Abstract
Right ventricular (RV) function is a strong predictor of outcome in cardiovascular diseases. Two components of RV function, longitudinal and transverse motion, have been investigated in pulmonary hypertension (PH). However, their individual clinical significance remains uncertain. The aim of this study was to determine the factors associated with transverse and longitudinal RV motion in patients with PH. In 149 treatment-naive patients with PH and 16 patients with suspected PH found to have mean pulmonary arterial pressure of <20 mmHg, cardiovascular magnetic resonance imaging was performed within 24 hours of right heart catheterization. In patients with PH, fractional longitudinal motion (fractional tricuspid annulus to apex distance [f-TAAD]) was significantly greater than fractional transverse motion (fractional septum to free wall distance [f-SFD];
Right ventricular (RV) dysfunction is considered a key determinant of adverse outcomes in several cardiopulmonary disease states. RV dilatation1–3 and progressive reduction in RV ejection fraction (RVEF) predicts mortality in patients with pulmonary arterial hypertension (PAH).1,3 In addition, RV dysfunction predicts mortality in patients following myocardial infarction4,5 and in nonischemic cardiomyopathy. 6
The transverse and longitudinal components of RV function have been studied previously in patients with pulmonary hypertension (PH).7,8 However, there are conflicting data regarding the importance of transverse and longitudinal shortening in relation to global RV function in PH. Longitudinal shortening measured using tricuspid annular plane systolic excursion (TAPSE) has been shown to be a strong predictor of adverse outcomes in patients with PH,9,10 and it has been postulated that longitudinal motion, rather than transverse motion, is the main determinant of RVEF in both healthy subjects and patients with PH. 8 In direct contrast, Kind et al. 7 demonstrated a stronger association between transverse RV motion and RVEF than between longitudinal RV motion and RVEF in patients with PH. Moreover, Mauritz et al. 11 identified transverse RV motion to be a stronger determinant of adverse outcomes in patients with severe PAH, with the floor effect of longitudinal motion masking end-stage RV decline. Longitudinal and transverse RV motion are both likely important markers of disease severity; however, their association with invasive hemodynamic, cardiac volumetric, and functional magnetic resonance imaging (MRI) measurements as well as their clinical significance remain unknown.
The aim of this study was to determine the covariate factors associated with transverse and longitudinal RV motion in patients with PH.
METHODS
Patients
Consecutive treatment-naive patients undergoing right heart catheterization (RHC) and MRI for suspected PH were identified over a 2-year period at a PH referral center from the ASPIRE (Assessing the Spectrum of Pulmonary Hypertension Identified at a Referral Centre) registry. 12 Inclusion criteria required that the patients’ RHC and MRI be performed within 48 hours after admission. Patients were excluded if the imaging was of nondiagnostic quality. Approval for retrospective analysis of imaging techniques was granted by the local research ethics committee.
MRI acquisition
MRI was performed on a 1.5-T whole-body scanner (GE HDx; GE Healthcare, Milwaukee, WI), using an 8-channel cardiac coil. Fourchamber and short-axis cine images were acquired using a cardiac gated multislice balanced steady-state free precession sequence (20 frames per cardiac cycle; slice thickness: 8 mm; field of view: 48; matrix: 256 × 256; bandwidth: 125 KHz/pixel; repetition time/echo time: 3.7/1.6 ms). A stack of images in the short-axis plane with slice thickness of 8 mm (2-mm interslice gap) were acquired fully covering both ventricles from base to apex. We corrected our MRI parameters where appropriate for body surface area (BSA), as reported elsewhere in the literature. 1
Image analysis
Image analysis was performed on a GE Advantage Workstation 4.1 by a pulmonary vascular radiologist (AJS) who was masked to patient clinical information and cardiac catheter parameters. A second observer analyzed 40 patients at random to assess interobserver agreement. Patients’ scans were defined as nondiagnostic when image quality significantly affected cardiac measurements or volumetric analysis could not be accurately performed.
RV volume and function
Endocardial surfaces were manually traced from the stack of short-axis cine images using our MRI workstation software (GE Advantage Workstation ReportCard) to obtain RV end-diastolic (RVEDV) and end-systolic (RVESV) volumes. From these, the RVEF was calculated as RVEF = (RVEDV - RVESV)/RVEDV.
