Abstract
Reversible lysine acetylation has emerged as a critical mechanism for controlling the function of nucleosomal histones as well as diverse nonhistone proteins. Acetyl groups are conjugated to lysine residues in proteins by histone acetyltransferases and removed by histone deacetylases (HDACs), which are also commonly referred to as lysine deacetylases. Over the past decade, many studies have shown that HDACs play crucial roles in the control of left ventricular (LV) cardiac remodeling in response to stress. Small molecule HDAC inhibitors block pathological hypertrophy and fibrosis and improve cardiac function in various preclinical models of LV failure. Only recently have HDACs been studied in the context of right ventricular (RV) failure, which commonly occurs in patients who experience pulmonary hypertension (PH). Here, we review recent findings with HDAC inhibitors in models of PH and RV remodeling, propose next steps for this newly uncovered area of research, and highlight potential for isoform-selective HDAC inhibitors for the treatment of PH and RV failure.
Heart failure due to systolic and/or diastolic ventricular dysfunction afflicts approximately 6 million Americans, placing an economic burden on the United States that is projected to increase to nearly $100 billion annually by 2030. 1 Most preclinical studies of heart failure focus on the left ventricle (LV) of the heart, because LV failure causes death in the large populations of patients who experience conditions such as ischemic heart disease and resistant systemic hypertension. As such, significantly more is known about the molecular mechanisms governing LV failure than about those associated with right ventricular (RV) failure.
In patients with pulmonary hypertension (PH), restricted blood flow through the pulmonary circulation increases pulmonary vascular resistance and often results in RV failure. Despite recent advances in the treatment of PH, the 5-year mortality rate for individuals with this disease still approaches 50%, highlighting an urgent need for novel therapeutics. 2 Current standards-of-care (SOC) for patients with PH involve the use of vasoactive drugs, including endothelin receptor antagonists, phosphodiesterase-5 inhibitors, and prostacyclins. 3 It is hypothesized that more effective therapeutic strategies will be based on the combined use of vasodilators and agents that target distinct pathogenic mechanisms in PH, such as pulmonary vascular inflammation and fibrosis, as well as aberrant proliferation of smooth muscle cells, endothelial cells, and fibroblasts in the lung vasculature. 4
