Abstract
Pressure overload of the heart, such as seen with pulmonary hypertension and/or systemic hypertension, can result in cardiac hypertrophy and the eventual development of heart failure. The development of hypertrophy and heart failure is accompanied by numerous molecular changes in the heart, including alterations in cardiac energy metabolism. Under normal conditions, the high energy (adenosine triphosphate [ATP]) demands of the heart are primarily provided by the mitochondrial oxidation of fatty acids, carbohydrates (glucose and lactate), and ketones. In contrast, the hypertrophied failing heart is energy deficient because of its inability to produce adequate amounts of ATP. This can be attributed to a reduction in mitochondrial oxidative metabolism, with the heart becoming more reliant on glycolysis as a source of ATP production. If glycolysis is uncoupled from glucose oxidation, a decrease in cardiac efficiency can occur, which can contribute to the severity of heart failure due to pressure-overload hypertrophy. These metabolic changes are accompanied by alterations in the enzymes that are involved in the regulation of fatty acid and carbohydrate metabolism. It is now becoming clear that optimizing both energy production and the source of energy production are potential targets for pharmacological intervention aimed at improving cardiac function in the hypertrophied failing heart. In this review, we will focus on what alterations in energy metabolism occur in pressure overload induced left and right heart failure. We will also discuss potential targets and pharmacological approaches that can be used to treat heart failure occurring secondary to pulmonary hypertension and/or systemic hypertension.
Keywords
Heart failure is the progressive deterioration in cardiac function and is the leading cause of morbidity and mortality in developed countries. 1 It affects over 5 million Americans, and 600,000 new cases are diagnosed each year. 2 Heart failure is clinically defined as “a complex clinical syndrome that can result from any structural or functional cardiac disorder that impairs the ability of the ventricle to fill with or eject blood.” 3 Heart failure can develop due to a wide variety of causes, including ischemic heart disease, viral/bacterial myocarditis, and cardiomyopathies as well as pressure and volume overload due to long-standing hypertension, valvular diseases, or pulmonary artery hypertension. 4 Pulmonary arterial hypertension can be idiopathic or occur secondary to conditions such as left heart failure, lung disease, hypoxia, or thromboembolism and is associated with a poor clinical outcome. 5
Regardless of the initiating cardiac abnormality, the syndrome of heart failure represents a complex clinical picture, including abnormal myocardial contractility, altered hemodynamics, ventricular remodeling, and neurohumoral activation. 6 Currently β-blockers, angiotensin converting enzyme inhibitors (ACEI), angiotensin receptor blockers (ARBs), nitrites, digoxin, aldosterone antagonists, implantable cardioverter-defibrillators, cardiac resynchronization therapy, left ventricular assist devices, and heart transplantation are available approaches to treat and manage heart failure. 7 The current management of right ventricular failure, which includes the use of digoxin, furosemide, inotropes, prostacyclin derivatives, endothelin receptor antagonists, and phosphodiesterase inhibitors, is largely empirical.8,9 These treatments focus largely on modifying hemodynamic and neurohormonal pathways. 10 Although current treatment strategies delay or lessen the worsening of heart failure, the prognosis of patients with heart failure remains poor.5,11–13 The 1-year and 5-year mortalities are 20% and 50% respectively. 14 The cost of managing patients with heart failure in the United States is approximately $39 billion. 1 Therefore, it is important to develop novel therapeutic approaches to treat heart failure.
In the failing heart, the structure of cardiomyocytes can be relatively well preserved despite significant contractile functional impairment. 10 This impairment in contractile function is partly due to alterations in energy substrate metabolism and alterations in enzymatic pathways that regulate energy metabolism in the heart. 15 Because the myocardium is viable but dysfunctional, 16 targeting energy metabolism to treat heart failure is a potential new treatment strategy. Therefore, targeting cardiac metabolism as an approach to treat heart failure has recently received considerable interest.
This article will focus on what alterations in cardiac energy metabolism occur in pressure overload–induced heart failure and the therapeutic approaches to normalize energy balance, with the aim of preventing the progression from compensated cardiac hypertrophy to decompensated heart failure.17–20
CARDIAC ENERGY METABOLISM
The heart has a very high energy demand, with more than 95% of this energy demand being met by adenosine triphosphate (ATP) derived from mitochondrial oxidative phosphorylation and the rest from glycolysis.21,22 In an adult heart, 60%–90% of the ATP is derived from oxidation of fatty acids, whereas 10%–40% is generated from glucose oxidation (Fig. 1). Glycolysis and lactate oxidation make up the majority of the remaining contribution.
