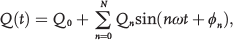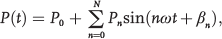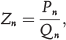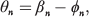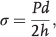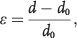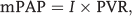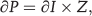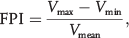Abstract
Recent studies have indicated that systemic arterial stiffening is a precursor to hypertension and that hypertension, in turn, can perpetuate arterial stiffening. Pulmonary artery (PA) stiffening is also well documented to occur in pulmonary hypertension (PH), and there is evidence that pulmonary vascular stiffness (PVS) may be a better predictor of outcome than pulmonary vascular resistance (PVR). We have hypothesized that the decreased flow-damping function of elastic PAs in PH likely initiates and/or perpetuates dysfunction of pulmonary microvasculature. Recent studies have shown that large-vessel stiffening increases flow pulsatility in the distal pulmonary vasculature, leading to endothelial dysfunction within a proinflammatory, vasoconstricting, and profibrogenic environment. The intricate role of stiffening-stimulated high pulsatile flow in endothelial cell dysfunction includes stepwise molecular events underlying PA hypertrophy, inflammation, endothelial-mesenchymal transition, and fibrosis. In addition to contributing to microenvironmental alterations of the distal vasculature, disordered proximal-distal PA coupling likely also plays a role in increasing ventricular afterload, ultimately causing right ventricle (RV) dysfunction and death. Current therapeutic treatments do not provide a realistic approach to destiffening arteries and, thus, to potentially abrogating the effects of high pulsatile flow on the distal pulmonary vasculature or the increased work imposed by stiffening on the RV. Scrutinizing the effect of PA stiffening on high pulsatile flow–induced cellular and molecular changes, and vice versa, might lead to important new therapeutic options that abrogate PA remodeling and PH development. With a clear understanding that PA stiffening may contribute to the progression of PH to an irreversible state by contributing to chronic microvascular damage in lungs, future studies should be aimed first at defining the underlying mechanisms leading to PA stiffening and then at improved treatment approaches based on these findings.
Keywords
Arterial stiffening is increasingly recognized as a risk factor of cardiovascular events as well as a guide for pharmacological treatment of cardiovascular diseases. Yet its exact role in the development and progression of cardiovascular diseases such as hypertension remains elusive. A recent study, however, presented convincing data supporting the possibility of a cause-effect relationship between arterial stiffness and systemic hypertension: higher levels of arterial stiffness and central pressures preceded and were associated with an increased risk of hypertension, but hypertension did not cause arterial stiffness. 1 This work demonstrated that increased vascular stiffness could be a precursor to hypertension. A key implication from these observations is that arterial stiffness, when used as a measure of cardiovascular risk, may identify novel therapeutic approaches to prevent the onset or progression of hypertension. 2 These findings are profound because commonly used antihypertensive medications are based largely on their vasodilating effects on smaller resistance vessels and have little effect on arterial stiffness. 3 Traditional vasodilatory drugs lower mean central pressures but do not have significant effects on pressure dy-
namics or so-called pulsation. In parallel to new findings about the role of arterial stiffness in the systemic circulation, pulmonary arterial stiffness is also increasingly recognized for its prognostic value as it relates to pulmonary hypertension (PH).4–8 Human PH patients and animal models for PH, such as hypoxic calves, rats, and mice, are all characterized by increased stiffness or reduced compliance of proximal pulmonary arteries (PAs) and/or increased PA impedance.7,9–11 Current therapies for PH, which are mainly directed at dilation of small PAs to reduce pulmonary vascular resistance (PVR), have shown only modest effects on reducing pulmonary vascular pressure and resistance and, as shown by emerging evidence, have little effect on the long-term mortality of severe-PH patients.12–14 This raises the possibility that, like systemic hypertension, pulmonary vascular stiffness (PVS) is an important factor that must be addressed/treated if PH outcome is to be improved.4,5,8 There is thus increased need to understand the mechanistic role of increased PVS in PH progression, which likely includes effects on (1) right ventricular load and function through pulse wave reflection and (2) the distal vasculature, through changes in flow pulsatility (magnitude and velocity), which induce injury/inflammatory responses. This is illustrated in Figure 1.
General hypothesis of perpetuation of pulmonary hypertension (PH) by vascular stiffening. Vascular stiffening increases the reflected wave component, thereby increasing flow pulsatility. High pulsatility causes injury and inflammation to distal vasculature. Increased reflected wave (which increases flow impedance) also causes adverse compensatory effects on right ventricular function by causing right ventricle (RV) overload and, at least initially, increasing the output of the RV, which increases flow pulsatility. HPF: high-pulsatility flow; mPAP: mean pulmonary arterial pressure; PA: pulmonary arteries.
MEASUREMENT OF PVS IN PH: HISTORICAL PERSPECTIVE
Studies of the pulmonary circulation in the 1960s began to measure proximal PVS (or its inverse, pulmonary vascular compliance) in animal models and in humans with PH.15–21 These studies clearly demonstrated that the PA significantly stiffens in disease and that these increases in stiffness were associated with increased right ventricular afterload.20,21 Clinically, PVS was measured as a component of impedance, using a pressure transducer and electromagnetic velocity sensor or using intravascular ultrasound during catheterization. 7 However, the labor-intensive and invasive nature of the measurement approaches used seemed to preclude them from routine clinical use, and with time, the concept of PVS as a critical component of the PH disease process lost clinical relevance. In recent years, noninvasive imaging modalities have been used to measure deformations and/or flows that were previously available only from invasive study, providing information vital to the calculation of stiffness and reinvigorating the clinical application of PVS to PH. Because of the increased appreciation of the contribution of PVS to PH, these methods are gaining popularity among researchers and physicians.22–24
PVS can be measured globally or in a site-specific fashion. 7 Historically, global in vivo stiffness of the pulmonary vascular bed was estimated with the total volumetric compliance (ΔV/ΔP), where V is the total pulmonary vascular volume and P is the pressure, in both animals and humans.15–19,21 Later, input impedance modulus, a characterization of distal load at a specific location, was used as an indicator of PVS and quantified both the static and the dynamic components of right ventricle (RV) afterload. Many groups recognized the importance of this total-afterload measurement that included the impacts of PVR and PVS.18,20,25,26 Womersley, 27 McDonald, 28 and O'Rourke and Taylor 29 demonstrated that the pressure and flow curves of pulmonary arterial blood flow could be expressed as a Fourier series of n harmonics. Then, the impedance (Zn) could be measured as the ratio of the pressure amplitude (Pn) to the flow amplitude (Qn) at the nth harmonic of the pressure and flow waves, respectively. The phase of the impedance is the difference in the phases of the nth harmonic of the pressure (β) and flow (φ) waves:
where Q(t) and P(t) are the flow and pressure at time t, Q0 and P0 are mean flow and pressure, Qn and Pn are flow and pressure amplitudes at the nth harmonic, respectively; ω is the fundamental frequency of oscillation, i.e., the heart rate; Zn and θn are the impedance and its phase at the nth harmonic, respectively; and φn and βn are the phase angles of flow and pressure at the nth harmonic, respectively. The contribution of pulsatile components of hemodynamics, directed by vascular stiffening, to the total afterload arose out of the work of Milnor et al. 20 in a sedated-canine model and, later, in a human model. 21 Another parameter arising from impedance measurement is the characteristic impedance (Zc), the input impedance without the wave reflection (Qm/Pm), which has been increasingly used as a global PVS measure and has been shown to be influenced by the properties of the arteries closest to the site of measurement, in particular their diameter. 30 The biggest challenge in measuring impedance remains the requirement of complete pressure and flow waveforms. 7
Local or site-specific stiffness measurement, which is likely more relevant to proximal vascular remodeling, was first obtained by Patel et al. 18 and Peterson et al., 31 using an invasive acquisition method in the main PA of dogs. They examined the distension of the PA as an engineering approximation by using the circumferential stress-strain relationships. This evaluation yielded the pressure-strain elastic modulus (Peterson modulus) as well as the circumferential elastic modulus (the slope of the circumferential stress-strain curve):
where σ is the circumferential or tangential stress, d is the artery diameter, h is the artery thickness, P is the transmural pressure, ε is the circumferential strain, and d0 is the artery diameter before distention. Bergel32,33 further supplemented this work by validating that the Peterson modulus of the dog PA increased with pressure. The Bergel group also measured the strain stiffening and investigated the viscoelastic properties of the dog PA. Greenfield and Griggs, 34 in patients undergoing open-heart surgery, demonstrated that the normal human PA was 5 times as distensible as the human aorta and that the PAs had significantly higher capacitance than systemic arteries. They also demonstrated that in patients with PH, the Peterson modulus of the main PA was significantly increased over that of the normal PA. 34
More recently, arterioventricular coupling and invasive techniques for its measurement, principally derived in the systemic circulation and left ventricle,35–41 have been applied to the right heart and the pulmonary circulation and have reemphasized the importance of vascular stiffening in PH diseases.42–46 When arterial load increases with PH severity, RV contractility cannot progress in parallel, and this leads to severe uncoupling. 45 There is a clear case for a relationship between PVS, arterioventricular coupling, and output flows from the heart, which is further discussed in the next section. Also, examining the RV function (afterload, contractility, etc.) and vascular function linkage further may reveal mechanisms that differentiate physiological and pathological ventricular remodeling. 47 The PA distensibility, a direct function of PA stiffness, decreases with progression of PH, during which the collagen content increases and the elastin content decreases in the PA as a result of remodeling.48–51 There is also little doubt about the effect of vascular mechanical properties on the hemodynamics of the pulmonary circulation, yet the underlying cellular mechanisms have to be comprehensively established. Some of these cellular mechanisms are discussed in “Effects of large-PA stiffening on flow pulsatility in the pulmonary circulation and the small-PA structure and function” below. In general terms, we may think of PVS as affecting the pulse pressure in a circulation; thus, both PVR and stiffening play a role in elevating RV pressure during systole. However, the interplay between PVS and RV function is not clearly understood and requires more detailed study.
