Abstract
Riociguat, a soluble guanylate cyclase stimulator, is a novel therapy for the treatment of pulmonary hypertension. Riociguat bioavailability is reduced in neutral versus acidic conditions and therefore may be affected by concomitant use of medications that increase gastric pH. The effect of coadministration of the proton pump inhibitor omeprazole or the antacid AlOH/MgOH on the pharmacokinetics, safety, and tolerability of riociguat 2.5 mg was characterized in two open-label, randomized, crossover studies in healthy males. In study 1, subjects pretreated for 4 days with omeprazole 40 mg received cotreatment with omeprazole plus riociguat or riociguat alone (no pretreatment) on day 5 (n = 12). In study 2, subjects received cotreatment with 10 mL AlOH/MgOH plus riociguat or riociguat alone (n = 12). Pre- and cotreatment with omeprazole decreased riociguat bioavailability (mean decreases in area under the plasma concentration-time curve [AUC] and maximum concentration in plasma [Cmax] were 26% and 35%, respectively). Cotreatment with AlOH/MgOH resulted in greater decreases in riociguat bioavailability (mean decreases in AUC and Cmax were 34% and 56%, respectively). In both studies, most adverse events (AEs) were of mild intensity, and no serious AEs were reported. No additional safety signals were identified. Treatment with riociguat, with or without omeprazole or AlOH/MgOH, was well tolerated, with a good safety profile. Owing to the resulting increase of gastric pH, riociguat bioavailability is reduced by coadministration with AlOH/MgOH and, to a lesser extent, by coadministration with omeprazole. Thus, antacids should not be administered within an hour of receiving riociguat, but no dose adjustment is required for coadministration of proton pump inhibitors.
Keywords
Riociguat is the first member of a novel class of therapeutics called soluble guanylate cyclase stimulators that has recently been approved in several regions, including the United States, Canada, and Europe, for the treatment of pulmonary arterial hypertension (PAH), inoperable chronic thromboembolic pulmonary hypertension (CTEPH), and recurrent/persistent pulmonary hypertension (PH) after pulmonary endarterectomy (PEA), following positive phase 3 studies in these indications.1,2 Riociguat was rapidly absorbed, had high oral bioavailability, and showed dose-proportional pharmacokinetics in pharmacokinetic studies. 3 While no clinically relevant drug-drug interactions have been demonstrated between riociguat and supportive treatments used in PAH/CTEPH, including warfarin and aspirin,4,5 in vitro data indicated that the solubility of riociguat was higher under acidic conditions. 6 Thus, concomitant use of medicines that alter gastric pH, such as proton pump inhibitors and antacids, may alter the bioavailability of riociguat. The aim of these two clinical pharmacology studies was to investigate the influence of omeprazole and aluminum hydroxide/magnesium hydroxide (AlOH/MgOH) on riociguat absorption and bioavailability in healthy subjects.
METHODS
Study population
Healthy male subjects aged 18–45 years were eligible to participate in these studies if they had a body mass index of 18–30. Exclusion criteria included a resting heart rate of <45 or >90 bpm, systolic blood pressure (SBP) of <100 or >145 mmHg, diastolic blood pressure (DBP) of >95 mmHg, a positive drug screen, history or evidence of organ or central nervous system diseases, medical conditions that could impair the subject's ability to participate in or complete the study, febrile illness in the week before the study, and pathological changes in the electrocardiogram (ECG), such as second- or third-degree atrioventricular block, prolongation of the QRS complex to >120 ms, or prolongation of the QT/QTc interval to >450 ms. Furthermore, subjects could not be enrolled in the studies if they had used medication in the preceding 2 weeks that could interfere with riociguat or the interaction partner drugs, if they had a preexisting condition where use of omeprazole or AlOH/MgOH was contraindicated, or if they had participated in a clinical trial in the previous 3 months. Participants gave written informed consent to participate in the studies.
Study design
Healthy subjects received two treatments in two separate, single-center, randomized, open-label, non-placebo-controlled, 2-way crossover studies, conducted to assess the pharmacokinetic characteristics of oral single-dose, immediate-release riociguat 2.5-mg tablets, with or without omeprazole or AlOH/MgOH. The omeprazole study was carried out at the Pharma Center of Bayer Pharma, Wuppertal, Germany, between November 2006 and January 2007. The study protocol was approved by the Ethics Committee of the North-Rhine Medical Council, Dusseldorf. The AlOH/MgOH study was carried out at Bayer Schering Pharma, Clinical Pharmacology, Berlin, Germany, between January and May 2007. The study protocol was approved by the State Office for Health and Social Affairs Ethics Committee of the State of Berlin. Both studies were carried out in accordance with the Declaration of Helsinki, the International Conference on Harmonisation Good Clinical Practice Guidelines, European Union Directive 2001/20/EC, and the German Drug Law. Randomization was carried out after the prestudy examination.
