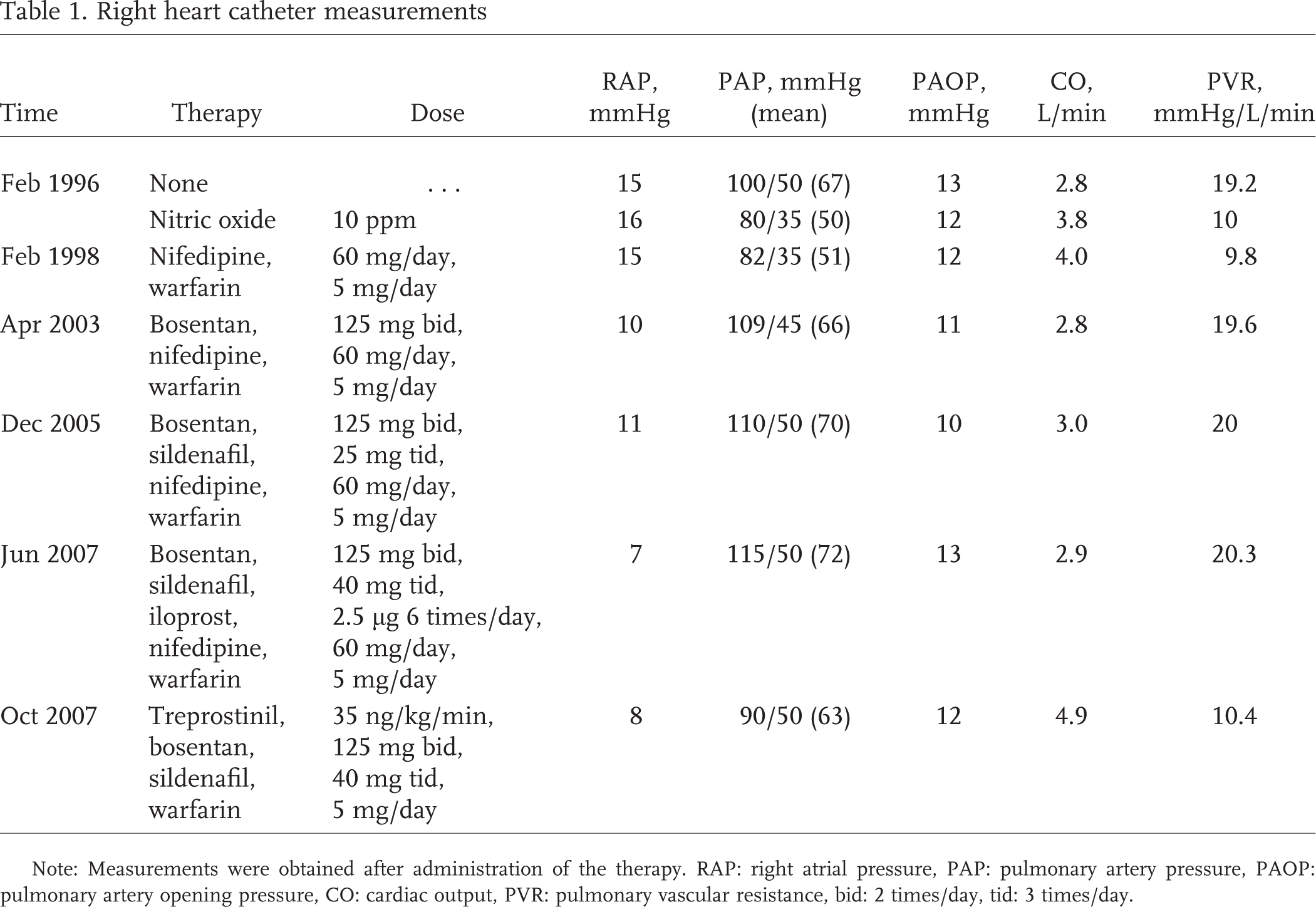
Note: Measurements were obtained after administration of the therapy. RAP: right atrial pressure, PAP: pulmonary artery pressure, PAOP: pulmonary artery opening pressure, CO: cardiac output, PVR: pulmonary vascular resistance, bid: 2 times/day, tid: 3 times/day.
