Abstract
Transition from prostacyclin analogue infusion to oral therapy in patients with pulmonary arterial hypertension (PAH) is possible with acceptable short- and midterm results. However, there is a paucity of data on long-term outcomes after successful transition. Using a predefined protocol, transition to oral therapy was attempted in 22 patients with clinically stable PAH. Clinical and hemodynamic data were retrospectively collected at baseline as well as during and after transition. Parameters for successful versus nonsuccessful transition were also evaluated. All patients had severe PAH at baseline and showed clinical and hemodynamic improvement with prostacyclin analogue infusion. Initial oral agents used for transition were bosentan (63.6%), sildenafil (31.8%), and tadalafil (4.5%). Combination therapy was used in 68% of the patients. Successful transition was achieved in 11 patients (50%) with a mean transition duration of 16 months. After successful transition, clinical and hemodynamic parameters remained stable at midterm (mean, 18 months) and long-term (mean, 60 months) follow-up. Compared with the successful transition group, patients who experienced failure were older, had a higher frequency of idiopathic PAH, and had worse hemodynamic parameters during treatment with prostacyclin analogue alone, as well as during the transition period. In conclusion, successful transition from prostacyclin analogue infusion to oral therapy can be achieved in a significant proportion of patients with clinically stable PAH. After an initial successful transition, patients were able to maintain clinical and hemodynamic stability at the mid- and long-term follow-up.
INTRODUCTION
Pulmonary arterial hypertension (PAH) is a life-threatening disease characterized by a progressive increase in pulmonary vascular resistance (PVR) that leads to right ventricular failure, with poor prognosis if untreated.1–3 The pathogenesis of PAH is still not completely understood; however, endothelial dysfunction and proliferative vasculopathy, leading to a local imbalance between vasoconstrictor and vasodilator mediators producing marked vasoconstriction, have been proposed, and they are targets of novel treatments.4,5
Prostacyclin analogue infusion therapy has been shown to improve hemodynamics, functional status, and survival, and it remains the gold standard for treatment of patients with severe PAH. 6 However, prostacyclin infusion is associated with significant side effects and complications. 7 Furthermore, abrupt discontinuation of prostacyclin can cause severe rebound pulmonary hypertension that may result in clinical deterioration and even death.7,8
Orally administered endothelin receptor antagonists, phosphodiesterase 5 inhibitors, and inhaled prostacyclin analogues have also demonstrated clinical and hemodynamic improvement in patients with PAH.9–12 Therefore, the possibility of transitioning patients off prostacyclin infusion to combination therapy with oral or inhaled therapy has been considered. It has been shown that the transition can be achieved without compromising hemodynamic status.13–21 However, the predictors of successful transition and long-term outcomes are not known. In this study, we compared clinical and hemodynamic data in PAH patients with or without successful transition from intravenous prostacyclin to oral therapy and evaluated the potential predictors of successful transition.
METHODS
Patients
After the Mount Sinai Medical Center (Miami Beach, FL) Institutional Review Board approved the protocol, we retrospectively reviewed the charts of all consecutive patients seen at the pulmonary hypertension clinic at our institution between January 1998 and September 2011. Patients who were receiving epoprostenol or treprostinil continuous infusion with an attempted transition to oral therapy were identified. Indications for transition were either significant side effects/adverse events or clinically stable PAH. Patients without evidence of right heart failure, in New York Heart Association (NYHA) functional class I or II, and without changes in their prostacyclin analogue dose for at least 3 months were classified as clinically stable.
Clinical, echocardiographic, and hemodynamic data were obtained at five different treatment periods for patients successfully transitioned from prostacyclin analogue infusion to oral therapy. Baseline data were considered those obtained at diagnosis or before initiation of any prostacyclin analogue infusion; PGI2-alone data were considered those obtained during treatment with stable doses of a prostacyclin analogue infusion (before initiation of oral therapy); transition data were considered those obtained during receipt of target doses of oral PAH therapy (before discontinuation of the prostacyclin infusion); and mid- and long-term follow-up data were considered those obtained between 6 and 30 months and >30 months, respectively, after transition from prostacyclin infusion to oral therapy alone. For patients in whom the transition attempt failed, clinical, echocardiographic, and hemodynamic data were collected at baseline, during treatment with prostacyclin infusion alone, and during treatment with a combination of oral agent(s) and prostacyclin infusion.
Transition
An endothelin receptor antagonist (bosentan or ambrisentan) or a phosphodiesterase 5 inhibitor (sildenafil or tadalafil) was started at the recommended doses at least 1 month before weaning the prostacyclin analogue infusion. The prostacyclin analogue infusion rate was then decreased by 0.5–2 ng/kg/min every week on an outpatient basis, as tolerated by the patient. A second oral agent (different class) was added when the prostacyclin analogue infusion rate was difficult to decrease. When the infusion rate had been titrated down to 6 ng/kg/min, the patients were hospitalized in the intensive care unit with continuous hemodynamic monitoring for the final prostacyclin analogue infusion discontinuation process. The transition attempt was discontinued if the patient was unable to taper down the prostacyclin infusion dose despite maximal doses of oral agent(s) (transition failure). In patients who experienced failure, the prostacyclin infusion dose was readjusted to continue with their pretransition clinical stability.
