Abstract
We describe a 63-year-old smoker who suffered from intractable facial pain secondary to an underlying lung neoplasm. Data from 30 previously reported and similar cases are also summarized. The clinical triad of a smoker suffering from periauricular pain and an elevated ESR should alert the clinician to the possibility of an occult lung mass. In these cases a computed tomography of the chest should always be obtained. Previously refractory pain typically responds to surgical resection of the mass and/or radiation therapy.
Keywords
Introduction
Facial pain has numerous potential aetiologies including dental, otorhinolaryngological, and neurological disorders, often leaving the clinician faced with an array of possible diagnoses. Diseases involving the thorax and abdominal viscera may also cause ‘atypical facial neuralgia’ as originally suggested by Fay in 1932 (1). Years later, Des Prez and Freemon described the first case of a patient suffering from facial pain thought to be secondary to an underlying occult lung mass (2). Since then, the largest collection of reported cases came from the Mayo Clinic in which 10 cases were discovered in the period of a decade (3). Though recognized as a rare culprit, underlying lung neoplasms must be considered in these cases because of the morbidity and mortality associated with delayed diagnosis. The purpose of this paper is to refine the clinical spectrum and therapeutic outcome of facial pain secondary to a lung mass. The underlying pathophysiology and suggestions for appropriate work-up will also be discussed.
Methods
A previously unreported patient suffering from facial pain secondary to a lung neoplasm is summarized as an illustrative case study. In addition, further cases were identified by searching the MEDLINE database (1966–2001/English only) by combining ‘facial pain’ with ‘lung cancer’. A total of 30 additional cases were found (2–11). Data were collected from all these cases and summarized.
Results
Illustrative case study
A 63-year-old man with a 65 pack-year history of smoking presented to the clinic with a chief complaint of right-sided facial pain of 5 weeks duration. The pain was an incapacitating, constant, dull ache which was maximal in the auricular and temporal areas. Prior attempts to control his pain with medications including opioids were unsuccessful. He had additional complaints of insomnia, cough, and a poor appetite leading to a 9-kg weight loss. There was no history of jaw claudication, visual changes or myalgias. Prior to our evaluation he had a magnetic resonance imaging (MRI) of the brain which was normal. Auscultation of the lungs revealed diminished breath sounds in the right-upper lobe. There was no clubbing, scalp tenderness or lymphadenopathy on examination, and the neurological examination was unremarkable.