Longitudinal RV motion was assessed using TAPSE, a measurement previously evaluated using echocardiography and MRI.7,9,13 TAPSE was calculated manually from the change of the tricuspid annulus to apex distance between end-diastolic and end-systolic four-chamber images. Fractional measure of longitudinal motion utilized the tricuspid annulus to apex distance change (f-TAAD) and was calculated as TAPSE divided by the tricuspid annulus to apex dimension at end diastole expressed as a percentage. This method has been described elsewhere by Kind et al. 7
Transverse RV motion was determined from the change in the septum to free wall perpendicular distance (SFD) on the four-chamber images. As described elsewhere by Kind et al., 7 lines were drawn between the tricuspid annulus and the apex and between the mitral annulus and the apex. The line intersecting the midpoints of these two lines defines the transverse axis of the heart. Septum to free wall dimensions followed this intersecting line (Fig. 1). SFD was measured manually as the change between the SFD at end diastole and the SFD at end systole. Fractional SFD (f-SFD) was calculated as for fractional longitudinal motion. 7
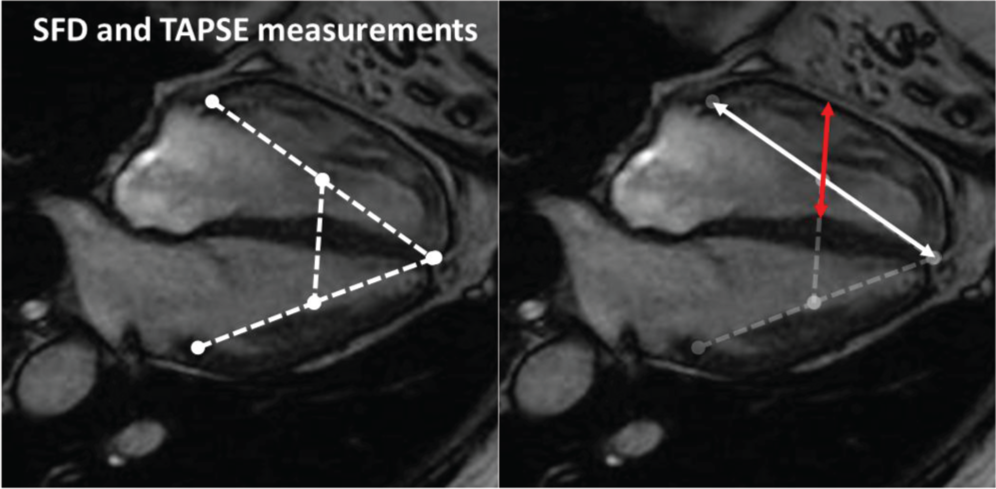
Four-chamber images from a patient with mild pulmonary hypertension showing tricuspid annulus to apex distance (TAAD) measurements (right image, white line) and septum to free wall distance (SFD) measurements (right image, red line).
Left ventricular (LV) eccentricity
LV eccentricity measurements have been traditionally expressed as the ratio of the length of two LV perpendicular minor-axis diameters. Systolic eccentricity index (sEI) measurements were obtained from the midchamber short-axis end-systolic image, and the ratio was calculated by the formula sEI = D2/D1, where D2 is the diameter parallel to the interventricular septum (IVS) and D1 is the diameter perpendicular to it. Abnormal values derived from echocardiography are considered to be >1.2. 14 Diastolic eccentricity index (dEI) was also calculated.
RV mass index and ventricular mass index (VMI)
The RV epicardial and endocardial borders on each end-diastolic short-axis slice image were outlined. The IVS was considered part of the LV. The myocardial volume for each slice was calculated by multiplying the area of the RV wall by the slice thickness. The product of the sum total of the myocardial slice volumes for each ventricle and the density of myocardium (1.05 g/cm 3 ) gave an estimate of RV mass.15,16 The LV epicardial and endocardial borders on each end-diastolic short-axis slice were outlined, and LV end-diastolic mass was derived as described above. VMI was defined as RV mass divided by LV mass.
RHC, echocardiography, and clinical evaluation
RHC was performed using a balloon-tipped 7.5-Fr thermodilution catheter (Becton Dickinson, Franklin Lakes, NJ). Patients referred for the investigation of suspected PH also underwent clinical evaluation, including blood testing, echocardiography, computed tomography scanning, lung function testing, incremental shuttle walk test (ISWT), exercise testing, and perfusion lung imaging. Diagnostic classification of the form of PH was done using standard criteria following multidisciplinary assessment. 17 Diagnostic classification was reached in accordance with standard criteria after multidisciplinary assessment by pulmonary vascular physicians and radiologists. Diagnosis was considered to occur at the time of the first RHC showing the presence of PH. Patients with Eisenmenger syndrome, in whom RHC is not routinely required, were excluded. 18 Echocardiography was performed by trained cardiac physiologists using Powervision 6000 and 8000 machines (Toshiba, Tokyo, Japan) as part of routine clinical care using a standard protocol for these patients. Multiple windows were used to obtain the optimal Doppler estimation of tricuspid regurgitant jet velocity (TRJV).
Clinical subgroup classification
To be classified as group 1 PAH, the pulmonary capillary wedge pressure (PCWP) at RHC was required to be ≥15. Pulmonary vascular resistance (PVR) was determined as follows: PVR = (mPAP - PCWP)/CO, where mPAP is mean pulmonary arterial pressure and CO is cardiac output. Patients with familial PAH or PAH in association with drug use were considered to have idiopathic PAH; this approach has been employed previously. 19 Patients with PH due to left heart disease (PH-LHD; group 2) were identified on the basis of echocardiographic and MRI assessment of LV and left atrium morphology and function, valvular sufficiency, left atrium size, and presence of LV hypertrophy in addition to PCWP. Patients with significant lung disease were subclassified accordingly as group 3. 20 Patients were classified as having no PH if mPAP was <20 mmHg at rest.
