Abstract
Background
Screening for unhealthy alcohol use in routine consultations can aid primary health care (PHC) providers in detecting patients with hazardous or harmful consumption and providing them with appropriate care. As part of larger trial testing strategies to improve implementation of alcohol screening in PHC, this study investigated the motivational (role security, therapeutic commitment, self-efficacy) and organizational context (leadership, work culture, resources, monitoring, community engagement) factors that were associated with the proportion of adult patients screened with AUDIT-C by PHC providers in Colombia, Mexico and Peru. Additionally, the study investigated whether the effect of the factors interacted with implementation strategies and the country.
Methods
Pen-and-paper questionnaires were completed by 386 providers at the start of their study participation (79% female, Mage = 39.5, 37.6% doctors, 15.0% nurses, 9.6% psychologists, 37.8% other professional roles). They were allocated to one of four intervention arms: control group; short training only; short training in presence of municipal support; and standard (long) training in presence of municipal support. Providers documented their screening practice during the five-month implementation period. Data were collected between April 2019 and March 2020.
Results
Negative binomial regression analysis found an inverse relationship of role security with the proportion of screened patients. Self-efficacy was associated with an increase in the proportion of screened patients only amongst Mexican providers. Support from leadership (formal leader in organization) was the only significant organizational context factor, but only in non-control arms.
Conclusion
Higher self-efficacy is a relevant factor in settings where screening practice is already ongoing. Leadership support can enhance effects of implementation strategies.
Keywords
Background
Alcohol use is amongst the ten leading risk factors for mortality and morbidity,1,2 causing about three million deaths annually. 3 Alcohol consumption increases the risk of alcohol use disorders, 4 liver disease, 5 cancer, 6 tuberculosis, 7 depression, 8 non-ischemic cardiovascular disease, 9 and heavy drinking occasions (drinking 60+ grams of pure alcohol on one occasion) increase the risk of ischemic cardiovascular disease. 10 In Latin America, alcohol is the fourth leading risk factor for morbidity, 11 necessitating the implementation of effective interventions to reduce consumption. Primary health care (PHC) providers play an important role in reducing consumption, as they can detect heavy drinkers through their regular contact with the general population, and because of their opportunity to establish long term, positive therapeutic relationships with patients. Screening for unhealthy alcohol use with a validated instrument (such as AUDIT 12 ) during the consultation, and providing patients with brief advice or motivational interviewing-based intervention for hazardous or harmful alcohol use, has a large and robust evidence base for effectiveness in PHC.13,14 Despite this evidence, screening and brief intervention are often not optimally implemented in routine practice, 15 and providers often cite lack of time, resources and training as barriers to implementation. 16
Previous studies have sought to identify implementation strategies that could help to address those barriers and increase rates of alcohol screening in PHC, such as training, municipal support and financial reimbursement.17,18 Building on existing evidence, the SCALA study seeks to test whether training and municipal support could scale-up PHC-based screening, intervention and treatment for heavy drinking and comorbid depression in three upper-middle income Latin American countries: Colombia, Mexico, and Peru. 19 The results of the SCALA outcome evaluation at the primary health care center (PHCC) level suggest that the training of providers significantly increased the proportion of adult patients screened with AUDIT-C, whilst municipal support did not increase the screening rates. 20 The latter might have been impacted by the need for an early pause of implementation due to the COVID-19 pandemic in Latin America. Here, we report the findings of process evaluation that aims to identify which baseline contextual (non-intervention) factors were associated with providers’ alcohol screening practice. In this paper, we focus on individual motivational and organizational context factors, listed and defined in Table 1.
Scale definitions.