Importantly, maintenance of RV function is the key determinant of survival in patients with PH, and it is unclear whether SOC therapy for LV failure (e.g., β-blockers and angiotensin-converting enzyme inhibitors) is effective for RV failure. 5 Clearly, increased emphasis needs to be placed on elucidating pathogenic mechanisms in this chamber of the heart.
Multiple small molecule inhibitors of histone deacetylase (HDAC) enzymes have been shown to be efficacious in preclinical models of LV failure, blocking pathological cardiac hypertrophy and fibrosis and improving ventricular function.6,7 However, roles of HDACs in PH and RV failure have only recently been addressed. This review highlights the findings made in these recent studies and emphasizes key issues that need to be rapidly resolved in this compelling and translationally relevant new area of cardiopulmonary research.
HDACs
There are 18 HDACs that are encoded by distinct genes and are grouped into four classes on the basis of similarity to yeast transcriptional repressors (Fig. 1). Class I HDACs (HDAC1, HDAC2, HDAC3, and HDAC8) are related to yeast RPD3, class II HDACs (HDAC4, HDAC5, HDAC6, HDAC9, and HDAC10) are related to yeast HDA1, and class III HDACs (SirT1–7) are related to yeast Sir2. Class II HDACs are further divided into two subclasses, IIa (HDAC4, HDAC5, HDAC7, and HDAC9) and IIb (HDAC6 and HDAC10). HDAC11 falls into a fourth class. 8 Coordination of a zinc ion in the catalytic domains of class I, II, and IV HDACs is required for catalysis. In contrast, class III HDACs (sirtuins) use nicotinamide adenine dinucleotide as a cofactor for catalytic activity. Although class III HDACs will likely be found to regulate pulmonary vascular and RV remodeling, these HDACs will not be discussed further in this review. This is due to the fact that class III HDACs are not inhibited by the small-molecule HDAC inhibitors, such as trichostatin A (TSA), 9 which were used in the preclinical models of PH described below; these inhibitors function by chelating zinc in the active sites of class I, II, and IV HDACs. 10
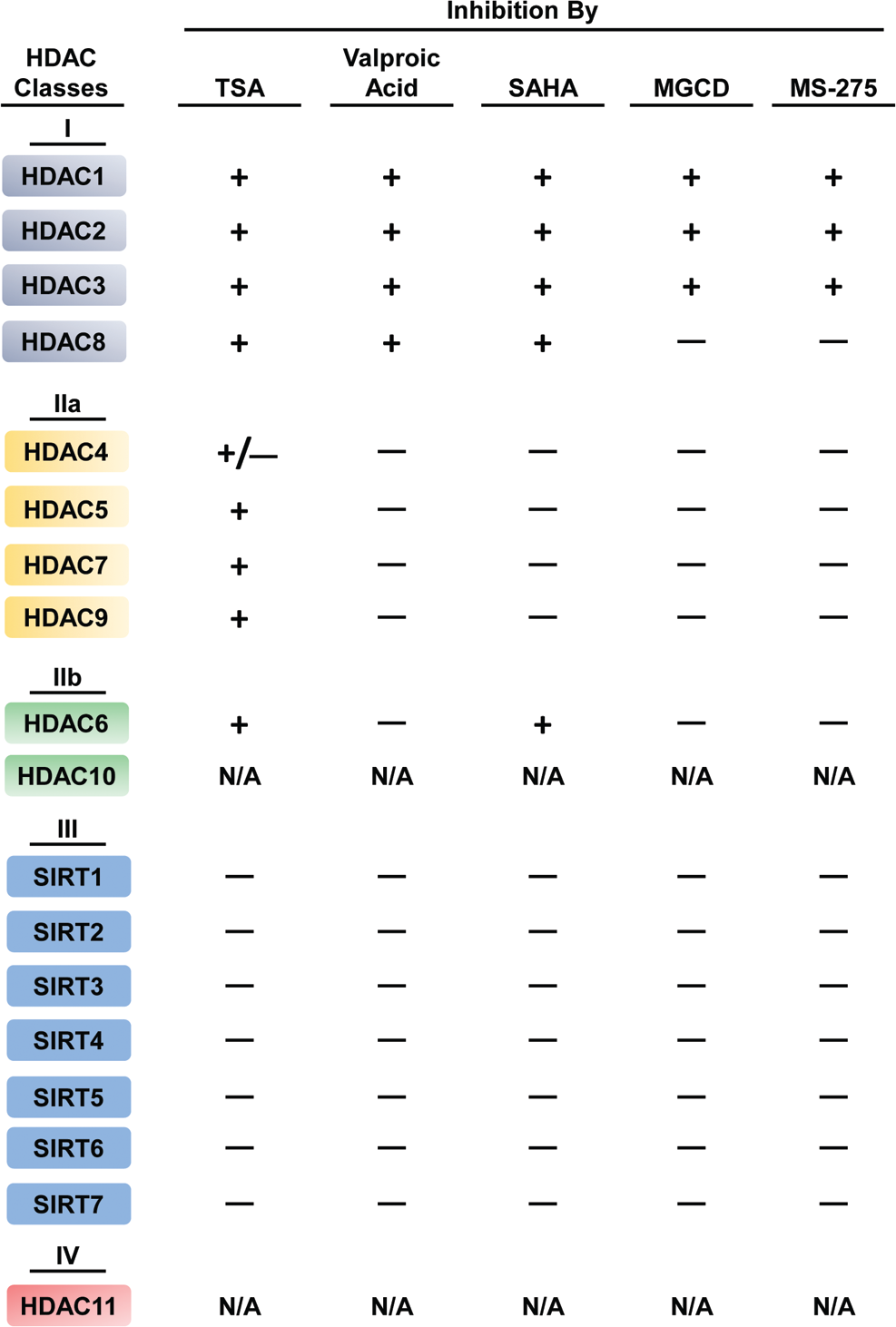
Histone deacetylase (HDAC) isoforms and sensitivity to inhibitors used in preclinical models of pulmonary hypertension and right ventricular remodeling. HDACs fall into four classes. Class II is further subdivided into class IIa and class IIb HDACs. Trichostatin A (TSA) is a broad-spectrum HDAC inhibitor that targets class I and class II HDACs. Suberoylanilide hydroxamic acid (SAHA) inhibits class I and IIb HDACs, whereas valproic acid, MGCD0103 (MGCD), and MS-275 are selective for class I HDACs. Class III HDACs are insensitive to all of the inhibitors shown, and the compounds have not been tested for inhibition of the sole class IV HDAC, HDAC11. N/A: not available; SIRT: sirtuin.
