Abstract
Vasoreactivity testing with inhaled NO is recommended for pulmonary arterial hypertension (PAH) because of its therapeutic and prognostic value. Sildenafil has acute pulmonary vasodilating properties, but its diagnostic and prognostic impact in PAH is unknown. Our objective was to compare acute vasodilating responses to sildenafil and those to NO during right heart catheterization and also their prognostic values in patients with PAH. Ninety-nine patients with idiopathic PAH and 99 with associated PAH underwent vasoreactivity testing with NO and sildenafil. Only mild adverse effects of sildenafil, in the form of hypotension, were observed, at a rate of 4.5%. The acute responder rate was 8.1% for NO and 11.6% for sildenafil. The NO-induced response in mean pulmonary arterial pressure and cardiac output correlated with the response to sildenafil. Thirteen patients were long-term responders to calcium channel blockers (CCBs), and 3 of them were correctly identified by acute vasoreactivity test with both drugs. The specificity of the vasoreactivity test for identifying long-term CCB responders was 88.9% for NO and 85.1% for sildenafil testing. A trend toward better survival was found in sildenafil and NO responders, compared with nonresponders. Use of sildenafil for vasoreactivity testing is safe. Sildenafil may be useful as alternative vasoreactivity-testing agent, identifying the same number of long-term CCB responders as NO. However, NO seems to be a more ideal testing drug because of its pharmacologic properties. Moreover, sildenafil vasoreactivity testing might contribute to an improved estimate of prognosis among patients with PAH.
Pulmonary arterial hypertension (PAH) is characterized by an increase in pulmonary arterial pressure leading to progressive right ventricular dysfunction and failure. Invasive hemodynamic measurement by right heart catheterization (RHC) is necessary to establish the diagnosis. In order that appropriate therapy can be chosen, acute vasodilator testing during RHC is recommended in patients with idiopathic PAH (IPAH). A “positive acute vasodilator response” predicts the long-term response to high-dose oral calcium channel blockers (CCBs)1,2 and is currently defined as a reduction in mean pulmonary arterial pressure (mPAP) by >10 mmHg leading to an mPAP of <40 mmHg and normal cardiac output (CO) upon acute pulmonary vasodilator challenge, generally performed with inhaled nitric oxide (iNO). 3 A formerly used definition of vasoreactivity is a decrease in both mPAP and pulmonary vascular resistance (PVR) by >20%. 4
IPAH patients with a significant acute response during vasoreactivity testing are recommended for treatment with high-dose CCBs. Furthermore, they have a better prognosis than nonresponders, for whom treatment with CCBs is not advisable.2,4 However, despite an initial positive response, only one-third of these patients show a long-term benefit from CCBs, rendering reevaluation of responders compulsory. 1
Sildenafil is approved and widely used for the treatment of PAH.5–7 It targets the cyclic guanosine monophosphate (cGMP) pathway downstream of NO. Administration of sildenafil leads to acute pulmonary vasodilation that can be tracked during hemodynamic measurements.8–11 It may thus be tempting to use sildenafil for acute vasoreactivity testing, as it is cheaper, more stable, and easier to handle than iNO and intravenous epoprostenol. However, it is not yet known how similar the acute responses to sildenafil and NO and the long-term therapeutic and prognostic implications are. Hence, we aimed to compare acute vasoreactivity in response to oral sildenafil with that to iNO in patients with PAH and to determine their prognostic values for long-term treatment.
METHODS
Patients
In this retrospective, open-label, single-center study, we included consecutive patients who were admitted to our adult pulmonary hypertension unit from 2002 to 2011 and met the following criteria. (1) Patients had PAH, defined as mPAP > 25 mmHg at rest and pulmonary capillary wedge pressure < 15 mmHg, with PVR > 240 dyn·s/cm.5,12 In case of congenital heart defect (CHD), only patients with repaired CHD and absence of shunts were included. (2) Patients were treatment naive. (3) Patients had undergone vasoreactivity testing with both NO and sildenafil during RHC at initial assessment.
RHC and vasoreactivity testing were performed on clinical grounds solely. Patients’ written informed consent was obtained. Compassionate treatment with sildenafil for patients who received the drug when it had not yet been approved was done in agreement with the local institutional review board and in accordance with national legal requirements.
The decision to apply sildenafil was made by the physician performing the RHC. Sildenafil was applied if the drug was considered as a treatment for the patient at hand, the systolic systemic arterial pressure (SAP) was >90 mmHg, and the general condition of the patient during the catheterization allowed for this longer testing procedure.
Assessment of pulmonary hemodynamics and vasoreactivity testing
A pulmonary artery catheter (Edwards Swan-Ganz, 93A-754H 7.5-F; Baxter Healthcare, Irvine, CA) was used to measure pulmonary hemodynamics. CO was measured by the Fick method. For patients receiving oxygen therapy, oxygen uptake was calculated with the formulas of LaFarge and Bergstra. 13 For the other patients, oxygen uptake was measured via indirect calorimetry with the Fitmate device (COSMED, Rome). Patients received continuous nasal oxygen throughout the test procedure if initial arterial oxygen saturation was <90%.
After evaluation of baseline parameters, acute vasoreactivity testing was performed with iNO at a concentration of 20 ppm for 5–10 minutes (INO Therapeutics, Lidingo, Sweden). After 30 minutes of washout, all patients received a single dose of 25 mg of oral sildenafil. Pulmonary hemodynamics were registered every 15 minutes for 60 minutes after the administration of sildenafil. The values at the time point with the greatest decrease in mPAP were used for further analysis. A positive vasoreactivity test was defined as a drop in mPAP of >10 mmHg leading to an absolute value of <40 mmHg and a normalization of cardiac index (CI) to a value of ≥2.4 L/min/m2.
