Abstract
Keywords
Generalized anxiety disorder (GAD) is a common anxiety disorder characterized by excessive and uncontrollable worry. The 12 month prevalence of GAD in Australia and New Zealand is 2.7% [1] and 2.0% [2], respectively. GAD often co-occurs with other Axis I disorders [3, 4] and is a chronic condition with fluctuating symptoms, but few sufferers ever experience a full remission of symptoms. GAD is also highly disabling, with data indicating that it is associated with levels of disability comparable to depression [5, 6]. People with GAD make considerable use of general health-care facilities [7, 8], visiting their doctor twice as frequently as patients with comparable chronic physical conditions and similar demographic characteristics [9].
GAD can be treated effectively with cognitive behavioural therapies (CBT) [10], particularly those that include components addressing the cognitive aspects of worry [11, 12]. GAD, however, is considered the least successfully treated anxiety disorder [13], and increasing the efficacy of existing interventions is an important priority.
This study is part of a research programme exploring the utility of computerized CBT (CCBT) in enhancing the capacity of existing mental health services to treat high-prevalence internalizing disorders such as anxiety and depression (see www.virtualclinic.org.au). CCBT programmes use a computer interface to present structured sessions of CBT either via the Internet or at a clinic, and may therefore reduce barriers to treatment [14, 15]. We have demonstrated the clinical efficacy of clinician-assisted or (CaCCBT) programmes in randomized controlled trials (RCTs) or open studies in patients with depression [16, 17], social phobia [18–25], and in a recent trial in patients with panic disorder [26]. These results are consistent with a growing body of Australian-based [27–29] and international [30–34] research indicating the clinical efficacy and effectiveness of Internet-based clinician-assisted CCBT (CaCCBT) in the effective treatment of anxiety and depression [35, 36].
Despite these encouraging results, to our knowledge only one open study of Internet-based treatment of GAD has been reported [37]. Although that study reported excellent resolution of clinically significant symptoms in three patients with GAD it is important to test the reliability of these findings using an RCT design, particularly because GAD is considered a difficult disorder to treat. The present study explores the efficacy of an Internet-based CaCCBT programme for GAD, the Worry programme, using a CONSORT-Revised compliant RCT design [38]. We hypothesized that treatment group participants would show significant improvement on measures of GAD, depression, and disability relative to controls; and that participants would rate the procedure as acceptable.
Method
Participants
Applicants applied online to www.virtualclinic.org.au, and the details of participant flow are shown in Figure 1. During the 4 weeks of recruitment, 67 individuals applied for this programme and 61 met inclusion criteria: (i) resident of Australia; (ii) at least 18 years of age; (iii) had access to a computer, the Internet, and use of a printer; (iv) not currently participating in CBT; (v) not using illicit drugs or consuming more than three standard drinks day−1; (vi) not currently experiencing a psychotic mental illness or severe symptoms of depression (defined as a total score >23 or responding >2 to Question 9 (suicidal ideation) on the Patient Health Questionnaire–9 Item (PHQ-9) [39]); and (vii) if taking medication, had been taking the same dose for at least 1 month and did not intend to change that dose during the course of the programme. Applicants who did not meet these criteria were informed via an onscreen message and email thanking them for their application, and encouraging them to discuss their symptoms with their physician. Participants who met the inclusion criteria then completed a 25-item questionnaire enquiring about demographic details and treatment history.