Postmortem examination demonstrated right ventricular hypertrophy with patent coronary arteries, no evidence of recent or healed myocardial infarction, and normal pericardium. Bilateral parenchymal consolidation was noted, and Pseudomonas aeruginosa was isolated from the lung. No pulmonary emboli were identified. The pulmonary trunk measured 15 cm in greatest circumference. Within the main pulmonary artery, 8 intimal tears were observed, with the largest measuring 9 cm in length (Fig. 1). Microscopic examination of the pulmonary artery revealed an acute intimal tear and several well-healed tears, with organized collagen and vascular smooth muscle cell remodeling (Fig. 2). Pulmonary arterioles revealed intimal proliferation, medial thickening, concentric laminar fibrosis, and plexiform lesions. No organisms were identified on smear or culture from the pericardial fluid.
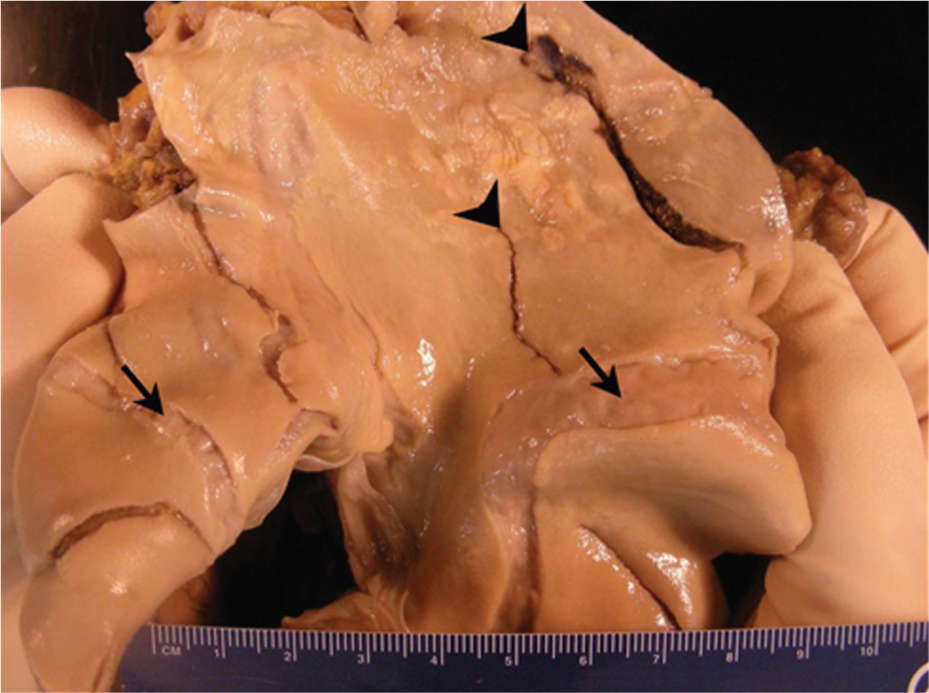
The main pulmonary arterial trunk opened to display massive aneurysmal dilatation of the pulmonary artery and multiple pulmonary artery tears (pulmonic valve is at lower left). The largest disruption (arrowhead, right) begins adjacent to the pulmonic valve and is 9 cm in length and 1.3 cm in greatest width. Note the interconnected nature of healed tears (arrows) and acute tears (arrowheads). Atherosclerotic plaques are also evident, indicative of long-standing pulmonary hypertension.