An ESR was mildly elevated (33 mm/h) and a chest X-ray showed a mass in the right hilar region (See Fig. 1). Biopsy was consistent with non-small cell carcinoma of the lung. The patient started both chemotherapy and radiation therapy but died shortly thereafter. Although improved, he was still suffering from pain at the time of his death.
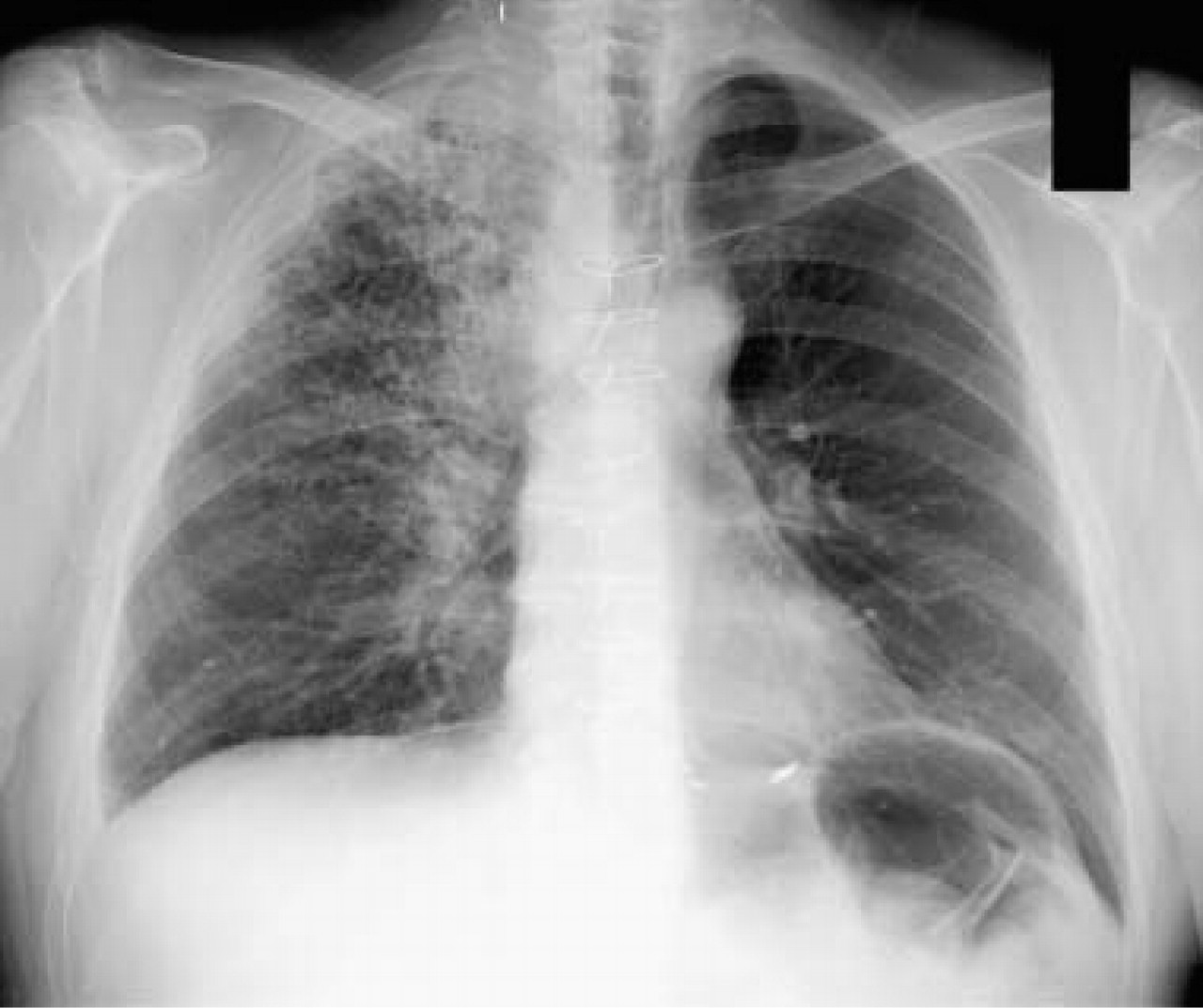
A chest X-ray showing a large mass in the paratracheal and hilar region with scattered infiltrates in the right upper lobe.
Summary of data
There are at present 31 cases of facial pain secondary to non-metastatic lung cancer in the literature. Of the patients, 61% were women. The average age at the time of presentation was 54.7 years with an age range from 34 to 78 years. All of the patients were either smokers or former smokers.
The most common (79%) description of the quality of pain was a ‘constant ache’. Specific complaints of auricular pain occurred in 84% of patients and represented the most common site of pain. Pain was more common on the right side (63%) than the left (37%). There is one case report in which the pain progressed to be bilateral (5). In all of the patients, the pain was ipsilateral to the lung mass. The average duration of facial pain prior to diagnosis was 8.3 months, with a range from 1 to 24 months. Symptoms suggestive of a lung malignancy (weight loss, new cough and/or haemoptysis) were present in 70% of the cases.
Newly developed digital clubbing was present in 33% of the patients in whom the digit examination was documented. Abnormal breath sounds ipsilateral to the lung mass were not uncommon, and the neurological examination was unremarkable in all the cases.
Computed tomography (CT) and MRI imaging of the brain were performed in 83% and 29% of the patients, respectively. Neuroimaging disclosed no evidence of cranial or cerebral metastasis. CSF analysis was normal in the 13% of patients who had lumbar punctures (5, 7). Chest CT revealed lung masses in 19% of the cases when the initial chest X-ray was ‘normal.’ An ESR was elevated in 77% of those patients who had the test performed. Of the 77% of the patients with an elevated ESR, 70% had an ESR> 65 mm/h; the remainder had an ESR of 33, 36 and 47 mm/h. Biopsy results most commonly (50%) showed findings consistent with adenocarcinoma of the lung. Other lung tumours included squamous cell (17%), small cell (10%), large cell (7%) and carcinoid (6%).