Lysine acetylation was originally thought to primarily control gene expression through effects on nucleosomal histone tails. However, proteomic studies defining the “acetylome” have revealed that thousands of proteins in all cellular compartments are subject to reversible lysine acetylation, and thus it is becoming clear that this posttranslational modification will rival phosphorylation in terms of biological import.11,12
An active area of ongoing research is focused on determining the substrate specificity of distinct HDAC isoforms. In this regard, it is important to note what is known about the subcellular distribution of HDACs. Class I HDACs—especially HDAC1, HDAC2, and HDAC3—are thought to reside primarily in the nucleus, where they serve canonical roles in the control of gene expression through deacetylation of histone tails. These HDACs are present in large multiprotein complexes referred to as Sin3, NuRD, CoREST, and NCoR/SMRT, which are recruited to gene regulatory elements bysequence-specific DNA-binding transcription factors. 13 In general, HDAC1 and HDAC2 are found together in Sin3, NuRD, and CoREST complexes, whereas HDAC3 is a component of the NCoR/SMRT complex. However, it is important to emphasize that this is an oversimplification. For example, HDAC3 has also been found at the plasma membrane, where it regulates Src tyrosine kinase activity, 14 and in cardiac myocytes, HDAC3 has been shown to colocalize with sarcomeres. 15
Compared with the other class I HDACs, very little is known about the role of HDAC8 in the control of gene expression, and it is unclear whether HDAC8 is even able to deacetylate histones in vivo. 16 However, HDAC8 has been shown to interact with the estrogen-related receptor α 17 and cyclic adenosine monophosphate response element-binding protein 18 transcription factors, suggesting a role for this HDAC in the control of gene expression. HDAC8 can also be found in the cytoplasm, where it has been shown to interact with α-smooth muscle actin and promote smooth muscle cell contraction, 19 and HDAC8 is able to deacetylate cytoplasmic heat shock protein 20. 20
Class IIa HDACs (HDAC4, HDAC5, HDAC7, and HDAC9) have several unique features. 21 First, these HDACs have long (˜500-amino acid) amino-terminal extensions, which harbor binding sites for transcription factors and cofactors. For example, all class IIa HDACs are able to bind to the myocyte enhancer factor 2 (MEF2) transcription factor by virtue of a conserved 18-amino acid MEF2 binding domain in their amino-terminal extensions.22–26 In muscle cells, binding of class IIa HDACs to MEF2 results in suppression of MEF2 target genes that govern cellular growth and differentiation.27,28 Second, class IIa HDACs undergo signal-dependent nuclear export upon phosphorylation of two serine residues within their amino-terminal extensions. Phosphorylation of these sites by kinases, such as protein kinase D (PKD) or calcium/calmodulin-dependent protein kinase (CaMK), creates docking sites for the 14-3-3 chaperone protein.29–37 The 14-3-3 binding masks the class IIa HDAC nuclear localization signal and activates a cryptic nuclear export signal in these HDAC isoforms. Thus, in response to PKD/CaMK signaling, class IIa HDACs are exported from the nucleus, freeing MEF2 to activate downstream target genes. Third, despite have conserved catalytic domains, class IIa HDACs are unable to deacetylate histones. 38 In fact, bona fide substrates of class IIa HDACs have yet to be identified, and class IIa HDAC catalytic activity can only be monitored using an artificial substrate. 39 Fourth, class IIa HDAC catalytic activity is largely resistant to commonly used HDAC inhibitors, including the compounds used in the preclinical PH models. The exception is TSA, which inhibits HDAC5, HDAC7, and HDAC9 (Fig. 1).
Class IIb HDACs, particularly HDAC6, are highly sensitive to most HDAC inhibitors (Fig. 1). HDAC6 contains two deacetylase domains and resides primarily in the cytoplasm, where it is known to deacetylate tubulin, heat shock protein 90, and the F-actin binding protein, cortactin. 40 One well-documented role for HDAC6 is in the control of misfolded protein clearance via autophagy.41–44 Deacetylation of tubulin by HDAC6 promotes transport of misfolded protein aggregates (aggresomes) to lysosomes, where they are degraded; HDAC6 associates with ubiquitinated proteins within aggresomes through a carboxyterminal ubiquitin-binding domain. Roles for HDAC6 in the heart or pulmonary vasculature have yet to be uncovered, although HDAC6 catalytic activity was shown to be elevated in RVs of rats exposed to chronic hypoxia or hypoxia plus the VEGF receptor-inhibitor SU5416. 45 The other class IIb HDAC, HDAC10, and the lone class IV HDAC, HDAC11, remain poorly characterized, in part due to the inability to effectively monitor their catalytic activity using in vitro assays. 10 As such, it is unclear whether existing HDAC inhibitors, including those used in PH models (below), target these HDAC isoforms.