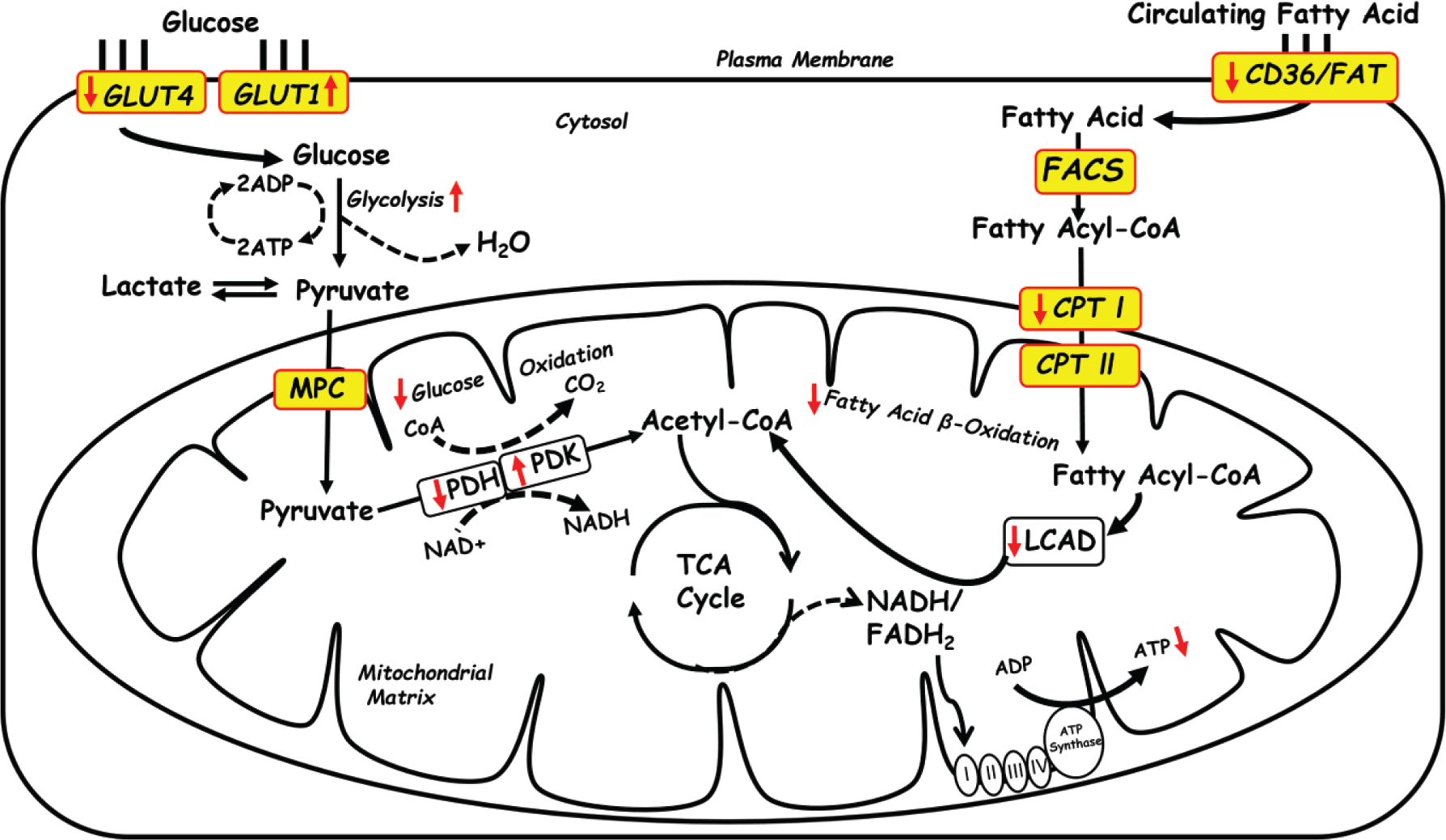
Alterations in myocardial energy substrate metabolism in heart failure. In the normal heart, fatty acids and glucose serve as the primary energy substrates to produce adenosine triphosphate (ATP) via oxidation. In the failing heart, decreases in fatty acid and glucose oxidation lead to energy deficit. Decreases in fatty acid oxidative enzymes contribute to decreases in fatty acid oxidation, whereas decreases in the glucose transporter GLUT4 and pyruvate dehydrogenase (PDH) kinase (PDK)–mediated inhibition of PDH contribute to decreased glucose oxidation. The heart becomes more reliant on glycolysis for ATP, which is partly mediated by enhanced GLUT1 expression. ADP: adenosine diphosphate; CD36: cluster of differentiation 36; CoA: coenzyme A; CPT: carnitine palmitoyltransferase; FACS: fatty acyl-CoA synthase; FADH2: flavin adenine dinucleotide; FAT: fatty acid translocase; LCAD: long-chain acyl-CoA dehydrogenase; MPC: mitochondrial pyruvate carrier; TCA: tricarboxylic acid.
Fatty acid oxidation
Free fatty acids in the cytosol of myocytes are activated to fatty acyl coenzyme A (CoA) moiety prior to metabolism. 23 Fatty acyl CoA requires carnitine palmitoyl transferase 1 (CPT1), the rate-limiting enzyme of mitochondrial fatty acid uptake, for conversion to fatty acyl carnitine and uptake by the mitochondria (Fig. 1).24–26 The acyl-carnitine is then converted back to fatty acyl CoA by CPT II located on the inner mitochondrial membrane. Fatty acyl CoA then undergoes β-oxidation in the mitochondrial matrix. 27 Malonyl CoA is a key negative regulator of fatty acid metabolism that inhibits CPT1 activity.28,29 It is synthesized by acetyl CoA carboxylase (ACC) and degraded by malonyl CoA decarboxylase (MCD). Phosphorylation of ACC by AMP-activated protein kinase (AMPK) inhibits malonyl CoA formation and enhances fatty acid oxidation.30–32
Glucose metabolism
Glucose transport into the adult cardiomyocytes involves the glucose transporters GLUT4 and GLUT1. 33 Glucose is then primarily converted to glucose-6-phosphate by hexokinase II, the first step in glycolysis. 34 During glycolysis, pyruvate generated from glucose can then subsequently be converted to lactate or oxidized in the mitochondria. Glycolysis yields 2 ATP per molecule of glucose. Oxidation of pyruvate involves the transport of pyruvate into the mitochondria via the mitochondrial pyruvate carrier. 35 Conversion of pyruvate to acetyl CoA is catalyzed by pyruvate dehydrogenase (PDH), the rate-limiting enzyme in glucose oxidation.36,37 PDH is phosphorylated and inhibited by PDH kinase 4 (PDK4). Complete oxidation of glucose yields 31 ATP per molecule of glucose.