Statistics
Comparison of the longitudinal versus transverse RV function was made using a paired t test. Receiver operating analysis was used to identify optimal thresholds of f-SFD and f-TAAD for detecting low RVEF (defined as <40%). Univariate analysis of longitudinal and transverse motion on all variables of interest was performed in all patients using the Pearson correlation coefficient. Multiple linear regression was used to test longitudinal motion (f-TAAD) and transverse motion (f-SFD) on the variables found to be significant (at the
RESULTS
A total of 165 patients with suspected PH were identified, including 149 patients with PH, and 16 patients without PH (mPAP of <20 mmHg) were also included. Echocardiographic results were available for 125 patients with PH, and ISWT results were available for 134 patients. Clinical classifications, demographics, invasive hemodynamic results, and cardiac MRI results are presented in Table 1.
Demographic, right heart catheterization, and cardiac magnetic resonance imaging (MRI) data in patients with pulmonary hypertension (PH) and in those without PH
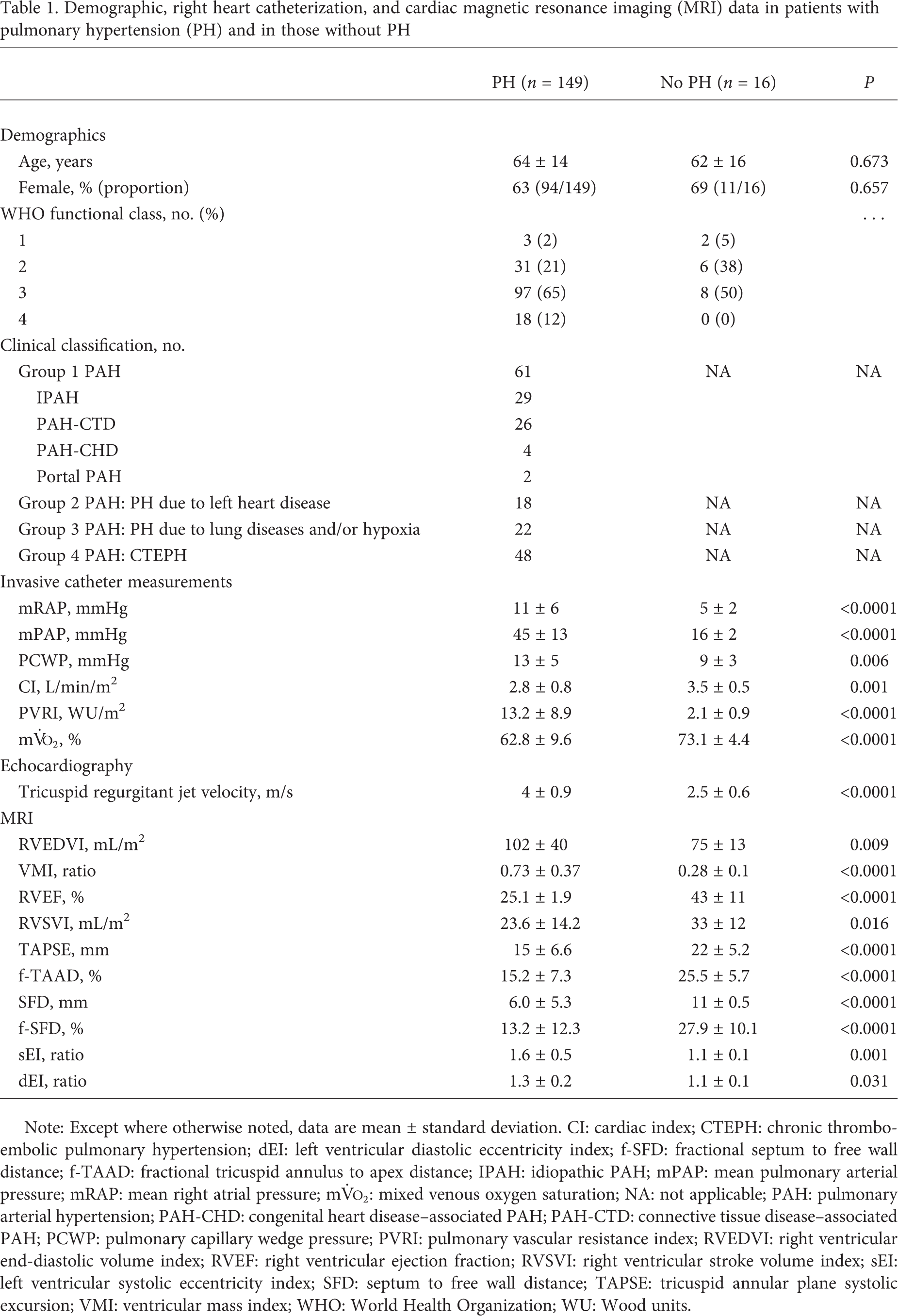
Note: Except where otherwise noted, data are mean ± standard deviation. CI: cardiac index; CTEPH: chronic thromboembolic pulmonary hypertension; dEI: left ventricular diastolic eccentricity index; f-SFD: fractional septum to free wall distance; f-TAAD: fractional tricuspid annulus to apex distance; IPAH: idiopathic PAH; mPAP: mean pulmonary arterial pressure; mRAP: mean right atrial pressure;
Comparison of longitudinal and transverse motion
In patients with PH, longitudinal RV measurements (TAPSE) were significantly greater than transverse motion (SFD) measurements; the mean difference was 9.4 mm (95% confidence interval: 8.4 – 1.0 mm;
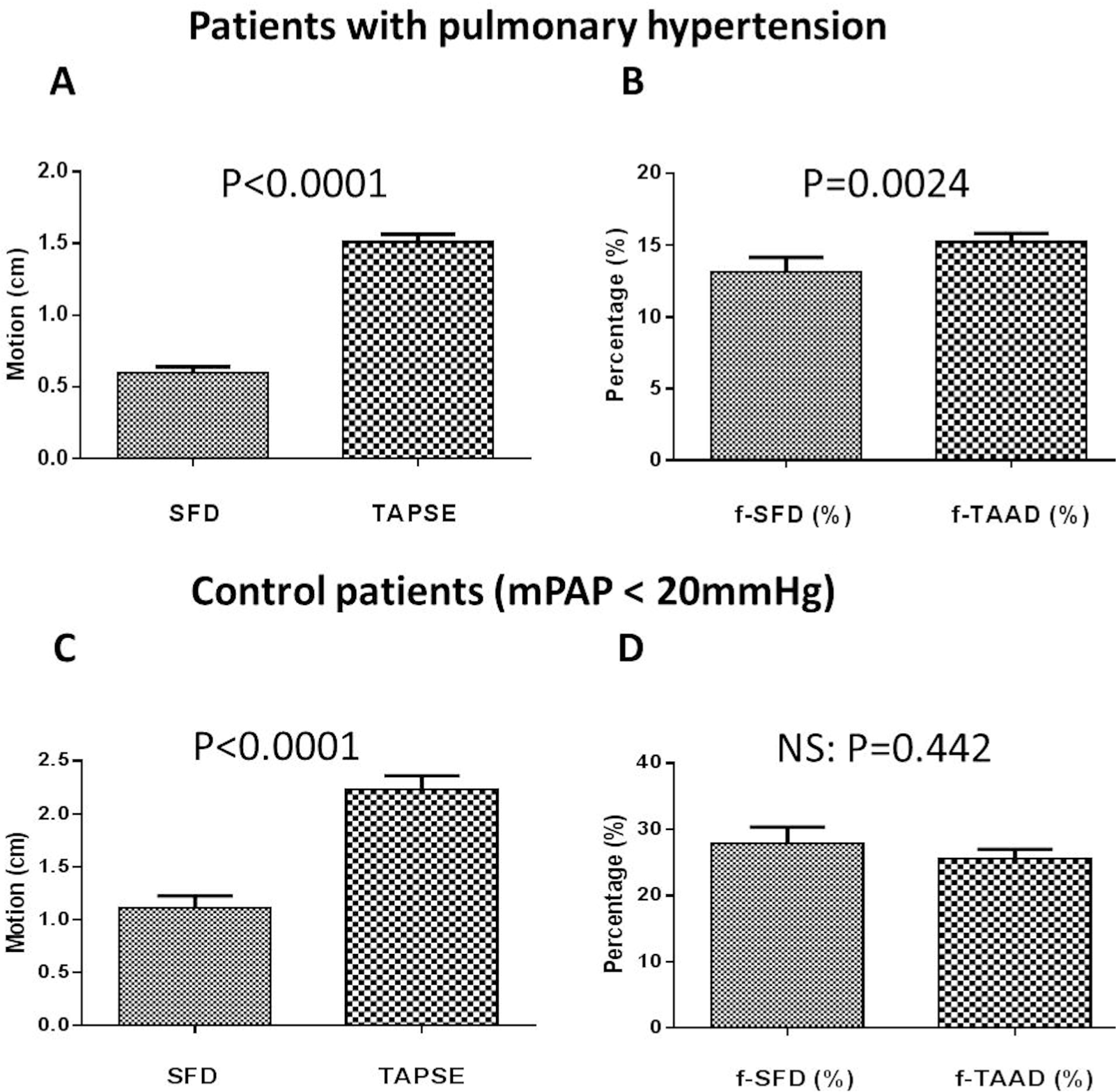
Comparison of transverse and longitudinal motion in patients with pulmonary hypertension (PH;
f-TAAD was significantly lower in men than in women (13% ± 5% vs. 17% ± 8%;
f-SFD (area under the curve [AUC]: 0.79) and f-TAAD (AUC: 0.83) showed similar accuracy for the detection of low RVEF (<40%), whereas SFD and TAPSE were less accurate for the detection of low RVEF (AUC: 0.67 and 0.76, respectively).