EFFECTS OF PROXIMAL PA STIFFENING ON RV FUNCTION
The majority of studies regarding PVS in PH have focused on its effects on right ventricular function.5–8,11,52 Studies using computational approaches and small- and large-animal models, as well as those using human patients, have provided convincing evidence that RV adaptation to chronic pressure overload is related not only to the levels of vascular resistance (steady afterload) but also to PA stiffness (pulsatile load). It has been shown that increased PA stiffness is independently associated with adverse RV remodeling and performance beyond the degree of PH determined by the levels of PVR index, providing a potential mechanistic link between PA stiffness and clinical outcome. 8 PA stiffness is independently associated with the degree of RV dysfunction, hypertrophy, and dilation in PH.5,8,53,54 The contribution of PA stiffness to impaired RV performance and remodeling is thought to be through an increase in afterload.6,8,55 Ventricular afterload can be expressed in terms of a steady component (the opposition that the ventricle encounters to maintaining forward flow) and an oscillatory component (the opposition faced by the ventricle to the pulsatile components of flow). Whereas the first component is generally quantified as vascular resistance, pulsatile afterload is often disregarded in clinical practice because it requires complex invasive quantification of input impedance.56,57 In the systemic circulation, approximately 10% of the hydraulic power generated by the left ventricle is used to maintain pulsatile flow and pressure. 56 However, in the pulmonary circulation, the RV spends approximately 30% of its power in generating pulsations.21,57–62 Pulsatile (or oscillatory) power is generally considered energy dissipated through the arterial bed.
In addition to the use of the hydraulic power to illustrate the effects of PVS on the energy expenditure required for the RV in the pulmonary circulation, another method is to use the impedance complex, as reviewed in detail by Wang and Chesler.6,47 Briefly, the impedance complex is derived from pulsatile pressure-flow relationships. The current paradigm of PH diagnosis and therapy is based on the assumption that the pulmonary circulation is a static system, where the driving force (or the mean PA pressure [mPAP]) linearly relates to the product of mean PA flow (I) and vascular resistance (PVR),
where PVR is in units of dyne s cm?5. However, the PA system is highly dynamic, with pulsatile frequency components. In this dynamic vascular system, the relationship between the driving potential (the pressure gradient, or ∂P) and blood flow (∂I) is governed by a differential equation. The complex version of the pulsatile-flow relationship can be expressed by
where ∂P and ∂I are the complex scalars in the pressure and flow, respectively, and Z is the complex impedance. Thus, impedance captures frequency-dependent “resistance.” Two approaches are commonly used to obtain the impedance, namely, a frequency-domain method and a time-domain method, 6 both yielding 2 important impedance metrics: (1) the input impedance (Z0), which is calculated either as the impedance magnitude at 0 Hz (in the frequency domain) or as total PVR (in the time domain), and (2) the characteristic impedance (Zc), which is calculated either as the impedance magnitude at high harmonic frequencies (in the frequency domain) or as the slope of the pressure-flow relationship in early systole (in the time domain). Therefore, impedance, by including the steady flow resistance (PVR) and the dynamic impedance component (Zc), provides a more complete description of the vascular loading demands for the ventricular output. As in the case of PVR, the assumptions for determining static PVS are different from the assumptions for determining dynamic PVS.
These recent studies using in vivo measures and numerical analyses of the pulsatile pressure-flow relationships have provided great insights into the physics of the pulmonary circulation. They have also introduced good insights into the mechanical demands for the RV as well as quantitative determination of the RV-PA coupling efficiency. Yet the fundamental hemodynamic mechanism underlying the effects of artery stiffness on the RV through changes in upstream pulsatile flow or pressure waves remains less well explored. Defining such a mechanism(s) is critical for unraveling the hemodynamic consequences of artery stiffening.
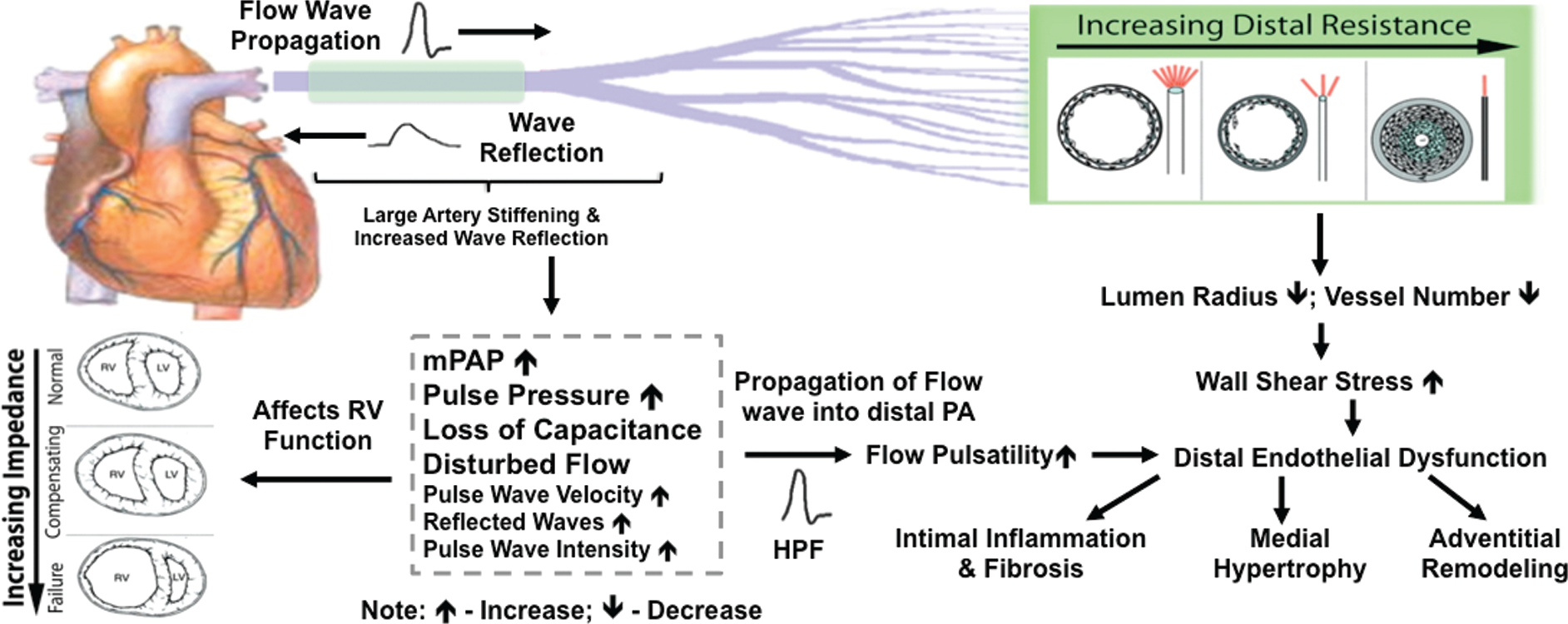
The normal pulmonary circulation is a low-pressure, low-resistance, and high-compliance circuit with little wave reflection.30,63,64 Therefore, pulmonary arterial pressure waves normally have rounded contours, in contrast to aortic pressure waves, where wave reflection determines a phase lag and early-systolic peaking of flow, with late-systolic peaking of pressure. 63 Patients with PH present with a right ventricular pressure wave with a sharp initial upstroke followed by a short plateau and a late-systolic peaking; a pulmonary wave with a high pulse pressure; and a pulmonary flow wave with a shortened time to peak velocity and a late- or midsystolic deceleration. 65 Each of these changes is largely determined by wave reflections. To understand the effects of wave reflection on PA pressure and flow waves, Furuno et al. 66 induced, respectively, proximal PA constriction (with snares to constrict both right and left PAs and thus reduce their compliance) and distal obstruction (with injection of small glass beads to produce the same increase in mean PA pressure) in dogs. The study illustrated the respective roles of proximal PA mechanics and distal PA resistance in altering wave reflection and the PA pressure and flow waves. As illustrated in Figure 2, the proximal constriction causes a midsystolic deceleration of flow even when mPAP is only moderately increased. This can be further analyzed in the frequency domain to decompose waves into their forward and backward components. In this case, midsystolic notching is clearly caused by the subtraction of an early-returned reflected wave on the forward wave. 66 Wave reflection explains the previously reported shorter time to notching on pulmonary arterial flow waves in embolic PH, relative to that in pulmonary arterial hypertension, in spite of lower mean PA pressures. 67 This result would not be affected by the adjustment of time to notching to heart rate, which is inherent to the notch ratio. 68 Constriction of the proximal PAs is also associated with a PA pulse pressure higher than that in the case of distal obstruction.66,69
Pulmonary artery pressure (Ppa) and flow (Q) recordings in a dog before and after induction of mild pulmonary hypertension by either proximal pulmonary arterial banding or the injection of small, 100-μm beads. Proximal resistance is associated with increased pulse pressure and midsystolic deceleration of flow. Decomposition of flow wave (R) shows that this is caused by an earlier return of the reflected wave (r) on the forward wave (a). 66
