Abstract
Pulmonary arterial hypertension (PAH) is a complex, multifactorial disease in which an increase in pulmonary vascular resistance leads to increased afterload on the right ventricle (RV), causing right heart failure and death. Our understanding of the pathophysiology of RV dysfunction in PAH is limited but is constantly improving. Increasing evidence suggests that in PAH RV dysfunction is associated with various components of metabolic syndrome, such as insulin resistance, hyperglycemia, and dyslipidemia. The relationship between RV dysfunction and fatty acid/glucose metabolites is multifaceted, and in PAH it is characterized by a shift in utilization of energy sources toward increased glucose utilization and reduced fatty acid consumption. RV dysfunction may be caused by maladaptive fatty acid metabolism resulting from an increase in fatty acid uptake by fatty acid transporter molecule CD36 and an imbalance between glucose and fatty acid oxidation in mitochondria. This leads to lipid accumulation in the form of triglycerides, diacylglycerol, and ceramides in the cytoplasm, hallmarks of lipotoxicity. Current interventions in animal models focus on improving RV dysfunction through altering fatty acid oxidation rates and limiting lipid accumulation, but more specific and effective therapies may be available in the coming years based on current research. In conclusion, a deeper understanding of the complex mechanisms of the metabolic remodeling of the RV will aid in the development of targeted treatments for RV failure in PAH.
Keywords
Pulmonary arterial hypertension (PAH) is a devastating disease characterized by progressive obliteration of the pulmonary vasculature, right heart failure, and death. The pathobiology of PAH is complex, and presently there is no curative treatment. Although PAH is classically thought to be a disease of the lungs, the role played by right ventricular (RV) hypertrophy and dysfunction that ultimately results in right heart failure and death is understudied. RV failure is the most common cause of death in PAH, 1 yet there are no specific therapies aimed at improving RV adaptation or function. However, it is well documented that pathological RV remodeling in PAH can be reversed with lung transplantation or with pulmonary thromboendarterectomy in chronic thromboembolic pulmonary hypertension (CTEPH).2–9 The molecular mechanisms that mediate the transition from adaptive RV compensation to failure or that can promote reversible RV remodeling are presently unknown. Recently, our group and others have found evidence indicating that intracellular lipid accumulation and decreased fatty acid oxidation (FAO) may be features of RV failure related to PAH.10–13 This raises a question: In PAH, can accumulation of fatty acids promote RV dysfunction, with a resultant progression to right heart failure and death? This article reviews the role played by increased fatty acid uptake and accumulation of fatty acid metabolites in PAH-induced RV failure and discusses what is known about the impact of these findings on human RV failure. Understanding the mechanisms and consequences of lipid deposition in the RV may suggest new diagnostic and therapeutic approaches to right heart failure in PAH.
RV DYSFUNCTION IN PAH AND ITS IMPORTANCE
In a healthy adult heart, the RV cavity is smaller than that of the left ventricle (LV) and has a much smaller wall thickness, making the RV well suited as a flow conduit rather than a pressure-generating pump. In PAH, the shape of the RV is changed from the normal conformation and RV wall stress is significantly increased14,15 as a result of an increase in pulmonary vascular resistance (PVR) with increased RV afterload.16,17 The progressive remodeling of the pulmonary vascular bed leads to an increase in PVR. In PAH, the initial response to increased RV afterload is adaptive RV hypertrophy, 18 characterized by an increase in protein synthesis and cardiomyocyte size through the addition of sarcomeres. 19 With sustained pressure overload, these initially adaptive changes transition to dysfunction, with the RV progressing to contractile dysfunction accompanied by thinning and dilation of the RV.16,20,21 Magnetic resonance imaging–derived RV pressure-volume loops can be used for assessment of RV myocardial contractility. In severe pulmonary hypertension, RV pressure overload is associated with reduced RV pump function despite enhanced RV myocardial contractility. 21 In PAH, RV ejection fraction (RVEF) is a better predictor of the long-term outcome of a disease than PVR. RV dysfunction can progress in PAH patients despite a decrease in PVR. However, in the same group of patients, those with decreased RVEF had significantly poorer survival than those with stable or increased RVEF. 22 In CTEPH patients, preoperative RV dysfunction is associated with increased postoperative mortality after pulmonary endarterectomy. Balloon pulmonary angioplasty has been shown to induce RV reverse remodeling and improved systolic dysfunction by ameliorating hemodynamics in patients with inoperable CTEPH. 23 The molecular mechanism of uncoupling the adaptive hypertrophic response of RV and the increased pressure overload causing RV failure is not well studied. Recently, there has been progress in categorizing animal models of RV failure or compensated hypertrophy, which may be useful to answer fundamental questions. For example, (1) What is the mechanism that triggers the RV to transition from compensatory mode to RV failure? (2) Why do some patients develop RV myocardial ischemia? (3) Do myocytes undergo apoptosis?