Assessments and long-term response to CCBs
Patients underwent clinical examination, a 6-minute walk test, and measurement of brain natriuretic peptide (BNP) at baseline and at each follow-up visit. The 6-minute walk test was performed according to the American Thoracic Society guidelines. Long-term responders to CCBs were defined as patients whose condition improved with CCB therapy according to clinical assessment of noninvasive parameters (functional class, 6-minute walk test, BNP) and were still receiving CCB monotherapy after 1 year.
Statistical analysis
Groups were compared by means of a t test or analysis of variance. The correlation coefficient r was computed via univariate linear regression, and graphs were plotted with IBM SPSS Statistics 20 graph builder (IBM, Armonk, NY). Differences in survival between groups were analyzed by log-rank test. A 2-tailed P value of <0.05 was considered significant.
RESULTS
Baseline characteristics
A total of 198 treatment-naive adult patients with PAH (group 1 of the Nizza classification) 15 underwent RHC and vasoreactivity testing with NO and oral sildenafil at the time of diagnosis. The patients had a mean age of 52.1 years, and 64% were women (Table 1). Half of the patients (n = 99) were diagnosed with IPAH. At the time of diagnosis, mean 6-minute walk distance was 320 m, and the majority of patients were in functional class III. Patients with IPAH showed a severe hemodynamic compromise (mPAP: 51.6 ± 13.9 mmHg, PVR: 969 ± 458 dyn·s/cm 5 , CI: 2.1 ± 0.6 L/min/m2). On average, those with associated PAH (APAH) had slightly less severe hemodynamic impairment, with elevated mPAP (49.3 ± 15.3 mmHg) and PVR (830 ± 483 dyn·s/cm 5 ), while the CI (2.5 ± 0.8 L/min/m2) was well preserved (Table 2).
Clinical characteristics of patients with pulmonary arterial hypertension
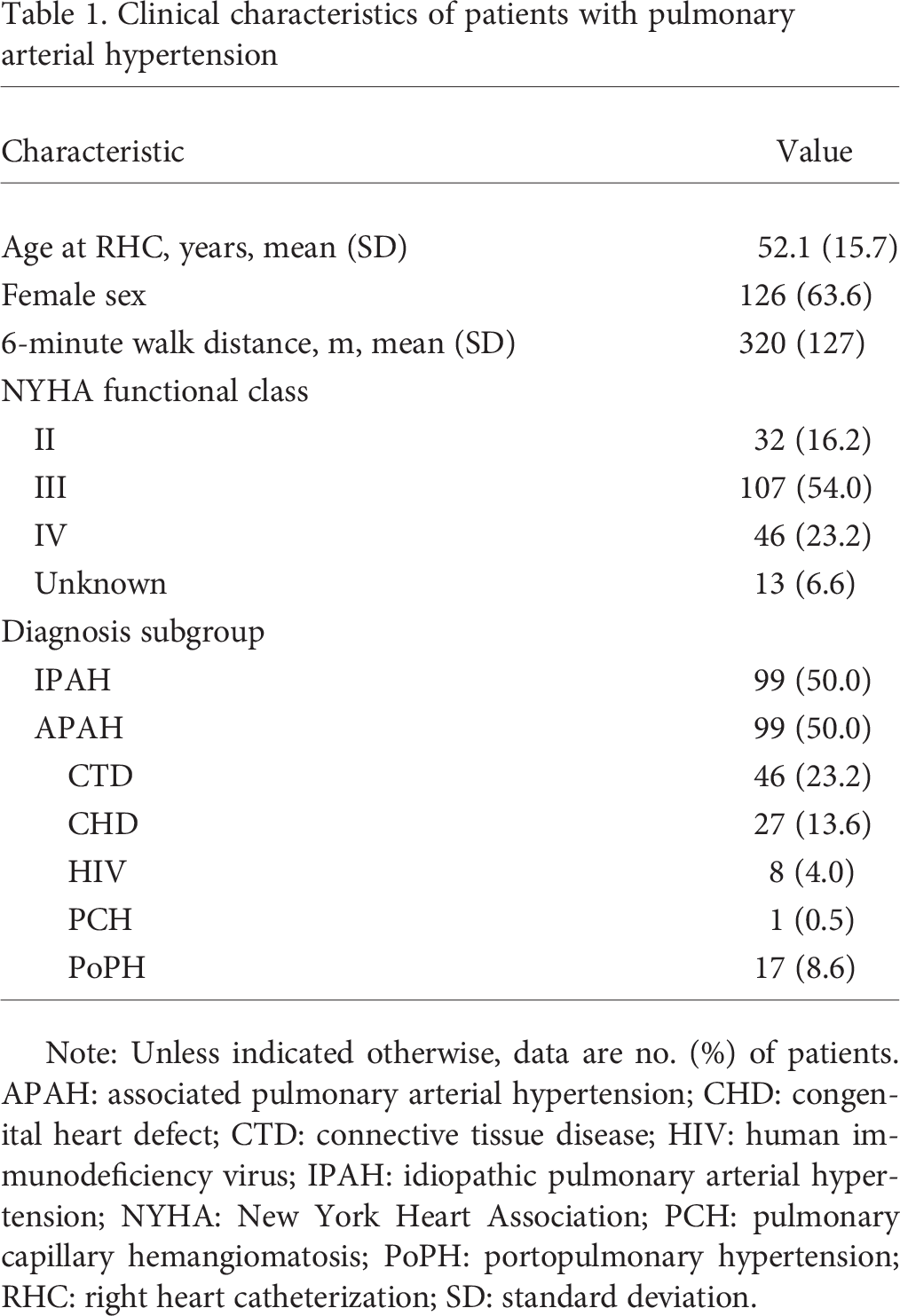
Note: Unless indicated otherwise, data are no. (%) of patients. APAH: associated pulmonary arterial hypertension; CHD: congenital heart defect; CTD: connective tissue disease; HIV: human immunodeficiency virus; IPAH: idiopathic pulmonary arterial hypertension; NYHA: New York Heart Association; PCH: pulmonary capillary hemangiomatosis; PoPH: portopulmonary hypertension; RHC: right heart catheterization; SD: standard deviation.