Consistent with these studies performed in dogs, human PH patients with different etiologies, as in the case of chronic pulmonary thromboembolism (CPTE) and idiopathic pulmonary arterial hypertension (iPAH), showing predominately proximal PA obstruction and distal PA obstruction, respectively, also provide insight into effects of changes in flow dynamics on RV function. In iPAH, a pulmonary obstructive vasculopathy involves distal and medium-to-small muscular (resistive) arteries. By contrast, in CPTE, the thrombi cause narrowing and stiffening of major (main, lobar, or segmental) elastic PAs.70,71 In normal elastic PA, the low-amplitude reflection peaks at or just after the dicrotic notch and seems to be one of the mechanisms optimizing the right ventricular–PA coupling.21,64,72 In experimental and clinical settings where PA compliance is decreased and pulse wave velocity (PWV) is increased, an earlier, increased reflected wave returns to the RV during systole rather than diastole, and this could contribute to the increase in PA pulse pressure,66,72–75 the prolonged time to peak pressure, 59 and the midsystolic deceleration of pulmonary blood flow in PH. 76 In CPTE, one approach for the identification of distal vasculopathy is the analysis of pressure decay curves after pulmonary arterial occlusion. 65 Such curves are made of a fast first component, which corresponds to the stoppage of flow through arterial resistance, and a slower component, which corresponds to the emptying of compliant capillaries through venous resistance. There is therefore an inflection point, from which one calculates an upstream resistance, essentially determined by the resistive properties of the large PAs, and a downstream resistance, determined by the cumulated resistances of small arterioles, venules, and capillaries. 77
The degree of right ventricular dysfunction, dilation, and hypertrophy in CPTE relative to that in iPAH is associated with PA stiffness. Through promoting an increase in pressure wave amplitude and early flow wave reflections, 78 arterial stiffening increases peak systolic and end-systolic pressure in upstream arteries 79 and myocardial oxygen consumption.80,81 Furthermore, increased systolic blood pressure induces myocardial hypertrophy and impairs diastolic myocardial function and ventricular ejection. These artery-stiffening effects on ventricular dysfunction were illustrated in a previous study in the systemic circulation in canines, which used a stiff conduit to substitute for the thoracic aorta and, thus, to reduce total compliance and increase central arterial pulse pressure by 2–3-fold. It was found that cardiac oxygen consumption increased 15% because of this increased load induced by stiffness. 69
In summary, both PA stiffening (i.e., changes in PA mechanics, including increase in stiffness and decrease in distensibility) and PA narrowing (i.e., changes in PA lumen diameter, including intimal inflammation and fibrosis and an increase in medial or adventitial thickness) are important contributors to right ventricular afterload via increasing oscillatory and steady ventricular work due to changes in pulse pressure and mean pressure, respectively. However, the current diagnostic and therapeutic approaches to PH have almost always highlighted only PA resistance due to narrowing or loss of distal pulmonary vasculature. PA pulse pressure correlated with pulmonary circulation stiffening, together with PA resistance, better predicts mortality.82,83 Further studies on examining hemodynamic roles of PA stiffness in pulmonary circulation and the independent predictive roles of arterial stiffness on PH should be performed.
EFFECTS OF LARGE-PA STIFFENING ON FLOW PULSATILITY IN THE PULMONARY CIRCULATION AND THE SMALL-PA STRUCTURE AND FUNCTION
Although it is becoming increasingly clear that PA stiffness or arterial flow pulse wave change likely will be incorporated into medical practice for diagnosis or prognosis of PH, many remain skeptical that vascular stiffness is a desirable treatment target. A major contributor to this skepticism is the lack of studies delineating a causal relationship between artery stiffness and PH progression. Little is known regarding the impact of PVS on initiating/perpetuating remodeling of the entire pulmonary circulation, particularly distal PA remodeling, a key feature in PH disease progression. To address this deficiency, we have performed complementary molecular, cellular, animal, and computational investigations into the role that increased proximal PVS and consequent increased flow pulsatility and pulse pressure play in PA remodeling.52,84–90 An understanding of the relationship between artery stiffness and distal vascular remodeling may be essential for the design of improved therapeutic approaches to alleviate the continuous perpetuation of small-vessel remodeling in chronic pulmonary hypertensive conditions.
As noted above, arterial pressure and flow, described by frequency-domain harmonics, are treated as the sum of sinusoidal wave trains oscillating about mean values. This separates the ventricular work into oscillatory work and work related to mean pressure and flow, making it difficult to directly relate ventricular work to the energy dissipated by the individual vessel components in the vascular network. Through the Windkessel effect and because of their compliance, elastic PAs function as a flow reservoir or hydraulic integrator that is charged by expanding passively during systole and discharged by recoiling during diastole. The compliance of a pulmonary circulatory model (Cp) is defined as the combined storage capacity of all PAs and arterioles and is related to arterial wall elasticity and vessel size (i.e., wall thickness and radius). This has 2 important effects, in that normal arterial compliance (1) converts pulsatile flow to more constant flow in distal vessels throughout the entire cardiac cycle and (2) dampens the pressure so that pressure variations in these arteries are smaller than those in the ventricle. The Cp takes into account the pulsatile components of the arterial load and therefore is an important factor contributing to systolic and diastolic pressure. It is also suggested that pulmonary arterial compliance is distributed over the entire pulmonary arterial bed, like PVR, 60 which is different from the systemic arterial tree, where the compliance is mainly located in the aorta (contributing to 80% of total compliance) and the resistance is mainly located in arterioles. Such compliance distribution suggests that pulmonary arterial compliance reduces both flow pulsatility and pressure variations throughout the relatively short (compared to the systemic circulation) pulmonary circulation.
Pressure and flow wave analysis can also be performed in the frequency domain, with results expressed as impedance spectra or pressure-flow ratios as a function of frequency. Our recent work has shown that abnormally increased pulsatile flow secondary to proximal PA stiffness induces inflammatory gene expression, cell proliferation, and leukocyte adhesion in the endothelium of distal vessels. 86 Compared to the systemic circulation, the pulmonary circulation is characterized by high flow and low pressure, because the distance traveled by the same amount of blood is much shorter compared to that in the systemic circulation. Previously, using a biaxial tensile test, the circumferential elastic moduli of bovine large PAs and thoracic arteries have been determined to vary between 50 and 100 kPa 49 and between 1,010 and 1,620 kPa, 91 respectively. Hence, large PAs are more elastic than large systemic arteries, and their flow-damping functions could be even more important.7,11 Because of these differences, the wave reflection is reduced and the cushion/damping function of large PAs is more complicated. Ejection of blood from the RV initiates nonlinear transients in pressure and flow at the root of the main PA. These transients initiate complex pulse patterns that are propagated throughout the relatively shorter pulmonary circulation.