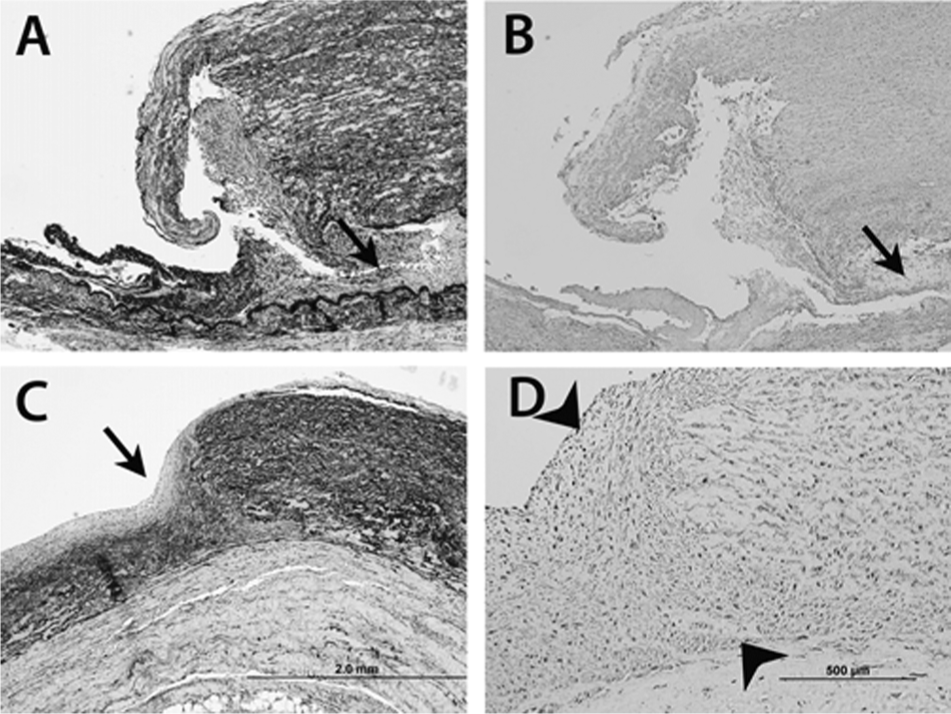
Photomicrographs of main pulmonary arterial wall, which is greatly thickened.
DISCUSSION
At time of diagnosis, chest pain occurs in 22%–47% of patients with PAH.1,2 Chest pain is often ascribed to right ventricular ischemia associated with normal coronary anatomy or left main coronary artery compression.3–6 However, pulmonary vascular conditions such as pulmonary artery dissection or pulmonary embolism are also associated with chest pain. Symptoms associated with pulmonary artery dissection include chest pain, fatigue, and progressive dyspnea. Notably, several reports describe acute onset of chest pain followed by cardiovascular collapse and death.7–9 Pathologic inspection of the pulmonary artery frequently reveals dilatation with an acute transmural tear and dissection into the mediastinum or pericardium.9,10 However, clinical and pathological description of chronic pulmonary artery dissection has not been well described. Clinical reports have described symptomatic pulmonary artery enlargement of weeks and months duration with poor outcomes but without pathologic description of the pulmonary vasculature.11,12 A report by Butto and colleagues 10 of pulmonary artery aneurysms describes features similar to our case: well-demarcated intimal lesions that under microscopy revealed neointima formation and healing of a previous dissection. This report indicates that pulmonary artery dilatation can lead to intimal injury, followed by healing noted by organizing collagen and vascular smooth muscle cells along the healed dissection site. In the case of this patient, we suspect that chest pain was related to right ventricular ischemia and chronic pulmonary artery dissection that resolved with initiation of treprostinil. Moreover, the findings of recent and healed intimal tears of the pulmonary artery indicate that large-vessel remodeling in the form of organized collagen and neointimal formation had occurred weeks to months before her death. Although fatal, acute pulmonary artery dissection has been previously reported, subclinical disease may also exist, manifested as recurrent or intermittent chest pain, as noted in the present case. With increasing survival for patients with PAH, complications such as pulmonary artery dissection may become more common. Moreover, since postmortem examination is frequently not performed, the frequency of chronic pulmonary artery dissection may be underestimated.