HDAC INHIBITORS
Most HDAC inhibitors possess a zinc-binding “warhead” group that docks in the active site, a linker, and a surface recognition domain that interacts with residues near the entrance to the active site. HDAC inhibitors are typically grouped into four classes: hydroxamic acids (e.g., suberanilohydroxamic acid [SAHA]), short-chain fatty acids (e.g., valproic acid [VPA]), benzamides (e.g., MGCD0103), and cyclic peptides (e.g., FK-228). Relative potencies and selectivity profiles differ between and within these classes (Fig. 1). 10 The strong zinc-chelating properties of the hydroxamic acid warhead produce potent (low nanomolar) “pan-HDAC inhibitors,” although these compounds only weakly inhibit class IIa HDACs. 10 In contrast, the short-chain fatty acids, such as VPA, are weak (millimolar) HDAC inhibitors that possess selectivity toward class I HDACs (HDAC1, HDAC2, HDAC3, and HDAC8). 46 Benzamide HDAC inhibitors are generally highly selective for HDAC1, HDAC2, and HDAC3. The cyclic peptide FK-228 is an extremely potent HDAC inhibitor that is able to suppress the catalytic activity of all zinc-dependent HDACs tested, including class IIa HDACs. 10
Two HDAC inhibitors, SAHA (vorinostat) and FK-228 (romidepsin), are approved for use in humans with cutaneous T cell lymphoma. These compounds are generally well tolerated, with the most notable adverse effects being thrombocytopenia, nausea, and fatigue. VPA has been used in the clinic for decades as an anticonvulsant and mood stabilizer. It is important to note that, in addition to being an HDAC inhibitor, VPA can influence ion channels, kinases, and other biochemical pathways. 47 As such, in experimental settings, it is difficult to attribute effects of VPA solely to inhibition of HDAC activity.
It is hypothesized that isoform-selective HDAC inhibition has the potential to provide superior efficacy with a greater safety profile than pan-HDAC inhibition. 48 In this regard, recent medicinal chemistry has led to the discovery of compounds with even greater selectively for certain HDAC isoforms. For example, compounds containing aryl substitutions on the benzamide warhead have recently been found to be highly selective for class I HDAC1 and HDAC2 over all other HDACs.49–52 Conversely, other scaffolds appear to be selective for HDAC3,53,54 and several selective inhibitors of HDAC8 have been developed.55,56 The first known HDAC6/class IIb-selective inhibitor, tubacin, was described in 2003. 57 More recent compounds, such as tubastatin A, 58 exhibit greater selectivity for HDAC6 than tubacin. Finally, the first potent and highly selective class IIa HDAC inhibitors were recently described. 59 Together, these isoform-selective HDAC inhibitors will serve as powerful chemical biological probes to discover novel HDAC substrates and dissect the roles of distinct HDACs in various pathophysiological processes. Additionally, isoform-selective HDAC inhibitors could promote development of HDAC inhibitor-based therapies that are better tolerated by humans than vorinostat and romidepsin.
HDAC INHIBITORS IN MODELS OF LV FAILURE