NORMAL CARDIAC ENERGY METABOLISM
Molecular characterization of a pattern of RV failure in PAH has pointed to a potential role for abnormal metabolic pattern in RV failure. 11 To understand this shift, we will first discuss the normal cardiac metabolic pattern. Despite well-described embryologic and physiologic differences between the RV and the LV,15,24–26 the majority of the available information on RV metabolism is based on studies conducted on the LV. 27 The adult healthy heart is an organ with very high energy utilization rates, which is derived from various oxidizable energy sources like fatty acids, glucose, lactate, ketones, and amino acids. 28 The normal heart adapts to changes in the environment and subsequent nutrient delivery by switching from one substrate to another. 29 In its basal metabolic state, free fatty acid is the predominant source of energy production (60%–90%), and carbohydrates (e.g., glucose) are secondary sources. Mitochondrial metabolism can use either carbohydrates (after glycolysis) or fatty acids to generate adenosine triphosphate (ATP).27,30
PAH, RV DYSFUNCTION, AND METABOLIC SYNDROME: COULD THEY BE RELATED?
Metabolic syndrome is a cluster of metabolic risk factors defined by dyslipidemia, systemic hypertension, elevated fasting glucose level, and central obesity. 31 Although metabolic syndrome is thought to be an interrelated collection of risk factors for cardiovascular disease, other complications have been recognized, and several groups are investigating the effect of this syndrome on the pulmonary vasculature and, more recently, the RV. Insulin resistance, hyperglycemia, and dyslipidemia have been reported in human PAH and appear to portend a worse prognosis.32–34 Elevated body mass index has also been reported to be common in PAH, 35 although waist circumference has not been studied in PAH. Because the RV is the primary determinant of mortality in PAH and the impact of these metabolic findings appears to be on mortality, one may hypothesize that metabolic derangement in PAH affects the RV. Metabolic syndrome may affect RV compensatory capacity or may even underlie RV failure in PAH. There is a large amount of evidence demonstrating the impact that metabolic syndrome has on the structure and function of the LV.36–39 All of the metabolic syndrome criteria significantly affect LV dysfunction. 40 LV diameters proportionally increase with increasing severity of metabolic syndrome. 41 LV hypertrophy increases progressively as the number of metabolic syndrome risk factors increases.40–43 Systolic and diastolic blood pressure and waist circumference are associated with LV hypertrophy.44,45 However, stability in body weight is thought to be a preventive factor for diabetes, one of the components of metabolic syndrome. 46 Among metabolic syndrome criteria, systolic blood pressure, waist circumference, hyperlipidemia, and glucose level are also shown to be independently associated with RV structure and function. 47 Specific to the RV, there may be impaired RV function in metabolic syndrome patients with preserved LV ejection fraction. 48 We have recently presented data from the MESA-RV cohort showing that in otherwise healthy humans insulin resistance may affect RV structure and function as measured by cardiac magnetic resonance. Specifically, insulin resistance was associated with reduced RV mass and ejection fraction. 49 Despite this preliminary work, the potential impact of several features of metabolic syndrome, such as systemic hypertension, hyperlipidemia, and central obesity with attendant adipokine dysregulation, are little studied in the human RV broadly and in the failing RV in particular. Given the strongest clinical evidence favoring an important role for altered glucose homeostasis in PAH, we will focus on this feature of metabolic syndrome for the remainder of this review and discuss how an altered balance of glucose and FAO may play a potential role in promotion of RV dysfunction in PAH.
ASSOCIATION BETWEEN RV DYSFUNCTION AND FATTY ACID/GLUCOSE METABOLITES IN PAH
Recent work by our group and others in both animal models of PAH and human disease suggested that in PAH insulin resistance (1) can be measured systemically, (2) worsens pulmonary vascular disease in animal models, and (3) may affect RV function.11,13,32,33,50–52 In PAH, RV failure is the strongest predictor of mortality
16
—thus the finding that a measure of chronic hyperglycemia, hemoglobin A1C (HbA1C), can serve as an independent prognostic factor of long-term PAH with a hazard ratio of 2.2 per unit increase in HbA1c,51,53 indirectly suggesting that there is an interaction between glucose homeostasis and RV function. Direct measurement of RV glucose uptake has also been implemented in PAH. In idiopathic PAH patients, myocardial glucose uptake is increased and correlates with mean pulmonary arterial pressure, presumably indicating the presence of RV functional impairment with a shift from fatty acid utilization to myocardial glucose utilization. This may serve as a marker of RV dysfunction.
54
Recently, Lundgrin et al.
55
suggested that PAH hearts have a pathological glycolytic metabolism as indirectly measured by increased 2-deoxy-2-[18F]fluoro-
Although a mitochondrial shift from fatty acids to glucose may be a critical mediator of RV dysfunction in PAH, there may be additional changes in fatty acid metabolism that promote RV failure; for instance, fatty acid cellular import or storage of fatty acids may also be affected. In humans, there is evidence that impaired myocardial fatty acid uptake may be closely related to RV systolic dysfunction and may underlie the poor prognosis in patients with pulmonary hypertension. 58 Studies in PAH patients have also shown that impaired fatty acid metabolism may exist in severely hypertrophic RV due to RV overload.56,59 At present, little is known about lipid storage in the normal or failing RV. Recently, we have shown that in heritable PAH impaired RV hypertrophy is associated with RV lipotoxicity, as demonstrated by increased lipid deposition in RV cardiomyocytes. 13 Magnetic resonance spectroscopy, a useful tool in metabolic imaging of cardiac disease, can reliably measure RV triglyceride content.55,60 In uncomplicated type 2 diabetes mellitus, high myocardial triglyceride content strongly correlates with RV systolic and diastolic dysfunction. 61 In hearts from fatty Zucker rats, triglyceride droplets are clearly visible close to mitochondria within myocardial cells. 62 In light of reduced mitochondrial use of lipids with at least normal cellular fatty acid uptake, one might hypothesize that lipid intermediaries would be increased in the cytoplasm and lead to a “lipotoxic cardiomyopathy.” 63 In a mouse model universally expressing a mutant form of bone morphogenic protein receptor type 2 (BMPR2), which underlies most forms of human heritable PAH, we have shown increased lipid content, especially triglycerides and ceramides, in RV tissue compared with control littermates. 13 However, no study has quantified levels of lipid intermediates in the living human RV. Although it is clear that there are alterations in lipid transport, metabolism, and storage, it remains unclear whether these directly contribute to RV dysfunction or are caused by myocardial dysfunction, conformational changes, electrophysiological changes, or other stimuli.