Univariate regression analysis
In univariate analysis, transverse motion as assessed by f-SFD was associated (
Correlations between transverse and longitudinal right ventricular motion parameters and covariate indexes in patients with pulmonary hypertension
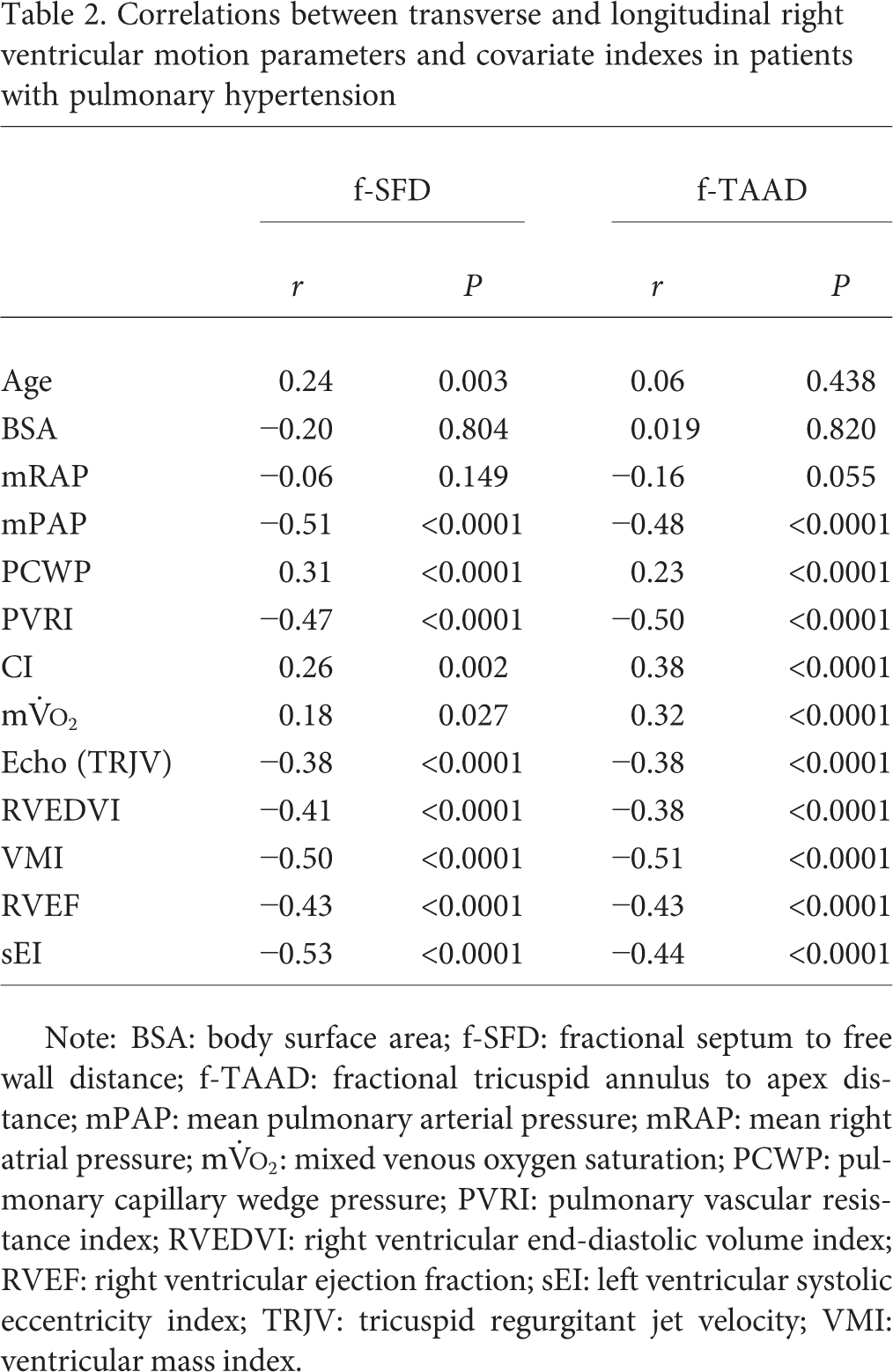
Note: BSA: body surface area; f-SFD: fractional septum to free wall distance; f-TAAD: fractional tricuspid annulus to apex distance; mPAP: mean pulmonary arterial pressure; mRAP: mean right atrial pressure;
In patients without PH, f-SFD and f-TAAD were associated only with RVEF (r = 0.40 and 0.38 [
Multivariate regression analysis
