Abstract
Keywords
Social phobia (fear and avoidance of being the centre of attention in case of embarrassment or shame) is a disorder that does not come to the attention of doctors even though it begins in adolescence and is very often chronic. In the Australian Burden of Disease study social phobia was associated with a similar burden to that of schizophrenia (approx. 18 000 disability adjusted life years lost) but only one in five people with the disorder sought treatment, and only 8% of the burden was averted by current treatment [1, 2]. Thus maximizing access to effective treatment is important. There is strong evidence for cognitive behavioural therapy in the treatment of social phobia [3]. Recent studies indicate that clinician-assisted computerized cognitive behavioural therapy that requires little therapist time can significantly reduce social phobia in the short and long term [4–7]. The improvement is equivalent to that obtained by face-to-face treatment. The importance of Internet therapies to people with social phobia is obvious. The present pragmatic randomized controlled trial (RCT) is part of a programme to explore the potential of computerized cognitive behaviour therapy (CCBT) in social phobia with decreasing amounts of clinician time [4–6, 8]. In the present study we used no clinician time but, guided by the literature [9], used an enhanced self-guided programme that included frequent email and short messaging service (SMS) reminders and compared this to a group who, in addition, received short weekly telephone calls from a research assistant.
Method
Participants
Applicants applied online to www.climateclinic.tv (now www.virtualclinic.org.au). Details of participant flow are in Figure 1. During the 6 weeks of recruitment, 420 individuals applied for one of the three treatment programmes and 193 met criteria for the social phobia programme. The inclusion criteria are those used in a previous trial [6] except that the Patient Health Questionnaire 9 (PHQ-9) [10] threshold for comorbid depression was raised to 22. A total of 183 individuals were able to be contacted and were given the social phobia section of the Mini International Neuropsychiatric Interview Version 5.0.0 [11] during a telephone interview to determine whether they meet DSM-IV criteria [12] for social phobia. A total of 168 applicants met all inclusion criteria.
Shyness 4 study flow chart. CBT, cognitive behavioural therapy; CCBT, self-guided computerized cognitive behavioural therapy group; MINI, Mini International Neuropsychiatric Interview; PHQ-9, Patient Health Questionnaire–Nine Item.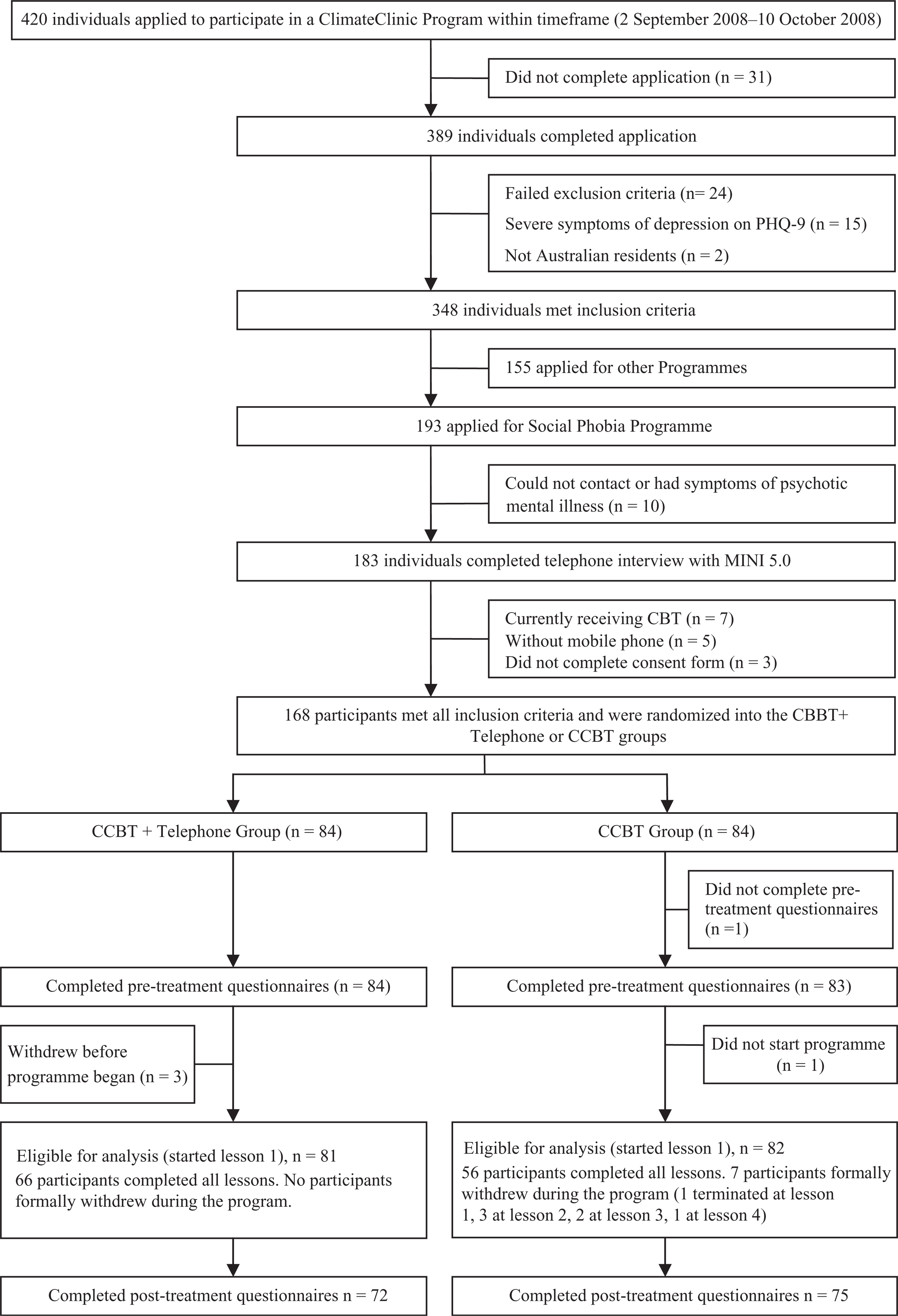
Interventions
Both groups received identical treatments delivered by computer: six online lessons; a summary/homework assignment for each lesson; comments by prior participants about each lesson; access to the supplementary materials; automatic emails and fortnightly SMS messages. Part of the content of each lesson was presented in the form of an illustrated story about a young man with social phobia who, with the help of a clinical psychologist, successfully gains mastery over his symptoms. Lessons 1 and 2 provided education about the symptoms and treatment of social phobia, lesson 3 provided instructions on how to develop an exposure hierarchy