CAN MALADAPTIVE FATTY ACID METABOLISM CAUSE RV DYSFUNCTION AND HYPERTROPHY IN PAH? (Fig. 1)
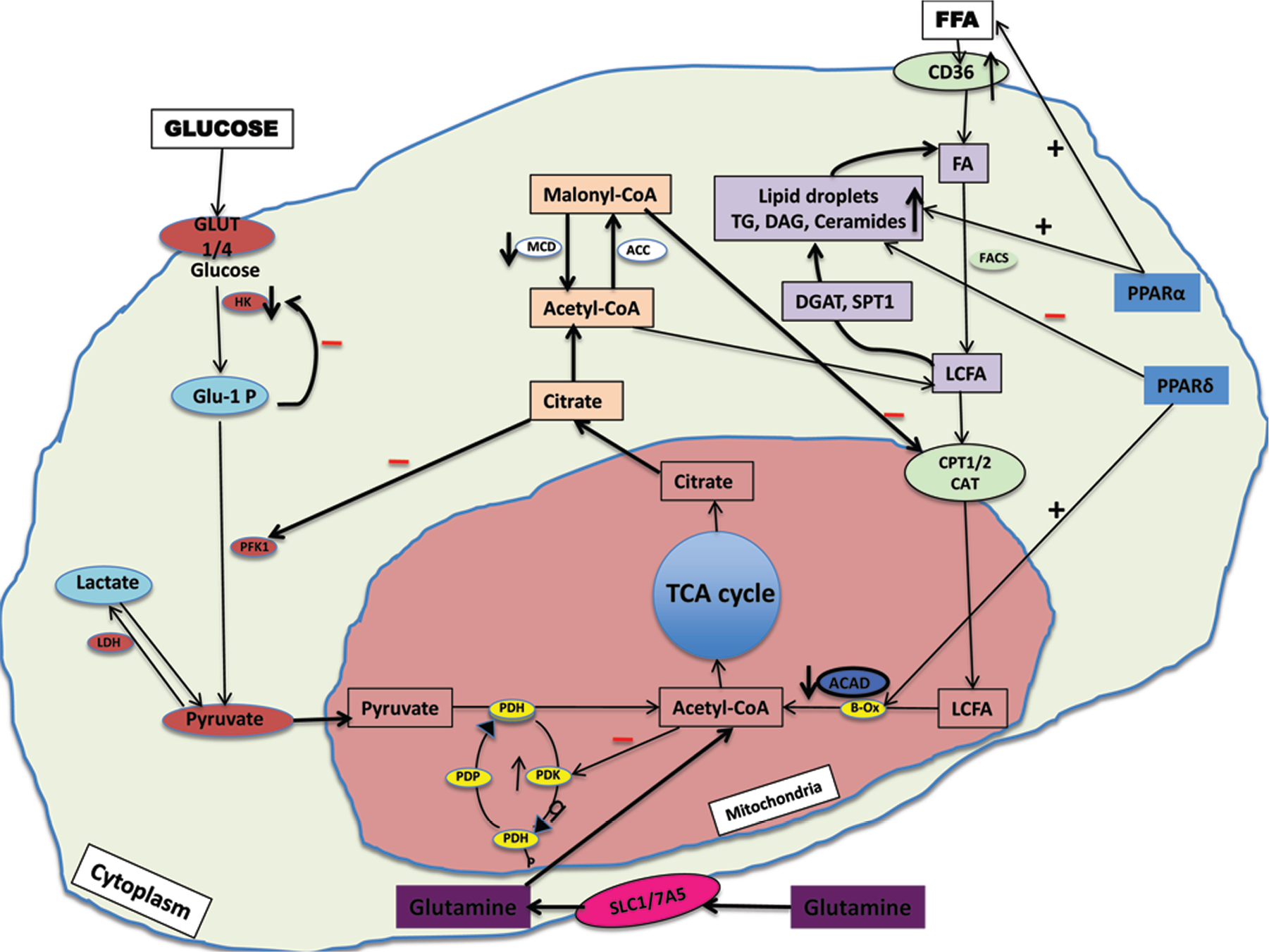
Imbalance between fatty acid and glucose oxidation in right ventricular (RV) cardiomyocytes in pulmonary arterial hypertension. Evidence-based literature suggests that the metabolic imbalance in RV cardiomyocytes may be due to maladaptive fatty acid metabolism as a result of an increase in fatty acid uptake by fatty acid transporter molecule CD36 and a disruption of the reciprocal relationship between glucose and fatty acid oxidation in the mitochondria. This leads to accumulation of lipids (triglycerides, diacylglycerol, and ceramides) in the cytoplasm, causing cardiac lipotoxicity. GLUT: glucose transporter; HK: hexokinase; Glu-1 P: glucose-1-phosphate; PFK: phosphofructokinase; LDH: lactate dehydrogenase; MCD: malonyl-CoA decarboxylase; ACC: acetyl-CoA carboxylase; TCA: tricarboxylic acid cycle; PDH: pyruvate dehydrogenase; PDK: pyruvate dehydrogenase kinase; PDP: pyruvate dehydrogenase phosphatase; ACAD: acetyl-CoA dehydrogenase; B-Ox: β-oxidation; LCFA: long-chain fatty acid; CPT: carnitine palmityl transferase; CAT: carnitine acyltransferase; DGAT: diglyceride acyltransferase; SPT: serine palmitoyltransferase; TG: triglycerides; DAG: diacylglycerol; FA: fatty acid; CD36: fatty acid transporter molecule; FFA: free fatty acid; PPAR: peroxisome proliferator–activated receptor; FACS: fatty acyl-CoA synthetase; SLC: solute carrier family.