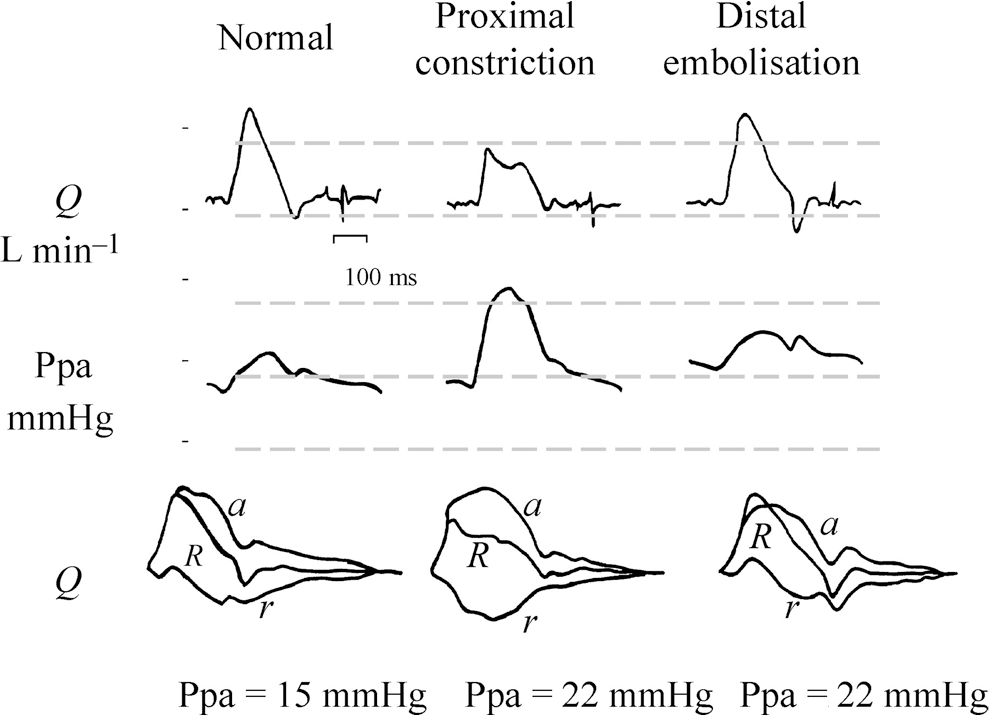
With that being said, vessels with high compliance (i.e., low stiffness) experience only small systolic pressure increases, with a relatively large increase in volume and a reduction of the wall shear stress,92–94 and also contribute to low flow and pressure pulsatility in downstream vessels.52,88,95 Conversely, stiffer vessels absorb a smaller fraction of the volume from each cardiac stroke, resulting in a substantial increase in pressure, which leads to relatively high pulse pressures96,97 and high wall shear stress as well as high flow and pressure pulsatility in downstream vessels. 52 Our data support the idea that these flow and pressure changes are sensed by the endothelial cells (ECs) lining the more downstream vessels and then transduced into biochemical signals that influence vascular remodeling. Particularly important in this mechanotransduction process is the flow effect on ECs in medium-to-small arteries. Although much is known about the effects of flow forces on the endothelium, current knowledge is based mainly on the effects of low flow or turbulent flow with low mean wall shear stress (WSS; ≤2 dyne/cm 2 ), simulating atherosclerosis-related flow conditions. Few studies have explored the impact of other pathological flow patterns. Considering that a major hemodynamic consequence of arterial stiffening is widening of the arterial pulse and increased cyclic changes of downstream arterial flow, the effect of artery stiffening–induced high-pulsatility flow (HPF) on distal artery remodeling remains largely unexplored. To that end, we have established in vitro circulatory flow systems as models that reproduce the different cushioning functions of normal elastic arteries or stiff diseased arteries and have studied how proximal stiffening-induced hemodynamic forces alter pulmonary arterial endothelial cells (PAECs) in the downstream pulmonary circulation.52,85–87,89 Using a system simulating the effect of proximal artery stiffening on increasing distal flow pulsatility for cells in culture, we have identified the flow pulsatility index (FPI) of unidirectional flow as a novel parameter that determines PA endothelial health. FPI is defined as follows:
where Vmax, Vmin, and Vmean are the maximum, minimum, and average velocity, respectively. We have shown that, with the same mean flow stresses (the static flow component), FPI, reflecting the dynamic component of flow mechanical stresses, determines distal PA cell responses.86–88 We showed that, compared to low-pulsatility flow (LPF; FPI = 0.2–0.5), HPF (FPI > 1) induced proinflammatory responses in the vascular endothelium. As illustrated in Figure 3, by imposing flows with varied FPIs on a monolayer of microvascular bovine PAECs, HPF with a physiological mean flow WSS (10–14 dyne/cm 2 ) consistently enhanced distal PAEC expression of proinflammatory molecules at the gene and protein levels, leading to in-creased monocyte adhesion. Recently, we also showed that HPF induces further EC dysfunction by inducing an endothelial-to-mesenchymal transition (EndoMT), as evidenced by upregulated α–smooth muscle actin (α-SMA), type I collagen (COL1α1), and transforming growth factor (TGF-)β1 expression and downregulated PECAM-1 (platelet endothelial cell adhesion molecule) in PAECs. HPF likely disrupted cadherin junctions and initiated an EndoMT-like response, causing cells to assume a spindle-shaped, mesenchymal-like appearance. This is consistent with recent studies of epithelial-mesenchymal transition (EMT), which show a chronic inflammatory microenvironment as a decisive factor in the induction of the pathological EMT.98,99 EMT is a crucial process regarded as a physiological attempt to control inflammatory responses and to “heal” damaged tissues, but in pathological contexts it is a process that can lead to tissue fibrosis.98,99
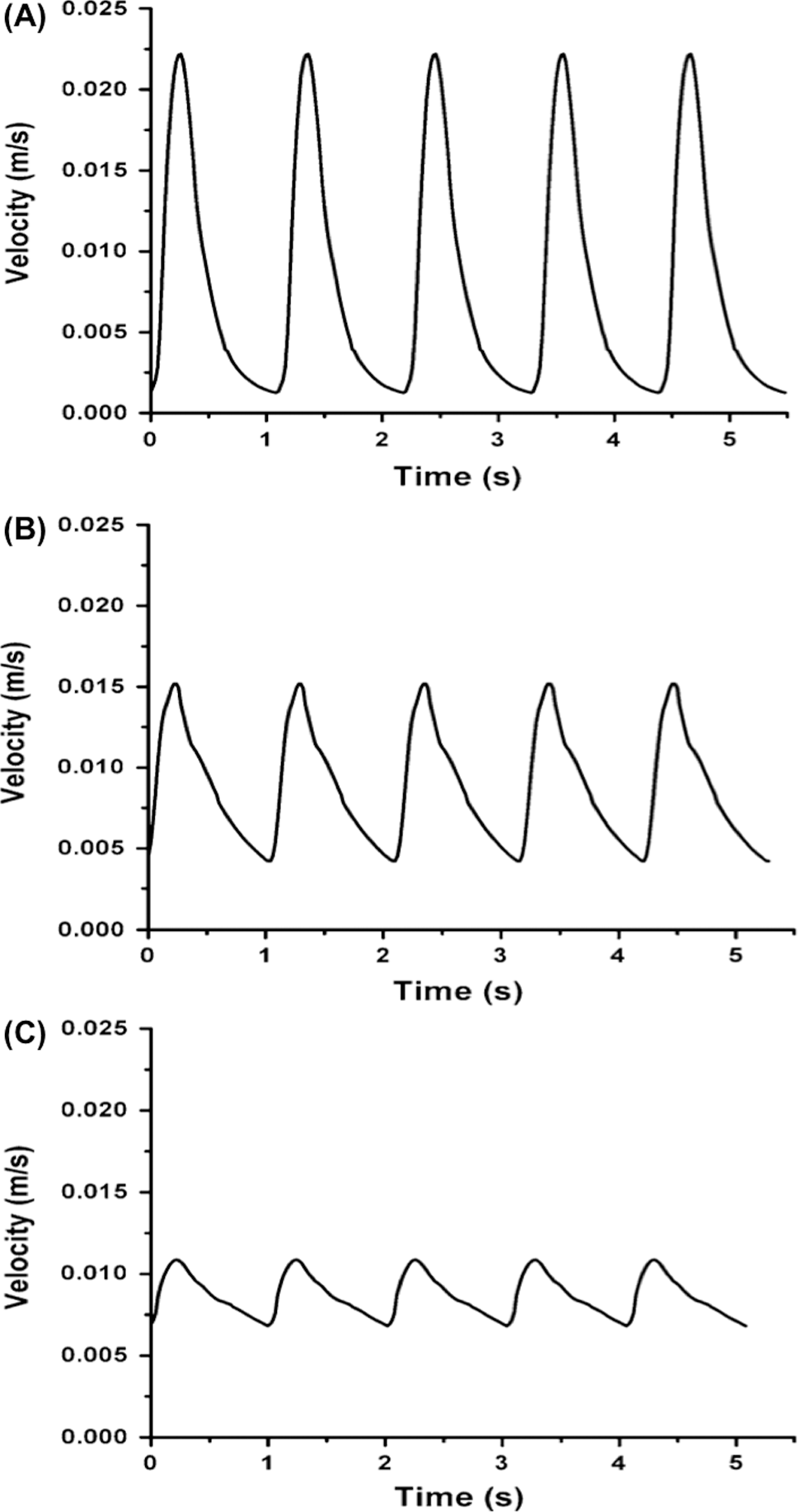
Flow pulsatility index of unidirectional flows (inlet velocity time history) profiles: high (A), medium (B), and low (C) pulsatility. 87
We recently extended cellular studies with HPF to exploration of the molecular mechanisms mediating endothelial mechanosensing and mechanotransduction of HPF into proinflammatory signals. As it has been well established that flow induces EC cytoskeletal reorganization, which then activates signaling cascades to alter EC function, we studied HPF influences on endothelial morphology and cytoskeletal mechanotransduction. Our results revealed that both HPF and high mean WSS (with low pulsatility) align and elongate endothelial structure but do so quite differently: HPF induces a higher polarity index in ECs. The polarity index of a cell is the maximum cell length–to–maximum cell width ratio, and this index for the HPF condition is almost 1.8 times that for the LPF condition. 