Hemodynamic variables at baseline and in response to inhaled NO and oral sildenafil
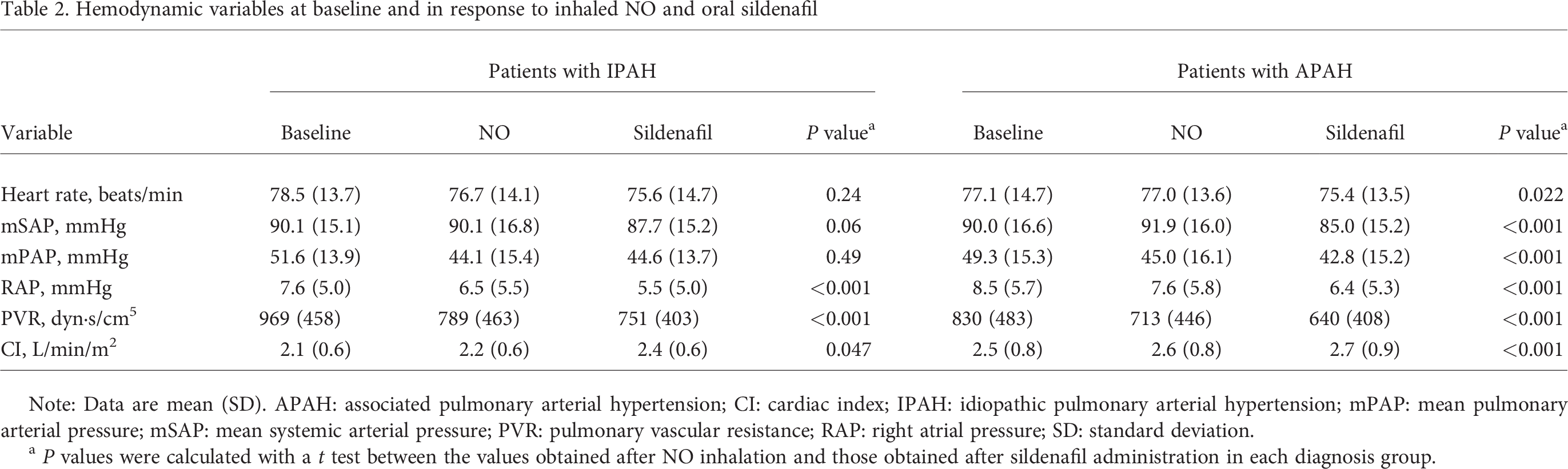
Note: Data are mean (SD). APAH: associated pulmonary arterial hypertension; CI: cardiac index; IPAH: idiopathic pulmonary arterial hypertension; mPAP: mean pulmonary arterial pressure; mSAP: mean systemic arterial pressure; PVR: pulmonary vascular resistance; RAP: right atrial pressure; SD: standard deviation.
P values were calculated with a t test between the values obtained after NO inhalation and those obtained after sildenafil administration in each diagnosis group.
Safety of vasoreactivity testing
No severe adverse events, such as pulmonary edema, were noted during vasoreactitvity testing with both drugs in the studied patients. Mild adverse effects were observed in response to sildenafil, in the form of systemic hypotension that could be managed by fluid infusion. We defined symptomatic systemic hypotension as a fall in systolic SAP below 90 mmHg and application of fluid infusion, and we found this in 9 patients (4.5%).
Vasoreactivity
Both patient groups showed a significant drop in mPAP and PVR in response to administration of each vasodilator, compared with baseline (Table 2; P < 0.001; P values in comparison to baseline not shown in the table). The mean SAP did not change in response to iNO, but a mild decrease was observed in response to sildenafil. In patients with IPAH, the mean response to sildenafil was significantly stronger than that to NO in terms of right atrial pressure (RAP), CI, and PVR, whereas the changes in mPAP and heart rate did not show significant differences (Table 2). In the APAH group, the mean response to sildenafil was significantly stronger than that to NO for all hemodynamic parameters.
Sixteen (8.1%) of the patients met the responder criteria for NO and 23 (11.6%) for sildenafil (Table 3). It was noted that, of the 16 NO responders, 13 were also sildenafil responders. The highest frequency of NO responders (10.1%) was found among patients with IPAH (Table 4). In patients with APAH, a positive NO response was found less often (6.1%). Responder rates for sildenafil were comparable in IPAH (11.1%) and APAH (12.1%); the highest frequency (18.5%) was found in patients with congenital heart defects.