Statistical methods
Continuous variables are expressed as mean ± standard deviation (SD) and were analyzed using analysis of variance followed by the Tukey test or Student's t test when appropriate. All dichotomous variables were compared using χ 2 analysis. A P value of <0.05 was considered statistically significant. Statistical analyses were done using SPSS software (ver. 17; SPSS, Chicago, IL).
RESULTS
Pretransition
Twenty-two patients who received treatment with prostacyclin analogue infusion and had undergone transition to oral therapy were included in the study. The cohort consisted of 22 patients (16 females [73%] and 6 males [27%]), with a mean ± SD age of 56 ± 15 years. All of the patients had World Health Organization (WHO) group I PAH (Tables 1, 2). At baseline, all patients were in NYHA class III or IV with hemodynamic parameters compatible with severe PAH, and 68% (n = 15) had clinical evidence of right heart failure (Table 1).
Baseline clinical and hemodynamic characteristics
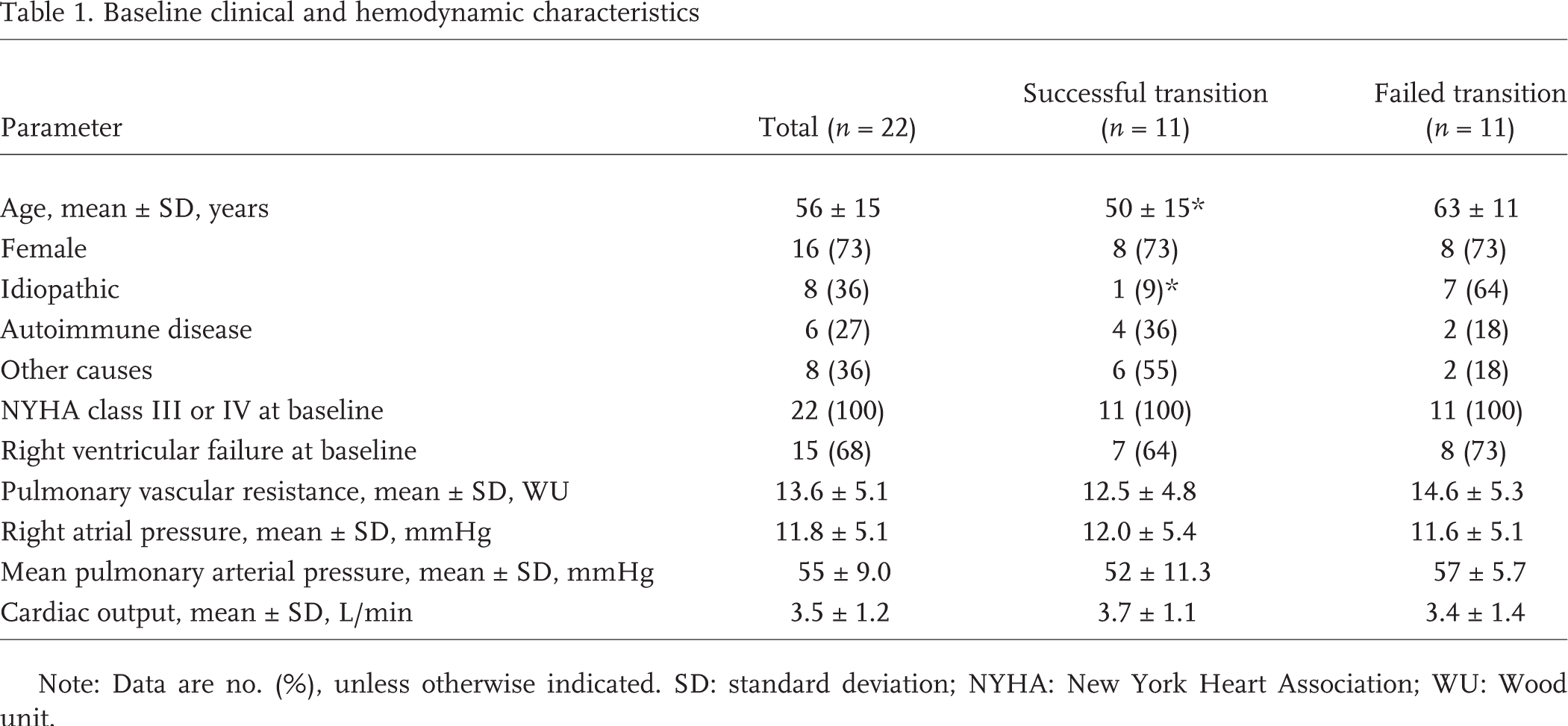
Note: Data are no. (%), unless otherwise indicated. SD: standard deviation; NYHA: New York Heart Association; WU: Wood unit.
