Abstract
Reports of paedoptera dermatitis are commonly found in tropical and subtropical regions, while reports in China are rare. In September 2022, an outbreak of paedoptera dermatitis occurred in a minority autonomous county in southwestern China. Here, we report 134 patients with paedoptera dermatitis who were treated at the People’s Hospital of Sandu Shui Autonomous County. The skin lesions of these patients were mostly located on the face, neck, trunk, or multiple sites. The skin lesions were mainly distributed in patches and were characterized by vesicular linear or “kissing” lesions. Most patients felt burning pain, and few patients felt pruritus. The treatments with oral antihistamines, calamine lotion, steroids, and antibiotics were effective. For patients with ocular involvement, treatments with oral prednisone and bufexamac cream were effective. All patients recovered within 2 wk. There is a possibility of another outbreak of paedoptera dermatitis in the region. Awareness of the condition and its clinical features will prevent misdiagnosis. Early diagnosis and timely treatment lead to a better prognosis for paederus dermatitis. Simple preventive measures can be undertaken based on the behavioral pattern of this nocturnal beetle.
Keywords
Introduction
Paediatera dermatitis is an acute erythematous and pustular skin inflammatory disease caused by the venom of the insect, mainly Paediatera toxin, which is produced by the insect’s bacterial flora.1,2 There have been reports of paedoptera dermatitis in multiple countries around the world, mostly those in tropical and subtropical regions.3,4 Guizhou Province is located in southwestern China, and the most common paedoptera is the genus Philanthus. Reports of outbreaks of paedoptera dermatitis in China are very rare.
Sandu Shui Autonomous County is located in the southeast of Guizhou Province, belonging to the humid monsoon climate type of the middle subtropical zone. In September 2022, there was an outbreak of paedoptera dermatitis in the region. From September 2 to September 24, 2022, Sandu County People’s Hospital admitted 134 patients with paedoptera dermatitis. Therefore, we decided to evaluate the epidemiological and clinical manifestations of paedoptera dermatitis during this epidemic.
Patients and Methods
One hundred thirty-four clinically confirmed patients with complete case data of paedoptera dermatitis admitted to Sandu County People’s Hospital in September 2022 were selected as the study population. All patients had no history of allergies or other skin conditions. Diagnostic criteria for paedoptera dermatitis 1 were as follows: 1) a history of contact with paedoptera; 2) patchy, striped, or mixed edematous erythema appearing on the exposed parts of the body, with surface erosion and dense pustules; 3) and burning pain and itching. Exclusion criteria were as follows: 1) patients who have been rediagnosed due to the same disease and 2) patients with other similar skin diseases, such as pustules, contact dermatitis, herpes zoster, bacterial folliculitis, etc.
Case information of the study subjects was collected, including general information and information about clinical features (consciousness symptoms, location of skin lesions, and nature of skin lesions) and treatment plans.
Results
A total of 134 patients treated at the People’s Hospital of Sandu Shui Autonomous County were included in this study, and 2 of them were hospitalized. These patients were aged between 9 mo and 83 y (mean age, 25.4±10.7 y; median age, 26 y). There were 58 male patients and 76 female patients. The cutaneous lesions were present from 1 to 5 d before presentation (mean, 2.2±1.3 d; median, 2.0 d). The main site of skin lesions was the exposed area, including 24 cases on the face (17.9%), 22 cases on the neck (16.4%), 24 cases on the trunk (17.9%), 19 cases on the limbs (14.2%), 4 cases on the perineum (3.0%), 5 cases on the armpit (3.7%), and 36 cases (26.9%) on multiple sites (>3 sites).
There were significant differences in skin lesions among patients with paedoptera dermatitis in this group, but the main manifestations were edematous erythema and multiple pustules, and some may have had erosion and exudation. In 12 patients (9.0%), the presentation was “kissing lesions” (Figure 1A). In 85 patients (63.4%), typical linear lesions were present (Figure 1B). In 37 patients (27.6%), the presentation included erythematous geographic patches with a “burnt” appearance (Figure 1C). Ninety-five patients (70.9%) complained of burning sensation over the lesions, and 35 (29.1%) had itching at the site of lesions. Vesicles were present in 11 patients (8.2%) and pustules in 38 patients (28.4%). Two patients were hospitalized due to fever (>38.5°C). The reason for the fever in these 2 patients may be secondary infection at the bite sites.