89 We also found, using agents that inhibit, enhance, or stabilize polymerization of cytoskeletal microtubule components such actin or tubulin, that the microtubule network is critically involved in PAEC sensing and conversion of HPF to proinflammatory signals through nuclear factor κB (NF-κB) activation. Specifically, using taxol in the in vitro flow system, we successfully reduced HPF-induced PAEC polarization, NF-κB activation, and inflammation (Figure 4). 90 Our studies are consistent with others demonstrating that atherosclerotic flow conditions lead to inflammatory events through effects on the cytoskeleton.100–102 Because acetylated α-tubulin (primary cilia) was recently identified as a novel flow sensor and is involved in EMT, we hypothesize that it could provide a specific mechanosensing mechanism for PAECs in response to HPF. Regarding the molecular signals downstream to the cytoskeleton, we have identified transcription factors (NF-κB and Krüppel-like factor 2 [KLF-2]) and a membrane-bound pattern recognition receptor (toll-like receptor 2 [TLR2]) as critical signals in the mechanotransduction of HPF signals. Unlike normal LPF, which induced a small, transient NF-κB activation in PAECs, HPF induced strong and sustained increases in NF-κB activation in ECs. In addition to NF-κB, the cytoskeletal reorganization downregulated the transcription factor KLF-2, which is known to mediate the transcription of numerous vasodilatory, antithrombotic, and antiproliferative genes involved in endothelial homeostasis.103–105 We also identified TLR2 as another signaling molecule involved in HPF-induced EC activation. HPF induced expression of TLR2 ligands in ECs in our model system that are capable of binding TLR2 and generating autocrine proinflammatory signaling, which likely provides generation of continuous signals supporting EC dysfunction via NF-κB in the setting of HPF. Inhibition of TLR2 using pharmacologic (OxPAPC) and molecular (small interfering RNA–small interfering TLR2) approaches reduced HPF-induced NF-κB activation and endothelial inflammation. 106 TLR2 expression in distal PAECs was found to be significantly enhanced in both human PH and severe bovine PH in our study. TLR2-based autocrine signaling may be a novel target for intervention where early stiffness is documented to occur. These observations are consistent with recent studies highlighting the role of TLR2/4 signaling in cardiovascular diseases, such as atherosclerosis, via stress-induced ligands.107–110
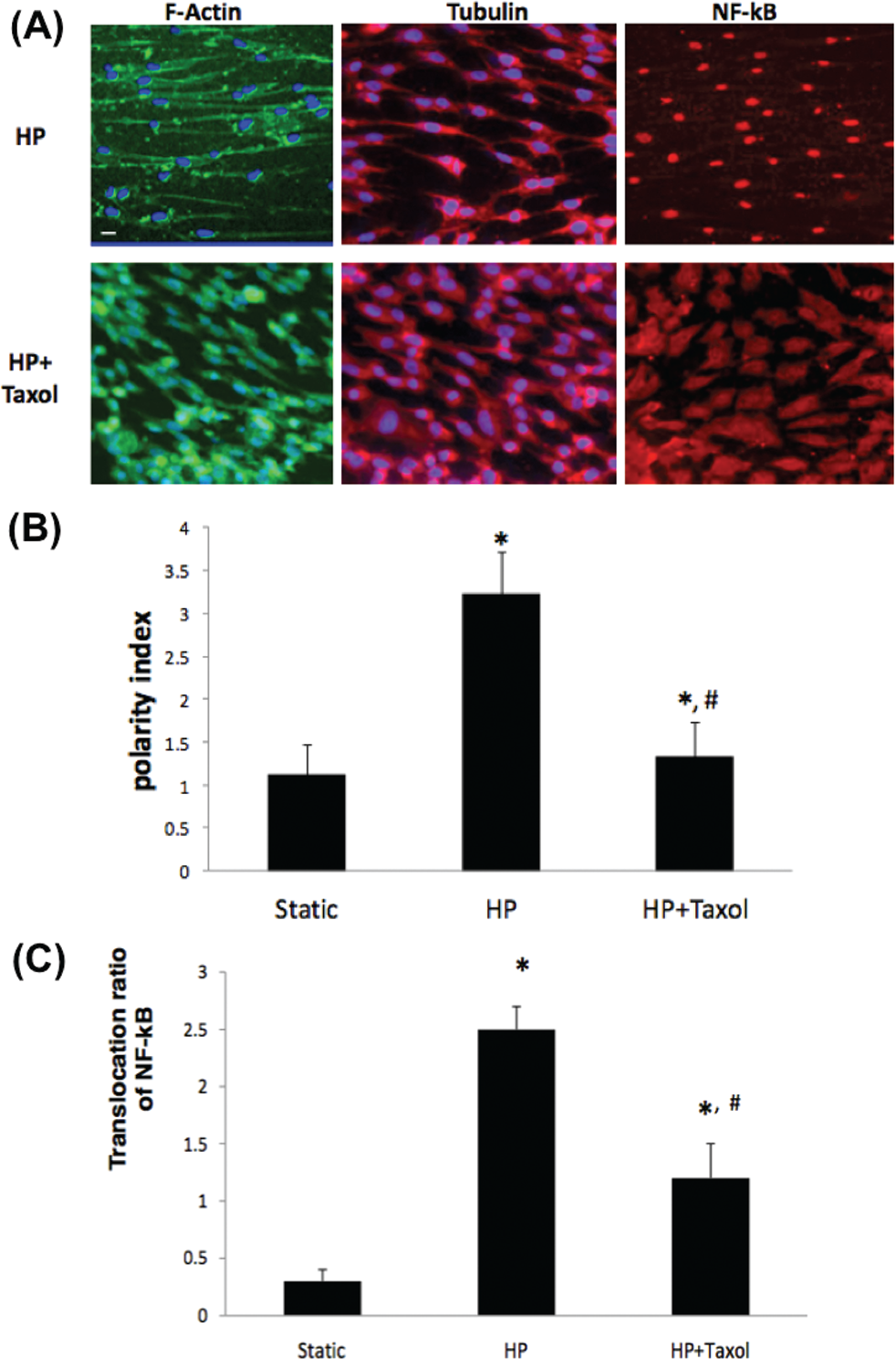
Effects of circulating taxol (10 nM) on the cell structure, polarity, and NF-κB translocation. A, Fluorescent images showing F-actin (green) and nuclei (blue), microtubulin (red), and NF-κB (red) in pulmonary arterial endothelial cells under HPF in the absence or presence of circulating taxol. B, Quantitative analysis of the cell polarity index, showing that circulating taxol significantly decreases HPF-induced polarity of cells. C, Quantitative analysis of NF-κB translocation, showing that circulating taxol significantly decreases HPF-induced NF-κB activation. *Significantly (P < .05) different from the untreated high-pressure (HP) condition. #Significantly (P < .05) different from the untreated static condition. HPF: high-pulsatility flow; NF-κB: nuclear factor κB; polarity index: ratio of maximum cell length to maximum cell width. 90
In addition to proinflammatory signals, the endothelium, uniquely situated at the interface between the blood and the vessel wall, is an efficient biological mechanotransducer that senses and converts flow shear forces to other biochemical signals, resulting in the production of cytokines and vasoactive agents capable of modulating smooth muscle tone and proliferation. To determine how FPI-induced endothelial dysfunction affects other vascular cells, we utilized a pulmonary circulatory system model, in which simulated pulsatile flow waves with varied FPIs were imposed on a multilayered vascular coculture composed of ECs and smooth muscle cells (SMCs) in a 3-dimensional collagen gel (Figure 5). 87 We showed that HPF increased SMC hypertrophy and SMC expression of contractile proteins α-SMA and smooth muscle–myosin heavy chain (SM-MHC), without affecting SMC proliferation, compared to both the LPF and static conditions. 87 These SMC responses were mediated via disordered vasoactive mediator production by ECs, including decreased endothelial NO synthase production and increased expression of angiotensin-converting enzyme (ACE), TGF-β1, and endothelin-1 (ET-1). 88 Targeting ACE and ET-1 with the ACE inhibitor ramiprilat and the ET-1 receptor inhibitor bosentan reduced SMC expression of α-SMA and SM-MHC in our coculture vascular mimetic system (Figure 6). 88 In addition to muscular tone and activity, adventitial fibroblast (AdvFB) responses, such as acquisition of a myofibroblast phenotype and enhanced migration (W. Tan, unpublished data), were also found to be regulated by ECs in response to high FPI. They might be explained, at least in part, by our observations that HPF stimulates TGF-β expression in ECs.