Demographics and pulmonary arterial hypertension targeted therapy at baseline, during transition, and at follow-up
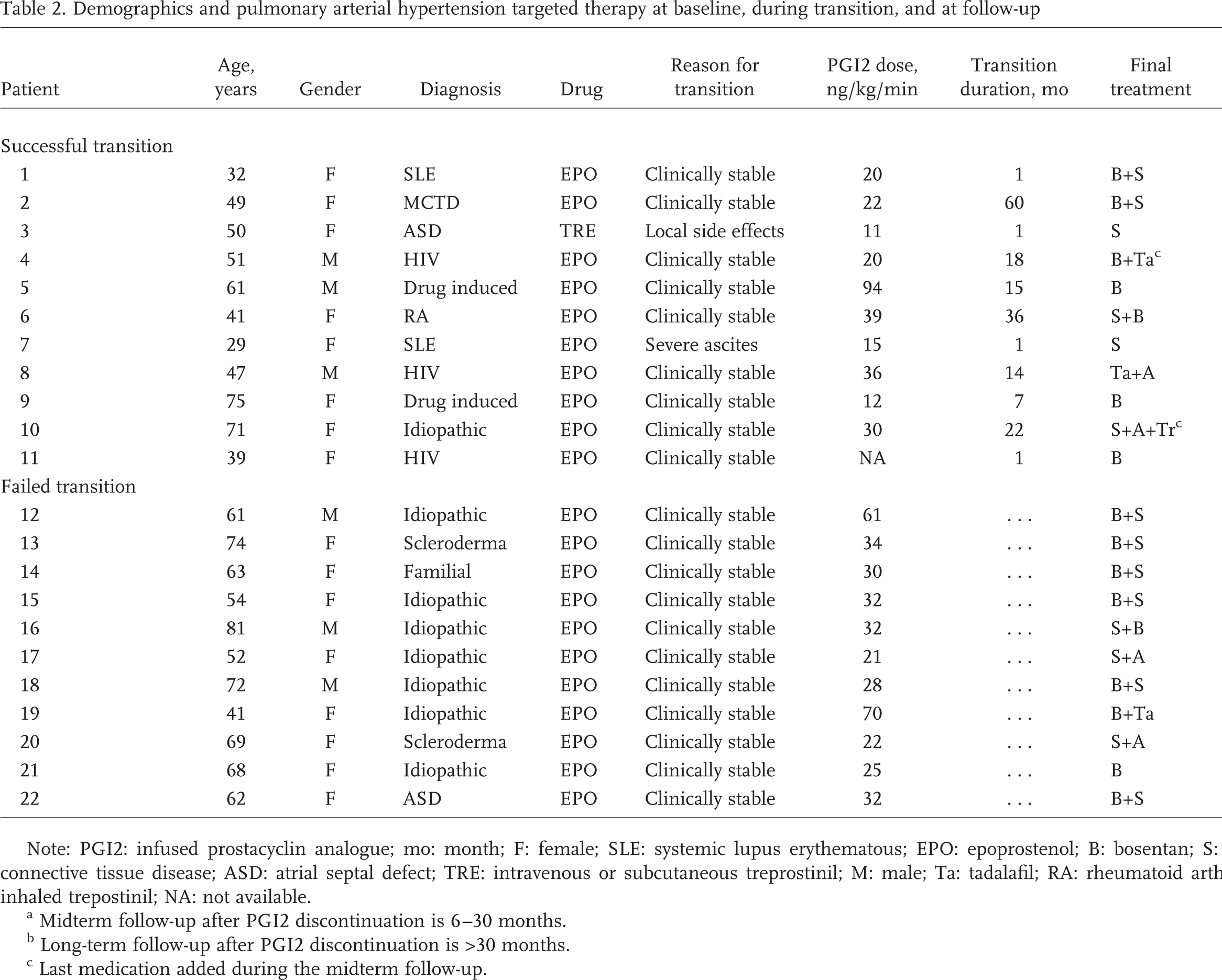
Note: PGI2: infused prostacyclin analogue; mo: month; F: female; SLE: systemic lupus erythematous; EPO: epoprostenol; B: bosentan; S: sildenafil; MCTD: mixed connective tissue disease; ASD: atrial septal defect; TRE: intravenous or subcutaneous treprostinil; M: male; Ta: tadalafil; RA: rheumatoid arthritis; A: ambrisentan; Tr: inhaled trepostinil; NA: not available.
Midterm follow-up after PGI2 discontinuation is 6–30 months.
Long-term follow-up after PGI2 discontinuation is >30 months.
Last medication added during the midterm follow-up.
