Abstract
This article describes the clinical presentation, differential diagnosis, and treatment of 2 unrelated cases with different presentations of black-spot Toxicodendron dermatitis. In the first case, a healthy 7-y-old male presented with a rash consisting of black dots with localized surrounding erythema on the left arm. The rash then progressed to a vesicular, pinpoint, raised rash spreading to the face, arms, and neck. In the second case, a 4-y-old male presented with non-pruritic, black, flat, non-erythematous lesions that did not progress. This patient’s older sibling had been diagnosed with poison ivy 1 wk prior, and they attended the same child care where the poison ivy was thought to be acquired. In both cases, diagnosis of black-spot Toxicodendron dermatitis was made. The black spot of Toxicodendron dermatitis is caused by urushiol oxidation on exposure to air. The subject may or may not go on to develop allergic contact dermatitis after the exposure. Diagnosis of this dermatitis is made on clinical presentation, with careful consideration of history, distribution, and lesion morphology. When allergic dermatitis does develop as in the first case, systemic treatment with oral steroids is recommended. In both of these cases the black dots completely resolved in 2 to 3 wk. Dermatologic referral for dermoscopy and biopsy may be necessary if the dermatosis does not resolve as anticipated.
Keywords
Introduction
Poison ivy species (Toxicodendron radicans), poison oak (T diversilobum), and poison Sumac (T vernix) plants in the Toxicodendron genus are one of the most common causes of allergic contact dermatitis, affecting 10 to 50 million Americans per year. 1 They are expected to become more common with increasing CO2 and fragmentation of habitats.2,3 Approximately 50 to 75% of the population are sensitive to urushiol (a colorless oleoresin), the substance in plants of the genus Toxicodendron that causes allergic contact dermatitis 4 and are therefore at risk for allergic reactions. The prevalence of sensitivity decreases in larger, urban areas where such plants are less common, 10 to 15% of the population does not react to a concentration 1000 mg of urushiol. 4 The peak frequency for sensitization occurs between the ages of 8 and 14 with less sensitization in infants. 5 Contact with any portion of the plant can potentially trigger a skin reaction. If the plant is traumatized, the sap is extruded, hardens, and the plant seals off the resin channels. Black dots may be visualized on the surface of the plants of the genus Toxicodendron in areas of trauma. 6 On exposure to air, urushiol in the sap oxidizes, polymerizes, and turns black, causing black skin discoloration.7,8
Black-spot poison ivy dermatitis is a rare presentation of poison ivy dermatitis first described in 1923. Black, enamel-like deposits were found on the hands of gardeners who were exposed to Toxicodendron sap. 9 Fewer than 25 cases have been reported in the literature prior to 2011.10,11
Histologic evaluation of these black spots demonstrates resin on the surface of the stratum corneum with a neutrophilic infiltrate and areas of epidermal necrosis beneath it, in contrast to typical poison-ivy dermatitis, which reveals superficial perivascular infiltration without evidence of resin or necrosis.12,13 Dermoscopy reveals a jagged, homogeneous, brown lesion with a red rim, suggesting uneven diffusion of urushiol within the stratum corneum. 14 The black spot tends to appear within 1 h of contact with urushiol and typically falls off in 1 to 2 wk. 15 Among those sensitive to urushiol, allergic symptoms after exposure are typically seen between 24 and 48 h, with a range of 5 h to 15 d. 16 While the most typical presentation of black-spot Toxicodendron dermatitis will have both the black dots and other classical signs of poison ivy dermatitis, 10 to 15% cases will only present with black spots in people who are not sensitive to urushiol. 12
Case Reports
Case 1
A 7-y-old otherwise healthy boy presented in early summer to a pediatric clinic in central Virginia for an evaluation of a rash located on his left arm. This rash was first noted 1 wk prior as black dots that did not wash off with soap and water. The guardian initially thought that the black dots were drawn with a permanent black marker. Two days before presenting to clinic, the patient developed nonpruritic, raised inflamed areas around the black dots, prompting the visit. The patient’s guardian had applied hydrocortisone cream without response. The patient had no other symptoms and no history of atopic dermatitis. The patient lived near the woods. He had no known exposures to insects, new foods, skin products, medications, or plants. On physical exam, all vitals were normal, and there were no abnormalities except for the skin findings. Examination of the skin revealed linear, raised, blanchable, erythematous areas on the neck measuring 2 cm at the greatest length with pinpoint vesicles, as well as linear, raised, blanchable, erythematous areas on the left arm measuring 3 cm at the greatest length with pinpoint vesicles around 3 black lesions (Figure 1).