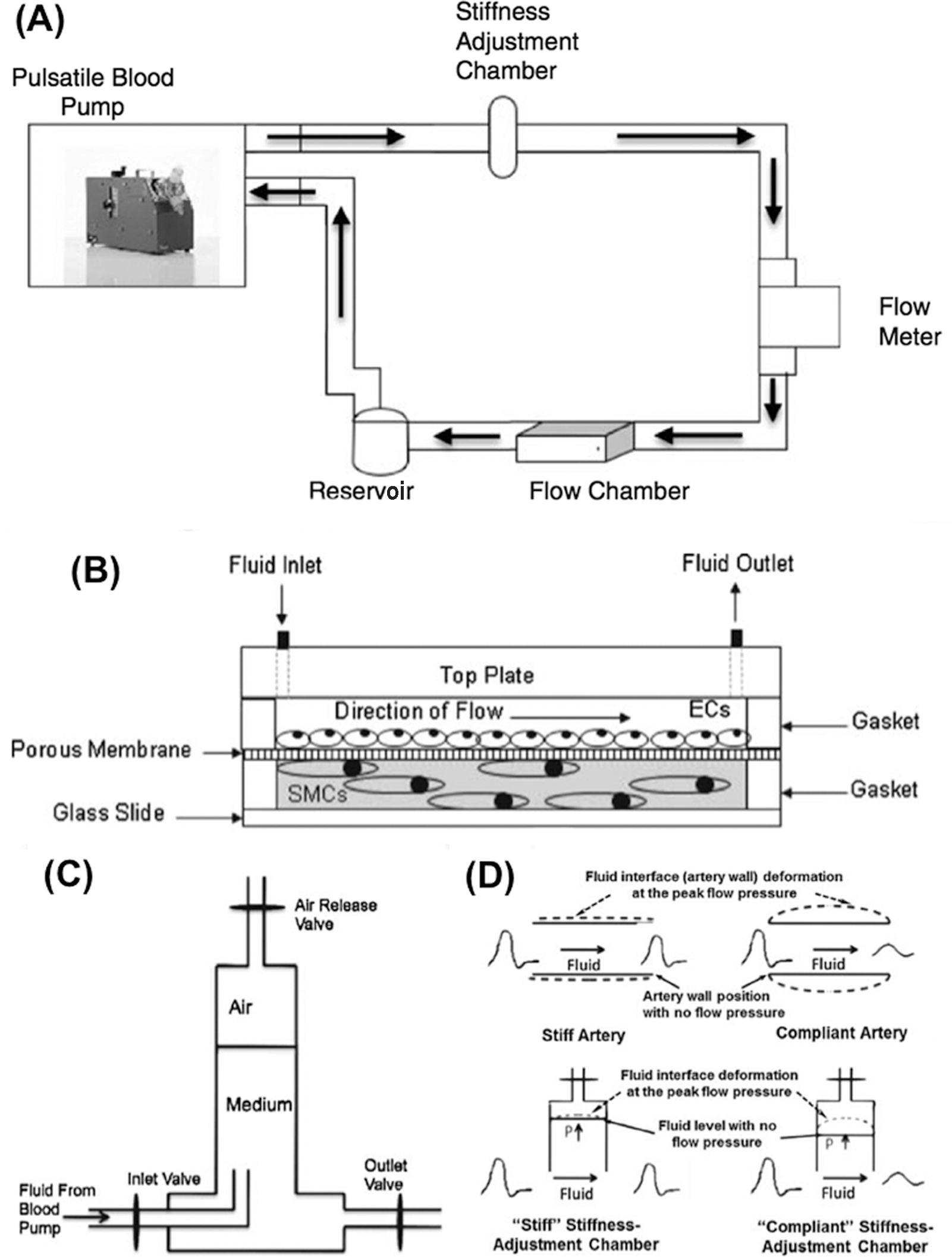
Schematic illustrations of the flow system (A), the mimetic coculture chamber (B), the stiffness-adjustment chamber (C), and the function similarity between a stiffness-adjustment chamber and an upstream large artery (D). A, The flow system demonstrates the flow circulation through different flow units. The arrows show the flow direction. B, Cross-sectional view of a flow coculture chamber with endothelial cells (ECs) seeded on a porous membrane in contact with smooth muscle cells (SMCs) embedded in a 3-dimensional collagen matrix. C, The stiffness-adjustment chamber has an air release valve for adjustments of liquid/air ratio as well as inlet and outlet valves allowing medium to flow through the chamber. Air in the chamber can absorb high pulse energy and reduce pulsatility of the flow wave. D, How the stiffness-adjustment chamber simulates the elastic function of the upstream elastic artery. The chamber is representative of the upstream artery in terms of its flow modulation function. A “stiff” chamber containing little air represents a stiff artery, which can barely expand at peak flow pressure, resulting in an unmodified high–pulse flow wave at the exit of the chamber. A “compliant” chamber, characterized by a high air/liquid ratio, represents a normal elastic artery, which is capable of undergoing large expansion under the peak (systolic) flow pressure, thus resulting in a dampened flow. The interface expansion shows the motion of the fluid position in the flow chamber or the artery wall under the peak (systolic) flow pressure. 87
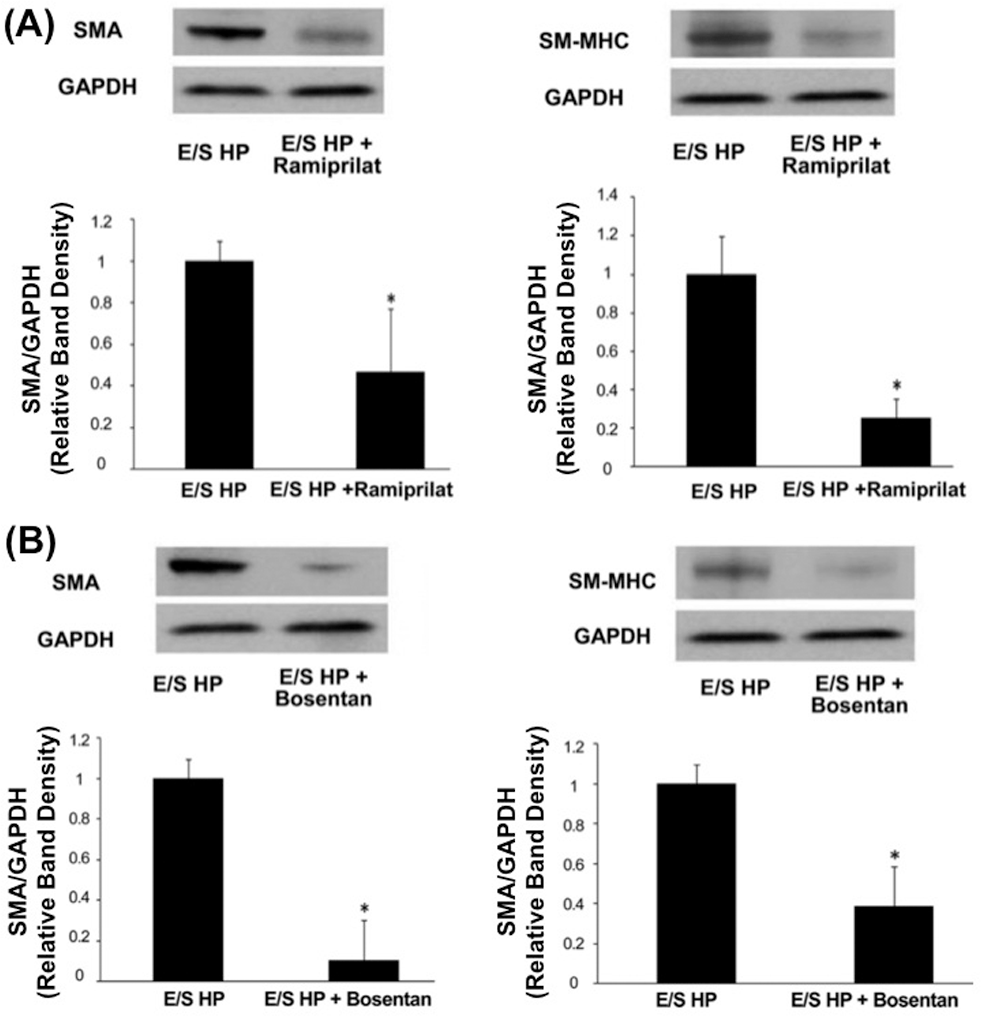
Angiotensin-converting enzyme (ACE) inhibitors (remiprilat) and ET-1 receptor antagonists (bosentan) reduced contractile protein expression in smooth muscle cells (SMCs) cocultured with endothelial cells (EC) under high pulsatility flow (E/S [i.e., EC/SMC] HP). Western blot results showed that SMC expression of smooth muscle actin (SMA) and smooth muscle–myosin heavy chain (SM-MHC) under E/S HP were significantly reduced by ACE inhibitor ramiprilat (A) and ET-1 receptor inhibitor bosentan (B). Both ramiprilat (10 μM) and bosentan (10 μM) were added in the flow media. *P < .05 compared with E/S HP. 88
Collectively, these findings showing that HPF can have significant effects on the functional phenotype of cells in all 3 layers of the vessel wall support a role for vascular stiffening and alterations in flow pulsatility in the distal PA remodeling observed in PH, which is characterized by structural and functional changes of all 3 layers of the PA, including medial hypertrophy; intimal fibrosis, consisting of highly heterogeneous cell types with many newly appearing myofibroblasts and/or inflammatory cells as well as adventitial fibrosis; and perivascular inflammation. The increased number of cells expressing α-SMA is a nearly universal finding in the remodeled artery; emerging evidence suggests that both ECs and AdvFB are possible sources of these SM-like cells (α-SMA+), likely via EndoMT and fibroblast activation, respectively.111,112 Ultimately, a more comprehensive understanding of hemodynamic effects on PA remodeling will require investigation of a greater variety of pulsatile flows and an elaboration of the combined effects of both the dynamic component (FPI) and the static component (mean WSS) of distal PA flow, correlating the cell responses to the FPI, mean WSS, and overall flow energy. It will also be important to explore the flow influence, together with that of other environmental stimuli (e.g., hypoxia inflammatory cells), in causing the pulmonary vascular remodeling.