There were 21 patients (95.4%) started on epoprostenol infusion and 1 patient (4.5%) started on subcutaneous treprostinil (Table 2), with a mean ± SD epoprostenol maximal dose of 34 ± 20 ng/kg/min. During treatment with the prostacyclin analogue infusion alone (PGI2 alone), all patients showed marked clinical improvement from baseline, with NYHA class I or II, and none had right heart failure. Compared with baseline, the hemodynamic parameters (mean ± SD) were significantly better during treatment with prostacyclin analogue infusion, including mean pulmonary arterial pressure (MPAP; 55 ± 9.0 vs. 44 ± 10.8 mmHg; P = 0.003), right atrial pressure (RAP; 11.8 ± 5.1 vs. 6.2 ± 5.0 mmHg; P = 0.005), cardiac output (CO; 3.5 ± 1.2 vs. 4.9 ± 1.3 L/min; P = 0.002), and PVR (13.06 ± 5.1 vs. 7.0 ± 2.7 Wood units [WU]; P < 0.001).
Transition
Clinically stable PAH and significant side effects from prostacyclin were the reason for transition in 91% (n = 20) and 9% (n = 2) of the patients, respectively (Table 2). The initial agents used for transition were bosentan (14 patients [63.6%]), sildenafil (7 patients [31.8%]), or tadalafil (1 patient [4.5%]). The combination of an endothelin receptor antagonist (bosentan or ambrisentan) and a phosphodiesterase 5 inhibitor (sildenafil or tadalafil) was used in 15 patients (68%). Successful transition was achieved in 11 patients (50%). The mean duration of prostacyclin analogue therapy before discontinuation and the mean transition duration were 56 and 16 months, respectively. Shortly before transition was successfully completed (transition data; n = 