In vivo studies have demonstrated that HDAC inhibitors can effectively halt and even reverse LV hypertrophy (Fig. 2). Treatment with TSA or VPA for 2 weeks blocked the development of cardiac hypertrophy in transgenic mice that overexpress the serum response factor inhibitor, Hop, in the heart. 60 Similarly, TSA and VPA suppressed LV hypertrophy induced by infusion of angiotensin II or pressure-overload due to transverse aortic constriction. 61
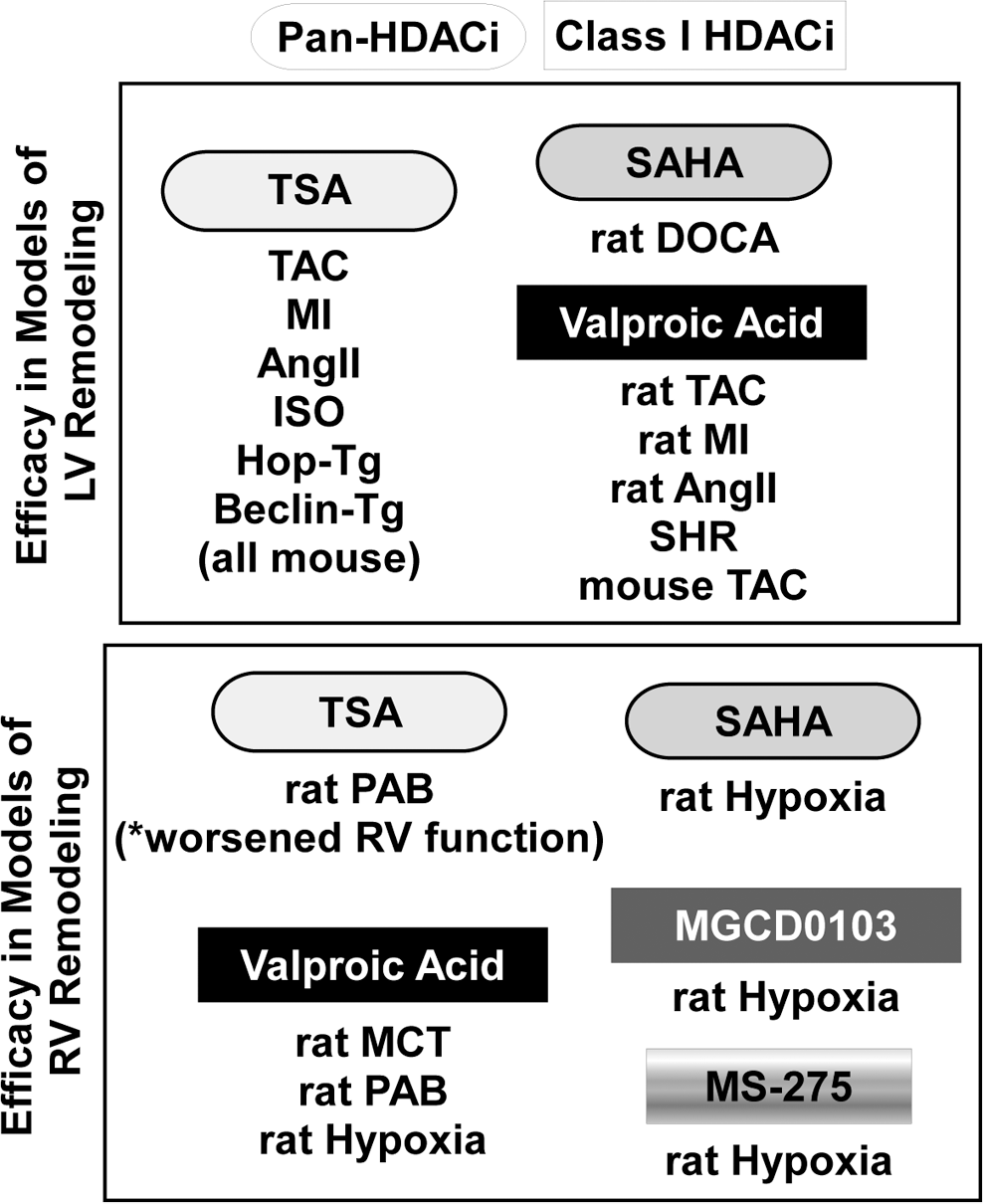
Efficacy of histone deacetylase (HDAC) inhibitors in models of left ventricular (LV) and right ventricular (RV) remodeling. Pan- and class I HDAC inhibitors have been tested in a variety of rodent models of LV and RV dysfunction. With one exception (trichostatin A [TSA] in the rat pulmonary artery banding [PAB] model), HDAC inhibitors have exerted beneficial effects in the heart. Ang II: angiotensin II; DOCA: deoxycorticosterone acetate; Hop: homeodomain only protein; ISO: isoproterenol; MCT: monocrotaline; MI: myocardial infarction; SAHA: suberoylanilide hydroxamic acid; SHR: spontaneously hypertensive rat; TAC: transverse aortic constriction; Tg: transgenic.
TSA treatment was also shown to regress established LV hypertrophy in mice subjected to aortic constriction, 61 and it reversed established atrial fibrosis in Hop-transgenic mice, 62 suggesting potential for HDAC inhibitors for the treatment of preexisting LV failure. Consistent with this, Hill and colleagues convincingly demonstrated that TSA reverses established LV hypertrophy in Beclin 1 transgenic mice subjected to pressure overload. 63 Beclin 1 is an autophagy effector, and the authors conclude that part of the mechanism by which HDAC inhibitors block LV hypertrophy is through suppression of autophagic flux. This was an extension of the group's earlier work showing that 3 weeks of treatment with TSA and another hydroxamic acid HDAC inhibitor, scriptaid, blunted LV hypertrophy in a pressure-overload mouse model, reducing cardiomyocyte size and significantly improving ventricular performance. 64 HDAC inhibitors have also been shown to reduce cell death and prevent maladaptive LV remodeling in rodent models of myocardial ischemia65–68 and in the setting of chronic hypertension in rats.69,70
It is likely that HDAC inhibitors block LV hypertrophy through multiple mechanisms in addition to suppression of autophagy. For example, we recently showed that class I HDAC–selective inhibitors derepress the gene encoding DUSP5, an ERK1/2-specific phosphatase. 71 As such, prohypertrophic ERK signaling is dampened in HDAC inhibitor–treated cardiomyocytes. HDAC inhibitors have also been shown to stimulate expression of an antihypertrophic transcription factor, Krüppel-like factor 4 (KLF4). Pan-HDAC inhibitors increase expression of KLF4 in cultured cardiomyocytes, and the resulting increase in KLF4 protein is sufficient to block agonist-dependent hypertrophy of the cells. 72 When thinking about HDAC inhibitor actions in the heart, an analogy to microRNA (miR) therapeutics can be drawn, because both strategies target multifactorial pathways rather than discrete pathogenic nodes.