Generalized anxiety disorder study flow chart. CBT, cognitive behavioural therapy. MINI 5.0.0, Mini International Neuropsychiatric Interview; PHQ-9, Patient Health Questionnaire–9 Item.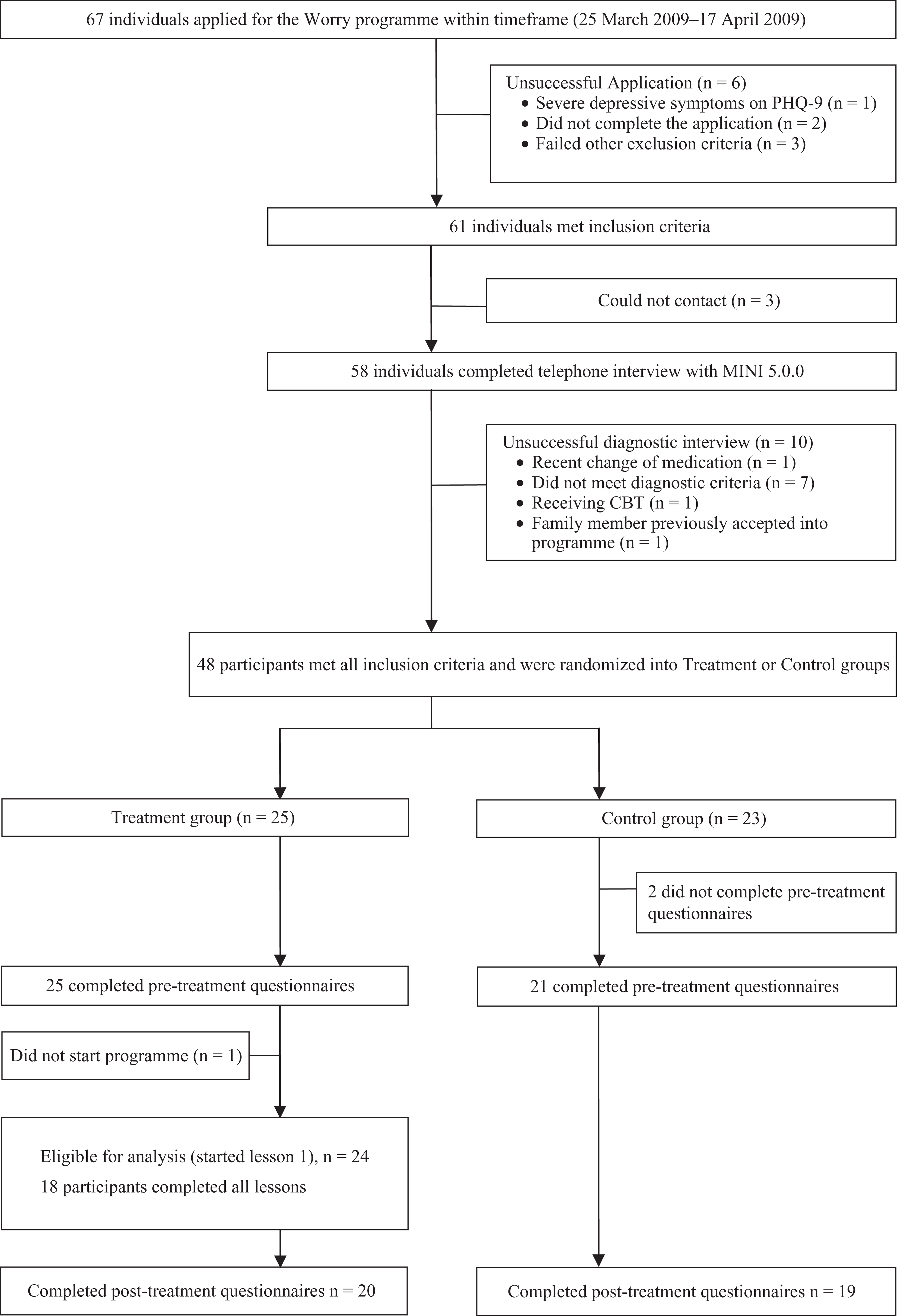
Fifty-eight individuals were contacted and were given the GAD section of the Mini International Neuropsychiatric Interview Version 5.0.0 [40] during a telephone interview to determine whether they met DSM-IV [41] criteria for GAD. A total of 48 applicants met all inclusion criteria and were randomly allocated to treatment (n = 25) or waitlist control (n = 23) groups. The unsuccessful applicants were advised about more appropriate treatment options. The study was approved by the Human Research Ethics Committee (HREC) of St Vincent's Hospital (Sydney, Australia) and the HREC of the University of New South Wales (Sydney, Australia), and the trial was registered as ACTRN12609000136202.