After multiple linear regression modeling of transverse motion (f-SFD) with significant covariates, RVEF (
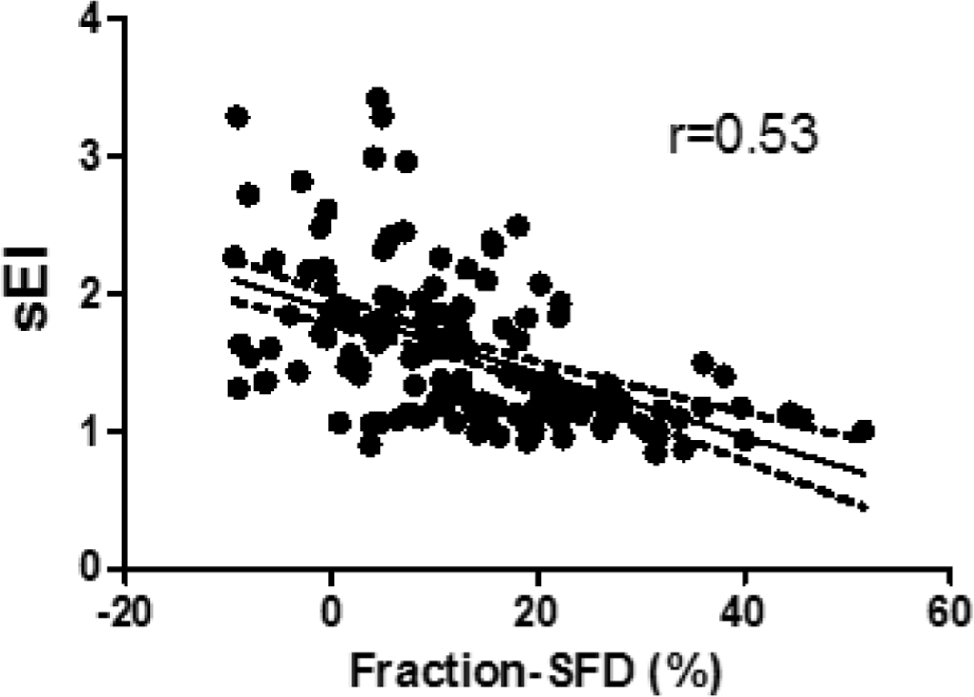
Scatterplot showing the association between fractional septum to free wall distance (SFD) and independent-covariates systolic eccentricity index (sEI).
In multivariate analysis of longitudinal motion (f-TAAD) versus significant covariates, f-TAAD was significantly associated with RVEF (
Multiple linear regression of longitudinal right ventricular function (fractional tricuspid annulus to apex distance) on covariate indexes
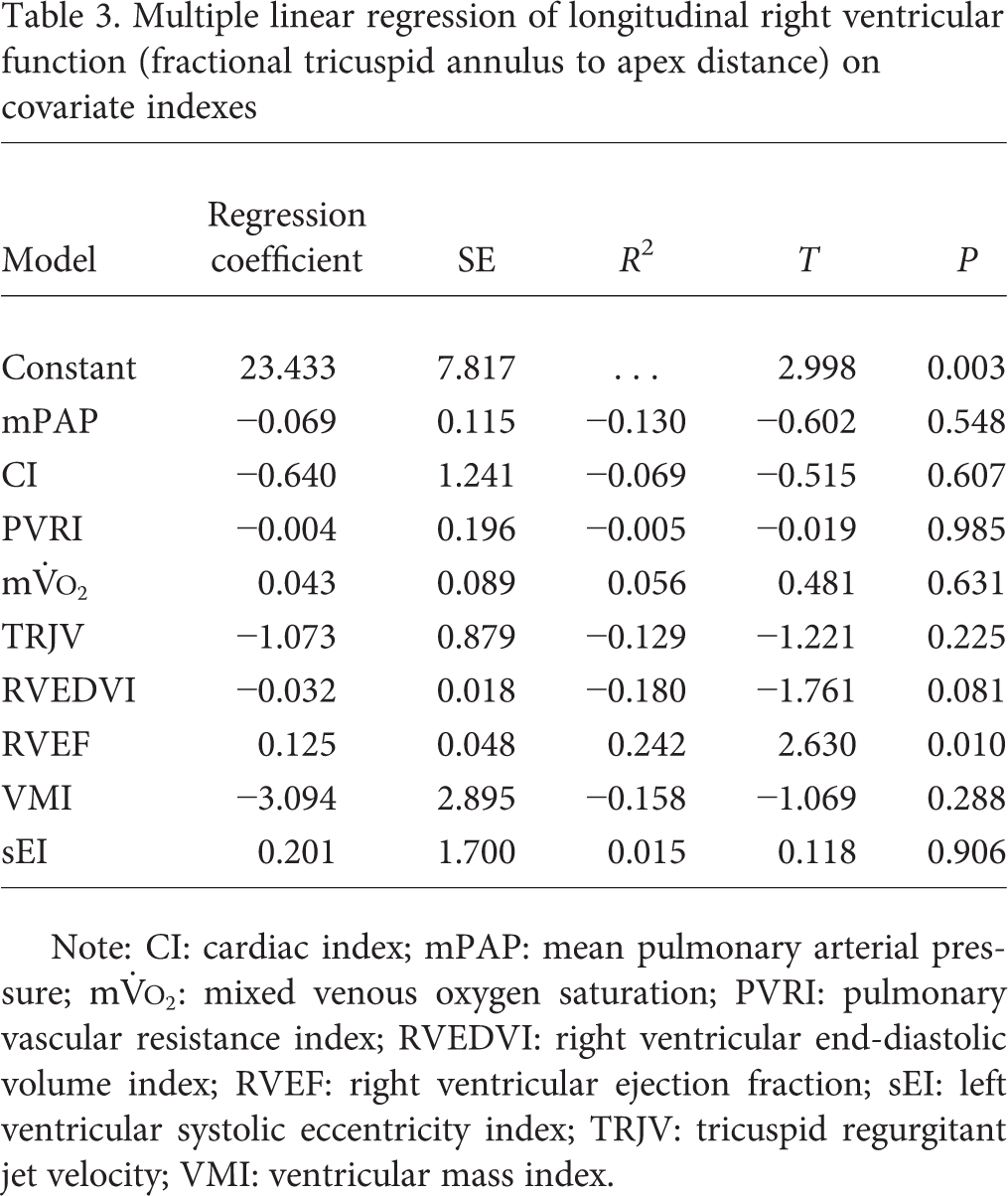
Note: CI: cardiac index; mPAP: mean pulmonary arterial pressure;