HDAC INHIBITORS IN MODELS OF PH AND RV HYPERTROPHY
Recent articles have addressed the role of HDACs in PH and RV remodeling (Fig. 2). Cho et al. 73 tested VPA, which selectively targets class I HDACs, for efficacy in a rat model of monocrotaline (MCT)-induced PH and RV hypertrophy in ˜4-week-old Sprague Dawley (SD) rats. These same investigators tested VPA in a rat model of pressure-overload RV hypertrophy mediated by pulmonary artery banding (PAB), also in 4-week-old SD rats. VPA was delivered via drinking water, concomitant with initiation of MCT or PAB, and RV hypertrophy was assessed after 3 weeks; increased histone acetylation in RVs of VPA-treated rats confirmed that the compound was efficiently exposed in the tissue of interest. VPA effectively reduced RV hypertrophy in both studies, as determined by echocardiographic assessment of RV wall thickness and quantification of RV mass at the time of necropsy. Echocardiography also revealed that VPA improved RV systolic function (ejection fraction) in animals subjected to MCT or PAB. However, it should be noted that echocardiographic assessment of RV function is notoriously difficult to achieve, 74 and thus pressure-volume analyses with an invasive catheter should also be performed in the future. In addition, the authors did not address whether VPA reduced PH in MCT-treated rats, which would obviously influence the RV hypertrophic response. Nonetheless, these studies were the first to implicate HDACs in the control of RV hypertrophy.
Bogaard et al. 75 performed an exhaustive study with TSA in male SD rats subjected to PAB. These investigators used a protocol in which the initial constriction of the pulmonary artery was mild; however, animal growth over the subsequent 6 weeks resulted in a progressive increase in RV systolic pressure and significant RV hypertrophy. This procedure does not result in RV failure. 76 Four weeks after PAB surgery, animals were given TSA via intraperitoneal injection for 5 days per week for 2 weeks. TSA did not suppress RV hypertrophy, and strikingly, treatment with this pan-HDAC inhibitor worsened RV function, as revealed by reduced cardiac output and increased RV dilatation. TSA treatment in the setting of PAB was also associated with exaggerated RV fibrosis, increased numbers of apoptotic cells in the RV, and capillary rarefaction in the RV.
Bogaard et al. 75 hypothesized that the deleterious effects of TSA on the RV are due, at least in part, to its ability to reduce capillary density in the chamber of the heart. Indeed, HDAC inhibitors have been shown to elicit antiangiogenic effects through suppression of VEGF signaling in cancer models.77,78 To provide mechanistic insight into the observed reduction in RV capillary density, the authors performed in vitro studies with cultured human cardiac microvascular endothelial cells and discovered that TSA reduced expression of several angiogenic factors in these cells, including VEGF and angiopoietin-1. Using RNA interference to knockdown expression of individual HDACs in mouse cardiac microvascular endothelial cells, it was determined that class II HDACs, particularly HDAC6, promote VEGF messenger RNA expression in these cells. Importantly, suppression of class I HDAC expression failed to reduce VEGF levels.
Supplemental data from Bogaard et al. 75 described effects of VPA in the rat PAB model. Importantly, although VPA appeared to cause a mild increase in RV inner diameter during diastole, it did not increase fibrosis or reduce capillary density; details regarding VPA dosing regimen were not provided. Because VPA only inhibits class I HDACs, these results suggest that isoform-selective HDAC inhibition will be better tolerated in the setting of PH and RV hypertrophy than nonselective pan-HDAC inhibition with compounds such as TSA.
We performed studies with the benzamide class I HDAC inhibitors, MGCD0103 and MS-275, 79 which are highly selective for class I HDACs (HDAC1, HDAC2, and HDAC3). 10 Ten-week-old male SD rats were subjected to hypobaric hypoxia and treated with vehicle control, MGCD0103, or MS-275 every other day for 3 weeks. Both class I HDAC inhibitors were well tolerated and were shown to effectively suppress class I HDAC catalytic activity in RV and lung. Both compounds blunted hypoxia-induced PH as well as pulmonary vascular smooth muscle cell proliferation and medial thickening. Importantly, exhaustive pressure-volume analyses of rat RVs after 3 weeks of class I HDAC inhibitor treatment failed to reveal any decrement in RV contractile function. Likewise, biochemical and histological analyses of RVs failed to reveal HDAC inhibitor-mediated apoptosis. These findings further suggest that isoform-selective HDAC inhibitors will be well tolerated in the setting of PH.
Surprisingly, class I HDAC inhibition only modestly decreased RV hypertrophy. 79 In this regard, it is important to note that RV hypertrophy per se is not deleterious, because it serves to reduce wall stress in the face of elevated afterload. It will be important to determine whether class I HDAC inhibitors suppress the transition from RV hypertrophy to chamber dilation and pump failure.
Together with Zhao and colleagues,80,81 we showed that VPA and the pan-HDAC inhibitor, SAHA, can reverse existing PH and RV hypertrophy in male SD rats exposed to normobaric hypoxia. Rats were housed under hypoxic conditions for 2 weeks before HDAC inhibitor treatment, via drinking water, for 2 additional weeks; immunoblotting confirmed that HDAC inhibitor treatment increased histone acetylation in the lungs. Reduced PH in HDAC inhibitor-treated rats was again associated with diminished muscularization of pulmonary arterioles and induction of antiproliferative genes in the lungs. HDAC inhibitor treatment was well tolerated by the rats. However, it should be noted that RV function was not evaluated in these studies, and thus an adverse effect of pan-HDAC inhibition with SAHA on the RV cannot be ruled out.