and about practising graded exposure, lessons 4 and 5 reinforced principles of graded exposure and demonstrated principles of cognitive restructuring, while lesson 6 included information about relapse prevention. Participants were encouraged to complete the first four lessons within the first 2 weeks, in order to provide more opportunity to practise the graded exposure, cognitive skills and other coping techniques in subsequent weeks. All participants were asked to complete the six lessons within 8 weeks of starting. In addition telephone group participants (CCBT + Tel) were telephoned each week by a research assistant, at a time specified by the participant, when they were commended and encouraged to persevere but no clinical advice was offered.
The modifications to enhance the existing content and user interface of the self-guided programme used in the previous RCT [6] were considerable. In that study the completion rate of the CCBT group who had no clinician contact was only 33%, but these participants attained a mean within-group effect size (ES) of 0.66, indicating potential if the self-guided programme was enhanced. The changes were as follows: (i) text, including instructions, directions, and explanations, were simplified; (ii) additional graphic images were included to represent important concepts; (iii) supplementary materials were added about conversation skills, assertiveness, public speaking, and managing mood; (iv) eight video clips were added introducing parts of the programme; (v) with consent, forum comments (n = 30) by participants in previous trials [4–6] on homework assignments and progress were inserted at appropriate stages of the programme (to increase relevance, these comments were displayed for each lesson according to participant gender and age); and (vi) an algorithm defining 62 different possible email messages was developed and appropriate emails were sent at specific stages of the programme (the criteria for sending an email included a participant completing a lesson, not completing a lesson within a specified time frame, or to alert participants to additional material that had been made available in relation to a specific lesson or issue).
Hypothesis
The hypothesis was that adherence and progress in the telephone group who had some human contact would be superior to the self-help group without human contact.
Outcomes
Applicants completed the Social Interaction Anxiety Scale (SIAS) [13]; the Social Phobia Scale (SPS) [13]; the PHQ-9 [10]; the Kessler 10 (K-10) [14]; and the Sheehan Disability Scales (SDS) [15]. Applicants completed a demographic questionnaire and the Credibility/Expectancy Questionnaire (CEQ) [16] to explore whether expectancies or perception of treatment credibility are related to outcomes. Changes in the SIAS and SPS were considered the primary social phobia outcome measures, changes in the PHQ-9, K-10, and SDS were the secondary outcome measures, changes in the CEQ were a process measure. After treatment, participants completed the aforementioned questionnaires and a seven-item treatment satisfaction questionnaire based on the Credibility/Expectancy Questionnaire [16, 17]. Results are reported for the end of treatment because follow up of Internet CBT has not resulted in reports of deterioration.