Increase in fatty acid uptake: role played by fatty acid transporter molecule CD36
CD36 is the main fatty acid transporter molecule in the healthy human heart and has been well studied in the LV. CD36 accounts for approximately 70% of fatty acid uptake into contracting cardiomyocytes.64,65 It is stored in intracellular compartments in cardiomyocytes and recruited to the sarcolemma to facilitate fatty acid uptake, which is a reversible process.66,67 This relocalization of CD36 is triggered by insulin, diet, muscle contraction, and pharmacological agents like caffeine.66,68–70 Relocalization of CD36 causes chronic elevation of long-chain fatty acid uptake into the heart followed by myocellular lipid accumulation, which is thought to lead to insulin resistance,68,69,71 not to just be caused by insulin resistance. CD36 has been implicated to play a role in the pathogenesis of various cardiac metabolic diseases involving alterations in cellular lipid metabolism (cardiac lipotoxicity) leading to cardiac contractile dysfunction. However, the role played by CD36 in RV lipotoxicity, which can lead to RV dysfunction in PAH, is still under investigation. Our recent findings in our mutant BMPR2 mouse model of PAH demonstrate an increase in the expression of CD36 protein in the mouse RV, 72 which may lead to increased uptake of fatty acids. Similarly, in a model of LV failure, RV hypertrophy is associated with an increase in CD36 gene expression. 73 A permanent relocation of CD36 to the sarcolemma can increase cardiac fatty acid uptake and induce cardiac hypertrophy and contractile dysfunction.68,70,74 However, it is important to remember that the reduced RV function is associated with an increase in the expression of several genes that regulate fatty acid metabolism, especially those regulating fatty acid uptake and intracellular transport. These include CD36, peroxisome proliferator–activated receptor (PPAR) a, and PPAR? coactivator 1a. 75 However, not all increases in CD36 expression are pathological; for example, exercise-induced cardiac hypertrophy does not lead to cardiac failure. 76 At present, information on CD36 movement, function, and expression in the RV and how it contributes to lipotoxic RV cardiomyopathy in both health and disease is very limited.
In the mitochondria: imbalance between glucose oxidation (GO) and FAO
The energetics of myocardium is affected by the myocardial substrate provided. 77 In cardiomyocytes, FAO is the major source of ATP production and oxygen consumption (60%–90%), whereas glucose metabolism (glycolysis and GO) is considered a secondary source (10%–40%) of energy production. 10 That said, it is known that the external power of the LV is higher for a given myocardial oxygen consumption when the myocardium has a low rate of fatty acid β-oxidation relative to glucose and lactate oxidation. 77 In the normal heart, 75% of the fatty acids in the cytoplasm are immediately oxidized. Fatty acids are converted into long-chain acyl–coenzyme A (CoA) esters by fatty acyl-CoA synthetase. Long-chain acyl-CoA is converted by carnitine palmitoyltransferase (CPT) to long-chain acylcarnitine. CPT is a key enzyme in the mitochondria that shuttles long-chain fatty acids into the mitochondria, where they undergo β-oxidation to produce acetyl-CoA that feeds into the Krebs cycle. There is a reciprocal relationship between FAO and GO, called the Randle cycle, such that inhibiting one increases the other. 29 Activation of FAO results in inhibition of pyruvate dehydrogenase (PDH) and vice versa, allowing for tissue-specific regulation of fuel supply to the mitochondria. Increasing GO and inhibiting FAO may be beneficial because FAO uses 12% more oxygen than GO to generate a given amount of ATP; 78 this may be at least in part due to capillary rarefaction in RV failure with resultant ischemia. 49 PDH kinase (PDK), also an important enzyme, regulates the relative balance between carbohydrate and fatty acid fuel supply to the mitochondria 79 by deactivating PDH, a critical enzyme required for GO. An acute increase in cardiac overload can cause a relative increase in glucose uptake compared with fatty acid uptake and β-oxidation,55,80 but that suggests only an increase in glycolysis, not GO. 80