Intervention
The Worry programme consists of the following components: six online lessons; a summary/homework assignment for each lesson; an online discussion forum for each lesson; and instant messaging to allow secure email-type messages with a clinician. Participants also had access to additional written resources. These included guidelines about assertiveness, health anxiety, and answers to frequently asked questions about the application of specific skills described in the lessons and summaries. Part of the content of each lesson was presented in the form of an illustrated story about a woman with GAD who, with the help of a clinical psychologist, successfully begins to gain mastery over her symptoms. Lessons 1 and 2 provided education about the symptoms and treatment of GAD and the basic principles of cognitive therapy, lesson 3 provided instructions about challenging positive and negative beliefs about excessive worry, lesson 4 provided education and guidelines about practicing graded exposure, lessons 5 provided education and guidelines about challenging core beliefs, while lesson 6 included information about relapse prevention. Participants were encouraged to complete the first four lessons within the first 4 weeks, in order to provide more opportunity to practise the graded exposure, cognitive skills and other coping techniques in subsequent weeks. Participants were asked to complete the six lessons within 9 weeks.
Therapist
One clinical psychologist (ER) provided all clinical contact with participants. A research assistant provided administrative support to collate data. The clinician contacted all treatment group participants during the first week by telephone to introduce herself and to develop rapport. Every contact was recorded, as was the total therapist time spent per participant.
Hypotheses
Two hypotheses were tested. First, that treatment group participants would show significant improvement on measures of GAD, depression, and disability relative to controls; and second, that participants would rate the procedure as acceptable.
Outcome measures
Participants completed the GAD–7 Item Scale (GAD-7) [7, 42], the Penn State Worry Questionnaire (PSWQ) [43], the PHQ-9, the Kessler 10 (K-10) [44]; and the Sheehan Disability Scales (SDS) [45]. The PSWQ is a well recognized clinical measure of worry with excellent psychometric properties. The GAD-7 is a brief measure of the symptoms and severity of GAD based on the DSM-IV diagnostic criteria for GAD, but there are limited data on its response to treatment. A score of 10 on the GAD-7, however, has been identified as an important threshold for identifying DSM-IV-congruent GAD, with increasing scores indicating greater severity of GAD [42]. The PHQ-9 is also a brief measure based on the DSM-IV criteria for depression, while the K-10 and SDS are standard clinical tools with well-established psychometric profiles. All questionnaires were re-administered again 1 week after treatment, while the GAD-7 and PHQ-9 were also administered mid-treatment (at week 4).
Applicants also completed a demographic questionnaire and the Credibility/Expectancy Questionnaire (CEQ) [46] to explore whether expectancies or perception of treatment credibility are related to outcomes. Changes in the GAD-7 and PSWQ were considered the primary GAD outcome measures, changes in the PHQ-9, K-10, and SDS were the secondary outcome measures. At post-treatment assessment the participants completed the aforementioned questionnaires and a seven-item treatment satisfaction questionnaire based on the CEQ.