Adrenergic signaling in heart
Adrenergic signaling in the heart occurs as a result of both epinephrine release from the adrenal glands and myocardial epinephrine release from cardiac sympathetic nerves.38,39 Epinephrine exerts its effects through activation of both α and β receptors in the heart. Although the importance of β receptors in the heart has long been recognized, more recently α receptors have also been shown to play a role. The stimulation of α and β receptors results in activation of phoshpholipase C/protein kinase C and adenylyl cyclase/protein kinase A pathways, respectively. Chronic excessive adrenergic stimulation of both receptors has been implicated in pathologic cardiac hypertrophy. Interestingly, in heart failure, β-1 adrenergic receptors are downregulated, which is an effect that has been attributed to catecholamine-induced enhanced receptor turnover and degradation. Furthermore, excess catecholamines lead to a decrease in functional activity of the cardiac β-1 receptor and marked desensitization of the heart to inotropic effects of epinephrine. 40
Although the effects of sympathetic stimulation on the heart have been well known, the mechanisms by which the heart generates ATP for increased work during sympathetic (epinephrine) stimulation was unknown. Reports from earlier studies are conflicting as to whether there is an increase in glucose uptake and oxidation 41 or an increase in fat extraction and oxidation. 42 More recently, epinephrine was shown to increase glucose oxidation rates by approximately 400% without significant increases in fatty acid oxidation rates in isolated working rat hearts. 43 Although adrenergic stimulation has been shown to increase glucose oxidation rates, β-blockers widely used in the treatment of heart failure have been shown to inhibit fat oxidation and result in an increase in glucose oxidation, 44 an effect that could be attributed to carnitine palmitoyltransferase I (CPT1) inhibition. 45
CARDIAC METABOLISM IN LEFT HEART FAILURE
A failing heart has been referred to as “an engine out of fuel.” 46 A number of studies have shown decreased phosphocreatine and ATP levels in failing myocardium of both animals and humans.23,47–49 Myocardial ATP content can decrease by 30%–40% in the failing heart relative to the normal heart. It has been proposed that the failing heart switches from primarily using fatty acids as energy substrates to primarily using glucose for energy production.50,51 However, the primary metabolic switch appears to be a switch from mitochondrial oxidative metabolism to an increase in glucose uptake and glycolysis.22,23,51–53 Early studies in hypertrophied hearts subjected to aortic banding showed an increase in glycolysis, with either no change or a decrease in both carbohydrate oxidation (glucose and lactate) or fatty acid oxidation.54–57 A similar increase in glucose uptake was observed in hypertrophied hearts from Dahl salt-sensitive rats. 52 This increase in glucose uptake and glycolysis can occur in the absence of any increase in glucose oxidation, resulting in an uncoupling of glycolysis from glucose oxidation. 58 Indeed, recent studies of failing swine hearts have shown that glucose oxidation rates can be significantly depressed, 59 which probably occurs secondary to a decrease in overall mitochondrial oxidative metabolism.
Myocardial energy deficits precede the development of heart failure
Although studies providing evidence of energy deficit in heart failure abound,23,46–49 whether alterations in substrate metabolism and energy deficit are a cause or consequence of heart failure has not been clearly delineated. In a model of aortic arch constriction, Doenst et al. 60 investigated cardiac function and fatty acid and glucose metabolism during the development of hypertrophy and heart failure. Diastolic and systolic dysfunction were observed at 6 weeks and 10 weeks, respectively, following aortic constriction. They observed that 2 weeks after pressure overload, when hypertrophy was evident with preserved cardiac function, there was a significant decrease in fatty acid (oleate) oxidation rates, whereas glucose oxidation rates were increased. This was associated with significantly decreased messenger RNA expression of fatty acid oxidative enzymes. Thus, decreased fatty acid oxidation involves both decreases in fatty acid uptake and mitochondrial oxidation. Thus, inhibition of oxidative metabolism and energy deficit precede the onset of heart failure.
Zhang et al. 61 also investigated the early alterations in myocardial substrate metabolism in pressure overload–induced heart failure. Mice that underwent abdominal aortic constriction (AAC) developed systolic dysfunction (heart failure) 3 weeks after the procedure. This was preceded by a 37% decrease in myocardial ATP production from mitochondrial oxidative metabolism within 2 weeks of an AAC. This was associated with decreases in both glycolysis and oxidative metabolism. Decreases in palmitate, glucose, and lactate oxidation were observed. Additional decreases in glycolysis and oxidative metabolism was observed at 3 weeks, when heart failure was evident. A 47% decrease in ATP production was observed at this time. Not only were the absolute glycolytic and glucose oxidation rates decreased, but the increase in glycolysis and glucose oxidation normally observed in sham (control) hearts were blunted in hearts from mice subjected to AAC. Thus, energy deficit was associated with insulin resistance as observed by decreased membrane GLUT4 expression in hearts from AAC mice. A number of studies have demonstrated systemic insulin resistance in patients with congestive heart failure.62–64 In this study, it was interesting to note that cardiac insulin resistance developed as early as 2 weeks after AAC, whereas systemic insulin resistance was not evident.