Treatments
In the omeprazole study, treatment A consisted of a single riociguat 2.5-mg tablet given to fasted subjects. The total observation time for treatment A was 3 days. Treatment B consisted of 4-day pretreatment with once-daily oral omeprazole 40 mg (Antra MUPS, AstraZeneca, Wedel, Germany, 2 × 20-mg tablets), followed by cotreatment with omeprazole 40 mg plus riociguat 2.5 mg on day 5. The total observation period for treatment B was 5 days (including the 4-day pretreatment outpatient phase). A washout period of at least 72 hours after administration of the study drugs followed each treatment period.
In the AlOH/MgOH study, treatment A consisted of a single riociguat 2.5-mg tablet given to fasted subjects. Treatment B consisted of a single riociguat 2.5-mg tablet plus cotreatment with a single oral dose of 10 mL of AlOH/MgOH 7-mmol suspension (Maalox, Cassella-med, Cologne, Germany) given to fasted subjects. A washout period of at least 5 days after administration of the study drugs followed each treatment period. The total observation time for each treatment was 3 days, and subjects underwent a final examination 2 weeks after the second study period.
Drug plasma concentration analyses
In both studies, blood was collected before dose (0 hours) and at regular intervals thereafter up to 48 hours after dosing for the determination of plasma concentrations of riociguat and M1 (BAY 60-4552, the major metabolite of riociguat).
In the omeprazole study, riociguat and M1 in plasma concentrations were analyzed with high-performance liquid chromatography coupled with mass spectrometry (HPLC/MS), with [2H3]riociguat as the internal standard. The calibration range of the procedure was from 0.1 μg/L (riociguat) and 0.2 μg/L (M1), the respective lower limits of quantification (LLOQ), to 100 μg/L. Quality control samples in the concentration ranges 0.3–80 μg/L for riociguat and 0.6–80 μg/L for M1 were determined with an accuracy of 98.5%–104% and 93.6%–105% and a precision of 1.90%–13.2% and 2.91%–8.05%, respectively (n = 16 for both analytes). All samples were stored below −15°C and analyzed within 2 months after sampling.
In the AlOH/MgOH study, quantitative analysis of riociguat and M1 plasma concentrations was performed with HPLC/MS, with [2H3]riociguat as the internal standard. The calibration range was 0.5–100 μg/L for both analytes. Quality control samples in the concentration range 1.5–80 μg/L for both analytes were determined with an accuracy of 94.2%–102% for riociguat and 87.9%–104% for M1 and a precision of 4.99%–15.0% (riociguat) and 3.98%–10.4% (M1; n = 22 for both analytes). All samples were stored at or below −15°C and analyzed within 2 months after sampling.
Pharmacokinetic analysis
Riociguat and M1 plasma concentration—time data were used to calculate pharmacokinetic parameters including area under the plasma concentration—time curve (AUC0–∞), maximum concentration in plasma (Cmax), time to Cmax (tmax), terminal elimination half-life interval (t1/2), and total body clearance of drug from plasma (CL/f). These parameters were calculated with model-independent (compartment-free) methods in WinNonlin (ver. 4.1.a; Pharsight, Mountain View, CA), in conjunction with Automation Extension (Bayer). Plasma concentration-time courses of riociguat, calculated when at least two-thirds of the individual data were above the LLOQ, are presented as geometric-mean values.
Statistical analysis
Statistical analysis was performed with the SAS software package, version 9.1 (Cary, NC). AUC0–∞ and Cmax were analyzed under the assumption of lognormally distributed data. The logarithms of these characteristics were analyzed with analysis of variance (ANOVA) including sequence, subject (sequence), period, and treatment effects. On the basis of these analyses, point estimates (least squares means) and exploratory 90% confidence intervals for the ratios (omeprazole + riociguat) : riociguat and (AlOH/MgOH + riociguat) : riociguat were calculated by retransformation of the logarithmic data using the intraindividual standard deviation of the ANOVA. A confirmatory statistical analysis was not performed.
Safety and tolerability
Safety was assessed via ECGs, vital signs, clinical laboratory tests, and monitoring of treatment-emergent adverse events (TEAEs) at screening, before dosing for each treatment period, and at the conclusion of the study. Subjects were given a physical examination at screening in both studies and also at a follow-up visit at the conclusion of the AlOH/MgOH study. TEAEs were assessed for severity (mild, moderate, or severe) and relation to treatment and summarized with Medical Dictionary for Regulatory Activities—preferred terms (ver. 9.1 for the omeprazole study; ver. 10.0 for the AlOH/MgOH study).