Definition from Gorman & Cartwright. 21
Definition adapted to the field of alcohol screening from Bandura. 21
Definition adapted to the field of alcohol screening from Bergström et al. 23
There is general theoretical support for the influence of the motivational factors on behavior. 24 Negative provider attitudes and low self-efficacy are commonly identified as barriers to undertaking alcohol screening in practice.25,26 Previous studies of attitudes, such as role security and therapeutic commitment to working with drinkers, reveal mixed findings, including positive associations27,28 but also no relationship.29,30 Self-efficacy has previously been found to be related to providers’ alcohol screening behavior. 31 Organizational context, including factors such as organizational support, resources, leadership, social relations and support, and organizational culture are also considered important implementation determinants.32–34 There is limited research on the influence of organizational context on PHC providers’ alcohol screening behavior, although factors such as lack of organizational support and supportive organizational culture are often cited as barriers in qualitative studies,25,26 including within Latin American settings. 35 In our study, we focused on five organizational contextual factors: leadership, work culture, resources, monitoring and community engagement.
Beyond assessing the relationship between baseline contextual factors and alcohol screening behavior, we recognize that their effect might be intervention dependent, that is only relevant for providers who receive certain implementation strategies, such as training on how to conduct screening, or activities at municipal level aimed at normalizing screening practice; or country dependent—differing between the three participating countries. The purpose of this study is thus to describe and compare the baseline motivational (attitudes, self-efficacy) and organizational context factors among the PHC providers in Colombia, Mexico and Peru, and explore if any of them are associated with the proportion of screened patients. Further, we investigate whether their effects differ based on study arm or country.
Methodology
Design
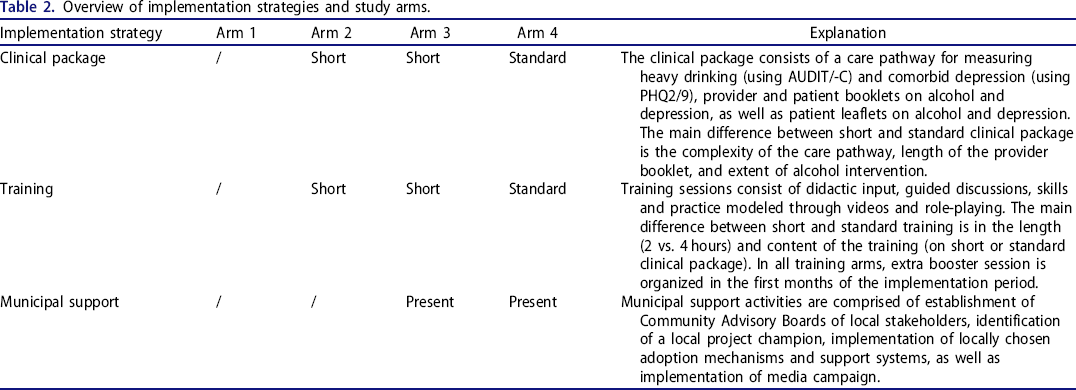
For the current study, we combined baseline provider questionnaire data with outcome data on provider screening behavior during the five-month study period. The longitudinal study was conducted as part of larger quasi-experimental trial (SCALA study), analyzing effects of different implementation strategies (clinical package, training and municipal support) on the screening for hazardous or harmful alcohol consumption and comorbid depression in 58 PHCCs based in Colombia, Mexico, and Peru (details available in full study protocol, 36 with short summary of study arms presented in Table 2).
Overview of implementation strategies and study arms.
Participants
Local researchers recruited PHCCs located in the selected intervention and control municipalities. Recruitment strategies within the PHCC varied by country. In Colombia, PHCC enrollment automatically included all providers in the study unless they opted out. In Peru, providers from participating PHCCs were asked to volunteer to participate. In Mexico, providers were in most cases selected and encouraged to enroll by their superior, but were free to decline. Any provider working with patients in a recruited PHCC was eligible to participate in the SCALA study upon signature of an informed consent form. To be included in analysis for this paper, providers had to complete the questionnaire during the baseline period and have available outcome data in at least one of the five months of the implementation period.
Data collection
The data were collected between April 2019 and March 2020. During a one-month baseline period (taking place between April and August 2019, depending on the PHCC), providers completed a 20-min baseline questionnaire and documented their regular screening activity by completing tally sheets for each time they screened patients using AUDIT-C. During the five-month implementation period (starting September–November 2019 and ending January–March 2020), providers returned completed tally sheets and provided information on the number of adult patient consultations. All data were collected in Spanish language and in paper format. Local research teams that visited the centers on a monthly basis collected the tally sheets and transferred data to the data management center in electronic format using secure encryption protocols.