Response to NO and sildenafil
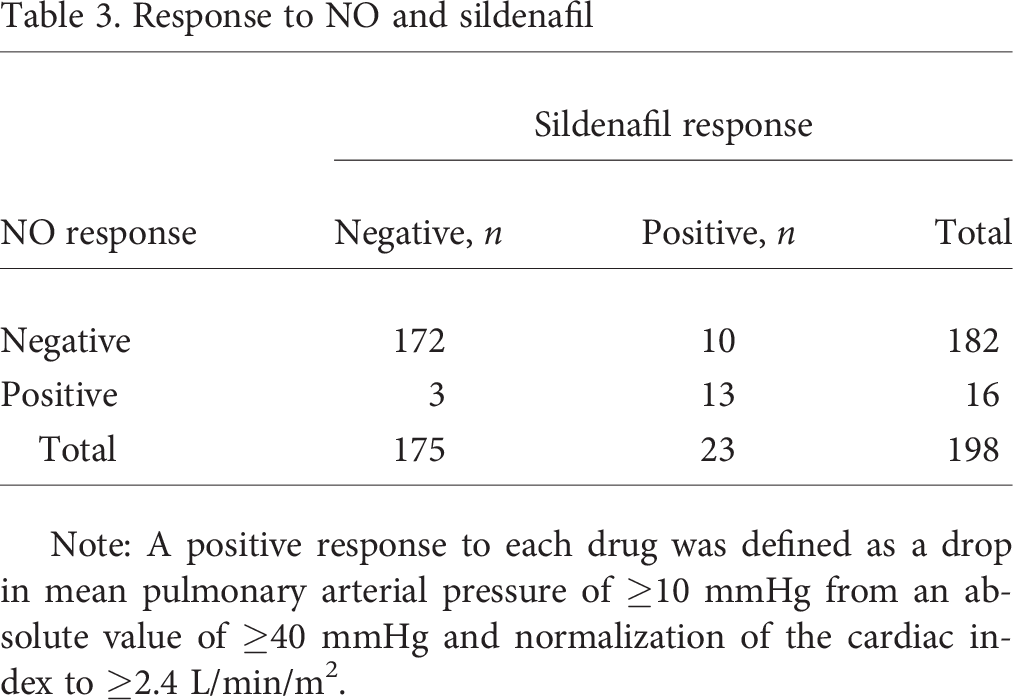
Note: A positive response to each drug was defined as a drop in mean pulmonary arterial pressure of ≥10 mmHg from an absolute value of ≥40 mmHg and normalization of the cardiac index to ≥2.4 L/min/m2.
Response to NO and sildenafil by diagnosis
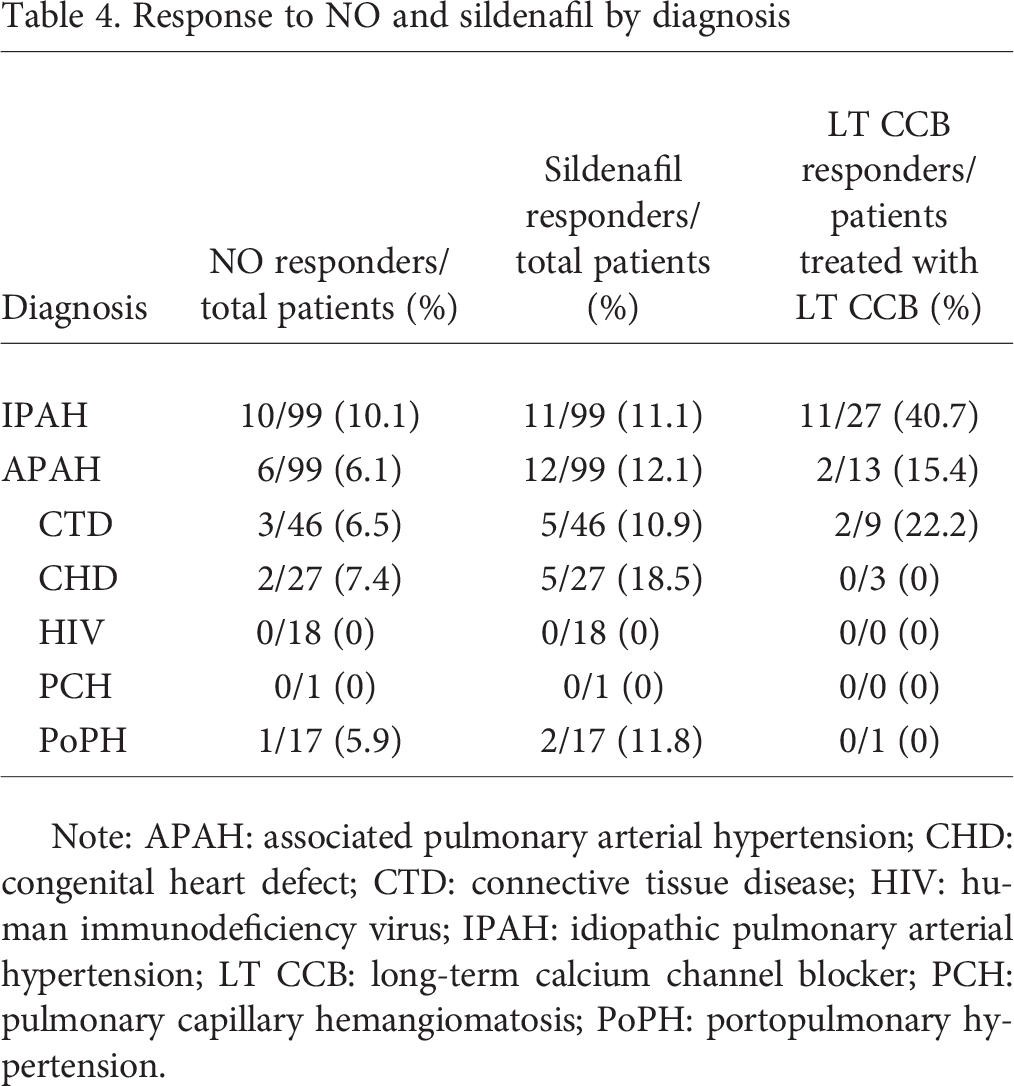
Note: APAH: associated pulmonary arterial hypertension; CHD: congenital heart defect; CTD: connective tissue disease; HIV: human immunodeficiency virus; IPAH: idiopathic pulmonary arterial hypertension; LT CCB: long-term calcium channel blocker; PCH: pulmonary capillary hemangiomatosis; PoPH: portopulmonary hypertension.
Comparing the intraindividual responses to both drugs, we found that the NO-induced decrease in mPAP correlated with the decrease in mPAP after sildenafil administration (Fig. 1A; r = 0.516, P < 0.001). The same was true for the increase in CO in response to both drugs (Fig. 1B; r = 0.521, P < 0.001).