11), patients remained in NYHA class I or II, without evidence of heart failure (Fig. 1). There was no significant difference in the hemodynamic parameters (mean ± SD) before and after successful transition, including MPAP (33 ± 8.2 vs. 32 ± 6.4 mmHg), RAP (2.8 ± 2.2 vs. 3.9 ± 3.6 mmHg), CO (5.4 ± 1.5 vs. 5.2 ± 1.7 L/min), and PVR (5.1 ± 2.0 vs. 4.9 ± 2.1 WU; Fig. 2). Patients in the successful transition group who had worse baseline pulmonary hemodynamics (PVR of >10 WU) more frequently required the use of combination therapy to achieve transition (P = 0.013).
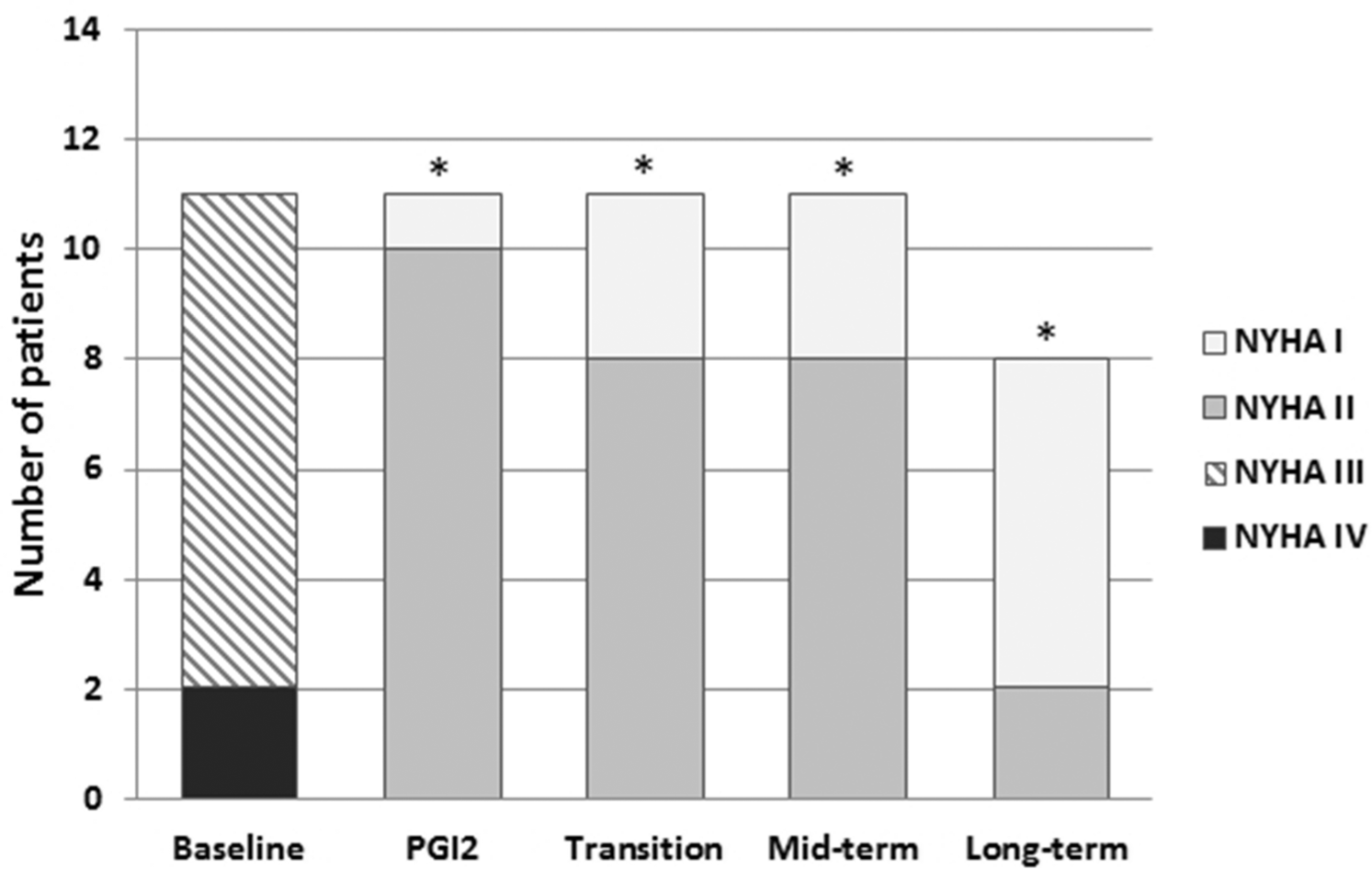
New York Heart Association (NYHA) functional class of patients in the successful transition group. Data are shown as the number of patients in each NYHA functional class at baseline, after therapy with intravenous prostacyclin (PGI2), during transition, and at mid- and long-term follow-up. Asterisks indicate significant differences from baseline (P < 0.001).
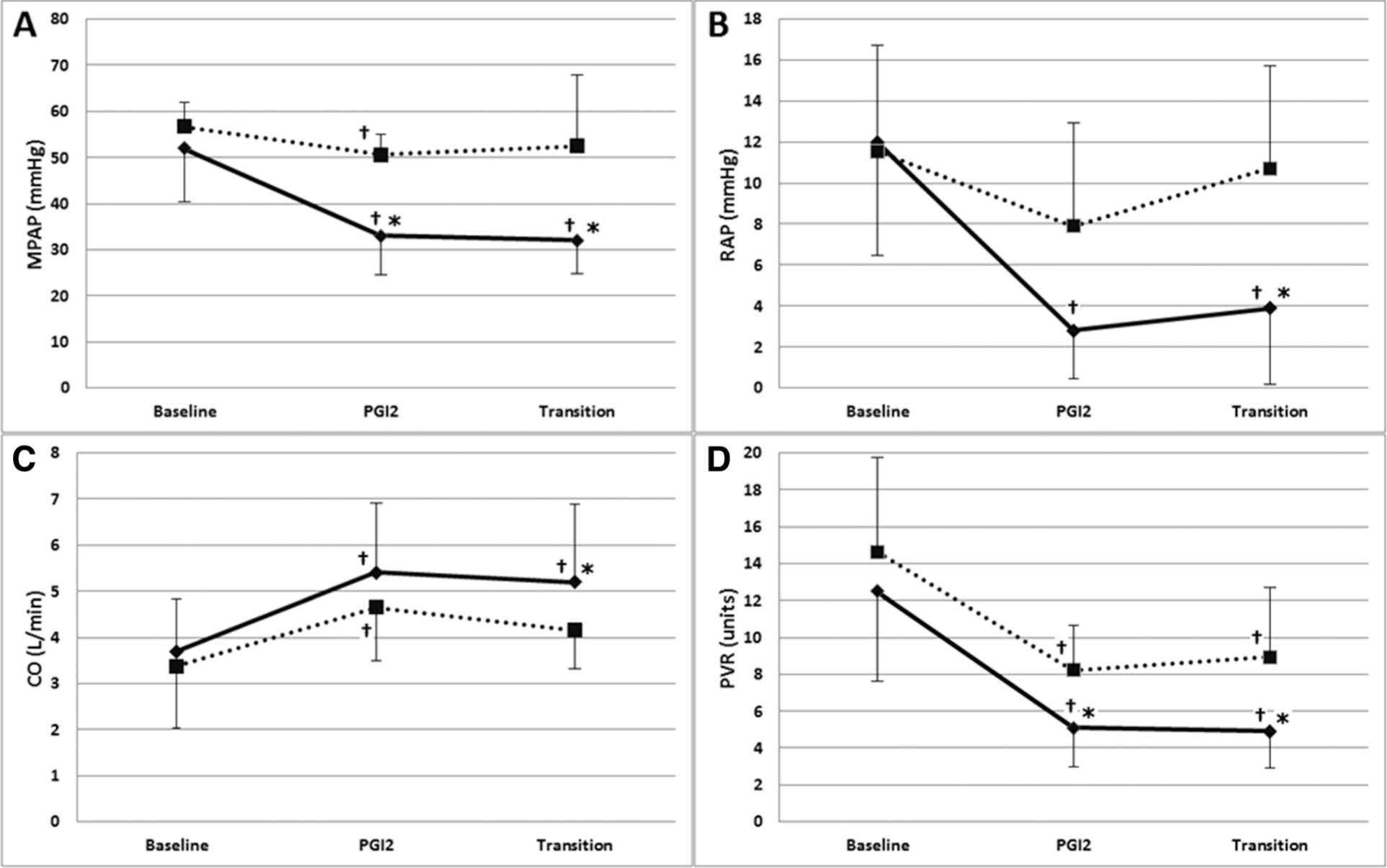
Pulmonary hemodynamics for the successful and failed transition groups at baseline, after therapy with intravenous prostacyclin (PGI2), and during transition. Data for the successful transition (solid line) and the failed transition (dotted line) groups are shown as mean ± standard deviation for mean pulmonary artery pressure (MPAP; A), right atrial pressure (RAP; B), cardiac output (CO; C), and pulmonary vascular resistance (PVR) in Wood units (D). Daggers indicate significant differences from baseline, and asterisks indicate significant differences from the failed transition group.