Selective decreases in glucose oxidation in heart failure
In agreement with previous studies of mice subjected to AAC 61 and pigs with heart failure, 59 Zhabyeyev et al. 65 observed a significant decrease in glucose oxidation 6 weeks after transverse aortic constriction (TAC)–induced heart failure. A decrease in glucose uptake and glycogen synthesis observed in TAC hearts was attributed to insulin resistance as shown by decreased phosphorylation of Akt and decreased membrane GLUT4 expression. However, these authors found no differences in fatty acid oxidation. Decreased malonyl CoA levels associated with AMPK-induced phosphorylation and inhibition of ACC possibly prevented the decrease in fatty acid oxidation observed in other studies.
Studies investigating the mechanisms of angiotensin II (Ang II)–mediated heart failure also reported selective decreases in glucose oxidation.66,67 Ang II is the main effector of the renin-angiotensin-aldosterone (RAS) system that is involved in adverse cardiac remodeling and heart failure.68,69 Ang II infusion in mice for 14 days resulted in cardiac hypertrophy, insulin resistance, and diastolic dysfunction. 66 This was accompanied by a decrease in the ability of insulin to stimulate glucose oxidation and to inhibit palmitate oxidation, compared with wild-type (WT) mice. The decrease in glucose oxidation can be attributed to PDK4-mediated phosphorylation of PDH and acetylation of PDH secondary to decreased SIRT3 (the deacetylase) expression. In response to insulin, although hearts from both groups produced similar amounts of ATP, Ang II–treated hearts produced 80% of ATP from palmitate, whereas WT hearts generated only 62%. This also resulted in diastolic dysfunction and reduced cardiac efficiency. Thus insulin resistance and decreased glucose oxidation play a role in RAS-mediated heart failure. To further confirm the role of glucose oxidation, mice lacking PDK4 knockout (KO) were investigated after treatment with Ang II. The lack of PDK4 removes the inhibition on PDH, the rate-limiting enzyme in glucose oxidation, thereby increasing glucose oxidation rates in the heart. Interestingly, Ang II–treated PDK4 KO hearts did not develop diastolic dysfunction and had glucose oxidation rates that were significantly higher than those in WT–Ang II hearts. However, no changes in palmitate oxidation were observed with Ang II treatment. Moreover, irbesartan, the AT1R blocker, prevented Ang II–induced diastolic dysfunction in WT mice. 67 In comparison to hearts treated with Ang II, irbesartan increased both glucose and palmitate oxidation rates and restored the energy deficit. Inhibition of PDK4 expression by irbesartan that led to increased PDH activity possibly contributed to the restoration of glucose oxidation. Similar to Ang II–induced heart failure, phenylephrine, the α-1 agonist, also induced cardiac hypertrophy and diastolic dysfunction that was associated with a selective reduction in glucose oxidation. 67 On the other hand, WT mice subjected to TAC showed increased glucose oxidation and glycolysis with no changes in palmitate oxidation. 51 Such observed differences could be attributed to the model of heart failure, strain, and age of mice studied and the degree and duration of pressure overload. Riehle et al. 43 investigated the metabolic and energetic alterations in mice deficient for PGC-1 β. Interestingly, basal rates of glucose and palmitate oxidation and glycolysis were increased in these hearts. In response to pressure overload 3 weeks after aortic banding, decreased cardiac efficiency was accompanied by a decrease in glycolysis and glucose oxidation, features that are consistent with insulin resistance, whereas no significant changes in palmitate oxidation were observed. These studies suggest that enhancing glucose oxidation and promoting better coupling between glycolysis and glucose oxidation could prove to be beneficial in the treatment of heart failure.
Decreased fatty acid oxidation in heart failure
In aortic banding–induced heart failure, palmitate oxidation rates determined from kinetic analysis of the 13C isotopic enrichment data for glutamate were significantly reduced compared with sham-operated rats. 70 In response to a β-adrenergic agonist challenge, palmitate oxidation rates increased in both groups, albeit to a lesser extent in failing hearts. 70 A recent study also found a similar metabolic profile, with hearts from mice subjected to TAC having lower fatty acid oxidation rates, whereas an increase in glycolysis and glucose oxidation was observed. 50 Consistent with these studies, Osorio et al. 71 observed a decrease in fatty acid oxidation rates in pacing-induced heart failure in conscious dogs. This was attributed to a decreased expression of CPT1 and medium-chain acyl-CoA dehydrogenase (MCAD). Sack 72 and Razeghi 73 previously reported decreased expression of genes involved in fatty acid oxidation. Decreased fatty acid metabolic gene expression has also been shown to be reduced in failing human hearts.72,73 Similar fatty acid metabolic gene profiles were observed in a spontaneous hypertension heart failure (SHHF/Mcc-fa cp ) rat model of hypertension, hypertrophy, and failure. 72 Contrary to these studies, palmitate oxidation rates were found to be significantly increased in WT mice subjected to TAC. 74 Proteomic and microarray analysis reveal increased expression of genes involved in mitochondrial oxidative phosphorylation in left ventricles from rabbit hearts after 4 weeks of aortic banding. 75
To further investigate the contribution of fatty acid oxidation to the development of cardiac hypertrophy and heart failure, pressure overload–induced models of heart failure were studied in genetically modified mice deficient for CPT1b 74 or acetyl CoA carboxylase 2 (ACC2−/−). 50 Although the former demonstrate decreased fatty acid oxidation, the latter have higher cardiac fatty acid oxidation rates. CPT1b is an enzyme present in the outer mitochondrial membrane that regulates the entry of long-chain fatty acids into the mitochondria for β-oxidation. As CPT1b-homozygous mice are embryonically lethal, the authors have used heterozygous (CPT1b+/−) mice that are partially deficient for CPT1b. TAC-induced pressure overload resulted in a precipitous decrease in ejection fraction and fractional shortening in the CPT1b+/− mice compared with WT mice. Palmitate oxidation was significantly decreased, whereas glucose oxidation was increased, in failing CPT1b hearts. This was also accompanied by cardiac hypertrophy that was significantly higher than that found in WT mice. CPT1b+/− mice subjected to TAC had higher accumulation of triglycerides and ceramides. Interestingly, enzymes involved in the uptake of fatty acids into the myocyte were down-regulated. The authors suggest that myocardial lipid accumulation and lipotoxicity was due to decreased palmitate oxidation rates rather than changes in fatty acid uptake. On the other hand, transgenic mice overexpressing fatty acid transport protein 1 (FATP1), 76 lipoprotein lipase, 77 long-chain acyl CoA synthetase, 78 and peroxisome proliferator activated receptor α (PPAR-α) 79 in which myocardial fatty acid uptake, esterification, or oxidation were enhanced were associated with cardiac hypertrophy, contractile dysfunction, and accumulation of lipids and lipid intermediates. Mice subjected to 10 weeks of pressure overload developed cardiac hypertrophy, had lower rate pressure product compared with sham-operated mice, and were associated with decreased CPT1 activity and decreased palmitate oxidation rates. 80