Measurements
Predictors
Role security and therapeutic commitment were measured by the 10‐item Short Alcohol and Alcohol Problems Perception Questionnaire (SAAPPQ) on a 7‐point Likert scale. (1 = Strongly disagree to 7 = Strongly agree), with 4 considered a neutral score on both scales,21,37 Reliability of the scales, using Cronbach's alpha, was 0.67 for role security (four items) and 0.69 for therapeutic commitment (six items). Self-efficacy was measured with five items specifically developed for this study on a 5-point Likert scale ranging from 1 = Very difficult to 5 = Very easy (α = 0.76). Organizational context was assessed using an adapted version of the Context Assessment for Community Health (COACH) tool, 23 developed specifically for use in low and middle-income countries. Whilst the original validated tool measures the overall organizational context in the PHCC using eight dimensions (Organizational resources, Community engagement, Monitoring services for action, Sources of knowledge, Commitment to work, Work culture, Leadership, Informal payment), we selected ten items considered most relevant to assess the organizational context in our study, and slightly adapted the selected questions to reflect organizational context related to alcohol prevention activities. Dimensions of Leadership (α = 0.85), Work Culture (α = 0.73), Resources (α = 0.93), Monitoring (α = 0.77) and Community engagement (α = 0.69) were thus assessed. Each scale consisted of two questions with answers on a 5-point Likert scale (1 = Completely disagree to 5 = Completely agree).
For role security and therapeutic commitment, the negatively worded items were reverse coded. 37 For all scales, any missing values on items were assigned the mean value of the remaining items of the scale for that participant (5.7% participants had a missing value on one item and 0.5% on two items). The scores for all items of the scale were then summed up and divided by the number of items to obtain the participant's score. The complete list of used items is available in Supplementary Table A.
Outcome variable
Proportion of consulting patients who were screened with AUDIT-C by the health care professional (alcohol screening proportion): During the 5-month implementation period, providers were asked to screen all adult patients who consulted for any reason, using AUDIT-C. 12 For each provider, the proportion was calculated as the total number of completed tally sheets (representing cases of screening), divided by the total number of adult consultations with the provider during the 5-month implementation period, multiplied by 100, and rounded to the nearest integer.
Covariates
Baseline proportion of consulting patients who were screened with AUDIT-C by the health care professional was calculated in the same manner as described above, but only for the screening done during the one-month baseline period. Arm indicates the combination of implementation strategies received by the provider, as described in Table 2 (1 = Arm 1, 2 = Arm 2, 3 = Arm 3, 4 = Arm 4). For demographics, provider data was collected on age, gender (1 = female, 2 = male), country (1 = Colombia, 2 = Mexico, 3 = Peru) and professional role (1 = doctor, 2 = nurse, 3 = psychologist, 4 = other staff (e.g. social worker, midwife, nurse technician)).
Data analysis
First, the reliability of the scales and sample characteristics were calculated, and we compared the study sample with the rest of providers participating in SCALA who did not meet the eligibility criteria described in the Participants section. Second, descriptive statistics (mean (M), standard deviation (SD), percent (%)) and simple Pearson correlations for the main predictor variables were calculated. The Kolmogorov-Smirnov test found a non-normal distribution for the predictor variables. Thus, comparisons by country and arm were made with the non-parametric Kruskal Wallis H test, with post-hoc analyses adjusted for multiple testing with the Bonferroni correction.
Next, the distribution of the outcome variable was checked, and found to be best described by a negative binomial distribution (Supplementary material Figure 1), which is a discrete probability distribution with lower bound at 0, and variance much larger than mean, suggesting the presence of overdispersion. 38 To avoid losing information by dichotomizing the data or using non-parametric tests, a generalized linear model (GLM) for a negative binomial distribution with a log link function was chosen for data analysis. Due to the data structure (providers nested in PHCCs and PHCCs within country), generalized linear mixed models were initially used to test for the inclusion of random effects. Models with country as a fixed effect and a random intercept varying at the PHCC level indicated redundancy of the variances of the random effect, with a better fit of the model without the random effects. Thus a GLM was used.