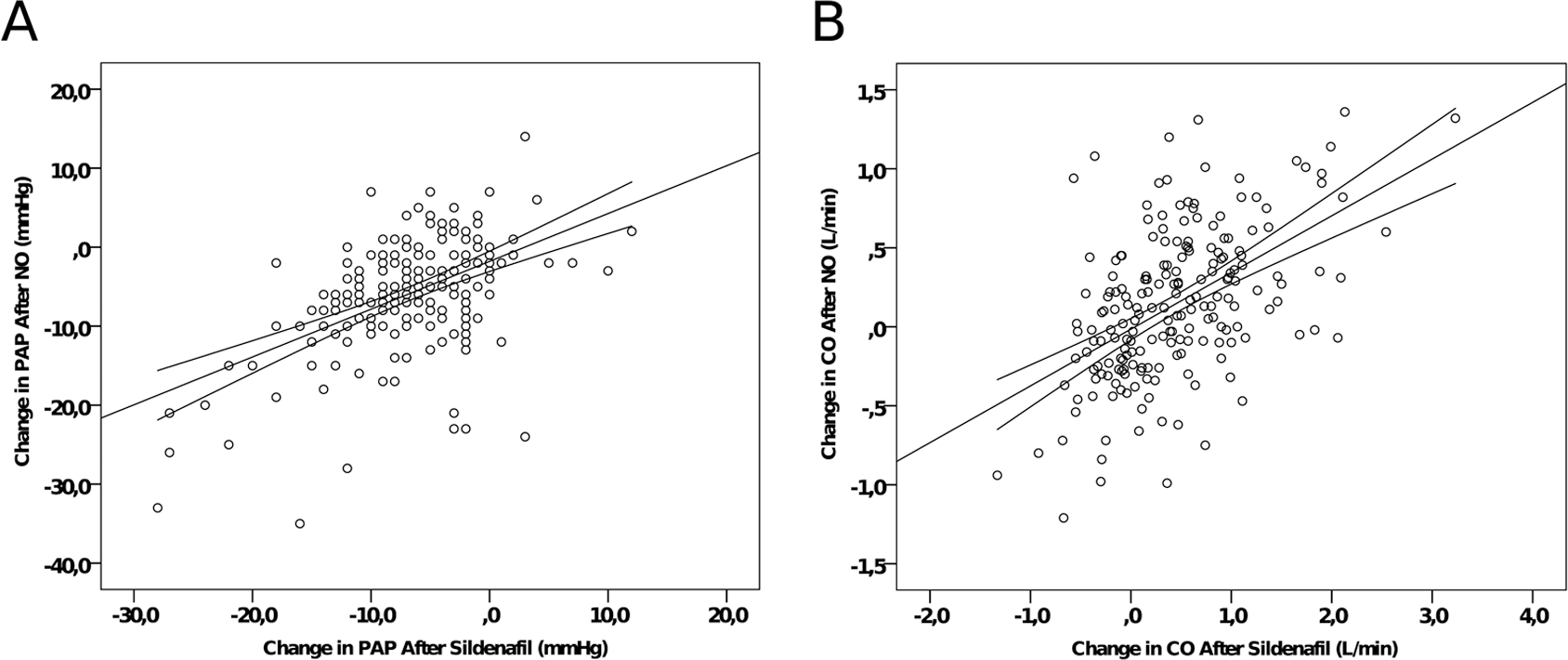
Correlation of hemodynamic responses induced by sildenafil and NO administration. A, For each patient, the change in mean pulmonary arterial pressure (mPAP) in response to sildenafil administration is plotted against the change in mPAP after NO inhalation. The correlation coefficient was r = 0.516, with P < 0.001. B, For each patient, the change in cardiac output (CO) in response to sildenafil is plotted against the change in CO in response to NO. The correlation coefficient was r = 0.521, with P < 0.001.
NO and sildenafil vasoreactivity and long-term CCB response
Therapy with CCBs was started if the patient met the acute vasoreactivity response criteria for NO valid at that time (until 2004, decreases in mPAP and PVR of >20%; from 2005 onward, the current criteria). 16 Therefore, the number of patients starting CCB therapy was greater than the number of patients who met the current NO responder criteria.
Of the 40 patients who received CCBs, 13 (32.5%) were long-term responders (Table 4), the majority of whom (n = 11) had IPAH. Two patients with APAH and a positive long-term response were noted, both of whom had connective tissue disease as the underlying disease.
We then looked at the initial response to vasoreactivity testing in those patients who received long-term CCB therapy and differentiated between long-term responders and nonresponders (according to the predefined criteria of treatment success described in “Methods”). Three of the 13 long-term responders to CCBs were correctly identified by acute vasoreactivity testing with both drugs (sensitivity: 23%; Table 5). The number of false positives—that is, patients who were responders in acute testing but nonresponders to long-term CCBs—was 3 for NO and 4 for sildenafil testing, resulting in a specificity of 88.9% for NO and 85.1% for sildenafil testing.