Although the previous study examined cardiac metabolism in a mouse model with low fatty acid oxidation, Kolwicz et al. 50 used a mouse model lacking ACC2 (ACC2−/−) in which higher cardiac fatty acid oxidation is found. Cardiac function was preserved in ACC2−/− mice despite higher fatty acid oxidation rates. Furthermore, preserved cardiac function and attenuated cardiac hypertrophy were observed in ACC2−/− mice subjected to TAC when compared with WT mice subjected to TAC. Of interest, lactate production rates were markedly decreased in the ACC2−/− mice, indicative of a better coupling between glycolysis and glucose oxidation.
In summary, heart failure is associated with an energy deficit state that precedes the onset of heart failure. This is associated with decreased oxidative metabolism (fatty acids and glucose) and a switch in substrate use from fatty acids to glucose for glycolysis.
CARDIAC METABOLISM IN RIGHT HEART FAILURE
Studies of right ventricular failure due to pressure overload are not as extensive as those of left ventricular failure. As in the left ventricle, the right ventricle develops hypertrophy in response to pressure overload.8,17,20 Due to the thin wall, the right ventricle undergoes rapid and exaggerated hypertrophic response. 81 Following hypertrophy, the right ventricle undergoes dilatation resulting in decreased contractile force, ultimately resulting in right ventricular failure.17,20 Similar to the left ventricle, the right ventricle also primarily depends on mitochondrial oxidative phosphorylation for ATP production from fatty acids and glucose.8,81 Right heart failure is also associated with low ATP production.82,83
Energy deficit in right ventricular hypertrophy and failure
Right ventricular hypertrophy (RVH) and failure are associated with a switch from oxidative metabolism to glycolysis. 81 In the early stages of RVH, glycolysis may compensate for lack of ATP production via oxidative metabolism. However, long-term reliance on glycolysis for ATP could lead to energy starvation and failure.46,84 In hypertrophied right ventricle of ferret hearts induced by pulmonary artery clipping, a decrease in creatine phosphate content but preserved ATP levels was observed. 83 In contrast, in monocrotaline-induced RVH, decreases in both phosphocreatine and ATP levels were observed. 82
Right ventricular dysfunction is associated with increased glycolysis
Takeyama et al. 85 observed that glucose uptake was increased in the right ventricle of conscious rats 4 weeks after pulmonary constriction (using 14C–2 deoxyglucose [2DG]). There was no difference in 14C β-methylheptadecanoic acid (BMHDA) accumulation, suggesting no differences in fatty acid uptake between sham and hypertrophied right ventricles. Interestingly, 14C-BMHDA uptake in the hypertrophied left ventricle was decreased compared with hearts from sham-operated rats. 85 The increase in 14C-2DG uptake would suggest either increased glycolysis or increased glycogen synthesis. Other studies have shown increases in glycolysis in hypertrophied hearts.54,55,86 Therefore, these authors suggest that glycolysis was increased in hypertrophied right ventricles after pulmonary constriction. Consistent with this study, subsequent studies have shown in both humans and rats with pulmonary hypertension that 18F-fluoro deoxyglucose (18FDG) uptake is increased in the right ventricle.87,88 Schwartz et al. 84 also reported that, in the right ventricle of pig hearts subjected to acute pulmonary constriction, glucose uptake tended to increase and free fatty acid uptake did not change compared with hearts from sham-operated pigs. However, acute pulmonary artery constriction in rats resulted in increased 14C-BMHDA deposition, with no changes in using 14C-2DG deposition. 85
In a monocrotaline-induced model of pulmonary hypertension, the development of RVH is a maladaptive response. The subsequent right ventricle dysfunction was associated with enhanced 2-fluoro-2-DG uptake, suggesting increased rates of glycolysis in this model. 88 Results were confirmed in isolated working hearts, where glycolysis rates were increased compared with controls, whereas no differences in glucose oxidation rates were observed. Molecular studies revealed increased GLUT1 expression consistent with increased glucose uptake. Increased GLUT1 expression could be a compensatory mechanism to enhance glucose transport for low levels of ATP production in glycolysis. However, in working hearts, where glucose oxidation rates were unchanged, phosphorylation of PDH, which is the rate-limiting enzyme for glucose oxidation, was increased. In contrast, in a model of pulmonary artery banding (PAB)–induced RVH (without pulmonary artery hypertension), right ventricle oxygen consumption was reduced in PAB hearts compared with controls, suggesting decreased rates of glucose oxidation. In this model, increased fatty acid oxidation rates were associated with increase in expression of CPT1, thus making CPT1 a target for treatment. Interestingly, PDH is inhibited much more in the monocrotaline-induced PAH model, in which RVH is maladaptive, than in the PAB-induced RVH model, which is an adaptive response to increased afterload. 89 In fawn-hooded rats with pulmonary hypertension and RVH, FOXO1-mediated upregulation of PDK4 resulted in decreased glucose oxidation and poor right ventricular function. 90 These studies would suggest that activating PDH through inhibition of PDK might be useful in conditions of pulmonary hypertension associated with pulmonary vascular endothelial damage. Taken together, these studies suggest uncoupling between glycolysis and glucose oxidation. In summary, a healthy right ventricle is able to generate ATP through the oxidation of both fatty acids and glucose as substrates and therefore is metabolically flexible. In contrast, a hypertrophied right ventricle is more reliant on glycolysis.