Overall, we estimated six models: Model 1 included only covariates; Model 2 added the predictors; Model 3 included predictors’ interactions with country and with arm; and, Model 4 removed all non-significant interactions and non-significant main effects, provided they were not part of significant interactions (all where p ≥ 0.05). We repeated this process in Models 5 and 6 until only significant main effects and non-significant main effects with significant interaction remained in the model. The likelihood ratio chi square test was used to assess improvement in model fit between the models, with the value calculated by the formula LR = 2*(lnL1–lnL2). In the results section, only the final model is presented with incident rate ratios (IRR) and the corresponding 95% confidence intervals (CI). The results of the other models are available in the Supplementary material Table 2 and Table 3.
All analyses were conducted in IBM SPSS 26. In statistical testing, a significance level of 5% was used.
Ethics
The Ethics Committee of the Technical University of Dresden gave final ethical approval for the project on 12 April 2019, EK90032018. In addition, the appropriate ethics boards in Colombia, Mexico, and Peru have approved the study. All participating PHC providers have signed an informed consent form for participation.
Results
Characteristics of the sample
In total, 386 providers (62.1% of all participating in SCALA) were included in the sample (Table 3). Remaining providers were excluded due to: 192 (30.9%) not completing the baseline questionnaire; 12 (1.9%) missing questionnaire data; and 32 (5.1%) missing outcome data on screenings during the implementation phase. Comparison with the excluded providers found that those eligible for inclusion differed in country distribution (a smaller proportion of Mexican respondents among the included providers) (χ2 = 47.91, p < 0.001), arm distribution (a larger proportion of participants in arm 1) (χ2 = 38.86, p < 0.001) and gender distribution (a larger proportion of females) (χ2 = 8.42, p = 0.004). There was no difference in age (t = −1.48, p = 0.139) or professional role (χ2 = 6.58, p = 0.089).
Sample characteristics description, overall and by country.
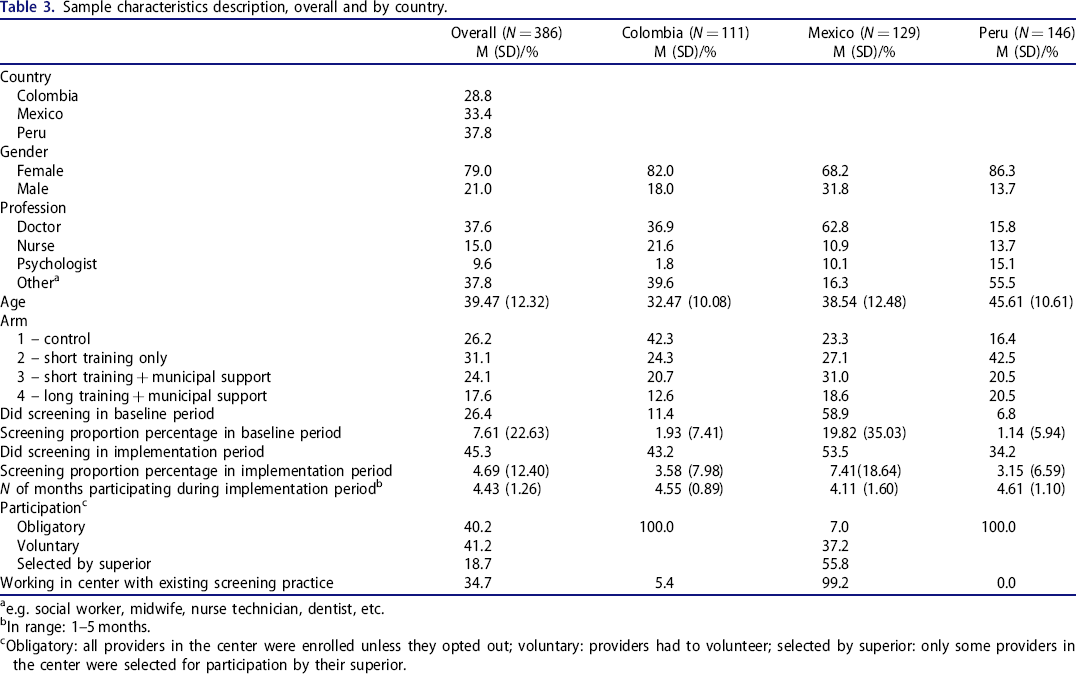
e.g. social worker, midwife, nurse technician, dentist, etc.