Cross-tabular comparison between long-term response to CCBs and acute response to nitric oxide and sildenafil
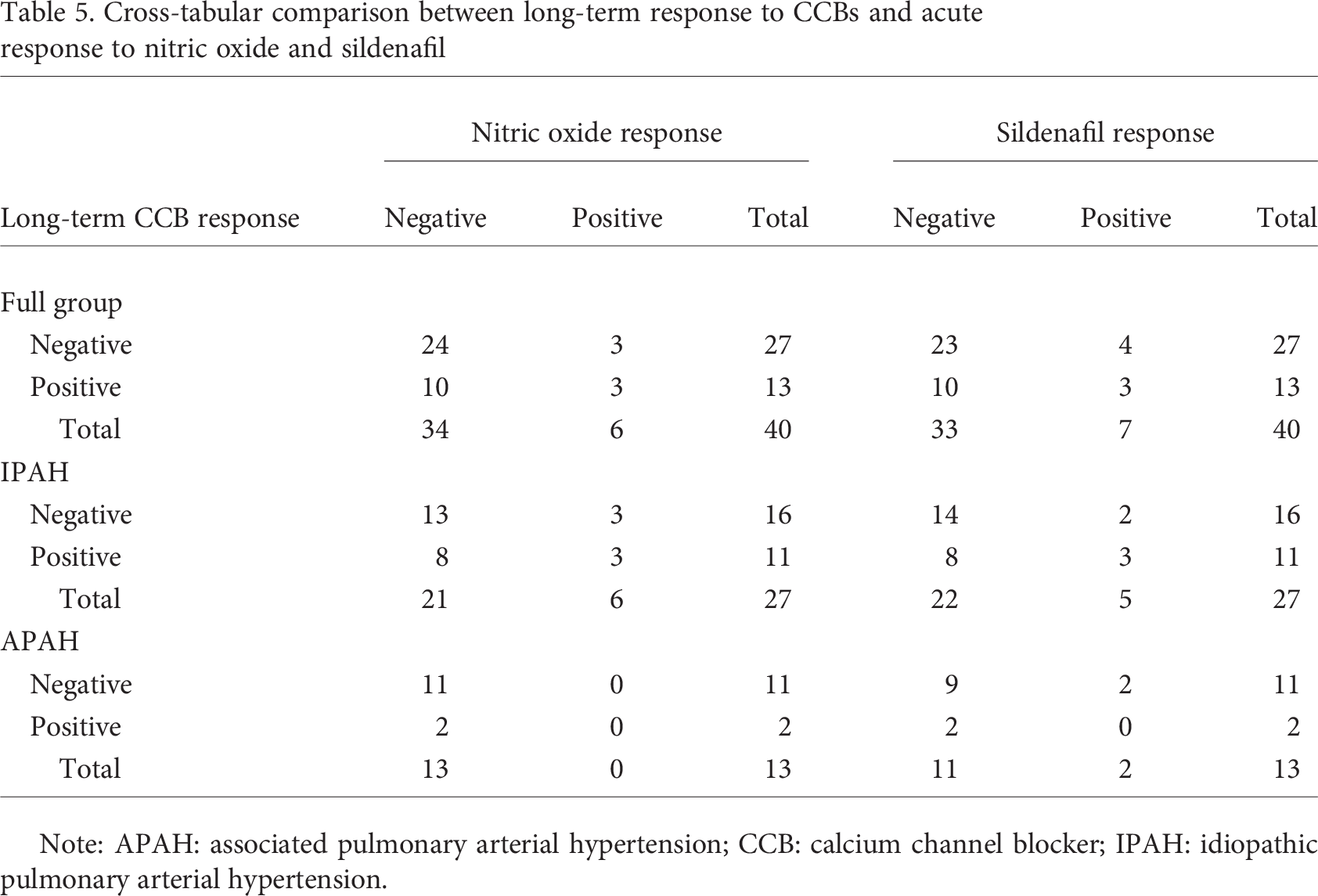
Note: APAH: associated pulmonary arterial hypertension; CCB: calcium channel blocker; IPAH: idiopathic pulmonary arterial hypertension.
We next looked at the potential of NO and sildenafil administration to predict long-term CCB response by the absolute changes in hemodynamic parameters (Table 6). Responders to long-term CCBs exhibited a significantly stronger decrease in mPAP and PVR after NO administration than did nonresponders to long-term CCBs (PmPAP < 0.001, PPVR = 0.001). In sildenafil testing this difference was smaller and nonsignificant.
Comparison of acute hemodynamic responses to NO and sildenafil of long-term responders and nonresponders to CCBs
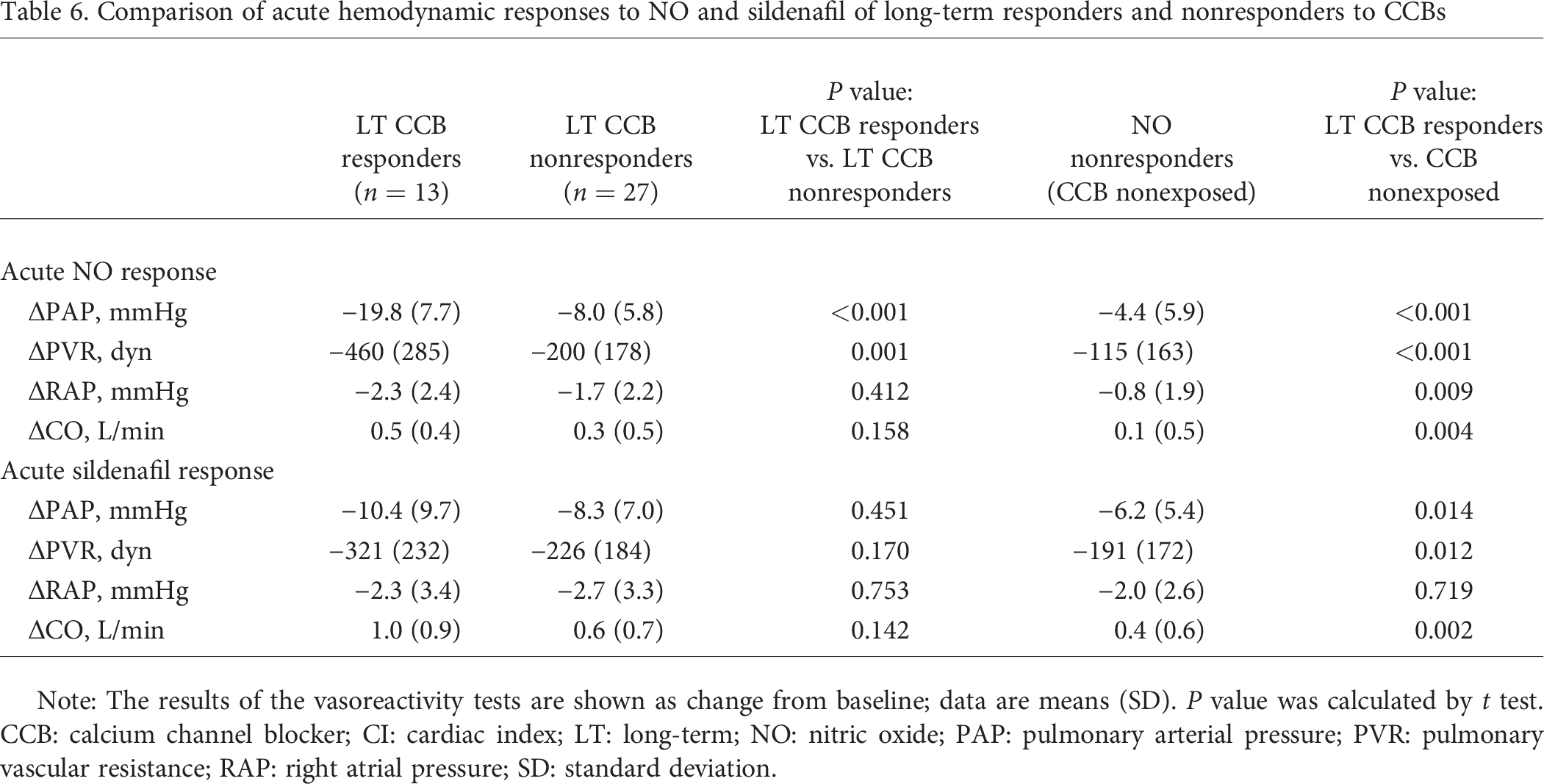
Note: The results of the vasoreactivity tests are shown as change from baseline; data are means (SD). P value was calculated by t test. CCB: calcium channel blocker; CI: cardiac index; LT: long-term; NO: nitric oxide; PAP: pulmonary arterial pressure; PVR: pulmonary vascular resistance; RAP: right atrial pressure; SD: standard deviation.
The receiver operating characteristic curves in Figures S1 and S2 (Figs. S1–S3 available online) confirm that the changes in mPAP and PVR in response to NO are suitable parameters for identifying long-term responders to CCBs (area under the curve: 0.763 and 0.713 for mPAP and PVR, respectively). Logistic regression analysis showed that the decrease of mPAP and the increase of CO after sildenafil and NO administration are independent predictors for long-term CCB response (Table S1, available online). After the patient sample was divided according to the diagnosis, a stable logistic regression model could no longer be built because of the low number of patients.
NO and sildenafil vasoreactivity and survival
A tendency toward better survival was noted for NO responders and sildenafil responders in comparison with nonresponders in the PAH patient sample, but the differences were not statistically significant, irrespective of long-term treatment. The 5-year survival rate was 75% for NO responders, versus 63% for nonresponders. For sildenafil responders the 5-year survival rate was 77%, while it was 62% for nonresponders (Fig. S3).
DISCUSSION
PAH is a severe disease requiring costly and complicated care and treatment. A positive response to acute vasodilator challenge identifies a subgroup of patients in whom mortality is lower than that of the general PAH group and long-term treatment with CCBs, relatively cheap drugs without significant toxicity, is effective. Performing acute vasodilator challenge involves expensive and difficult-to-manage drugs such as iNO or epoprostenol and is therefore currently limited to specialized centers in developed countries. With PAH increasingly recognized as a disease that is common in developing countries, where resources are scarce, a less complex and costly vasoreactivity test is needed. We compared acute vasoresponse to iNO and oral sildenafil in a large cohort of patients with IPAH and APAH and assessed the related prognostic value for prediction of long-term outcomes in this population.