APPROACHES TO TREAT LEFT HEART FAILURE
Inhibiting fat oxidation
Heart failure is associated with decreased glucose oxidation and increased glycolysis. Therefore, one approach to treat heart failure is to enhance glucose oxidation and to promote a better coupling between glycolysis and glucose oxidation.23,27 This can be achieved by inhibiting fatty acid oxidation or directly enhancing glucose oxidation. Inhibiting fatty acid oxidation to promote glucose oxidation involves exploiting the Randle cycle. 91 Acetyl CoA derived from fatty acid oxidation inhibits PDH thus lowering glucose oxidation. As a result, inhibiting fatty acid oxidation would enhance glucose oxidation. The rate of fatty acid oxidation can be regulated by inhibiting CPT1, by inhibiting MCD (the enzyme that degrades malonyl CoA to promote malonyl CoA inhibition of CPT1), or by inhibiting long-chain 3-ketoacyl-CoA thiolase (KAT; Fig. 2).23,27
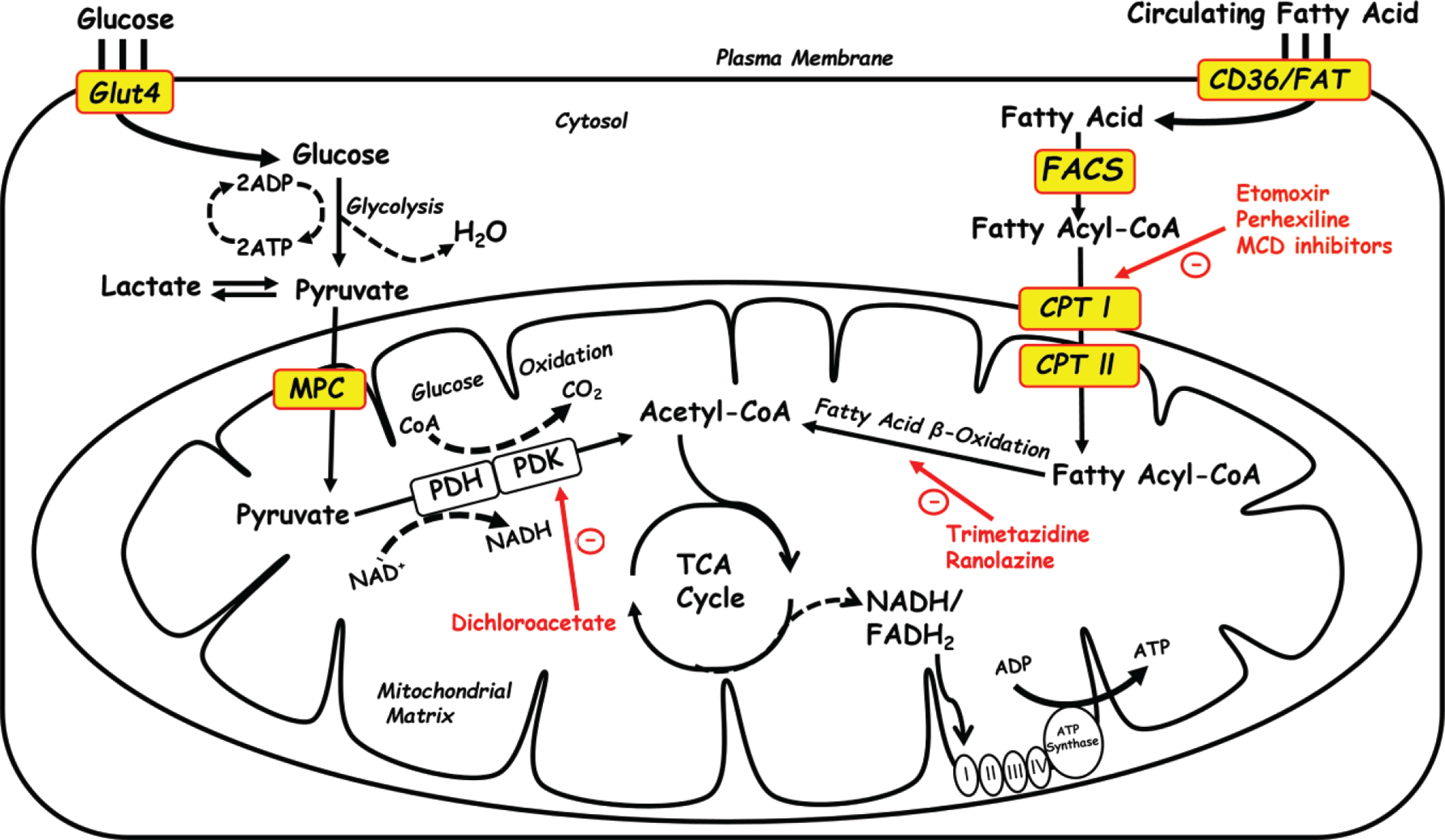
Targeting cardiac energy metabolism for the treatment of heart failure. Fatty acid oxidation can be targeted at the level of fatty acid uptake through cluster of differentiation 36 (CD36)/fatty acid translocase (FAT), mitochondrial fatty acid uptake via carnitine palmitoyltransferase (CPT) I, or fatty acid oxidation in the mitochondria. Mitochondrial fatty acid uptake can be inhibited using CPT I inhibitors such as etomoxir, perhexline, and malonyl coenzyme A (CoA) decarboxylase (MCD) inhibitors. Glucose oxidation can be enhanced by dichloroacetate, the pyruvate dehydrogenase kinase (PDK) inhibitor. ADP: adenosine diphosphate; ATP: adenosine triphosphate; FACS: fatty acyl-CoA synthase; FADH2: flavin adenine dinucleotide; LCAD: long-chain acyl-CoA dehydrogenase; MPC: mitochondrial pyruvate carrier; TCA: tricarboxylic acid.
CPT1 is the rate-limiting enzyme for mitochondrial fatty acid uptake.24,25 Etomoxir is an irreversible inhibitor of CPT1. 92 Etomoxir has been shown to improve cardiac function in rat hearts subjected to pressure overload. 93 Furthermore, in a clinical trial of patients with New York Heart Association (NYHA) class II heart failure, etomoxir (80 mg/day for 3 months) improved left ventricular ejection fraction and cardiac output at peak exercise. 94 Perhexiline, another CPT1 inhibitor, has also been shown to improve systolic function, exercise capacity, and overall cardiac energetics in patients with heart failure.95,96
Inhibition of MCD increases malonyl CoA content in hearts, which would subsequently exert its inhibitory effect on CPT1.97,98 MCD inhibitors have been shown to improve insulin sensitivity and enhance glucose oxidation via inhibition of fatty acid oxidation. 30 Although a number of studies have shown beneficial effects in the setting of ischemic heart disease,99,100 it remains to be seen whether it will improve heart failure.