In range: 1–5 months.
Obligatory: all providers in the center were enrolled unless they opted out; voluntary: providers had to volunteer; selected by superior: only some providers in the center were selected for participation by their superior.
Country and arm comparisons of predictor variables
There were significant differences between countries for all the predictors (Table 4). In most predictors, Mexican providers had the highest mean scores, with the exception of therapeutic commitment and work culture, where the Peruvian providers scored highest. Comparison of predictor variables was made also by arm, and no differences were found in all predictors except for therapeutic commitment, with post-hoc testing showing that providers from Arm 1 had significantly lower therapeutic commitment than providers from Arm 4 (M(SD)Arm1 = 4.58(0.86), M(SD)Arm4 = 5.08(0.72); p < 0.001). Simple Pearson correlations between scales’ constructs are available in Supplementary material Table 1.
Comparison of motivational and organizational predictors by country.
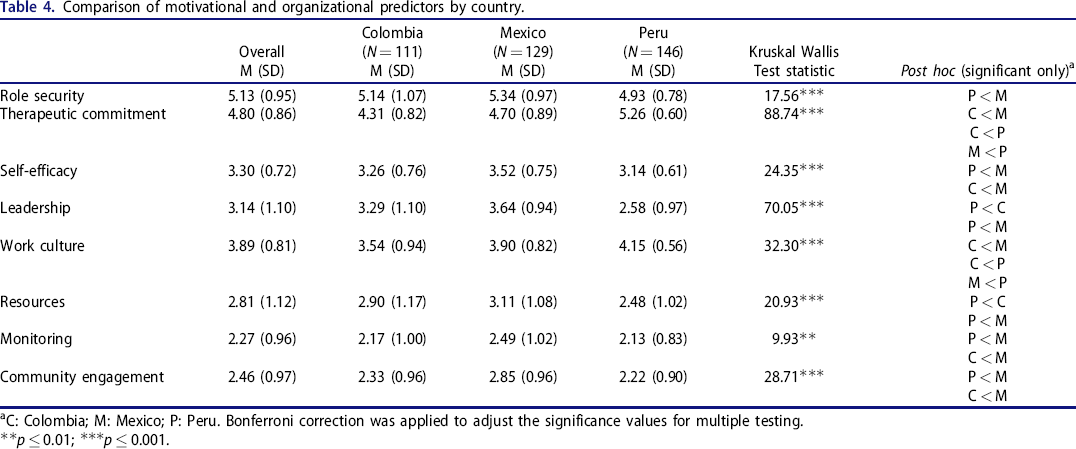
C: Colombia; M: Mexico; P: Peru. Bonferroni correction was applied to adjust the significance values for multiple testing.
p ≤ 0.01;
p ≤ 0.001.
Predictors of alcohol screening
Next, we examined the fit of the tested models to predict the alcohol screening proportion. Table 5 presents the log likelihood values for all models, and the calculated likelihood ratio chi square values for selected models’ comparisons. Only Models 4, 5 and 6 significantly improved the fit compared to Model 1. Those three models were then compared to each other, and the larger models (4 and 5) did not have a significantly better fit than Model 6. Model 6 was thus selected as the final best fitting model. Full results for all the models are available in Tables 2 and 3 of the Supplementary material.
Model specification and fit comparison.