In PAH, increased delivery of fatty acids could affect FAO rates and thus alter compensatory RV hypertrophy and/or promote RV dysfunction. Little is known about the role played by FAO in RV failure. In adult Sprague-Dawley rats, PAB-induced RV hypertrophy shows increased RV FAO rates, reduced cardiac output and treadmill walking distance, and elevated plasma epinephrine levels. In this model, the increase in RV FAO is accompanied by an increase in CPT1 expression and a decrease in GO and PDH activity. 57 Most of the available literature on RV dysfunction and failure in PAH is mainly focused on glucose homeostasis (see below), and very limited information on FAO alterations in PAH is available. Simonsen and Kjekshus 81 have shown that the adaptive response induced by catecholamine and atrial pacing can increase myocardial oxygen consumption due to increased fatty acid uptake. In the specific context of the RV, we have recently demonstrated that metabolic changes in human RVs from PAH patients, as determined by gene expression analysis, suggest suppression of the TCA cycle, increased glycolysis, and decreased derivation of energy from lipid oxidation compared with controls. 13 Similarly, metabolomic analysis of human pulmonary microvascular endothelial cells expressing two different disease-causing BMPR2 mutations uncovered significant decreases in carnitine and FAO pathways as well as impairment of the TCA cycle, and it confirmed an increase in aerobic glycolysis. 82
A key regulatory enzyme for FAO is malonyl-CoA decarboxylase (MCD). MCD decarboxylates malonyl-CoA to acetyl-CoA. Malonyl-CoA inhibits CPT1, the rate-limiting pathway for fatty acid entry into mitochondria. Thus, inhibition of MCD increases malonyl-CoA, decreases FAO, and subsequently activates PDH and GO. 83 In the myocardium, lack of MCD promotes GO and improves cardiac efficiency during ischemia/reperfusion injury in Mlycd−/− mice.84,85 The limited FAO in these mice under normal conditions keeps PDH tonically activated, promoting GO. The role played by MCD in RV failure is unknown.
Another important molecule in the mitochondrial metabolism of cardiomyocytes is PPARδ. PPARδ is the predominant subtype in the heart, 86 where it plays an important role in cardiac metabolism by regulating the expression of genes involved in fatty acid and glucose utilization.87,88 In mice, cardiomyocyte-restricted deletion of the PPARδ gene results in decreased myocardial FAO, increased myocardial lipid accumulation, and dilated cardiomyopathy. 87 In neonatal cardiomyocytes, phenylephrine-induced hypertrophy is accompanied by a reduction in the expression of the genes for M-CPT1 and PDK4 (involved in fatty acid metabolism and activation of nuclear factor κB), which can be abolished by activators of PPARδ, 88 but it is not studied specifically in RV.
In PAH, aerobic glycolysis, or a shift from GO to glycolysis in the presence of adequate oxygen, is known to occur in pulmonary vascular cells89,90 and hypertrophied RV myocytes. 79 Aerobic glycolysis is also known as the Warburg effect 91 and induces glutaminolysis. 92 Although these are the hallmarks of cancer metabolism, in PAH-associated RV hypertrophy a maladaptive metabolic switch to aerobic glycolysis is observed. 79 This is mediated by increased expression and activity of PDK4, resulting in inhibition of PDH, 93 the key enzyme in GO. In the monocrotaline model of pulmonary hypertension with RV failure, reduced RV function and electrical remodeling is shown in part to be the result of increased activity and expression of PDK, which mediates glycolytic shift in the RV. 94 In the context of Warburg metabolism, glutamine serves as an alternate carbon source. Cells can oxidatively metabolize glutamine-derived α-ketoglutarate (αKG) in the TCA cycle and generate pyruvate from malate by glutaminolysis. 95 Alternatively, cells can reductively carboxylate αKG to generate citrate via an isocitrate dehydrogenase reaction, which is highly reversible. The monocrotaline mouse model of RV hypertrophy demonstrates an increase in glutaminolysis accompanied by an increase in the expression of glutamine transporters (solute carrier family [SLC] 1A5 and SLC7A5) and mitochondrial malic enzymes (Me1 and Me2), which convert malate to pyruvate, in the RV. Similarly, in PAH patients with RV hypertrophy there is a capillary rarefaction and upregulation of glutamine transporter, suggesting that cardiac glutaminolysis is associated with microvascular rarefaction/ischemia. 94
To summarize, in RV failure there appears to be a suppression of FAO rates and an increase in the rate of glucose utilization. There is greater understanding of the metabolic pattern of RV failure than of the underlying mechanisms that promote these changes, particularly in the context of FAO.