β-blockers are widely used in the treatment of heart failure. Because of their negative inotropic and chronotropic effects, β-blockers reduce cardiac workload and are therefore beneficial in the treatment of heart failure. In addition to these effects, β-blockers have also been shown to have metabolic modulating effects. Metoprolol has been shown to reduce CPT1 activity in dogs with heart failure. 45 In patients with left ventricle dysfunction, metoprolol treatment reduced oxidative metabolism and resulted in an improvement in cardiac efficiency in patients with left ventricle dysfunction. Subsequently, carvedilol has also been shown to inhibit CPT1. 101 In noncachectic patients with moderately severe heart failure, carvedilol reduced fatty acid oxidation and increased glucose oxidation rates. This was associated with improvement in NYHA classsymptoms. 102
Trimetazidine is a partial fatty acid oxidation inhibitor that inhibits KAT.103,104 This results in an increase in glucose oxidation. In pressure overload–induced hypertrophied rat hearts, trimetazidine reduces glycolysis, enhances glucose oxidation, and improves postischemic recovery. 105 In patients with heart failure, trimetazidine treatment was associated with a reduction in whole-body resting energy expenditure. 106 Furthermore, in a randomized clinical trial, trimetazidine improves NYHA functional class, left ventricular ejection fraction,107,108 and whole-body insulin sensitivity. 109 A recent retrospective study has shown that trimetazidine treatment is effective in reducing mortality and improving event-free survival in patients with congestive heart failure. 106 Ranolazine, another partial fatty acid β-oxidation inhibitor, has also been shown to increase glucose oxidation and PDH activity. 110 It also improves the coupling between glycolysis and glucose oxidation. 110 Ranolazine treatment of intracoronary embolization–induced heart failure in dogs was associated with improvement in left ventricular systolic function without alterations in cardiovascular hemodynamics, suggesting that ranolazine primarily targets cardiac metabolism. 111 Currently, a clinical trial investigating the effect of ranolazine on heart failure with preserved ejection fraction is ongoing. 112
Enhancing glucose oxidation
Inhibiting PDK (the enzyme that phosphorylates and inhibits PDH) using dichloroacetate (DCA) appears to be beneficial in pressure overload heart failure.23,27 DCA selectively stimulates glucose oxidation and promotes coupling between glycolysis and glucose oxidation.113,114 This would result in decreased proton production, which otherwise could worsen cardiac efficiency. Treatment of Dahl salt-sensitive rats with DCA prevented the progression of hypertrophy to heart failure and improved systolic cardiac function and survival. 52 In this study, DCA treatment was associated with increased 18FDG uptake and PDH activity. Therefore, the authors speculate that DCA primarily increased glucose oxidation and ameliorated heart failure. A limitation of this study is that 18FDG is a marker of glycolysis and cannot reliably measure glucose oxidation rates.