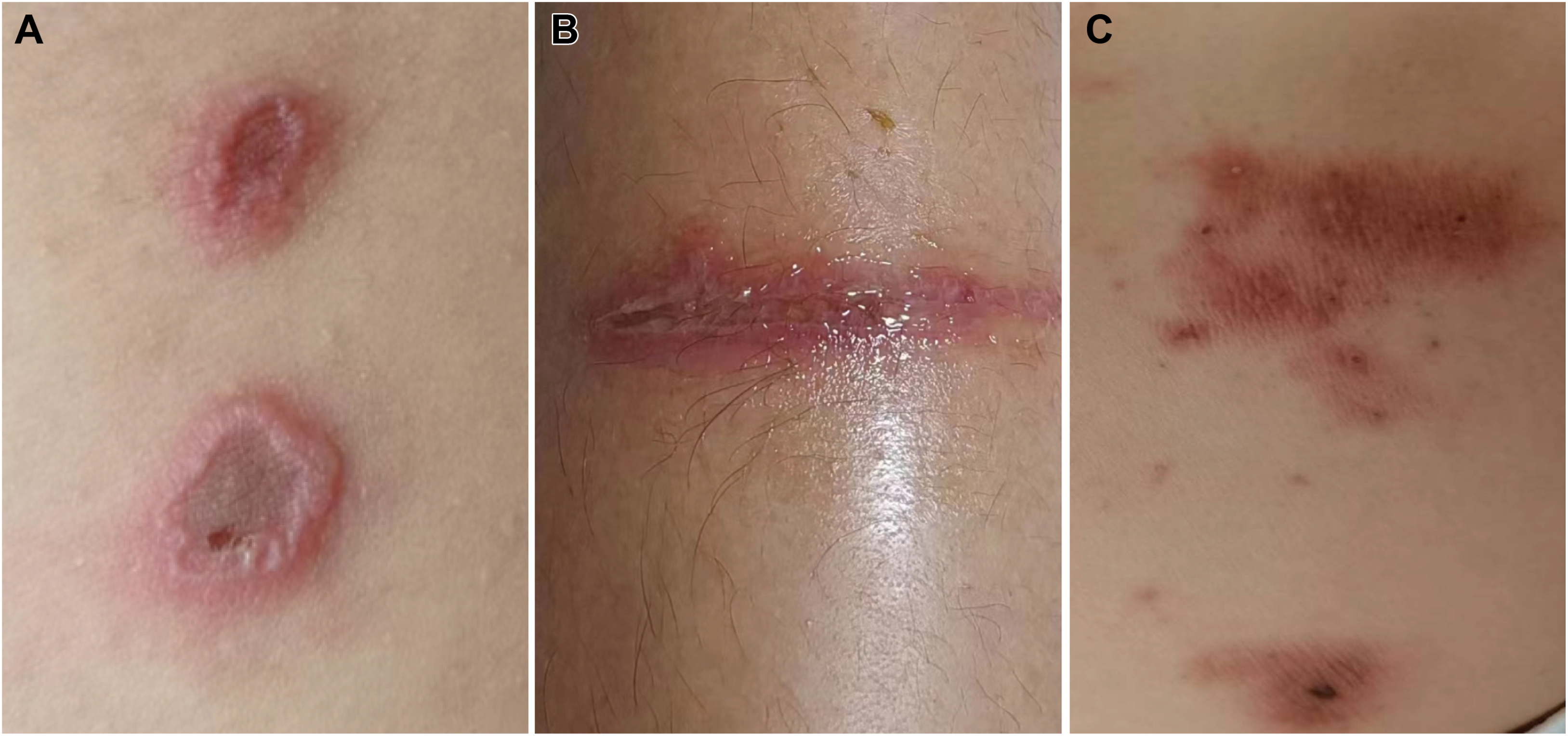
Skin lesions caused by paedoptera. A, Characteristic “kissing” lesion on abdomen. B, Vesicular linear erythema on forearm. C, Erythematous patches in shoulder region.
These patients received a basic treatment plan, including scrubbing the damaged skin with a 5% sodium bicarbonate solution, oral antihistamines combined with topical calamine lotion, and glucocorticoids. Thirty-five patients (26.1%) received local antibiotic treatment, and 2 patients (1.5%) received systemic antibiotic therapy. All patients recovered within 2 wk. The mean time for wound recovery in these patients was 7±5 d. One hundred twelve patients (83.6%) developed pigmentation at the end of 2 wk.