CURRENT STRATEGIES OF ARTERIAL DESTIFFENING: DRUGS AND TREATMENTS
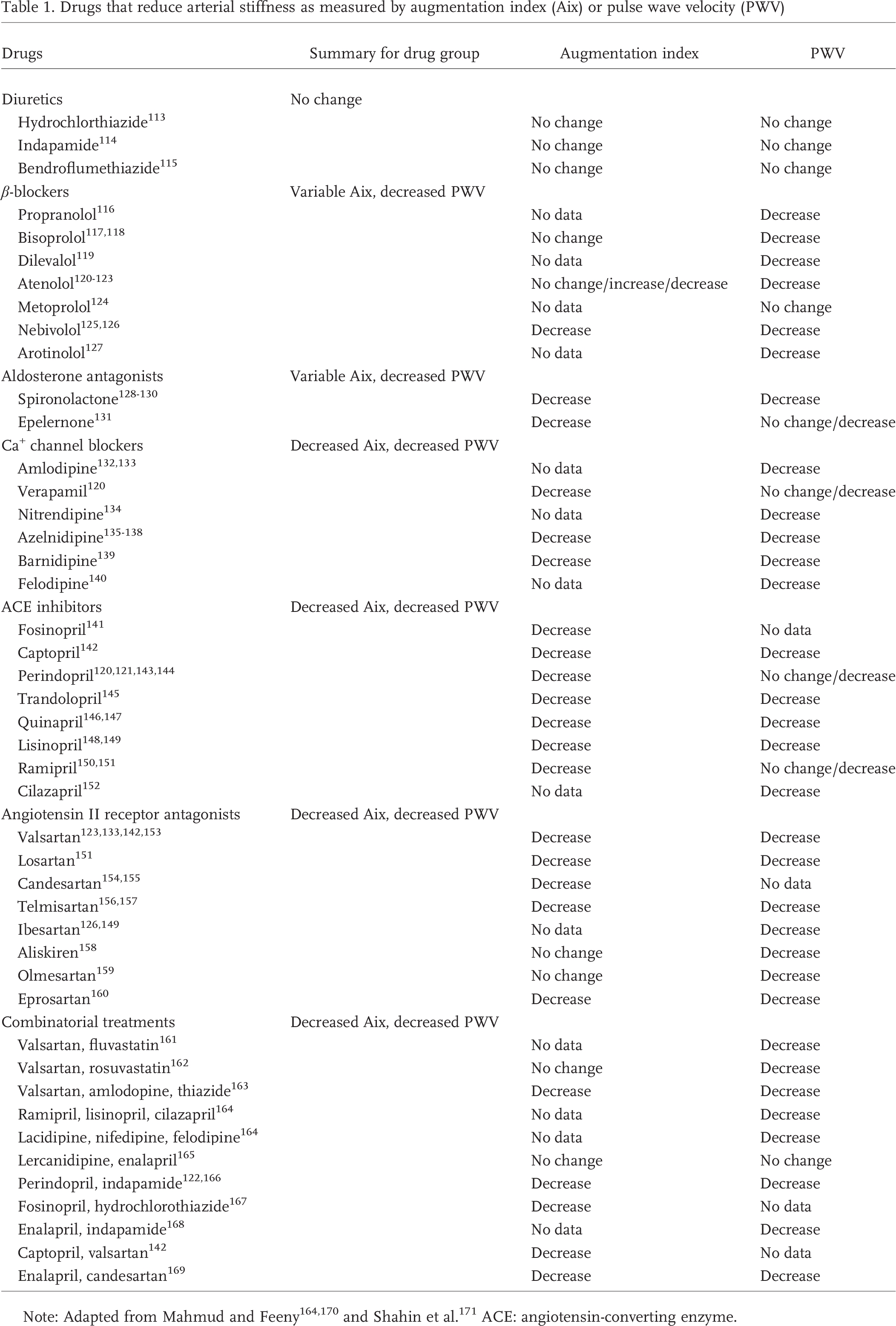
Collectively, the data shown above support the hypothesis that therapies aimed at decreasing arterial stiffness could be beneficial in treating PH. To our knowledge, the effects of current drug therapy for PH on impedance or PA stiffness are unknown. However, some insight may be gained by analyzing the experience of drug treatments for systemic hypertension, where, as demonstrated above, large-vessel stiffening plays an important role in morbidity and mortality. The effects of commonly used drugs on 2 indices used to assess stiffness are shown in Table 1, adapted from Mahmud and Feely125,164,170 Diuretics and vasodilators have no effect on these stiffening indices. 90 Calcium (Ca+) channel blockers have been used to reduce both pulse wave reflection and the augmentation index (Aix) with some success.120,135–137,139 Another approach gaining interest is to reduce fibrosis and/or modify structural proteins linked to stiffness. Drugs that inhibit angiotensin II and particularly aldosterone are intriguing in this regard.172,173 Both may have the added advantage of targeting both vascular and ventricular changes. Efforts to enhance elastin by blocking the elastolytic effects of neutrophils have yielded very exciting results in both the heart and the vasculature.174,175 However, translation to effective human treatment with these drugs has been limited by their toxicity, and this avenue remains one undergoing investigation. A different strategy that may also target both heart and arteries is the use of agents that break crosslinking of advanced glycation end products.176–180 Additional approaches include serine protease inhibitors and anti-inflammatory agents. 181
Drugs that reduce arterial stiffness as measured by augmentation index (Aix) or pulse wave velocity (PWV)
ACE inhibitors and renin angiotensin aldosterone system (RAAS) blockers
There is extensive literature to show that most ACE inhibitors and RAAS blockers have a positive effect on reducing arterial stiffness. The RAAS is traditionally described as acting primarily on the arterioles, with resulting vasoconstriction. However, the vascular effects of the RAAS involve modification of not only arteriolar but also large-artery structure and function, through effects on collagen and elastin production and degradation. One of the ways by which the RAAS may change arterial stiffness is through the potent vasoconstrictor angiotensin II. In healthy volunteers, angiotensin II infusion increases PWV in a manner that is only partly blood pressure dependent. 182 It also increases the Aix and aortic pulse pressure (PP) without any simultaneous change in peripheral PP. 183 Furthermore, environmental factors affecting the RAAS, such as sodium intake and the changes in sodium sensitivity with aging, play a major role in the increase in aortic stiffness.184,185 Traditionally, angiotensin II has been viewed as a primary factor causing adverse functional and structural alterations in the vessel wall. However, substantial evidence has emerged to show that aldosterone also plays an independent role in mediating cardiovascular damage. Aldosterone plays a major role in cardiac and vascular remodeling by regulating collagen turnover and fibrous-tissue formation, while there is also some evidence that it probably has short-term vascular effects, leading to vasoconstriction in both in vitro studies and in vivo in humans.170,186–188 Blacher et al. 189 have shown a relationship between increased plasma levels of aldosterone and decreased systemic compliance in patients with long-standing hypertension. To our knowledge, no studies have specifically addressed the role of RAAS antagonists in the vascular stiffening known to occur in PH.