RESULTS
Demographics
The characteristics of the healthy male subjects enrolled in both studies who were valid for pharmacokinetic analyses are shown in Table 1. Of the 12 subjects enrolled in the omeprazole study, all completed the study and were valid for pharmacokinetic and safety analyses. Of the 13 subjects enrolled in the AlOH/MgOH study, 12 completed the study and were valid for pharmacokinetic and safety analyses (1 was withdrawn because of an adverse event [AE], arrhythmia, before receiving any medication).
Demographics of healthy subjects who were valid for pharmacokinetic analyses in the omeprazole and AlOH/MgOH studies
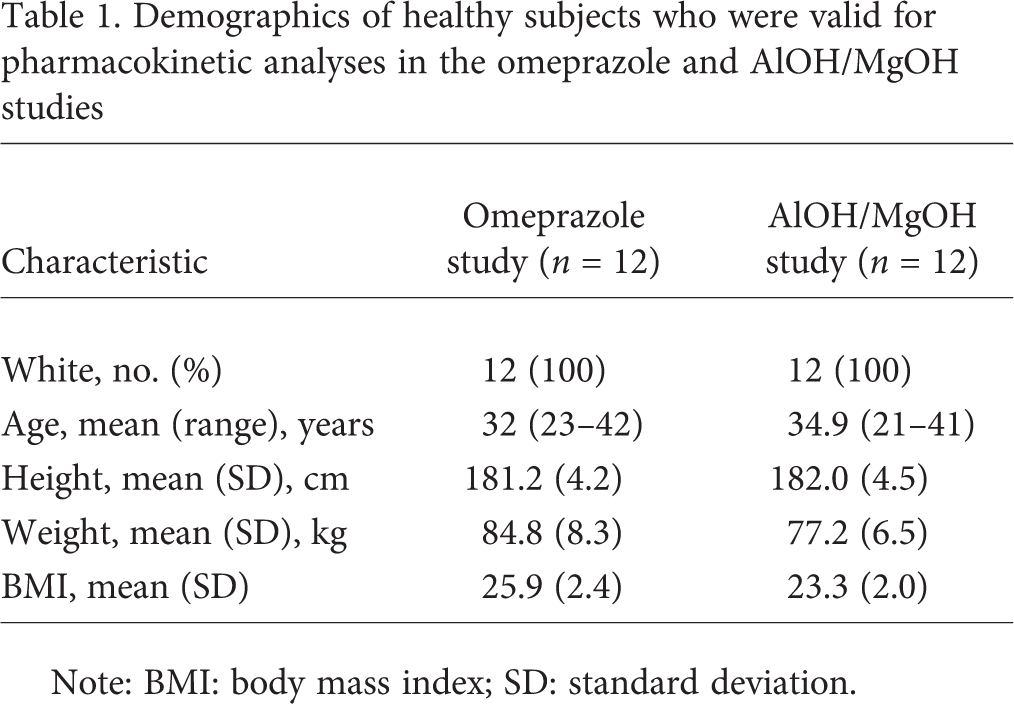
Note: BMI: body mass index; SD: standard deviation.
Pharmacokinetics
Pre- and cotreatment with omeprazole resulted in a reduction in riociguat bioavailability, with a geometric-mean AUC0–∞ decrease of 26% and a geometric-mean Cmax decrease of approximately 35% (Table 2; Fig. 1). Riociguat t1/2 increased from 7.9 to 9.0 hours, and CL/f increased from 4.3 to 5.8 L/h when riociguat was given concomitantly with omeprazole. Pre- and cotreatment with omeprazole had no effect on tmax (3.0 hours with and without omeprazole).