In the cytoplasm: lipid accumulation in the form of triglycerides, diacylglycerol, and ceramides
The increased sarcolemmal CD36 abundance, together with an increased plasma fatty acid concentration, demonstrates an increased rate of fatty acid uptake. Without a concomitant substantial increase in the mitochondrial FAO rate, this can lead to excess production of long-chain acyl-CoA in the cytoplasm, which can be converted into a number of complex intracellular lipid intermediates (like esterification into triacylglycerols [TAG]), and to increased concentrations of fatty acid metabolites, such as diacylglycerols (DAG) and ceramides. 96 The conversion of fatty acids into complex lipids such as TAG, DAG, and ceramides has recently received considerable interest, as the accumulation of these potentially harmful intermediates have been implicated in the development of insulin resistance, cardiac dysfunction, and right heart failure.13,32,97–99 In PAH patients with insulin resistance, the triglyceride/high-density lipoprotein cholesterol (HDL-C) ratio was significantly higher. 33 In PAH patients, lower plasma levels of HDL-C and higher total cholesterol/HDL-C ratios directly correlate with right heart failure. 32 At the cellular level, in RVs from a transgenic mouse model of PAH expressing mutant Bmpr2, we have demonstrated a significant increase in intracardiomyocyte triglyceride deposition and ceramide content. 13 We recently found that metabolomic analysis of peripheral blood from PAH patients shows an increase in medium- and long-chain acylcarnitines (E. Brittian, unpublished data). Lipids that accumulate in the form of triglycerides are synthesized by the enzyme diacylglycerol acyl transferase (DGAT), the final enzyme in the synthesis of triglycerides. Cardiomyocyte-specific DGAT1-overexpressing transgenic mice demonstrate an increase in LV lipid accumulation and a reduction in mitochondrial biogenesis, with the development of significant cardiomyopathy and systolic dysfunction over time. This occurs in the absence of hyperglycemia or plasma dyslipidemia, suggesting that triglyceride accumulation results in cardiac dysfunction. 100 In hearts from middle-aged mice, an increase in myocardial CD36 expression contributes to high-fat diet–induced cardiac hypertrophy, mediated by elevated levels of ceramide via signaling through the AMP-activated protein kinase pathway. 74 In cultured cardiomyocytes, ceramides induce apoptosis by a mechanism involving increased Ca2+ influx, mitochondrial network fragmentation, and loss of the mitochondrial Ca2+ buffer capacity, which triggers cardiomyocyte death via the activation of calpains. 101 Cardiac-specific overexpression of the fatty acid–activated nuclear receptor PPARα (myosin heavy-chain PPARα) in mouse hearts exhibits myocyte lipid accumulation and cardiac dysfunction. CD36 is necessary for the development of lipotoxic cardiomyopathy in these mice.97,102 This suggests that in PAH RV lipotoxicity could be the result of increased fatty acid uptake or impaired mitochondrial FAO; further investigation is required to determine the primary disorder.
Complex relationship between lipid deposition and insulin resistance (Fig. 2)
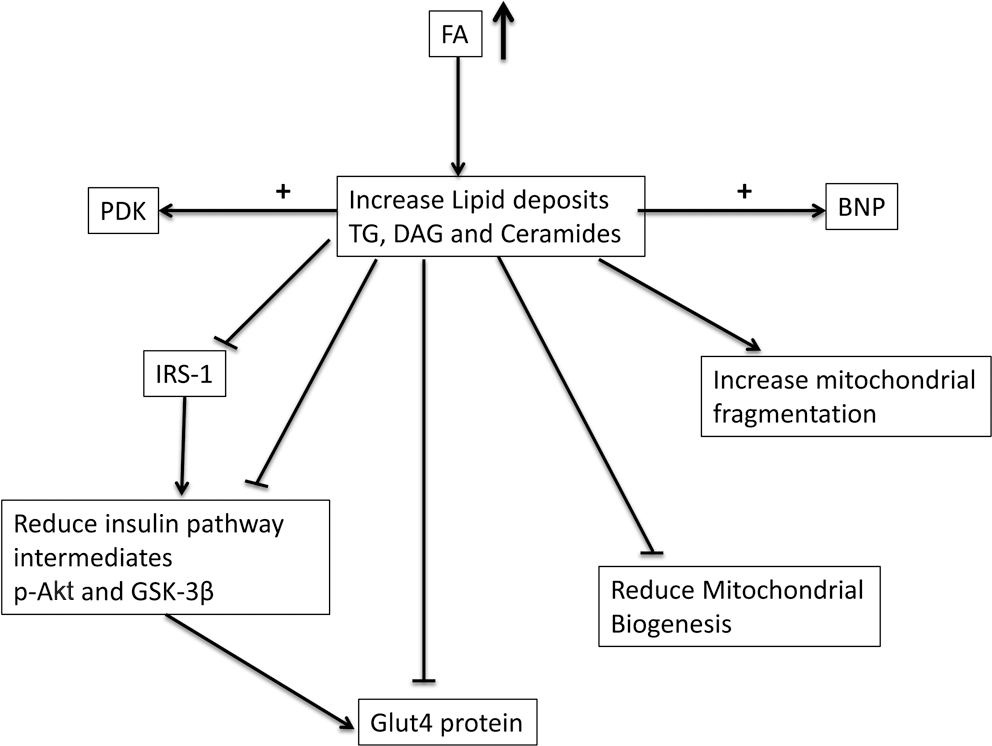
Effect of right ventricular (RV) lipotoxicity in pulmonary arterial hypertension (PAH). Lipid deposition in RV cardiomyocytes in PAH could affect mitochondrial metabolism, lead to insulin resistance, inhibit intermediates of glucose oxidation, and elicit a response to hypertrophy. FA: fatty acid; PDK: pyruvate dehydrogenase kinase; TG: triglycerides; DAG: diacylglycerol; BNP: brain natriuretic peptide; IRS: insulin receptor substrate; p-Akt: phosphorylated Akt; GSK: glycogen synthase kinase; Glut: glucose transporter.