β-blockers
β-blockers inhibit the effects of the sympathetic nervous system on the heart. This reduces the work of the heart, so that it requires less blood and oxygen. As a result, the heart does not have to work as hard, which in turn lowers blood pressure. β-blockers help control heart rate and are also used in the treatment of abnormal heart rhythms that are either too fast or irregular. Most studies have shown that β-blockers reduce pulse pressure.164,170 β-blockers lower the heart rate, which leads to an increase in PWV and the Aix.141,190 Kelly et al. 119 showed that vasodilating β-blockers may have a favorable influence on pulse wave reflection. However, there was no difference found between atenolol and nebivolol, a vasodilating β-blocker, in reference to their effect on the Aix. 125 It is well known that β-blockers have deleterious effects on patients with portopulmonary hypertension. 191 Yet it is suggested that β-blockers may be carefully administered to PH patients, even though β-blockers pose the threat of increasing the RV output. 192 De Man et al. 193 demonstrated that bisoprolol treatment in rats not only slowed the advancement toward right heart failure in experimental PH, by improving RV contractility and compliance, but also restored β-adrenergic receptor signaling and reduced RV fibrosis and inflammation.
Serine protease inhibitors
Serpins are a group of proteins with similar structures that inhibit proteases and have been used in the past in the treatment and management of systemic hypertension. Chae and Park 181 have demonstrated that brachial-ankle PWV increased with an increase in the serum level of complement 1 inhibitor. Klein et al. 194 demonstrated that combined inhibition of tyrosine and serine/threonine kinases, using sorafenib, prevents pulmonary remodeling and improves cardiac and pulmonary function by exerting direct myocardial antihypertrophic effects, probably mediated via the inhibition of the Raf (rapidly accelerated fibrosarcoma) kinase pathway.
Anti-inflammatory agents
Recent studies have elucidated the role of inflammation as a potential determinant of arterial stiffness.195–197 A decline in inflammation in patients with autoimmune diseases has been related to decreases in arterial stiffness.198–200 Rheumatoid arthritis and vasculitis have been shown to be associated with increased arterial stiffness, which may be driven by chronic vascular inflammation and ultimately arterial calcification, changes thought to be irreversible. 201 However, some studies have indicated that in patients with rheumatoid arthritis, PWV and endothelial function improved after anti-inflammatory treatment, which suggests that these changes may be partly reversible. 198 Even among the healthy older population, there is good evidence that levels of C-reactive protein are related to aortic stiffness. 202 Generally, it is thought that statins do not induce any improvement in arterial stiffness, yet some clinical trials have suggested that statins are beneficial in reducing arterial stiffness because of their pleiotropic anti-inflammatory effects.203–205
SUMMARY
Stiffening of the PAs (both large elastic and, likely, small resistance vessels) occurs in all forms of PH to some degree or another. In PH, it is still not clear whether arterial stiffening is a cause or a consequence, a question that will have to be addressed separately in all the different classes and forms of PH. However, it is evident that PA stiffening increases flow pulsatility in the pulmonary vasculature, which can contribute to endothelial dysfunction by stimulating a proinflammatory, vasoconstricting, and profibrogenic milieu (Figure 7).52,85,88,89 The disordered flow-buffering function of elastic PAs in PH likely perpetuates dysfunction of distal arteries (Figure 7). The multifaceted role of stiffening-induced HPF in EC dysfunction includes stepwise molecular events underlying PA hypertrophy, inflammation, EndoMT, and fibrosis. Disordered proximal-distal PA coupling, together with other microenvironmental alterations, may also play a critical role in continuously increasing ventricular afterload, ultimately causing RV failure and death. Unraveling the causes of proximal vascular stiffening, as well as those of HPF-induced cellular and molecular alterations in the distal pulmonary vasculatures, could lead to important new therapeutic options to halt PA remodeling and PH progression. Further refining a mimetic vascular physiological model similar to the so-called lung on a chip206,207 may be instrumental to such understanding. Future studies should be aimed at the root cause of arterial stiffening to develop therapeutic interventions, which will treat the cause and not the symptom.
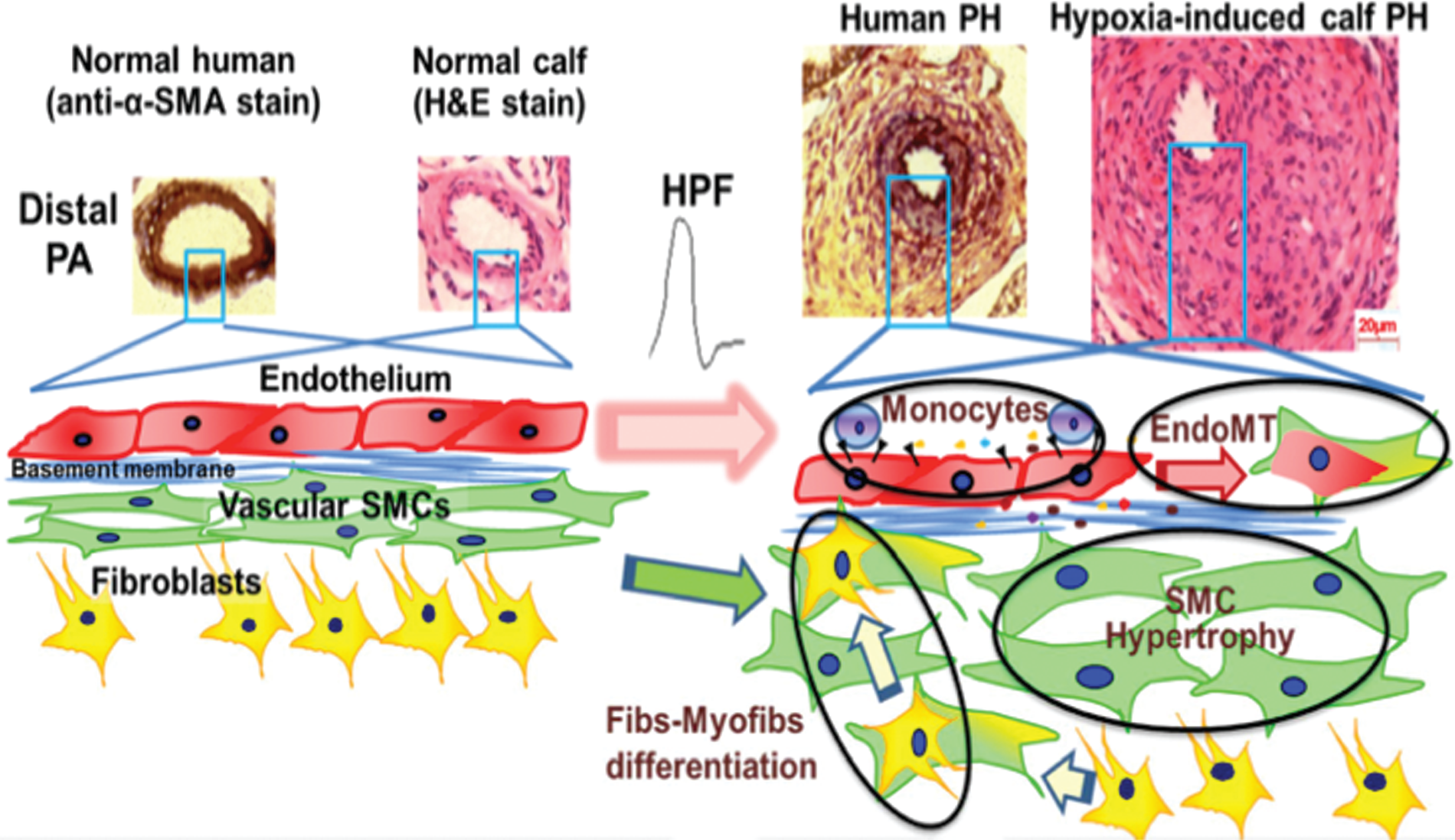
Summary of the effect of large-elastic-pulmonary-artery (PA) stiffening on the distal circulation. Large-PA stiffening increases flow pulsatility. Increased pulsatility increases the flow shear stress downstream as a result of decreases in artery diameter. This, along with the high pulsatile flow (HPF), causes distal endothelial dysfunction that leads to intimal inflammation and fibrosis, medial hypertrophy, and adverse adventitial remodeling. α-SMA: α–smooth muscle actin; endoMT: endothelial-to-mesenchymal transition; fibs-myofibs: fibroblasts-myofibroblasts; H&E: hematoxylin and eosin; PH: pulmonary hypertension; SMC: smooth muscle cell.