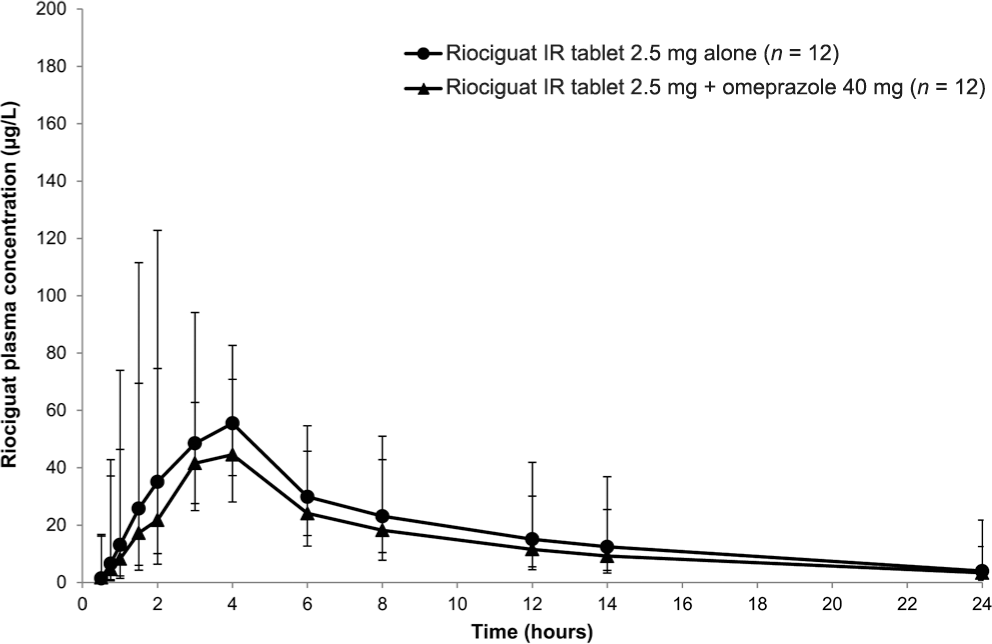
Plasma concentrations of riociguat after a single oral dose of riociguat 2.5 mg with and without pre- and cotreatment with once-daily omeprazole 40 mg (geometric means ± geometric standard deviation, linear scale; all subjects valid for pharmacokinetic analysis; n = 12). IR: immediate release.
Omeprazole study: pharmacokinetic parameters of riociguat following a single oral dose of riociguat 2.5 mg ± omeprazole 40 mg
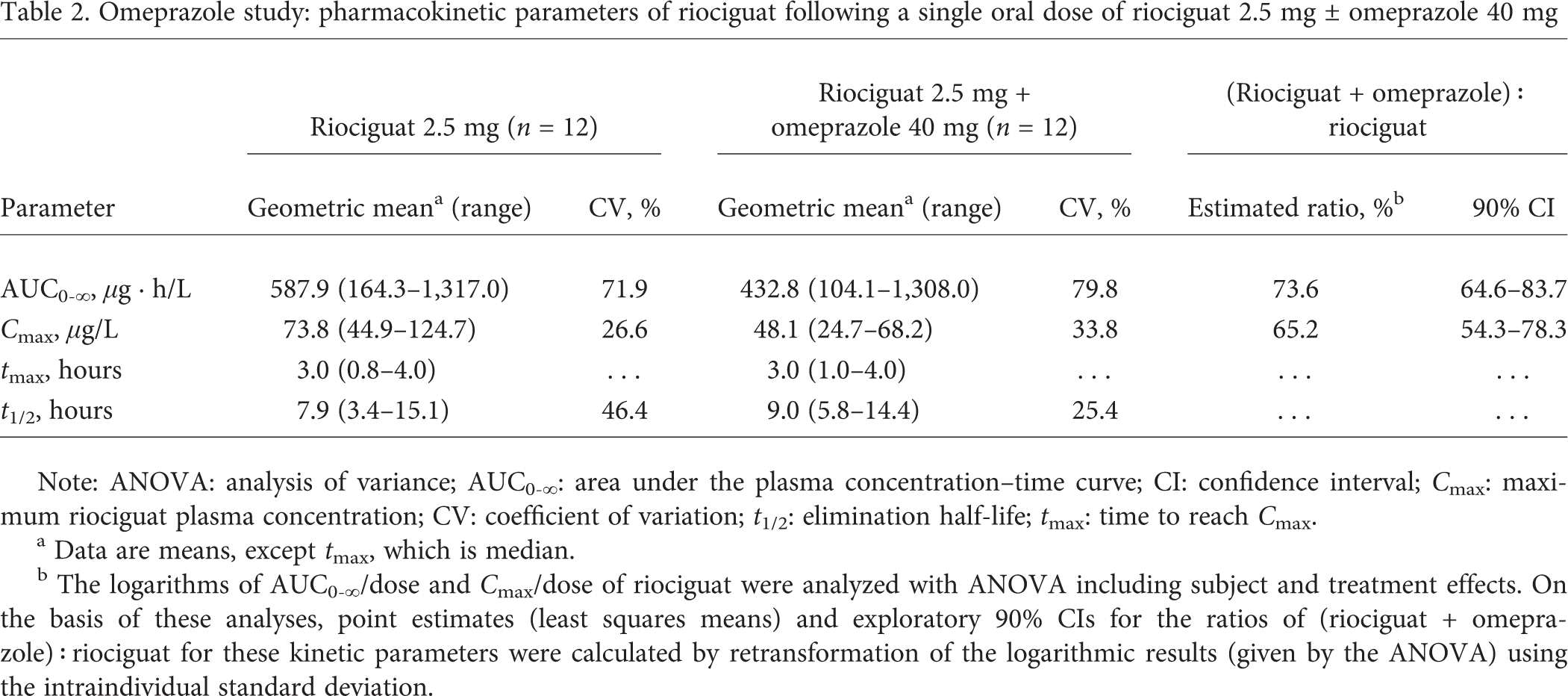
Note: ANOVA: analysis of variance; AUC0-∞: area under the plasma concentration-time curve; CI: confidence interval; Cmax: maximum riociguat plasma concentration; CV: coefficient of variation; t1/2: elimination half-life; tmax: time to reach Cmax.