As sildenafil also causes systemic vasodilation and has a half-life of 4 hours, it might induce a higher number or increased severity of adverse effects, compared to iNO. In our study, administration of sildenafil was safe, as no severe adverse effects were observed with 25 mg of sildenafil. The rate of mild adverse events, namely, hypotension that was managed by fluid infusion, was moderate. However, sildenafil was not applied if a patient's systolic SAP was already <90 mmHg. Our patient cohort is comparable to other cohorts of patients with IPAH and APAH in terms of age, female predominance, and severity of elevation of pulmonary arterial pressure.1,17
The previous definition of a positive vasoractivity test (relative drop in mPAP and PVR by at least 20%) has been replaced by the current criteria of a drop in mPAP of >10 mmHg to an absolute value of <40 mmHg and a normalization of CI to a value of ≥2.4 L/min/m2. Under these criteria, the rate of positive acute vasoreactivity to NO in patients with IPAH in our study was 10.1%, which is slightly less than the rate reported in previous studies. 4 This could be due, at least in part, to the application of the more recent response criteria, as opposed to the less strict criteria used in former studies. As shown previously and also in our study, positive vasoreactivity to NO was less frequent in patients with APAH than in patients with IPAH. 17
Our data suggest that sildenafil may also be used for vasoreactivity testing in patients with IPAH, identifying the same number of long-term responders to CCBs as the gold standard iNO when current criteria are used. Moreover, the intraindividual responses to the two drugs were highly correlated, and the specificity to identify long-term CCB responders by vasoreactivity testing was similar with both drugs.
Recently, the intravenous formulation of sildenafil has become available, with the potential of shortening the vasoreactivity testing procedure because of a more rapid onset of action and more reproducible bioavailability than with the oral formulation. Nevertheless, iNO seems more discriminative, as the difference in the acute vasoresponse between long-term CCB responders and nonresponders was larger than that with sildenafil (19.8 vs. 8.0 mmHg for iNO, 10.4 vs. 8.3 mmHg for sildenafil). The rate of positive vasoreactivity was higher for sildenafil than for iNO (11.6% vs. 8.0%). This difference was largely observed in the patients with APAH, who exhibited a clinically significant response to sildenafil but not to iNO. Comparing the intraindividual responses to the two drugs, we have shown that 25 mg of sildenafil exerts a stronger acute effect on all hemodynamic parameters than does iNO in patients with APAH. Similar observations of a more pronounced acute response to sildenafil compared to iNO were made in previous studies using higher doses of iNO and oral sildenafil in patients with PAH10,11 or intravenous sildenafil in patients with chronic thromboembolic pulmonary hypertension. 18 In contrast to our study, those studies were conducted on small numbers of patients and did not evaluate the prognostic value of the vasoreactivity testing. In patients with IPAH, the drop in mPAP was equivalent in response to both drugs, but a significantly stronger response to sildenafil was noted for RAP, PVR, and CI. The reasons for these differences may be found in the pharmacodynamic profiles of the drugs, but they may also reflect a different pathogenesis or state of the underlying disease.