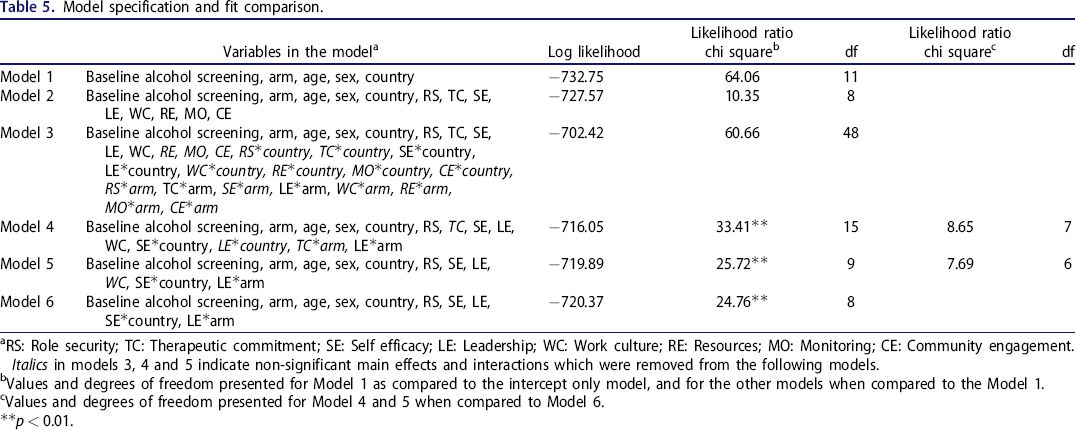
RS: Role security; TC: Therapeutic commitment; SE: Self efficacy; LE: Leadership; WC: Work culture; RE: Resources; MO: Monitoring; CE: Community engagement. Italics in models 3, 4 and 5 indicate non-significant main effects and interactions which were removed from the following models.
Values and degrees of freedom presented for Model 1 as compared to the intercept only model, and for the other models when compared to the Model 1.
Values and degrees of freedom presented for Model 4 and 5 when compared to Model 6.
p < 0.01.
Table 6 displays the results of the negative binomial regression of the selected Model 6, including role security, self-efficacy and its interaction with country, and leadership and its interaction with arm. Effects of therapeutic commitment, work culture, resources, monitoring and community engagement or their interactions with country and arm were not large enough to be included in the final model. Overall, female providers were more likely to screen a higher proportion of patients than male providers. Doctors were less likely to screen compared to psychologists, but more likely to screen compared to nurses and other professions.
Results of negative binomial regression for the final model.
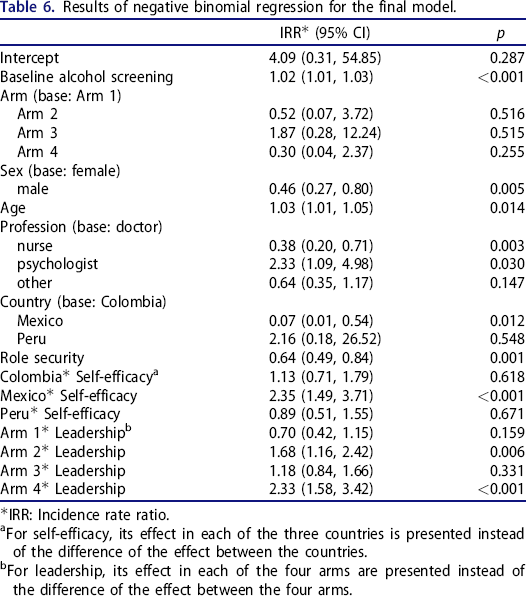
IRR: Incidence rate ratio.
For self-efficacy, its effect in each of the three countries is presented instead of the difference of the effect between the countries.
For leadership, its effect in each of the four arms are presented instead of the difference of the effect between the four arms.