Data are means, except tmax, which is median.
The logarithms of AUC0-∞/dose and Cmax/dose of riociguat were analyzed with ANOVA including subject and treatment effects. On the basis of these analyses, point estimates (least squares means) and exploratory 90% CIs for the ratios of (riociguat + omeprazole) : riociguat for these kinetic parameters were calculated by retransformation of the logarithmic results (given by the ANOVA) using the intraindividual standard deviation.
Pre- and cotreatment with omeprazole did not influence the bioavailability of M1, the main metabolite of riociguat, with mean Cmax and mean AUC0–∞ remaining almost constant (+7% and −3%, respectively). M1 t1/2 decreased slightly, from 14.2 to 13.6 hours, when riociguat was given concomitantly with omeprazole, and tmax decreased from 13 to 12 hours.
Pre- and cotreatment with AlOH/MgOH resulted in reduced bioavailability of riociguat, with a geometric-mean AUC0–∞ decrease of 34% and a geometric-mean Cmax decrease of approximately 56% (Table 3; Fig. 2). Riociguat t1/2 increased from 5.9 to 8.6 hours, and CL/f increased from 5.4 to 8.1 L/h when riociguat was given concomitantly with AlOH/MgOH (Table 3). Pre- and cotreatment with AlOH/MgOH increased tmax from 1 to 2.5 hours (Table 3).
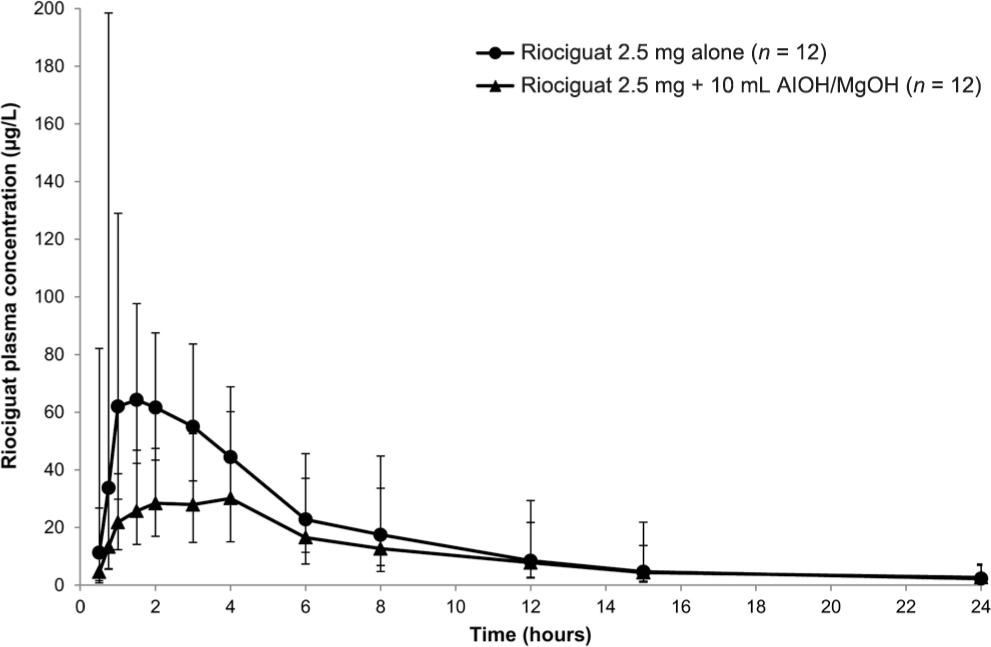
Plasma concentrations of riociguat after a single oral dose of riociguat 2.5 mg with and without coadministration of 10 mL AlOH/MgOH (geometric means ± geometric standard deviation, linear scale; all subjects valid for pharmacokinetic analysis; n = 12).