NO is a physiologically produced gas with an extremely short half-life. When inhaled, it is almost 100% pulmonary selective and, through an increase in wedge pressure, may additionally unmask left heart disease as a cause of pulmonary hypertension. 4
The phosphodiesterase-5 inhibitor sildenafil targets the cGMP pathway downstream of NO. Sildenafil exhibits systemic vasodilatory effects, and animal studies suggest that it might have additional long-term effects, beyond vasodilation, that counteract remodeling processes in the heart and vasculature.19,20 Further, there is evidence that phosphodiesterase type 5 inhibitors may directly enhance right ventricular contractility through cGMP-mediated inhibition of phosphodiesterase type 3.21,22
Systemic hypotensive effects of sildenafil might have secondary effects on pulmonary hemodynamics. However, these secondary effects can be recognized by a reflectory increase in heart rate. As heart rate did not increase in response to sildenafil in our study, this does not seem to be a major contributor here.
Even though NO and phosphodiesterase-5 inhibitors target the same pathway, different responses to both substances may be observed within a patient because of the different endogenous activities of NO-synthase and phosphodiesterase-5. It can be speculated, for instance, that in a patient with high basal phosphodiesterase-5 activity and normal endogenous NO production, a strong response to phosphodiesterase-5 inhibitors can be observed, while exogenous NO inhalation is hardly effective. On the other hand, patients with low endogenous phosphodiesterase-5 activity may not respond well to phosphodiesterase-5 inhibitors, whereas they may show a good response to iNO. The downregulation of NO synthase found in some patients with IPAH reported by Giaid and Saleh 23 could provide a clue to this differential responsiveness to agents targeting the same signaling pathways on different levels.
Of note, only 1 in every 3 patients receiving CCB therapy was a long-term responder. In accordance with previous studies, 17 we found that long-term responders to CCBs were almost exclusively patients with IPAH, suggesting that CCB therapy should be started only in these patients. Surprisingly, sensitivity for detection of long-term responders to CCBs by both iNO and sildenafil vasoreactivity testing with the current criteria was low (23% for both substances). Several of the long-term responders to CCBs fulfilled the old, but not the new, criteria or just barely missed them. The current criteria were defined after retrospective analysis of one large, single-center IPAH cohort, 1 but they have not been prospectively evaluated. Hence, the reasons for the low sensitivity of these criteria in our cohort may be diverse. Differences in patients’ characteristics relative to those of the defining cohort could be an explanation for the unsatisfying transferability.
Previous studies have found large differences in the positive predictive value of acute vasoreactivity testing for long-term response to CCB therapy. Jing et al. 24 recently found that acute responsiveness to adenosine infusion and iloprost inhalation successfully predicted long-term CCB response in 9 young patients with IPAH. On the other hand, Barst et al. 25 found that 15 of 31 children who were acute responders did not improve with long-term CCB therapy. From a practical point of view, we suggest that patients with IPAH who fulfill the old or new responder criteria for iNO or sildenafil testing should start CCB therapy with close monitoring. The ability to closely monitor therapeutic response is prerequisite to initiating CCB therapy as, even in patients identified by vasoreactivity testing, the rate of long-term nonresponders may be high. Moreover, vasoreactivity testing remains crucial to identifying nonresponders and saving them from a potentially dangerous trial of CCBs.
It has been suggested that good initial vasoreactivity may identify patients in an earlier disease state or a more benign variant of the disease.2,26,27 Our data indicate that initial vasoreactivity to both iNO and sildenafil, irrespective of the modern specific treatments later applied in the nonresponders, might be of prognostic value for the long-term outcome. However, the difference was not statistically significant for both drugs, possibly because of the low number of patients in the responder group.
Limitations of the study
The main limitation of this study is its retrospective design. A prospective study to confirm the value of the current vasoreactivity criteria for the prediction of long-term CCB response has not yet been conducted and would be desirable. However, with the retrospective data and other treatment options for this fatal disease available, such a study could not be performed for ethical reasons.
Moreover, selection bias cannot be excluded, as only treatment-naive patients who underwent vasoreactivity testing with both iNO and sildenafil were studied. Another limitation of the study, which is due to the low rate of positive vasoreactivity, is the low number of patients in the long-term CCB analyses.
Finally, a systematic bias was inherent to this analysis, as the decision to start long-term CCB treatment was based solely on the hemodynamic criteria achieved with iNO and not those achieved with sildenafil. Therefore, we cannot provide data on the long-term CCB response of patients who responded to sildenafil but not to iNO.
Conclusion
We conclude that sildenafil may serve as a vasoreactivity testing agent in patients with IPAH, even though iNO might be more discriminative and should be preferred because of its pulmonary selectivity and short half-life. Therefore, when sildenafil is used for vasoreactivity testing, the positive predictive value to identify long-term CCB responders should be assessed to provide more evidence for this approach. Given the low number of positive acute responders to NO and the even lower rate of long-term CCB response in patients with APAH, vasoreactivity testing may be dispensable for these patients in terms of CCB trial. Interestingly, our data suggest that acute vasoresponsiveness to sildenafil might be of prognostic value for both IPAH and APAH patients, regardless of the type of PAH-specific treatment.