Sample size
Power calculations based on a between-group ES of 0.4, with power of 80%, and alpha of 0.05 indicated that a total sample size of 156 participants was required [18]. A total of 168 were recruited.
Randomization
Primary and secondary outcome measures: intention to treat
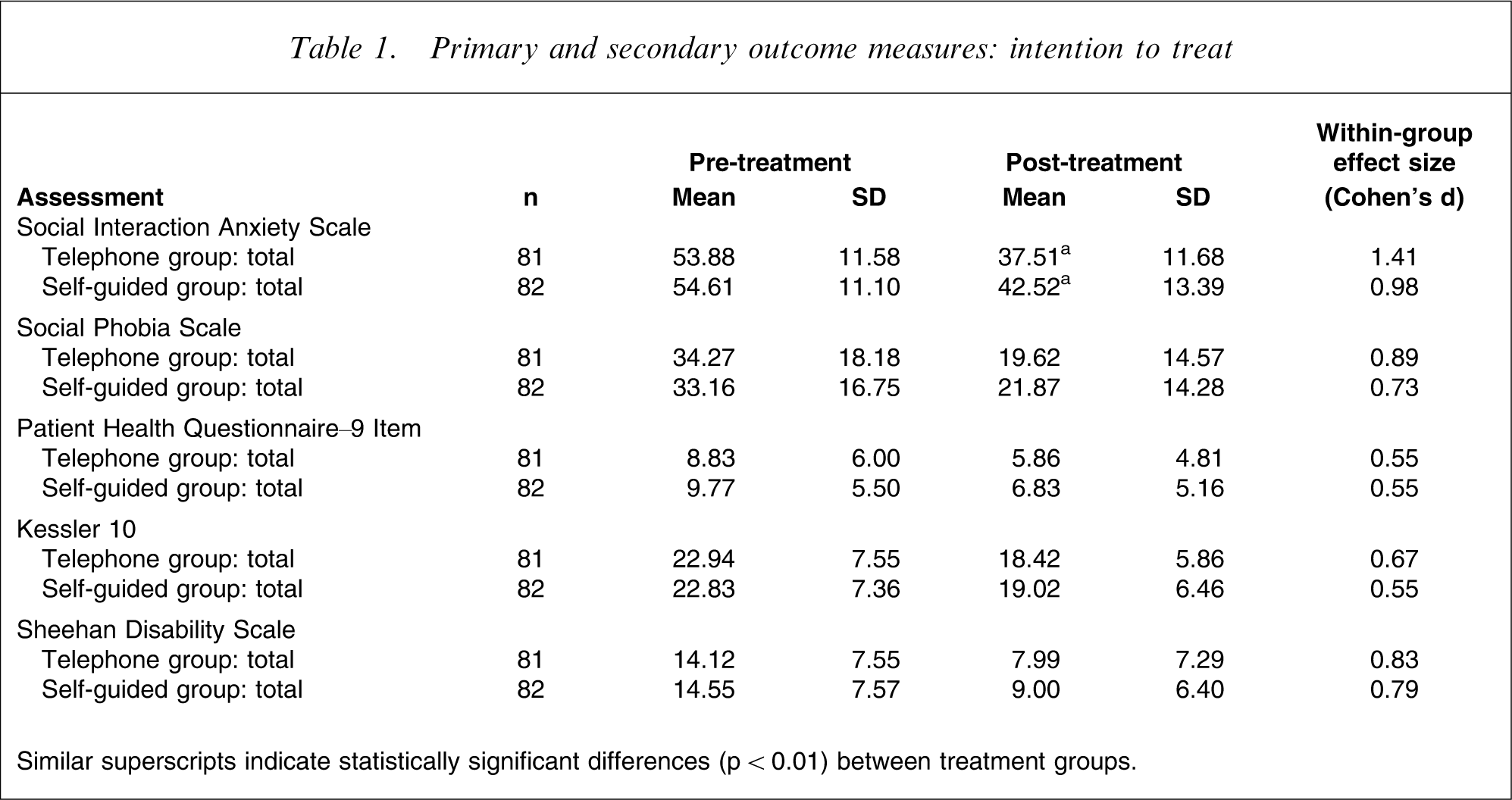
Similar superscripts indicate statistically significant differences (p < 0.01) between treatment groups.