MECHANISMS OF ACTION OF HDAC INHIBITORS IN PH
The beneficial effects of HDAC inhibitors in PH models relate, in part, to their ability to block abnormal proliferation of pulmonary vascular cells. The class I HDAC inhibitor MGCD0103 reduced hypoxia-induced medial thickening of lung arterioles through a mechanism involving suppression of smooth muscle cell proliferation. 79 In vivo and in cultured pulmonary artery smooth muscle cells, MGCD0103 stimulated expression of antiproliferative factors, such as Fox03a and the cyclin-dependent kinase (CDK) inhibitor, p27. 79 Consistent with this, in a separate study, both SAHA and VPA were shown to stimulate the p21 CDK in lungs of chronically hypoxic rats, and this was associated with reduced pulmonary arteriolar muscularization. 80 HDAC inhibitors also reduced expression of the antiapoptotic protein BCL-2 in these rats, which suggests that HDAC inhibition blocks pulmonary vascular remodeling by concomitantly suppressing cell proliferation and promoting cell death.
Studies with cultured cells have begun to reveal the molecular mechanisms by which HDAC inhibitors impact pulmonary vascular cells. Pulmonary artery cells from calves with PH due to chronic hypoxia have been invaluable for these studies. Cells with high proliferative capacity can be isolated from both the adventitia (PH fibroblasts) and media (R cells) of the bovine vessels. Strikingly, these cells maintain a hyperproliferative phenotype over many passages in culture, which suggests a role for epigenetics in this process, because, by definition, epigenetic events are heritable. We found that class I HDAC expression and activity are dramatically elevated in PH fibroblasts and R cells, and selective class I HDAC inhibitors (VPA and apicidin) block the ability of both cell types to proliferate.80,82 Once again, the antiproliferative action of class I HDAC inhibitors in PH fibroblasts and R cells was associated with induction of FoxO3a and p21. Importantly, HDAC inhibitors were able to block pulmonary vascular cell proliferation at doses that did not alter cell viability.
Inflammation is increasingly appreciated to play an important role in the pathogenesis of PH. 83 Vascular remodeling in PH is characterized by accumulation of activated monocytes and macrophages in the pulmonary vascular adventitia.84,85 Our recent findings demonstrated that perivascular inflammation in PH is perpetuated by activated adventitial fibroblasts (PH fibroblasts), which, through sustained production of proinflammatory cytokines and chemokines and adhesion molecules (including monocyte chemoattractant protein 1 [MCP-1], stromal cell-derived factor 1, interleukin 6, and vascular cell adhesion protein 1), induce accumulation, retention, and activation of monocytes and macrophages. We showed that HDAC inhibitors (e.g., SAHA and apicidin) markedly reduced proinflammatory activation of PH fibroblasts and their ability to induce monocyte migration and retention, which suggests that activated proinflammatory phenotype of PH fibroblasts was due, at least in part, to epigenetic modifications involving HDACs. 82
More recently, the efficacy of HDAC inhibitors in PH fibroblasts was linked to induction of miR-124. 86 miR-124 had previously been shown to have antiproliferative action in glioblastoma cells. 87 In cultured PH fibroblasts (both human and bovine), miR-124 expression was found to be dramatically downregulated. Upon treatment with class I HDAC inhibitors, miR-124 was derepressed, which resulted in reduced expression of the miR-124 target, polypyrimidine tract binding protein 1 (PTBP1), and reversal of the hyperproliferative and proinflammatory phenotype of PH fibroblasts. 86 PTBP1 was found to downregulate expression of p21 and FoxO3a in PH fibroblasts. Interestingly, miR-124 was also found to directly regulate expression of the potent inflammatory chemokine, MCP-1 (CCL2). Together, this work defined a class I HDAC/miR regulatory circuit that controls aberrant proliferation and proinflammatory effects of pulmonary vascular cells in response to cues for PH (Fig. 3).