Discussion
Paediatera is a type of beetle in the Coleoptera order with a wide distribution range. There are more than 600 species in the genus Paediatera, among which there are more than 20 species of toxic Paediatera that can cause dermatitis.5,6 The main cause of paedopteran dermatitis is the toxin pederin (pH 1–2), but the insect cannot produce pederin by itself; it is produced by Pseudomonas aeruginosa living symbiotically within female adult Paederus. 1 Paederus does not cause dermatitis by biting the human skin. There are 2 main ways of infection: one is by directly crushing the insect’s body onto the skin, which is called direct infection; the other is indirect contamination, which occurs when clothing, towels, or hands with venom come into contact with other parts of the body after contact with paedoptera. Regardless of the form, there is often a kneading action, which is also one of the reasons for the diverse shapes and different sizes of damaged areas of dermatitis.
In the past, there has been no outbreak of paedoptera dermatitis in Sandu Shui Autonomous County. In the past 6 mo (March to August 2022), only 5 such patients have visited the hospital for treatment. This outbreak may be related to climate change. In September 2022, the temperature and humidity in the region were higher than in previous years. Previous reports have shown a close correlation between the number of adult beetles and humidity, and humid climate conditions are conducive to the large-scale reproduction of beetles. 7 This study found that the clinical characteristics of paederus dermatitis in the region are consistent with those reported in previous studies. 8 The face, neck, and inner forearm are the most prone areas to skin damage, which is more common in exposed areas and less common in the eyes and genitals. In this report, there were 3 patients with orbital involvement who developed varying degrees of eyelid edema and conjunctival congestion. The most typical symptom of paedoptera dermatitis is burning pain, followed by itching. 9 The typical skin lesions present as erythema and pustular-like changes in the center of the erythema, followed by new keratinocytes maturing at the bottom of the pustule, forming a scab. 10 When the lesion exhibits “linear” or “kissing” lesions, it needs to be differentiated from herpes zoster, bullous pustulosis, and other related diseases. 11 A previous study has reported that paederus dermatitis can cause ulcers of up to 7 cm in diameter, 12 although in this series of cases, no patient’s condition evolved to this severity. There are several species that can cause dermatitis, and variations in the presentation of manifestations in different regions or periods may depend, among multiple variables, on the species of Paederus that caused the case or outbreak.
We adopted a treatment plan based on scrubbing damaged skin with a 5% sodium bicarbonate solution, oral antihistamines combined with topical calamine lotion, and glucocorticoids, which is safe and effective. For patients with mild conditions, mometasone furoate cream can be used as a local topical hormone, which belongs to the category of medium effective glucocorticoids. It is anti-inflammatory and antiallergic, and after absorption, it can effectively relieve itching and reduce exudation. However, long-term use carries the risk of skin atrophy and secondary infection. Topical antiseptic solutions were also used to treat ulcerative lesions caused by insects of the Paederus genus. 12
For patients with orbital lesions, oral steroid hormone therapy is given, 13 while benzoic acid cream is used externally. Butyrrhetinic acid cream is a nonsteroidal anti-inflammatory drug with anti-inflammatory and antiallergic functions. Patients with poor tolerance to mupirocin can choose fluoxetine cream. Phimosis is a self-limited disease with a course of 7 to 10 d, but it can cause complications such as pigmentation, secondary infection, extensive desquamation, and ulcerative dermatitis. 14 In addition, potassium permanganate is a powerful oxidant that has extensive antibacterial activity. It also promotes the formation of collagen and granulation tissue, which favors wound healing. 12
There is a possibility of another outbreak of paedoptera dermatitis in the region. Awareness of the condition and its clinical features will prevent misdiagnosis. Early diagnosis and timely treatment lead to a better prognosis for paederus dermatitis. Simple preventive measures can be undertaken based on the behavioral pattern of this nocturnal beetle, such as having windows closed, staying away from humid environments, spraying with pesticides, and keeping doors closed in the evening and night.
Footnotes
Acknowledgements
Author Contributions: study conception and design (XF); data collection (JL); literature survey (JM); contribution to writing and checking of the manuscript (BF).
Financial/Material Support: This work was supported by NSFC numbers 82060209 and 82160362 and by the National Natural Science Foundation of China.
Disclosures: None.
Patient and public involvement: Patients and/or the public were not involved in the design, conduct, reporting, or dissemination plans of this research.
Patient consent for publication: Written informed consent was obtained from the patient for publication of this case report and any accompanying images.
Ethics approval: There are no ethical/legal conflicts involved in the article.