Transition failure
Patients in the failed transition group were older (mean age, 63 vs. 50 years; P = 0.027) and had more idiopathic pulmonary hypertension (64 vs. 9%; P = 0.012) than patients in the successful transition group (Table 1). Baseline clinical and hemodynamic parameters were similar in both groups (Table 1). Both groups had statistically significant improvement in hemodynamic parameters during treatment with prostacyclin analogue infusion except for mean RAP in the failed transition group (Fig. 2). Compared with patients in the failed transition group, patients with successful transition had a better improvement of hemodynamic parameters with PGI2 infusion alone, including RAP (2.8 ± 2.2 vs. 7.9 ± 5.2 mmHg; P = 0.058), MPAP (33 ± 8.2 vs. 51 ± 5.6 mmHg; P < 0.001), and PVR (5.1 ± 2.0 vs. 8.2 ± 2.5 WU; P = 0.014; Fig. 2). For the failed transition group (n = 11), the addition of oral therapy (an endothelin receptor antagonist alone or in combination with a phosphodiesterase 5 inhibitor) to the treatment with the prostacyclin analogue infusion did not significantly change any hemodynamic parameter (mean ± SD), including MPAP (51 ± 5.6 vs. 52 ± 15.4 mmHg), RAP (7.9 ± 5.2 vs. 10.7 ± 5.1 mmHg), CO (4.7 ± 1.1 vs. 4.2 ± 0.9 L/min), or PVR (8.2 ± 2.5 vs. 8.9 ± 3.8 WU; Fig. 2). During transition, all of the hemodynamic parameters were better in the successful versus the failed transition group (Fig. 2). Univariable analysis was performed to assess for possible predictors of transition failure. Age of >55 years, idiopathic PAH, use of combination therapy, and hemodynamic parameters during treatment with prostacyclin infusion alone (including RAP of >5 mmHg, MPAP of >40 mmHg, PSAP of >70 mmHg, and PVR of >6.5 WU) were identified as significant predictors. However, given the small number of patients, none of these variables achieved statistical significance in the multivariable analysis.
Follow-up
Midterm follow-up data were available for all patients (n = 11) who had an initial successful transition (mean follow-up, 18 months; Table 2). There were no differences in clinical or hemodynamic parameters at the midterm follow-up after successful transition (Figs. 1, 3). However, in 2 patients the addition of another oral agent (tadalafil) or inhaled treprostinil was required during this period. Up-to-date long-term follow-up data have been obtained for 8 patients (mean follow-up, 60 months; Table 2); there were no significant differences with regard to clinical or hemodynamic parameters after successful transition (Figs. 1, 3). None of the patients required additional oral agents after 30 months. The hemodynamic parameters of all of the patients who completed a successful transition are shown in Figure 3. There were no deaths at any point during the follow-up period after successful transition. However, 3 (27%) of 11 patients in the failed transition group died because of progression of their disease despite receiving optimal medical therapy.