An association between lipid accumulation within cardiomyocytes and insulin resistance is widely accepted. Studies by Randle and colleagues in rodent heart and diaphragm muscle suggest that fatty acids impair insulin-mediated glucose uptake in muscle by inhibition of PDH; this leads to reductions in GO and accumulation of glycolytic intermediates. 103 It is well known that fatty acid intermediates can trigger a cascade of reactions that interfere with insulin-induced translocation of glucose transporter type 4 (GLUT4) to the sarcolemma. In mice fed a high-fat diet, increased myocardial lipid deposition leads to increased glucose intolerance due to intracellular retention of GLUT4 and decreased insulin receptor substrate 1 expression. 104 Similarly, Zucker diabetic fatty rats, a model of diabetic cardiomyopathy, are obese, hyperglycemic, hyperinsulinemic, and dyslipidemic. In addition, in these rats the RV diastolic diameter is increased and RV metabolic rates of glucose utilization are decreased, with a consistent decrease in GLUT4 expression. This is due to a decrease in insulin-dependent phosphorylation of Akt-Ser473 and glycogen synthase kinase 3β. 105 In skeletal muscle and cardiomyocytes, saturated fatty acid oversupply concomitantly induces the accumulation of ceramide and diacylglycerol, which inhibits insulin stimulation of Akt/protein kinase B, a serine/threonine kinase. 106 In the cardiomyocyte cell line AC16, C6-ceramide downregulates GLUT4 expression and upregulates PDK4 and brain natriuretic peptide expression, but it also decreases phosphorylated Akt and phosphorylated glycogen synthase kinase 3β in a concentration-dependent manner. 107 Palmitate-treated cardiomyocytes show an increase in ceramides or triglycerides accompanied by a decrease in the rate of glycolysis and insulin resistance. 108 All of these changes are associated with abnormalities in the insulin signaling cascade due to lipid accumulation in cardiomyocytes. Although cardiac fat is associated with impairment in heart metabolism and cardiac dysfunction, the interplay among cardiac fat accumulation, insulin resistance, and cardiac dysfunction in the context of the RV remains to be fully established.
INTERVENTIONS TO IMPROVE RV STRESS DUE TO LIPID ACCUMULATION (Table 1)
Interventions to improve right ventricular (RV) stress due to lipid accumulation
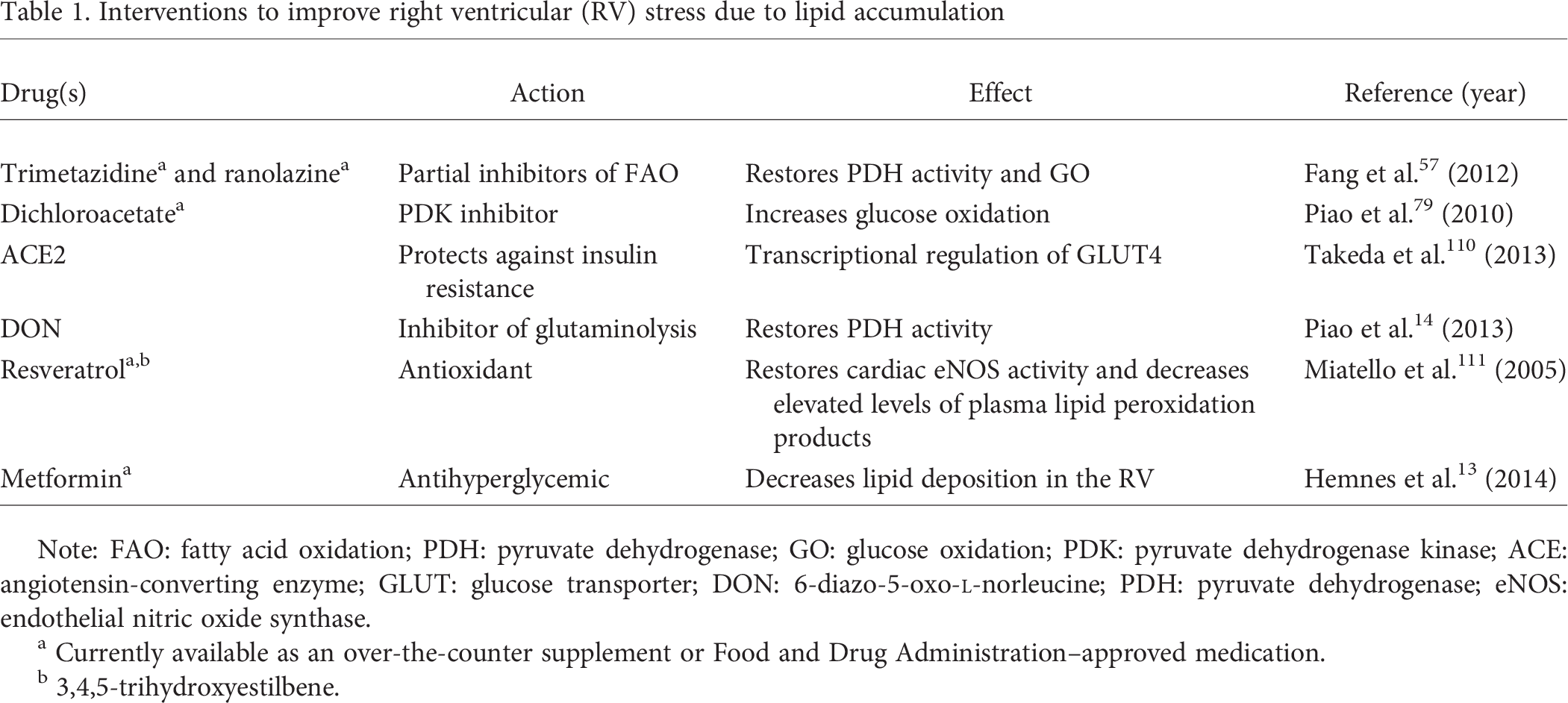
Note: FAO: fatty acid oxidation; PDH: pyruvate dehydrogenase; GO: glucose oxidation; PDK: pyruvate dehydrogenase kinase; ACE: angiotensin-converting enzyme; GLUT: glucose transporter; DON: 6-diazo-5-oxo-
Currently available as an over-the-counter supplement or Food and Drug Administration–approved medication.