Multiple linear regression of transverse right ventricular function (fractional septum to free wall distance) on covariate indexes
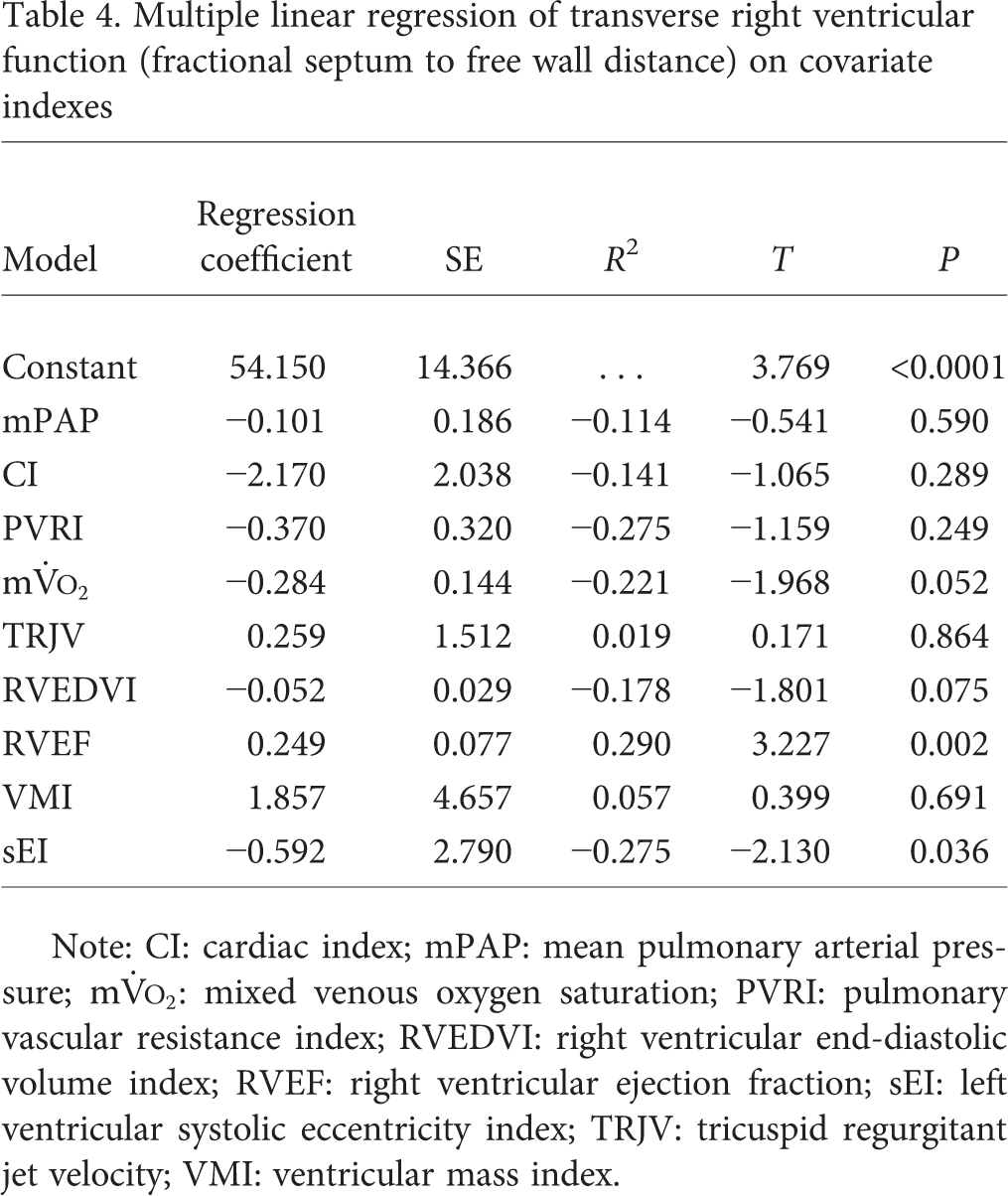
Note: CI: cardiac index; mPAP: mean pulmonary arterial pressure;
In subgroup analysis, sEI was the only variable independently linked to f-SFD in patents with PAH (
Reproducibility
Good reproducibility of SFD measurements was identified (bias: 0.01 cm; SD: 0.38), with limits of agreement of −0.7 to 0.7 cm. TAPSE measurements were similarly reproducible: the bias for TAPSE measurements was 0.1 cm (SD: 0.37), with narrow limits of agreement of −0.8 to 0.6 cm.