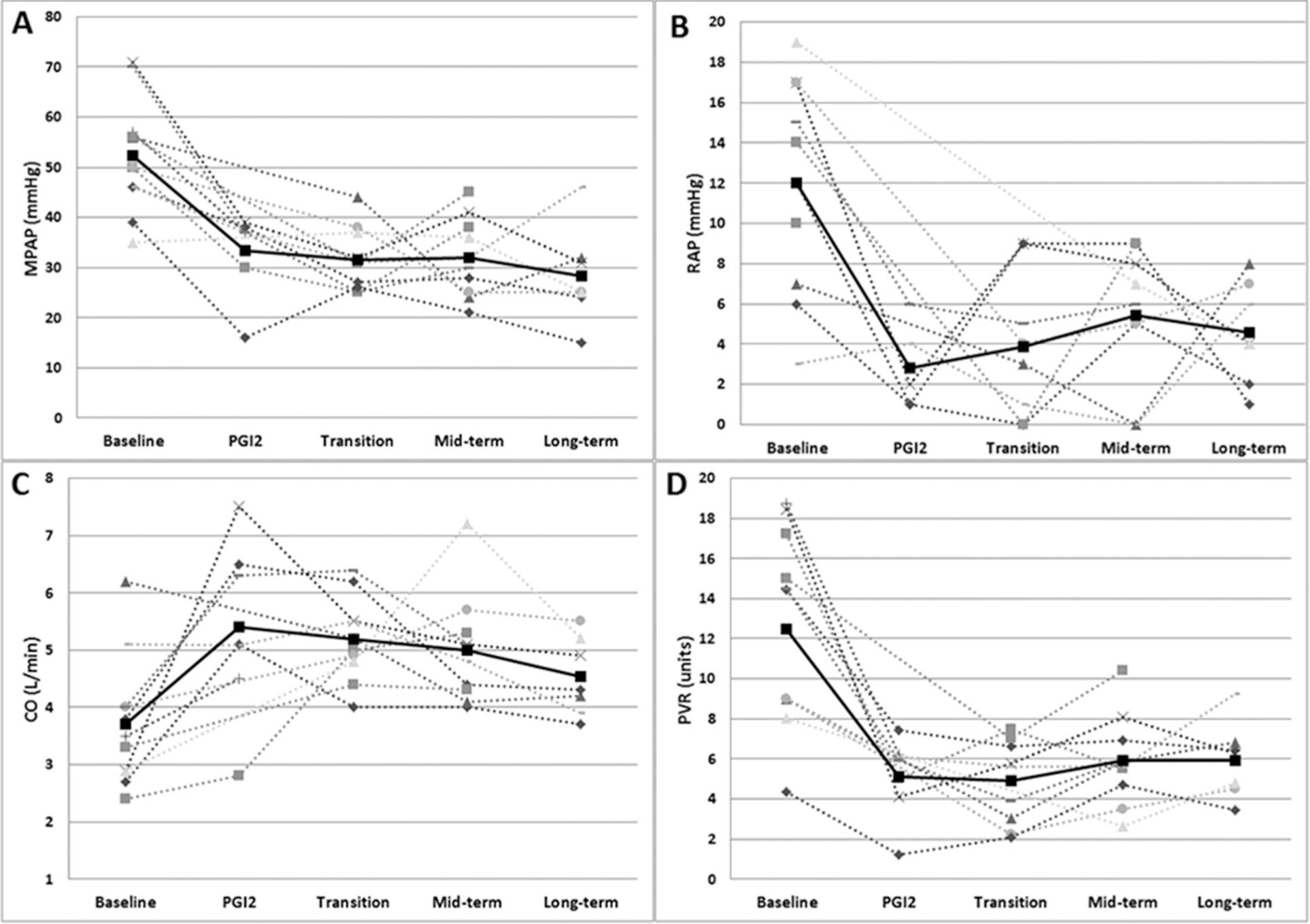
Pulmonary hemodynamics for the successful transition group at baseline, after therapy with intravenous prostacyclin (PGI2), during transition, and at mid- and long-term follow-up. Shown are data for individual patients and means for mean pulmonary artery pressure (MPAP; A), right atrial pressure (RAP; B), cardiac output (CO; C), and pulmonary vascular resistance (PVR) in Wood units (D).
DISCUSSION
Our study demonstrates that half of patients with clinically stable PAH receiving continuous infusion of prostacyclin analogues can be successfully transitioned to oral therapy. We also provide evidence that after successful transition clinical and hemodynamic improvement can be maintained at the long-term follow-up for up to 5 years.