Randomization
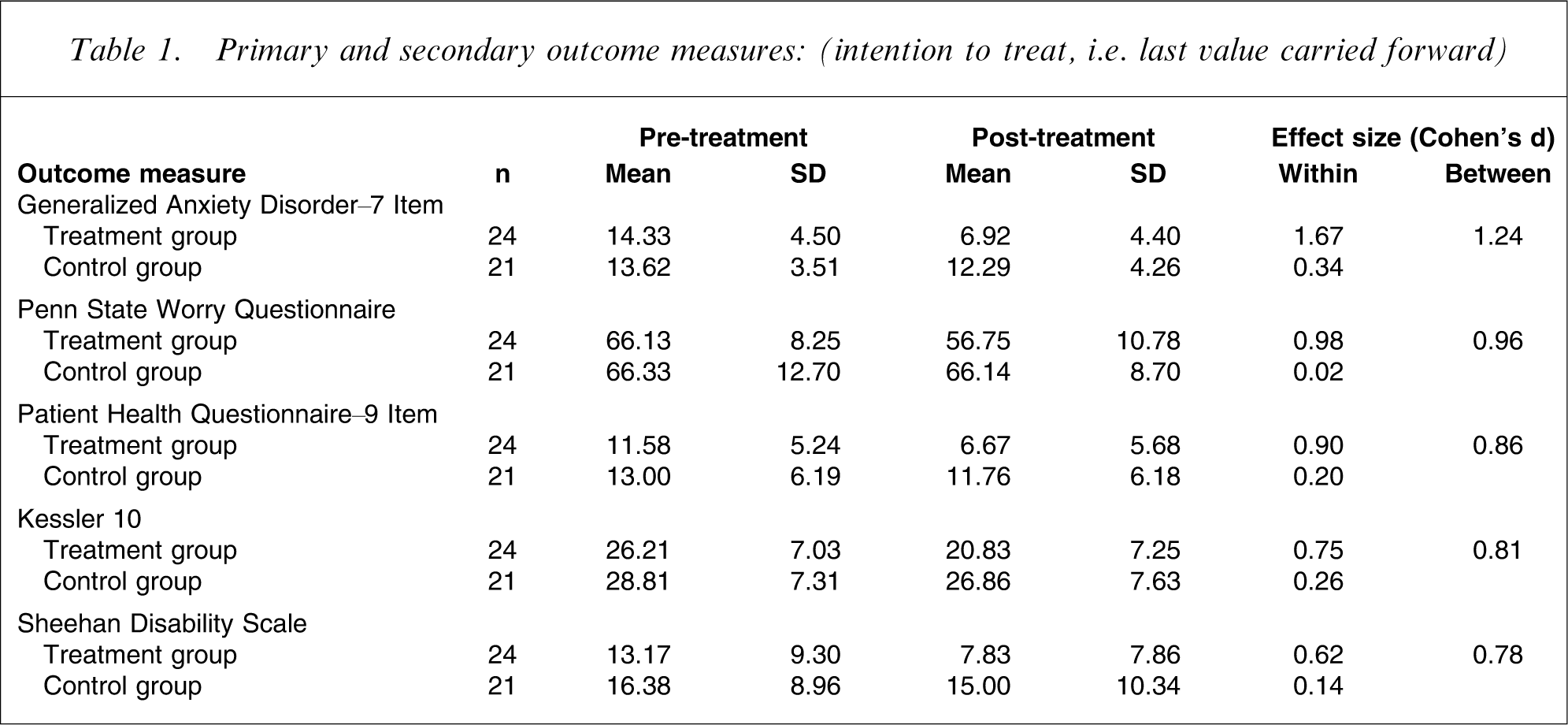
Primary and secondary outcome measures: (intention to treat, i.e. last value carried forward).
Statistical methods
Group differences in demographic data, pre-treatment measures, and pre-treatment expectations were analysed on one-way ANOVA and χ2 tests. Two factor scores (credibility and expectancy) were derived from the CEQ as described [46]. Change scores for each outcome measure were calculated and Pearson product moment correlations (using Bonferroni corrected p) were subsequently calculated between these and the two CEQ factor scores to explore variables that may affect outcomes.
All post-treatment analyses involved an intention-to-treat (ITT) design. Pre–post-treatment changes in participant questionnaire scores were analysed using univariate analyses of covariance (ANCOVAs) [47, 48]. Effect sizes (Cohen's d) were calculated for within- and between-group changes, based on the pooled standard deviation.
Results
Participant flow
The flow is shown in Figure 1. Recruitment occurred during March 2009 and April 2009. Two control group participants did not complete the pre-treatment questionnaires and one treatment group participant did not begin the Worry programme, resulting in 24 treatment and 21 control group participants. Eighteen (75%) treatment group participants completed all six lessons within the required time frame.