DISCUSSION
This study has shown that the association between RV longitudinal motion and ejection fraction is independent of demographic, hemodynamic, and cardiac MRI indexes in PH. In contrast, RV transverse verse motion is independently influenced by ventricular interaction measured by LV eccentricity and therefore is not solely associated with RVEF.
Brown et al. 8 have demonstrated that in healthy subjects longitudinal motion contributes approximately 80% of global RV function. In patients with PAH, selective recovery of longitudinal rather than transverse RV function was demonstrated with therapy. The authors concluded that longitudinal function is a more important contributor to ejection fraction than transverse function in PAH. Our study has also shown that in patients with PAH and CTEPH the magnitude of RV motion is significantly greater in the longitudinal direction than in the transverse direction, whereas the RV of patients without PH (mPAP of <20 mmHg) functions with equal contributions of transverse and longitudinal motion. Patients with PH-LHD and PH-RESP also had no difference in longitudinal and transverse motion. Patient numbers were smallest in these two groups, and thus failure to find significance may be the result of type II error. In addition, patients with PH-LHD do not tend to exhibit septal deviation as greatly, 16 as the pressure on the left side tends to be higher than that on the right throughout the cardiac cycle. In patients with PAH, PH-RESP, and CTEPH, transverse motion is independently linked to LV eccentricity; however, the same trend did not exist in patients with PH-LHD, similarly reflecting the lack of septal deviation in PH-LHD. Kind et al. 7 found that global RV function was more strongly associated with transverse RV motion than longitudinal RV motion in patients with PAH. The authors concluded that transverse RV motion may be a superior marker of RV dysfunction in PH.
The present study is the first to investigate transverse and longitudinal RV motion in terms of their associations with hemodynamic and cardiovascular MRI measurements. The findings demonstrate that both longitudinal and transverse RV motion measurements are independently associated with global RV function as measured by cardiovascular magnetic resonance–derived ejection fraction. The relationship lationship between longitudinal motion and global RV function is independent of all hemodynamic and imaging covariates. However, transverse RV motion is independently influenced by sEI, which is a measure of the effect of interventricular septal deviation on the LV. Patients without PH (mPAP of <20 mmHg) did not exhibit this trend. Both longitudinal and transverse motions were independently associated with global RV function, with no significant covariates identified. A recent echocardiography study has shown that, in patients with PH, reduced transverse RV function is a reliable indicator of the presence of high pulmonary arterial pressure, which is reflected in our data as transverse function and is influenced by LV eccentricity, a marker of disease severity in PH. 21 Second, the authors found, as we do in the present study, that reduced RV longitudinal function is more closely linked with impairment of cardiac function. 21 Mauritz et al. 11 showed that changes in transverse RV motion in severe PH were associated with increased risk of adverse outcomes. The authors suggested that a decline in transverse motion reflects progressive paradoxical interventricular motion in the later stages of the disease course. These findings are consistent with those of the present study, in which an independent association between LV eccentricity and transverse motion has been identified, and with those of previous studies showing the prognostic significance of LV eccentricity.10,22
Limitations
This was a single-center study. Technical limitations include difficulties defining the endocardium of the RV, and due to complex trabeculations of the free wall inaccuracies may occur in the measurement of SFD. Furthermore, transverse and longitudinal motion were measured manually from four-chamber images, which may not be fully representative of their relative contributions to RVEF. Modeling the contributions of transverse and longitudinal motion using isotropic three-dimensional imaging may improve accuracy.
Conclusions
The magnitude of RV motion is significantly greater in the longitudinal direction in patients with PH, whereas patients without PH have equal contributions of transverse and longitudinal motion. Longitudinal and transverse components of RV function are independently linked to global RV pump function measured by RVEF. However, transverse RV motion not only reflects global pump function but is independently influenced by ventricular interaction in PH.
Footnotes
ACKNOWLEDGMENTS
This article presents independent research funded by the NIHR. The views expressed are those of the authors and are not necessarily those of the National Health Service, the NIHR, or the Department of Health. JMW is also funded by the Engineering and Physical Sciences Research Council.