AlOH/MgOH study: pharmacokinetic parameters of riociguat following a single oral dose of riociguat 2.5 mg ± 10 mL 7-mmol AlOH/MgOH
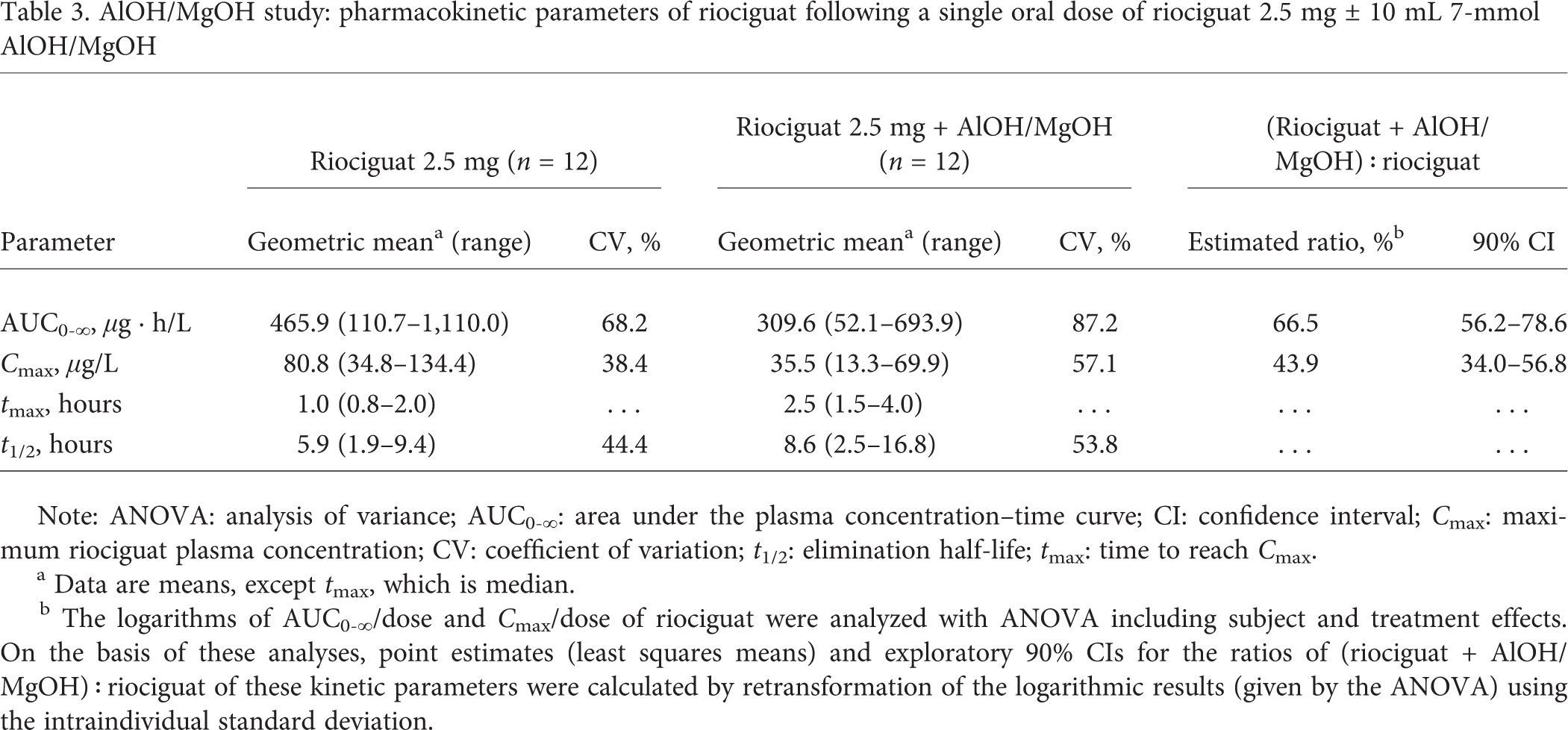
Note: ANOVA: analysis of variance; AUC0-∞: area under the plasma concentration-time curve; CI: confidence interval; Cmax: maximum riociguat plasma concentration; CV: coefficient of variation; t1/2: elimination half-life; tmax: time to reach Cmax.
Data are means, except tmax, which is median.
The logarithms of AUC0-∞/dose and Cmax/dose of riociguat were analyzed with ANOVA including subject and treatment effects. On the basis of these analyses, point estimates (least squares means) and exploratory 90% CIs for the ratios of (riociguat + AlOH/MgOH) : riociguat of these kinetic parameters were calculated by retransformation of the logarithmic results (given by the ANOVA) using the intraindividual standard deviation.
Coadministration of AlOH/MgOH led to reduced M1 bioavailability, with a mean Cmax decrease of approximately 44% and a mean AUC0–∞ decrease of 33%. In addition, M1 t1/2 increased slightly, from 12.2 to 14.2 hours, CL/f increased from 3.7 to 5.4 L/h, and tmax increased from 4 to 6 hours when riociguat was given concomitantly with AlOH/MgOH.
Safety and tolerability
Riociguat was well tolerated in both studies, and most AEs were of mild intensity and were as expected from the mechanism of action of riociguat. TEAEs for both studies are shown in Table 4.