At the time of diagnosis 79% of the patients had regional spread and 14% had distant metastases. The most common type of treatment was radiation therapy followed by surgical resection and then chemotherapy. All of the reported patients who had surgical resection had immediate relief of their pain. Patients who survived long enough had good to excellent control of their pain with radiation therapy. Only one patient who received only chemotherapy had a satisfactory response (7). Table 1 summarizes the clinical profile of patients suffering from facial pain secondary to an underlying lung neoplasm.
Clinical profile of patients suffering from facial pain secondary to an underlying lung neoplasm

Discussion
In previous publications, infiltration of the vagus nerve has been implicated to explain the mechanism by which a mass in the lung can refer pain to the ipsilateral ear (2, 3, 5). The vagus is known to be a mixed nerve possessing parasympathetic, motor and sensory components. General visceral afferents (GVA) project sensation from the pharynx, larynx, thorax and abdomen to the nodose ganglion, which is then sent to the nucleus solitarius situated in the medulla. The jugular ganglion, on the other hand, sends general somatic afferents (GSA) to the descending nucleus of the trigeminal system. These GSA fibres carry sensory information from the dura mater of the posterior fossa, the pharynx, and a portion of the tympanic membrane and concha of the ear via the auricular ramus (4). A lung mass which abuts or infiltrates the vagus nerve can thus refer pain to the ear via the convergence of GVA and GSA in the medulla (5). Supporting this theory, Fay noticed that during surgical procedures which stimulated or applied traction to the vagus stump, pain was referred to the tongue, pharynx and ear (1). Furthermore, these GVA signals can cause a vague ipsilateral facial pain via convergence at the level of the descending nucleus of the trigeminal system (3, 5) (see Fig. 2).

The anatomical connections that provide an explanation for how a lung mass can cause referred pain to the ipsilateral ear and face. GVA, General visceral afferents; GSA, general somatic afferents; JG, jugular ganglion; NDG, nodose ganglion; NA, nucleus ambiguus; DM, dorsal motor nucleus; NS, nucleus solitarius; STT, spinal trigeminal tract and nucleus; M, motor fibres; N of A, nerve of Arnold.
Because of the relative rarity of non-metastatic lung cancer presenting as facial pain, the clinical profile of these patients has been slow to develop. Our analysis reveals that the most consistent clinical features include: a current or former smoker (100%), pain in the ipsilateral ear (84%), and an elevated ESR (77%). Almost two-thirds of patients (who had available data) had this clinical triad; therefore, it should alert the clinician to the possibility of an occult lung mass. Additional suspicion should be raised if a patient complains of weight loss, new cough or haemoptysis, or the exam reveals new onset clubbing or abnormal breath sounds. All patients should have a chest X-ray. If the chest X-ray is negative or equivocal, a CT scan of the chest should be done, since chest X-rays may not reveal the pathology in up to 20% of cases.
The most definitive and immediate form of pain control is surgical resection. Patients generally have an excellent response, with most becoming pain free. Unfortunately, because of delayed diagnosis, surgical resection is often not feasible. In fact, because of advanced disease only one-third of the patients were able to be treated surgically. At the time of diagnosis, 79% had regional spread and 14% had distant metastasis. Early detection affords the opportunity for improved mortality rates in these patients. Radiation therapy has proved to be an effective means to control pain, but patients are apt to respond more slowly over weeks to months. Because patients with advanced disease are often treated with radiation (not a surgical candidate), they may die before satisfactory pain relief is obtained. Chemotherapy was infrequently employed and was the least effective in ameliorating the facial pain. There is only one case report of a patient's pain responding to chemotherapy alone (7). Like radiation therapy, the analgesic effect from chemotherapy is often delayed. As a rule, medical management including opioids is ineffective in controlling these patients’ pain and more definitive treatment must be sought.