Statistical methods
Group differences in demographic data, pre-treatment measures, and pre-treatment expectations were analysed on one-way ANOVAs and χ2 tests. Two factor scores (credibility and expectancy) were derived from the CEQ as described [16]. Change scores for each outcome measure were calculated and Pearson product moment correlations (using Bonferroni corrected p) were subsequently calculated between these and the two CEQ factor scores to explore variables that may affect outcomes.
All post-treatment analyses involve an intention-to-treat design, unless otherwise specified. Pre–post-treatment changes in participant questionnaire scores were analysed using univariate analyses of covariance (ANCOVAs), followed by t-tests with Bonferroni corrected p as recommended [19, 20]. The ESs (Cohen's d) were calculated for within-group changes, based on the pooled standard deviation. Participants were then divided into completers and non-completers and ANOVAs and χ2 analyses were conducted on pre-treatment variables to determine characteristics predicting completion.
The study was approved by the Human Research Ethics Committee (HREC) of St Vincent's Hospital (Sydney, Australia) and the HREC of the University of New South Wales (Sydney, Australia). This trial was registered as ACTRN12608000465358. It is reported as a pragmatic RCT [21] based on the premise that the results inform service decisions about implementation of treatment programmes for social phobia.
Results
Participant flow
The flow is shown in Figure 1. Recruitment occurred between September 2008 and October 2008. Three CCBT + Tel and two CCBT group participants withdrew before beginning treatment, resulting in 81 CCBT + Tel and 82 CCBT group participants. Sixty-six (81%) CCBT + Tel group and 56 (68%) CCBT group participants completed all six lessons within the required time frame (p < 0.05). Consistent with this, CCBT + Tel group participants completed more (mean = 5.68, SD = 0.79) of the six lessons than participants in the CCBT group (mean = 5.26, SD = 1.35; F1,161=5.95, p < 0.02).
Baseline data
The mean age of participants was 41.2 years and 48% were men. A total of 47% of participants reported having talked to a health professional about their symptoms of social phobia, and 22% reported taking medication for mood and/or anxiety. A total of 32% of participants reported using the Internet more than 11 h per week, and 43% reported they were very confident using computers and the Internet. No between-group differences on pre-treatment measures or pre-treatment expectations (CEQ factor scores) were observed using one way ANOVAs (F1,161=0.01–1.54, p > 0.05).
Numbers analysed
Post-treatment data were collected from 72/81 (89%) CCBT + Tel group participants and 75/82 (91%) CCBT group participants. In accordance with the intention-to-treat paradigm, the pre-treatment scores of the 16 participants who did not complete the post-treatment questionnaires were replicated as their post-treatment scores.
Outcomes
A univariate ANCOVAS on post-treatment SIAS and SPS scores, controlling for pre-treatment scores (Table 1), showed that the CCBT + Tel group had significantly lower SIAS post-treatment scores than the CCBT group (p < 0.01), but that the difference was small (ES = 0.3). No between-group differences were found on the SPS. There were no significant differences between groups on the PHQ-9, K-10 or SDS, the secondary outcome measures. Pre-treatment expectancies did not systematically predict outcome. Treatment satisfaction was high, but not significantly higher in the CCBT + Tel group as compared to the CCBT group.
Participants were divided into completers (n = 122) and non-completers (n = 41). No pre-treatment differences were found between completers and non-completers using ANOVAs or χ2 statistics. Completers reported greater reductions in symptom severity on the SIAS (F1,145=9.26, p = 0.01), SPS (F1,145=8.01, p = 0.01), and K-10 (F1,145=5.14, p = 0.03) than non-completers. Predictably, non-completers rated their motivation, and their confidence that they could learn to manage their symptoms, as lower than completers (χ2=10.57, p = 0.02; χ2=20.95, p = 0.01).
Each participant in both groups received four SMS messages; these were sent in bulk to the 163 participants, and required approximately 5 min of staff time to send each set of messages. Each participant also received an average of 15 automated emails during the programme, including emails sent at the completion of each lesson, reminder emails, and emails providing information about additional resources. In addition, each participant in the CCBT + Tel group received 8 telephone calls. The calls used an average 38.7 min per participant of research assistant time.
Internet activity
No difference was found between the total number of times the CCBT + Tel (mean = 23) and CCBT (mean = 23) groups logged on to the program. Three-quarters of website visits for participants in each group were spent viewing the first three lessons, the remaining quarter on the second three lessons. There were no adverse events during the programme.