Incidence of TEAEs in the two studies
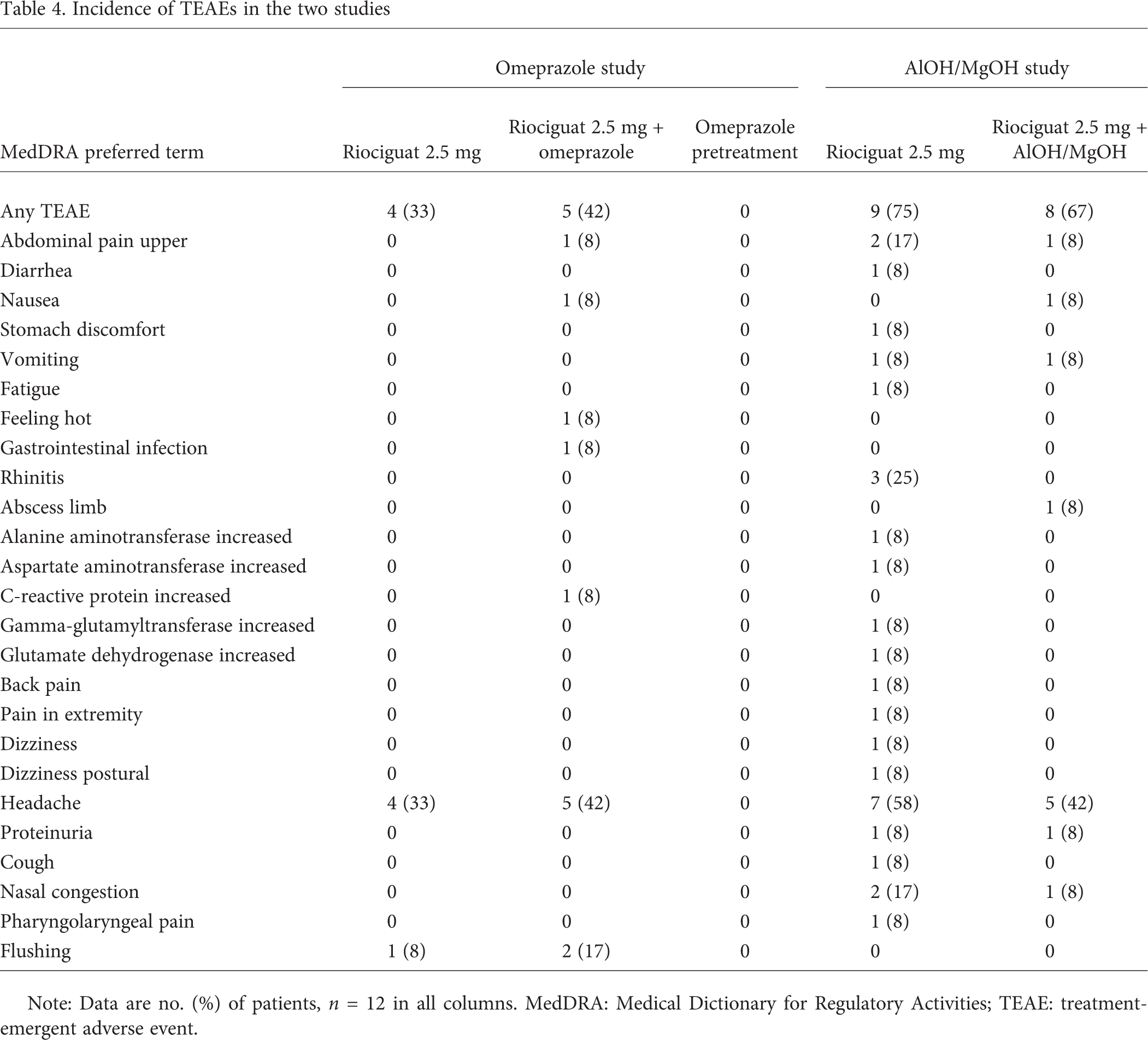
Note: Data are no. (%) of patients, n = 12 in all columns. MedDRA: Medical Dictionary for Regulatory Activities; TEAE: treatment-emergent adverse event.
In the omeprazole study, TEAEs were reported in 4 (33%) subjects receiving riociguat only and in 5 (42%) subjects receiving riociguat plus omeprazole, with no AEs reported during the omeprazole pretreatment phase. The most common TEAEs were headache (9 events in 8 subjects, 5 drug related) and flushing (3 events in 2 subjects, all drug related). All AEs were of mild severity, except for 1 AE of headache in a subject receiving riociguat plus omeprazole that was reported as moderate in severity and considered drug related.