Role security was the only predictor with a significant main effect. For every 1-point increase in the role security scale (with other variables held constant), the associated relative decrease in the proportion of alcohol screening was 36%. Effect of self-efficacy was only significant in Mexico; for each 1-point increase on self-efficacy scale, the associated relative increase in screening proportion was 135%. In the other two countries, self-efficacy was not significantly associated with the outcome. The leadership effect differed by arm: in arm 1 (control arm), a 1-point increase in the leadership scale was associated with a 30% decrease in the screening proportion (effect not significant), in the other three arms a 1-point increase in the leadership scale was associated with an increase in screening proportion: 68% in Arm 2; 18% in Arm 3 (effect not significant); and 133% in Arm 4. Other interactions that were significant in the largest model (Model 3) but not included in the final model (as presented in Supplementary material Table 2) were interaction between therapeutic commitment and arm (indicating that for providers from Arm 1, but not from other arms, an increase in therapeutic commitment was associated with an increased screening proportion) and interaction between leadership and country (indicating that increase in leadership support in Colombia and Mexico, but not in Peru, was associated with an increased screening proportion).
Discussion
This study investigated which motivational and organizational context factors were associated with alcohol screening behavior of PHC providers in Colombia, Mexico and Peru. We found that role security and leadership support were the only factors associated with alcohol screening proportion across the three countries, although the effect of leadership differed by arm, and was only significant in Arm 2 and 4. Self-efficacy was associated with alcohol screening proportion only in Mexico.
Initial country comparisons of predictor variables showed significant country differences on all eight studied predictors. Whilst one explanation for such findings could be that providers from the three countries had different survey response styles, we believe this interpretation is less likely to explain the country differences, as the responses did not differ consistently in the same direction: e.g. providers in Peru did not have lower ratings on all variables. An alternative and more plausible explanation entails that the country differences may reflect the different contexts in the countries and can be interpreted in the light of two factors that differed at country level: existing alcohol screening practice in the center, and manner of provider recruitment. Mexico was the only country in which alcohol screening was already embedded within routine practice, as official standards require PHC providers to ask their patients about alcohol consumption and include this information in their clinical history.39,40 This could explain the higher baseline alcohol screening proportion, and the highest mean role security and mean self-efficacy found in Mexico. In contrast, Peru's scores might reflect the fact that only motivated providers with high therapeutic commitment joined the study, but that they felt less experienced in alcohol preventative work, as they also had the lowest role security and self-efficacy scores.
Our study revealed that an increase in role security was related to decreased alcohol screening proportion, which differs from results of previous European studies.27,28,41 An explanation for this could be that on average, our sample had high levels of existing role security (around 5 on 7-point scale, similar to scores reported in Bendtsen et al. 29 and higher than reported in Anderson et al. 28 ) and therefore further increase in role security did not contribute to higher alcohol screening proportion. Higher self-efficacy appeared to be the most important predictor of practice, but only in Mexico. This could be due to existing official standards; many of the providers had previous experience with alcohol screening practice, and they could base their self-efficacy ratings on their actual experiences. Domain-specific self-efficacy has previously been found to be an important predictor of health professionals’ behaviour. 31
Leadership appeared to be the only important organizational context factor and was associated with increased alcohol screening rates in the three non-control arms. From the PHC providers’ perspective, the main difference between arm 1 and arms 2–4 was that they had a chance to participate in the training. Municipal support, the other implementation strategy, was directed toward a supportive environment (at PHCC and municipal level), and also not fully implemented due to COVID-19 pandemic. This suggests training as a possible key factor that made a difference in the effect of leadership. With our definition of leadership as supportive actions from the formal leader in the organization, this means that more support from the PHCC manager was associated with an increase in the proportion of screened patients, but only when the providers also received training. This confirms the postulated relevance of leadership in the implementation frameworks.32–34 A question remains as to why the effect of leadership was smaller (and non-significant) in arm 3. This will be explored through further qualitative phases of the process evaluation.