Baseline data
The mean age of participants was 44 years (SD = 12.98), 34 (76%) were women, 30 (67%) were married or in a de facto relationship, 34 (76%) had post-secondary education or training, and 18 (40%) were in full-time employment. Thirty-one (69%) reported having previously talked to a health professional about their symptoms of GAD, and 13 (29%) reported taking medication for mood and/or anxiety. Fifteen (33%) participants reported using the Internet more than 10 h per week (mean = 13 h, SD = 13.90), and 35 (78%) reported they were confident or very confident using computers and the Internet. No between-group differences on demographic characteristics, pre-treatment measures or pre-treatment expectations (CEQ factor scores) were observed on one-way ANOVAs (F1,43=0.00–1.48, p > 0.05) or χ2 tests (p > 0.05).
Numbers analysed
Post-treatment data were collected from 21/24 (88%) treatment group participants and 19/21 (90%) control group participants. In accordance with the ITT paradigm, the pre-treatment scores of the five participants who did not complete the post-treatment questionnaires were replicated as their post-treatment scores.
Primary outcome measures
Univariate ANCOVAs on post-treatment GAD-7 and PSWQ scores, controlling for pre-treatment scores (Table 1), showed that the treatment group had significantly lower post-treatment scores than the control group (F1,42=27.38, p < 0.001; F1,42=12.89, p < 0.001), respectively.
Secondary outcome measures
Univariate ANCOVAs were also conducted on the PHQ-9, K-10, and SDS post-treatment scores, while controlling for pre-treatment scores. These also indicated significant difference between treatment and control groups (F1,42=8.65, p < 0.01; F1,42=6.93, p < 0.01), and (F1,42=5.71, p < 0.02), respectively.
Effect sizes
Within- and between-group effect sizes for the outcome measures are included in Table 1. Large within-group effect sizes were found for the treatment group for the GAD-7 (1.67), PSWQ (0.98), PHQ-9 (0.90), and moderate within-group effect sizes for the K-10 (0.75), and SDS (0.62). Large–moderate between-group effect sizes were found for the GAD-7 (1.24), PSWQ (0.96), PHQ-9 (0.86), K-10 (0.81), and SDS (0.78).
Remission and recovery
At pre-treatment assessment a total of 20/24 (83%) of treatment group and 19/21 (90%) of control group participants had a GAD-7 score ≥10, congruent with a diagnosis of GAD. At post-treatment assessment (using the ITT design), 5/24 (21%) of treatment group participants and 18/21 (86%) of control group participants continued to have a GAD-7 score >10. With respect to recovery (i.e. reductions >50% of pre-treatment GAD-7 scores), 63% of treatment group participants and 10% of controls met this criterion at post-treatment assessment.
Pre-treatment expectancies and treatment satisfaction
Pre-treatment expectancies, as measured on the expectancy factors from the CEQ, were not significantly correlated with any of the outcome measure change scores. Treatment group participants who completed the post-treatment satisfaction questionnaires reported an acceptable level of satisfaction with the overall programme, with 17/20 (85%) reporting being either very satisfied or mostly satisfied, and 3/20 (15%) neutral/somewhat satisfied. Most responding participants (95%) rated the quality of the treatment modules as excellent or good; 85% rated the quality of Internet correspondence with the therapist as excellent or good, while 15% rated it as satisfactory.
When asked to provide a rating from 1 to 10, where 10 indicates a high level of agreement, the average participant rated the treatment as logical (9/10); they reported feeling confident that the treatment would be successful at teaching them techniques for managing their symptoms (8/10); and they reported a high level of confidence in recommending this treatment to a friend with GAD (9/10).
Time/contact events spent per participant
The mean total therapist time per treatment group participant was 130 min including monitoring of the discussion forum, instant messages, and telephone calls. An additional average 30 min per patient was required for administrative purposes, including the diagnostic telephone interview. During the programme the software sent a total of 568 automatic emails to treatment group participants (mean = 23.7 per participant), and the clinician sent 132 personal instant messages (mean = 5.5 per participant). The clinician also made a total of 98 telephone calls (mean = 4.1 telephone calls per participant) and made 26 forum postings to the entire group.