The effect of dichloroacetate on cardiac function in patients with congestive heart failure is conflicting. In a small clinical study involving 10 patients with moderate to severe heart failure, dichloroacetate administration improved left ventricular mechanical efficiency, increased stroke volume and left ventricular minute work with a simultaneous reduction in myocardial oxygen consumption. 115 However, a subsequent study failed to show benefits in patients with congestive heart failure. 116
Enhancing fatty acid oxidation
Because pressure overload heart failure is consistently associated with decreased fatty acid oxidation, another approach to treat heart failure is to enhance fatty acid oxidation. A number of experimental studies have shown favorable effects of a high-fat diet on cardiac function and survival in different disease states, such as myocardial infarction, heart failure, and hypertension. 11 In an attempt to enhance fatty acid oxidation, rats subjected to pressure overload were fed a high-fat diet or diet supplemented with omega-3 polysaturated fatty acid. This resulted in attenuation of left ventricular remodeling and dysfunction.85,117,118 In a subsequent study, a linoleate-enriched high-fat diet (but not saturated high-fat diet) attenuated cardiac hypertrophy, left ventricular chamber dilation, and improved systolic function in aged hypertensive heart failure rats. 119 Moreover, a high-fat diet reduced cardiac hypertrophy and improved contractile function in Dahl salt-sensitive rats.120,121
In these studies, pressure overload was induced in lean (nonobese) animals and then a high-fat diet was fed to the animals in an attempt to increase fatty acid oxidation. In humans, heart failure is associated with other risk factors such as obesity, 122 diabetes, 123 and hypertension, 124 each of which can also independently increase the risk of heart failure. Obesity and diabetes are associated with insulin resistance and increased cardiac fatty acid oxidation. 125 Therefore, further studies are needed to ascertain the effect of accelerating fat oxidation in heart failure models associated with obesity and diabetes.
APPROACHES TO TREAT RIGHT HEART FAILURE
Inhibiting fat oxidation
In a PAB model of right ventricle failure in rats in which increased fatty acid oxidation is maladaptive, both trimetazidine and ranolazine inhibit fatty acid oxidation and glycolysis and enhance glucose oxidation. This results in a better coupling between glycolysis and glucose oxidation and is associated with better cardiac index and exercise capacity. Treatment with these fatty acid oxidation inhibitors also led to some regression in RVH. 126 The PAB model is similar to that of pulmonary stenosis in which there is right ventricle outflow obstruction. Thus, fatty acid oxidation inhibitors, by modulating metabolism, may prove to be useful despite persistence of pulmonary stenosis. Additional clinical studies are needed to investigate the effect of fatty acid oxidation inhibitors in right heart failure. We expect that, in a manner similar to the beneficial effects observed in the treatment of congestive heart failure, inhibition of fat oxidation would also improve right heart failure.
Enhancing glucose oxidation
The effect of DCA has been more extensively investigated in experimental models of right heart failure. In a monocrotaline-induced model of RVH and failure, DCA, a PDK inhibitor, reduced cardiac hypertrophy and improved cardiac output as measured in vivo. 88 In a working heart model, DCA acutely improved cardiac function and increased glucose oxidation rates. DCA induced a threefold increase in glucose oxidation rates, whereas glycolysis increased by a mere 25%. The marked increase in glucose oxidation rates, disproportionate to minor increases in glycolytic rates, implies a better coupling between glycolysis and glucose oxidation. DCA also increased right ventricle cardiac output in a PAB model of right ventricle failure. This was associated with decreased GLUT1 expression and increased oxygen consumption rates, which suggests improved glucose oxidation. Furthermore, in the fawn-hooded rat model of PAH and RVH, DCA inhibited FOXO1-mediated PDK4 upregulation, which resulted in improved cardiac output and right ventricle function that was associated with stimulation of glucose oxidation. 90
RVH is also associated with higher mitochondrial membrane potential (hyperpolarization) in addition to alterations in cardiac energy metabolism. 127 Increases in intracellular and intramitochondrial calcium could lead to mitochondrial hyperpolarization and activation of the transcription factor NFAT, which is involved in cardiac hypertrophy.128,129 Furthermore, this study reported that DCA reverses mitochondrial hyperpolarization in monocrotaline-induced RVH. 127 In addition, in Langendorff perfusions, DCA increased right ventricular inotropy only in the hypertrophied right ventricles and not in normal right ventricles, which is an effect that could be attributed to normalization of mitochondrial membrane potential. Furthermore, improved coupling of glycolysis to glucose oxidation by DCA in the hypertrophied right ventricle, which is more dependent on glycolysis than a healthy ventricle, could explain why increased inotropy was observed only in the hypertrophied right ventricle and not in the healthy ventricle.
CONCLUSIONS
Heart failure is associated with alterations in cardiac energy metabolism that lead to an energy deficit. In heart failure, there is a switch from oxidative metabolism to greater reliance on glycolysis. Specifically, decreases in fatty acid and glucose oxidation result in energy deficit that is inadequately compensated by glycolysis. Increased glycolysis and decreased glucose oxidation results in lactate and proton build up in the myocardium that compromises efficiency. Targeting metabolism as a therapeutic strategy may be one approach to treat heart failure. Pharmacological inhibition of fatty acid oxidation or stimulating glucose oxidation may restore energy imbalance and improve cardiac function.