Discussion
Interpretation
Completion rates and progress (ESs) for both groups were good; certainly superior to the results in the previous trial when only 33% completed. We concluded that the enhancements to the content and functionality of the programme had been effective. The group with additional non-clinical telephone support had completion rates of 81%, and within-group ESs on the self-report scales, SIAS and SPS of 1.41 and 0.89, respectively (mean = 1.15). The outcomes for the group without telephone support were 68%, with ESs of 0.98, and 0.73, respectively (mean = 0.86). The outcomes achieved by the two groups were significantly different but both sets of results are good, similar to outcomes reported from good face-to-face treatment programmes for social phobia [22, 23]. The results are consistent with previous studies indicating that completion rates and clinical outcomes of Internet-based self-guided programmes can be enhanced by regular reminders or prompts [9, 24]. Treatment satisfaction remained high in both groups. The present findings indicate that people with social phobia may still make considerable progress even if no clinician is available. Such programmes are likely to be valuable.
This is the fourth RCT in a series exploring the utility of Internet treatment for social phobia. In the first two trials the version of the social phobia programme consists of six online lessons (see www.virtualclinic.org.au), cognitive behavioural homework assignments, regular email contact with a clinician, and participation in an online discussion forum. These two intervention versus waitlist control RCTs (n = 99, n = 81) both generated ESs of ≥1.0 with 2½ h of clinician contact time per participant [4, 5]. At 6 month follow up the results were sustained, and the programme was as acceptable to participants as face-to-face treatment [8].
The third RCT (n = 95), as noted, compared the clinician-assisted CCBT version of the programme with a self-guided (CCBT) version without clinical contact to determine whether participants could benefit in the absence of clinician guidance [6]. Adherence in self-guided CCBT programmes is usually low [25, 26]. In this RCT the results of the clinician-guided group were consistent with the earlier studies: a completion rate of 80%, and a mean ES versus waitlist >1.0. The completion rate of the CCBT group who had no clinical contact was 33%, but the participants who completed the programme attained a mean within-group ES of 0.66, indicating potential if a better self-guided programme could be developed.
Clinician-guided computerized cognitive behaviour therapy for many anxiety and depressive disorders has been shown to be comparable to the best face-to-face therapy [4–6, 8, 27–29]. The difficulty is that even though the requirement for clinician time is reduced by up to 80% compared to face-to-face therapy, the demand for therapist time precludes wide implementation in specialist or primary care. The aim of the present study was to examine the effect of an enhanced self-guided version of the social phobia Internet programme with and without a low level of non-clinical support. Both versions were satisfactory.
Limitations
This programme is unlikely to be as beneficial if placed on the web for anyone to use. Adherence to open programmes is very low. The present participants volunteered for treatment, were diagnosed as having social phobia, and enrolled in a defined treatment programme. The results are evidence that this programme, without further staff input, can be associated with substantial benefit. It is evidence that less than an hour of practice nurse or receptionist time for reminder phone calls is associated with improvement in adherence, clinical outcome and patient satisfaction. This improvement was not large and it is a pragmatic decision by a practice or service whether the investment of this extra time is justified.
Generalizability
This is the first evidence that people with social phobia can recover with Internet therapy without clinician input. The participants were typical of persons seeking help. The findings are a logical extension of a previous trial [6]. The number of participants was substantial but the findings require replication.
This study indicates that a self-guided version of the social phobia programme, enhanced with resources and regular reminders, can result in completion rates, clinical outcomes, and acceptability ratings comparable with much face-to-face treatment. The addition of weekly non-clinician contact via telephone produced significantly better adherence, benefit and satisfaction. Because both interventions are effective, it is a pragmatic decision for a practice or a service as to whether the increase in efficacy justifies the investment in 1 h of practice nurse or receptionist time. At 20 min of administration time per participant, both versions of the programme are clearly very cost-effective. These findings provide further evidence that Internet-based treatment programmes for the common mental disorders may considerably enhance existing mental health services. Providing that they are safe, effective, and acceptable to patients, clinicians, managers of mental health services, and funders, and they appear to be all these things, then they should be implemented within a stepped care model of service provision.
Footnotes
Acknowledgements
The authors gratefully acknowledge the participants for their involvement and helpful comments. We also wish to gratefully acknowledge the contributions to the development of the Climate Clinic programme by Mr Jason Hando, and Mr Daniel Winter.