3,4,5-trihydroxyestilbene.
Interventions that can completely or partially reverse the adverse effect of cardiac lipotoxicity in the RV hold promise to substantially improve the longevity and functional compensation of the RV. Because of the complex balance between FAO and GO in cardiomyocytes, interventions to alter one side of the metabolic equation (i.e., FAO) must be considered in the context of their effects on the opposing side (i.e., GO) and their global effects on RV compensation and survival. Trimetazidine and ranolazine, partial inhibitors of FAO, have been shown to reduce elevated RV glycogen levels in the hypertrophic rat RV, to increase cardiac output and exercise capacity, and to attenuate exertional lactic acidemia. These FAO inhibitors restore PDH activity and GO, thereby increasing ATP levels; therefore, they may have therapeutic potential in RV hypertrophy.
57
Similarly, the PDK inhibitor dichloroacetate acutely increases GO and cardiac output in monocrotaline-induced RV hypertrophy. Chronic dichloroacetate therapy has been shown to improve RV repolarization and function in vivo and in the RV Langendorff model.
79
A specific inhibitor of glutaminolysis, 6-diazo-5-oxo-
CD36, the key molecule of RV lipotoxicity, can serve as a therapeutic target for the prevention and/or treatment of insulin resistance–related cardiac contractile dysfunction. In a genetic mouse model of cardiac lipotoxicity overexpressing PPARα but deficient in CD36 (Myh-Ppara/Cd36−/−), myocyte triacylglyceride accumulation and cardiac dysfunction is prevented and glucose uptake and oxidation is increased, although fatty acid utilization remains unchanged; this suggests that CD36 is required for the development of lipotoxic cardiomyopathy, and novel therapeutic strategies aimed at reducing CD36-mediated fatty acid uptake may prevent or treat cardiac dysfunction. 97 Ablation of CD36 prevents the effect of metabolic stress due to the Western diet and the high-blood-pressure mechanophysical stress on cardiac remodeling and dysfunction caused by lipid accumulation. 112 Lipoprotein lipase deficiency due to deletion of CD36 can rescue myocyte triglyceride accumulation, mitochondrial gene regulatory derangements, and contractile function.97,102 These novel therapeutic strategies aimed at reducing CD36-mediated fatty acid uptake show promise for the prevention or treatment of cardiac dysfunction related to high-fat diet and GO, but as yet small molecules that target cardiomyocyte lipid import are not available.
PPARβ/δ agonist GW0742 has been shown to reduce RV hypertrophy and systolic pressures in an animal model of hypoxia-induced PAH. 113 Another selective PPARδ agonist, GW610742X, has been shown to normalize cardiac substrate metabolism and reduce RV hypertrophy in an experimental model of congestive heart failure. 73 These findings suggest that PPARδ has the potential to be a therapeutic target for the treatment of RV failure in PAH associated with reduced FAO and lipid accumulation, such as lipotoxic cardiomyopathy. Unfortunately, the track record of prior PPARδ agonists in heart failure is poor, dimming enthusiasm at least for the thiazoladinedione class of medications targeting this important molecule.
Currently there are no specific strategies that can be directed toward management of human RV failure and no interventions that might best preserve RV function in PAH. The available therapies in PAH are directed toward improving the function of the pulmonary vascular bed, which indirectly modulates the function of the RV in PAH. The inhibitors or agonists discussed above may have the potential to be developed into new strategies in combination with existing drugs, the development of new drugs, or individualized gene therapy.
CONCLUSIONS
RV failure is characterized by decreased rates of FAO, increased lipid import, and accumulation of lipotoxic compounds, such as ceramide. It is presently unknown how these changes occur and whether interventions of these altered pathways can ameliorate RV failure in PAH. These complex pathways may be altered by currently available compounds, which may bring new, desperately needed therapeutics for RV failure to patients in the upcoming years. Further understanding of the mechanisms of metabolic remodeling in RV failure will aid in the development of new, more specific treatments for RV failure of many types in the future.