Mean heart rate increased continuously until 8 hours after drug administration by a maximum of 12 bpm, compared to baseline, when riociguat was given alone and by a maximum of 10 bpm when given in combination with omeprazole. ECG findings did not reveal any unexpected or untoward effects attributable to riociguat.
One case was reported of transient increase in C-reactive protein (CRP) to more than 12 times the upper limit of normal (ULN) 3 days after dosing. The subject did not present with any signs of an acute inflammatory condition. The reason for the extent of the CRP increase is unknown. All other abnormalities of laboratory values to levels above the ULN were minor, transient, and without clinical relevance. There was no signal for drug-induced laboratory parameter changes. No relevant laboratory abnormalities below the lower limit of normal (LLN) were detected.
In the AlOH/MgOH study, TEAEs were reported in 9 subjects (75%) receiving riociguat only and in 8 subjects (67%) receiving riociguat plus AlOH/MgOH. The most common TEAEs were headache (12 events in 7 subjects, all drug related), rhinitis (3 events in 3 subjects, none drug related), upper abdominal pain (3 events in 2 subjects, none drug related), and nasal congestion (3 events in 2 subjects, 2 drug related). All TEAEs were of mild severity, except for 4 that were reported as moderate (2 cases of headache and 1 each of dizziness and pain in the extremities, all in subjects receiving riociguat only; the headache and dizziness were considered to be drug related). TEAEs such as nasal congestion, postural dizziness, flushing, and headache were considered to be associated with the vasodilatory properties of riociguat and therefore to be drug related.
Mean heart rate increased from baseline by a maximum of 12.5 bpm 6 hours after drug administration when riociguat was given alone and by a maximum of 10.4 bpm 6 hours after drug administration when given in combination with AlOH/MgOH. ECG findings, especially QTc analyses (according to the formula of Bazett and Fridericia), did not reveal any unexpected or untoward effects attributable to riociguat.
Most elevations of laboratory values above the ULN were minor, transient, and without clinical relevance. In 1 subject, transient liver enzyme elevations and increases in CRP were observed 11 days after dosing. These were considered to be unrelated to study medication and possibly due to a viral infection. In 2 subjects, transient creatine kinase elevations were observed during the outpatient follow-up period. These were considered to be unrelated to study medication and due to physical strain. The laboratory abnormalities had returned to normal or near normal by the end of the observation period. No relevant laboratory abnormalities below the LLN were detected.
No serious TEAEs occurred in either study, and all TEAEs had resolved at the end of the observation periods. In both studies, SBP and DBP decreased slightly, with a concomitant increase in heart rate following treatment with riociguat.
DISCUSSION
Riociguat has been approved in several regions, including the United States, Europe, and Canada, for the treatment of PAH, inoperable CTEPH, and recurrent/persistent PH after PEA. Dyspepsia and heartburn are common AEs with riociguat treatment;1,2 therefore, it is likely that patients prescribed riociguat may be taking prescription medications that alter gastric pH. Indeed, approximately 56% of patients participating in the phase 2/3 trials receiving riociguat also received drugs acting on gastric acidity (e.g., antacids, proton pump inhibitors, and H2 antagonists). 7 In vitro data have shown that riociguat solubility is higher in acidic media than in neutral media;6,8 therefore, these two clinical pharmacological trials investigated the pH dependency of the absorption of riociguat when coadministered with either the proton pump inhibitor omeprazole or the antacid AlOH/MgOH in healthy male subjects. Pre- and cotreatment with omeprazole led to a slight decrease in riociguat bioavailability, and cotreatment with AlOH/MgOH resulted in a greater decrease in riociguat bioavailability, confirming the findings of the in vitro investigation. This effect on riociguat bioavailability highlights the importance of maintaining the 3-times-daily dosing regimen of riociguat for the treatment of PAH, inoperable CTEPH, or recurrent/persistent PH after PEA. In light of these findings, it is recommended that antacids should not be taken within 1 hour of taking riociguat,6–8 but no dose adjustment or time delay is needed for coadministration of riociguat and proton pump inhibitors.
Treatment with riociguat, with or without omeprazole or AlOH/MgOH, was well tolerated, with a good safety profile. In both studies, SBP and DBP decreased slightly, with a concomitant increase in heart rate following treatment with riociguat. Most TEAEs were of mild severity and were as expected from the mechanism of action of riociguat.
In conclusion, the bioavailability of riociguat is affected by an increase in gastric pH via the use of AlOH/MgOH and, to a lesser extent, by omeprazole. Therefore, antacids should not be administered within 1 hour of taking riociguat.6,8 However, general dose adaptation is not necessary for patients with comedication acting on gastric pH, such as proton pump inhibitors, beyond the dose-adjustment concept1,2 for riociguat.