Discussion
Because GAD is a chronic and disabling condition that is associated with considerable health service utilization, the development of new treatment techniques is a priority. To our knowledge the present study is the first published report of an RCT exploring the efficacy of an Internet-based CaCCBT treatment programme for this condition. Participants in the present study had non-trivial levels of GAD that were consistent with those seeking traditional face-to-face treatment. Furthermore, 15/24 (63%) treatment group participants reported scores on a measure of depression consistent with a DSM-IV diagnosis of depression, indicating that rates of comorbidity with depression appeared consistent with other clinical groups.
The first hypothesis, that participants would show significant improvements on measures of GAD, depression, and disability, was supported. Mean within- and between-group effect sizes (Cohen's d) for the GAD-7 and PSWQ were 1.33 and 1.10, respectively. This is comparable to improvements typically reported in meta-analyses of face-to-face CBT-based treatment of GAD [49, 50]. Within- and between-group effect sizes for the secondary outcome measures was as follows: for the PHQ-9 they were 0.90 and 0.86, respectively; for the K-10 they were 0.75 and 0.81, and for the SDS these were 0.62 and 0.78, respectively.
Remission rates (GAD-7 total scores below the cut-off for a likely diagnosis of GAD) at post-treatment assessment were 79% and 14% for the treatment and control group participants, respectively, providing further evidence of clinical efficacy. A similar pattern emerged in rates of recovery (i.e. reductions >50% of pre-treatment GAD-7 scores), with 63% of treatment group participants and 10% of controls meeting this criteria at post-treatment assessment. The pattern of change on the GAD-7 and PSWQ differed slightly: scores on the GAD-7 improved in both treatment and control groups, but not on the PSWQ, although the final between-groups effect size was comparable. This provides preliminary support for the use of the GAD-7 as a measure of treatment response, but it may be that the GAD-7 reflects state GAD, while the PSWQ reflects trait GAD, and will thus change more slowly than the GAD-7. If this is so then changes in the PSWQ will not be evident until follow up. Although further evaluations are required to determine the psychometric properties and utility of the GAD-7, it may be a useful tool for identifying early change in treatment.
The second hypothesis, that participants would rate the treatment programme acceptable, was supported. That is, 75% of participants completed the programme, 85% of treatment group participants who completed the post-treatment questionnaires reported being either very satisfied or mostly satisfied with the programme, 15% evaluated the programme as neutral, with no participants reporting that they were dissatisfied with the programme.
Consistent with many Internet-based treatment programmes, these results were obtained with less therapist time (a mean of 130 min of therapist time per patient) than that typical of face-to-face treatment programmes. Despite the reduced time, patients received a mean total of 33 direct contacts during the 9 week programme, which consisted of automatic emails and instant messages and telephone calls from the therapist. The ability to efficiently apply therapist time by using assistive technologies while maintaining high numbers of patient contacts is an important potential strength of the Internet approach, given recent evidence that completion rates and clinical outcomes are potentiated by automatic reminders [23, 24].
Limitations
One limitation of the present study was the small sample size, and this issue will be addressed in a forthcoming RCT using a much larger sample. A second limitation is the absence of follow up; this is also planned, and will be subsequently reported.
Conclusions
These preliminary results indicate that the Worry programme has clinical efficacy and completion rates comparable to those associated with face-to-face treatment, and is a procedure that appears acceptable to participants. These findings are consistent with our previous reports of the efficacy of similar treatment programmes for depression, panic disorder, and social phobia [16–26]. The challenge now is to determine the most acceptable and effective ways of incorporating such programmes into the existing mental health systems to improve the care of people with common mental disorders.
Footnotes
Acknowledgements
The authors gratefully acknowledge the participants for their involvement and helpful comments, and the Australian Rotary Health Research Fund for their funding of this study. We also wish to gratefully acknowledge the contributions to the development of the Virtual Clinic programme by Mr Jason Hando and Mr Daniel Winter.