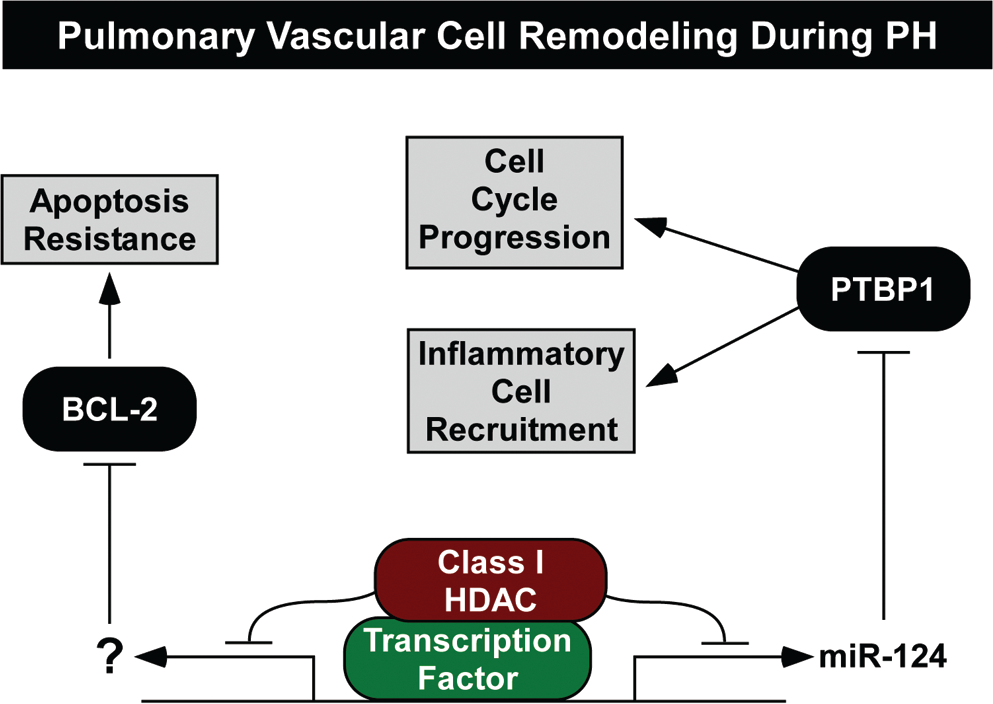
Model for inhibition of aberrant pulmonary vascular cell proliferation and inflammation by histone deacetylase (HDAC) inhibitors. Class I HDACs inhibit expression of microRNA-124 (miR-124) in the setting of pulmonary hypertension (PH). miR-124 normally blocks expression of polypyrimidine tract binding protein 1 (PTBP1), which positively regulates genes involved in cell cycle progression and inflammation. Class I HDAC inhibition leads to derepression of miR-124 expression, resulting in suppression of PTBP1. Class I HDACs also confer resistance of pulmonary vascular cells to apoptosis by promoting expression of the anti-apoptotic protein BCL-2. It is proposed that class I HDAC inhibition stimulates expression of a pro-apoptotic factor that suppresses BCL-2 expression.
Inflammatory mechanisms are also implicated in the RV dysfunction that characterizes PH. 88 Although the roles of class I HDACs in RV cardiomyocytes remain largely un-characterized, at least part of the mechanism for the beneficial effect of class I HDAC inhibition on the RV appears to be governed via suppression of inflammation. 79
CONCLUSIONS
The initial findings with HDAC inhibitors in models of PH and RV hypertrophy highlight a previously underappreciated role for lysine acetylation in the control of pathological cardiopulmonary remodeling. There is a clear need for additional investigation to better understand the mechanistic underpinnings of HDAC inhibitor action in preclinical models of PH and RV hypertrophy and the relevant HDAC isoforms.
Several questions need to be addressed. For example, can an adequate therapeutic index be achieved with an HDAC inhibitor to warrant testing in patients with PH? For these studies, it will be essential to test multiple isoform-selective HDAC inhibitors and confirm the pharmacodynamic actions of the compounds (i.e., confirm that the compounds got to the lungs and RV and selectively inhibited specific HDAC isoforms in these tissues). Furthermore, given the demonstration that TSA actually worsened RV function in the setting of PAB,75,89 it will be critical to determine whether this is due to general HDAC inhibition with TSA or whether this is a consequence of off-target action of TSA. To address this issue, multiple pan- and isoform-selective HDAC inhibitors must be tested in the PAB model. It will also be essential to determine whether class I HDAC inhibitors are able to reverse existing PH and RV dysfunction. The rat Sugen/hypoxia model of severe angioproliferative PH is ideally suited to address this question. With regard to class I HDAC inhibition, MGCD0103 and MS-275 inhibit HDAC1, HDAC2, and HDAC3. It will be important to determine whether these HDAC isoforms function redundantly in the control of PH and RV remodeling, or whether selective inhibition of HDAC1, HDAC2, or HDAC3 is sufficient to confer benefit. Such experiments are now feasible because of the recent discovery of even more selective HDAC inhibitors. 48 Finally, little is known about molecular mechanisms for regulation of pulmonary vascular and RV remodeling by HDACs. Do HDACs function nongenomically to control acetylation of proteins that control signaling events in the cardiopulmonary axis? Answers to these questions should be rapidly forthcoming and could dramatically impact future efforts to treat patients with PH and RV failure.
Footnotes
Conflict of Interest: None declared.