Different protocols to transition patients from prostacyclin analogue infusion to oral therapy have been used,13–18 and there are no guidelines to safely achieve this transition. Most of the reported protocols were done on an outpatient basis and used a fixed-interval or fixed-dose weaning schedule,13–16 sometimes with adjustments on the basis of symptoms. 16 Our protocol consisted of a symptom- and hemodynamic-guided weaning process that was tailored to each patient. The length of the transition period varied widely among the prior studies, ranging from as low as 6.6 weeks 16 to up to 3.4 years in pediatric patients. 18 In our study, the mean duration of transition was longer than that in most of the prior studies in the adult population (16 vs. 4–12 months).13–15 This difference in transition length may be explained by the type of protocol we used or simply by the fact the mean prostacyclin analogue dose before transition was higher in our study.13,14,16,17
It has been shown that the rate of initial success after attempted transition from prostacyclin infusion to oral therapy ranges from 45% to 100%;13–20 however, long-term success may be limited.13,15,19 Suleman and Frost 19 and Steiner et al. 15 reported a success rate of 65% and 45%, respectively, while only 40% and 32% of their patients remained off prostacyclin infusion at 12 months. In the present study, we report a comparable initial success rate (50%); however, all of the transitioned patients were able to maintain clinical and hemodynamic stability during 5 years of follow-up. The high long-term success rate achieved may be due to the fact that a combination of an endothelin receptor antagonist and a phosphodiesterase 5 inhibitor was employed in 68% of the patients in our study. This is consistent with previous observations showing a higher success rate with combination therapy14,18 than with monotherapy used for transition.15,19
Predictors of successful transition are not well established because of the small number of patients in different studies. Although the etiology of PAH has not been related to the transition outcome, one study has suggested that patients with systemic lupus erythematous may have better long-term outcomes. 14 In our study, compared with the successful transition group, patients who experienced transition failure were significantly older, and more had idiopathic PAH. Older patients may have had PAH for a longer period of time, and therefore they may have had a more advanced stage of the disease, making them less likely to transition successfully. With the exception of patients with idiopathic PAH, who may have worse disease than others, we found no correlation between the etiology of PAH and the transition outcome. Similar to the results of one study, 14 we found no correlation between baseline hemodynamic parameters and transition outcome. This is in contrast to the observation of Steiner et al., 15 who found that lower baseline systolic and mean pulmonary pressures were predictors of successful transition. Lower pulmonary artery pressure and PVR during treatment with prostacyclin analogue have been reported as possible predictors of successful transition.13,19 Diaz-Guzman et al. 14 showed that patients who were successfully transitioned had higher CO and lower MPAP and PVR prior to prostacyclin analogue discontinuation, compared with patients in the failed transition group. Similarly, patients in our study who successfully transitioned had significantly better hemodynamic parameters during treatment with prostacyclin analogue alone as well as during the transition period. Thus, it is possible that an incomplete response to the prostacyclin analogue may be a significant predictor of transition attempt outcome. Although our analysis was limited by the number of subjects in the cohort and we could not identify clear predictors of transition failure in the multivariable analysis, RAP of >5 mmHg, MPAP of >40 mmHg, PSAP of >70 mmHg, and PVR of >6.5 WU during treatment with prostacyclin infusion were significantly associated with transition failure in the univariable analysis. Patients with these clinical characteristics and hemodynamic cutoffs may have a higher chance of failure, and therefore the decision of whether to attempt a transition should be individualized.
The prostacyclin analogue dose before transition has also been related with transition outcome. Two prior studies have found that lower doses of prostacyclin analogue were associated with successful transition,15,19 while in another study transitioned patients were receiving higher doses compared with those who experienced transition failure. 14 Diaz-Guzman et al. 14 found that successfully transitioned patients had a longer duration of prostacyclin therapy, suggesting that such therapy might positively affect remodeling of the pulmonary vasculature. We did not find any correlation between prostacyclin dose or duration of therapy and transition outcomes. Prostacyclin analogue excess symptoms during transition, longer duration of oral therapy before prostacyclin analogue infusion discontinuation, slow weaning process, and combination therapy have also been suggested as possible predictors of successful transition,14,15 and some of these might have positively affected the success rate in our study.
There is clear evidence that successful transition from prostacyclin analogue infusion to oral therapy can be achieved in selected patients with clinically stable PAH.13–20 Prior studies have also demonstrated that most of those patients maintain clinical and hemodynamic stability at short- and midterm follow-up.13–20 However, there is a paucity of data on long-term outcomes (>24 months) after successful transition in adults. Melnick et al. 18 reported a >90% success rate at a mean follow-up of 3.3 years in pediatric patients with idiopathic or familial PAH. Only one study has reported long-term results in an adult population. 21 From a group of 23 patients, Suleman and Frost 19 presented 11 (48%) patients who were successfully transitioned to an oral endothelin receptor antagonist and were able to maintain clinical stability at the midterm follow-up (mean, 9.6 months). Those 11 patients were followed up for 5 years, and their outcomes were presented by Safdar 21 in 2009. It was shown in that study that after initial successful transition, 64% (7/11) of the patients resumed parenteral prostacyclin therapy because of clinical deterioration, with a mean duration off prostacyclin of only 28 ± 21 months. 21 The author concluded that those patients were able to have a “prostanoid-free honeymoon period” without compromising clinical status long term. Our data are similar to their findings with regard to the initial and midterm success rates. However, the present study shows for the first time that patients carefully and slowly transitioned to single or combination oral therapy can continue enjoying clinical stability for up to 5 years without need of resuming parenteral prostacyclin therapy.
Our study has various limitations. It is a single-center retrospective study, with specific selection criteria and our own transition protocol. Therefore, our results may not be reproducible in other centers with different transition approaches. Although our results are similar to those of some of the prior published reports, the small sample size limits the ability to draw firm conclusions.
In conclusion, a significant proportion of clinically stable patients with severe PAH receiving treatment with prostacyclin analogue infusion can be successfully transitioned to oral therapy. Specific predictors of successful transition are difficult to identify; however, those receiving of combination therapy, younger patients, those with nonidiopathic PAH, and better responders to the prostacyclin analogue are more likely to achieve a long-term successful transition.
Footnotes
ACKNOWLEDGMENTS
Presented at the American College of Cardiology 2013 Scientific Sessions, San Francisco, California, March 9, 2013.