Strengths and limitations of the study
This study incorporated a range of contextual factors, which have been postulated to be important influencers of provider behavior in theory and practice in other fields, but less researched in the field of alcohol screening. The main strength of the study is that the outcome variable was actual behavior based on documentary information provided by PHCCs as opposed to self-report measures (e.g. recall-based questionnaires), resulting in high ecological validity. While there exist more objective methods to gather outcome data (e.g. observation), we consider documenting screening with tally sheets a suitable solution to achieve good balance between objectivity and feasibility (especially in the resource-limited context), used also in previous similar international studies.27,36 However, it should be noted that in the baseline period, the providers received the tally sheets from the researchers and were asked to document their activity, which, in itself, could be considered an intervention. Using more objective measures might result in lower baseline screening rates. Furthermore, we designed the study to anticipate contextual variability (as the providers were coming from different countries and embedded in different organizational settings). At the same time, this lack of uniformity between countries could also be seen as a disadvantage of the study design. Providers with previous experience with alcohol screening came predominantly from one country (Mexico) and presumably responded to the questions according to their actual experience; whereas for the rest of the sample without previous experience in alcohol screening, it is more likely that they responded to the questions according to their anticipated behavior. We sought to mitigate the impact of this potential limitation by including the country interactions in our analysis model, and by interpreting the results in the light of information of the country context. Finally, despite including a relatively large number of covariates, we might have missed other important baseline factors that contributed to the outcome.
Implications for practice
The findings of our study have a number of practical implications. First, increasing providers’ self-efficacy seems important in increasing the proportion of screened patients. This could be achieved through theory-based training that incorporates evidence-based methods shown to increase self-efficacy, such as guided practice, enactive mastery experiences or modelling.22,42 Second, the interaction of leadership support with the intervention arms found in our study points to the necessity of ongoing sensitization of PHCC leadership to the importance of preventive screening – their approval and support can enhance the results of the implementation efforts. Third, the highest baseline and implementation period screening rates in Mexico can be partially attributed to existing policy at the national level, described above. This implies that if the public health goal is to maximize the number of screened patients, directing efforts at introducing such policies might ultimately be more effective than implementation strategies focused only on providers (however, the time horizon needed to negotiate and achieve the implementation of such policies would likely exceed the usual length of research projects, making them less feasible). More feasible might be focusing efforts on introducing such policies at the PHCC level. Overall, the country differences in the studied factors and their relationship with the outcomes point to the importance of considering broader cultural and policy contexts in which the providers are embedded when trying to understand factors that influence screening practice, and tailoring the implementation strategies to the needs of the setting.
Conclusion
This study investigated factors affecting alcohol screening behavior amongst primary health care providers in Colombia, Mexico and Peru and their interaction with tested implementation strategies, as well as the setting of the study. Attitudes such as role security and therapeutic commitment were not prerequisites for alcohol screening behavior, with an increase in role security actually decreasing the proportion of alcohol screening undertaken. Higher self-efficacy appeared to be an important factor in an environment with existing alcohol screening practice. Leadership support was the only significant organizational context factor that also seemed to be important across all countries, but only in arms where providers received training.
Footnotes
Disclosure statement
No potential conflict of interest was reported by the author(s).
Author contributions
DK, EJL, LM, HDV and PA, drafted the first version of the paper, DK analyzed the data and revised the paper based on coauthors’ feedback and comments. EJL, LM, HDV, PA, AOD, BS, CSS, TG, EK, APG, JMT, GNR, PM, MP and IB contributed to the Grant Application for SCALA study, and provided feedback on design and material development for this study. APG, JMT, GNR, PM, MP and IB implemented the study at country level and collected the data. MJJMC supported the data analysis. All coauthors commented on subsequent drafts of the manuscript, read and approved the final version.
Funding
The research leading to these results or outcomes has received funding from the European Horizon 2020 Programme for research, technological development and demonstration under Grant Agreement no. 778048 – Scale-up of Prevention and Management of Alcohol Use Disorders and Comorbid Depression in Latin America (SCALA). Participant organizations in SCALA can be seen at: ![]() . The views expressed here reflect those of the authors only and the European Union is not liable for any use that may be made of the information contained therein.
. The views expressed here reflect those of the authors only and the European Union is not liable for any use that may be made of the information contained therein.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