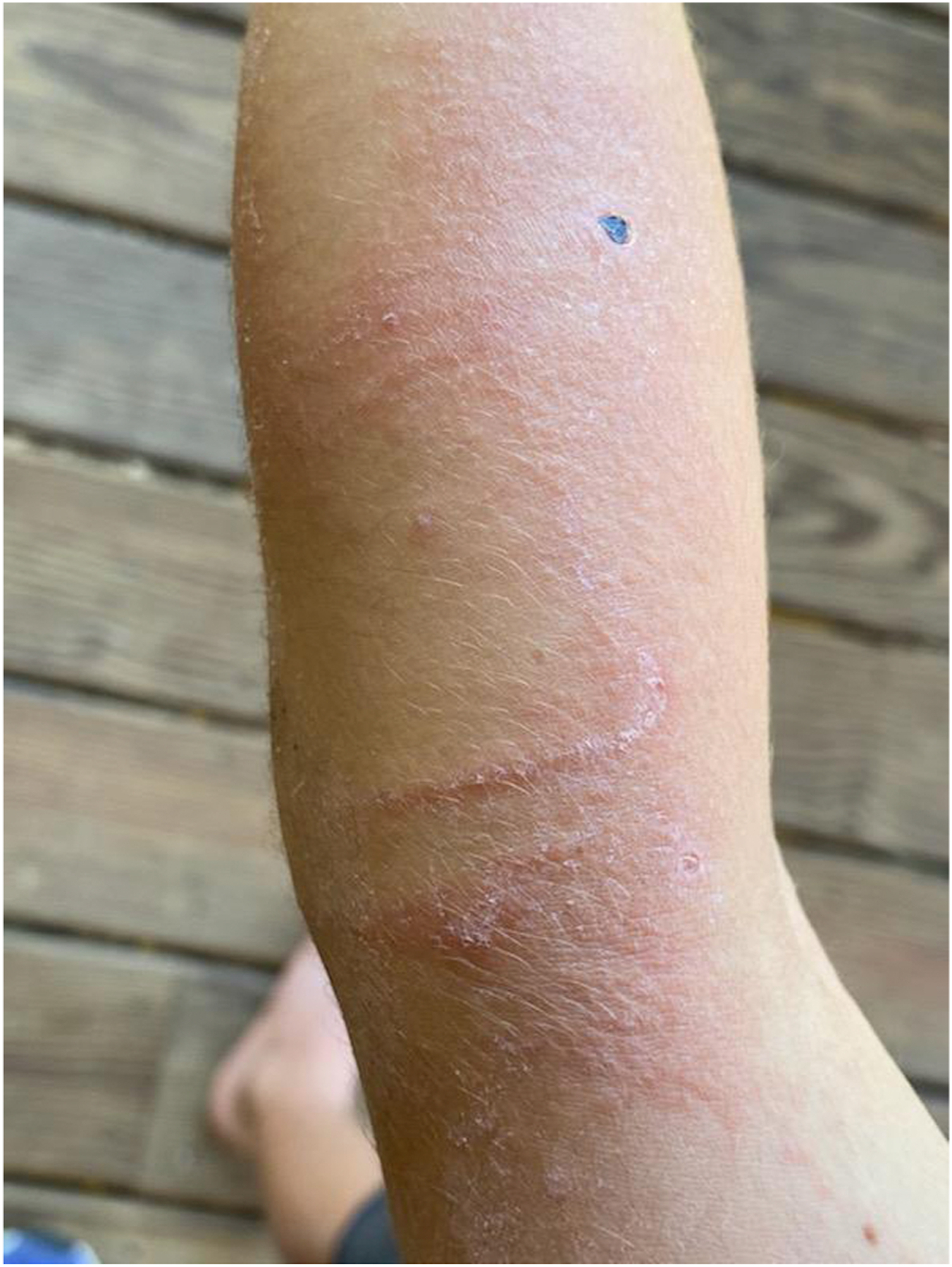
Case 1: Triangular-shaped black lesion on left arm with surrounding erythematous, vesicular rash extending from upper arm through elbow to lower arm.
Based on the clinical distribution the clinical distribution of the rash, time course, and potential exposure living by the woods, a diagnosis of black-spot poison ivy dermatitis was made. Poison ivy predominates in central Virginia. Since the rash was localized, the patient was given triamcinolone 0.1% ointment for treatment of the local allergic reaction. Follow-up was recommended if skin findings worsened or any new symptoms developed. Five days later, the guardian called for concern that the rash was spreading and was now causing severe itching. The physical exam was unchanged except for skin findings, which had significantly worsened. The rash was now raised, blanchable, erythematous with some pinpoint vesicles and had spread to both arms, the right cheek, right ear, and neck with areas measuring up to 9 × 4 cm. The patient was diagnosed with poison ivy dermatitis with significant allergic reaction. The patient was prescribed a taper of oral prednisone at a starting dose of 1 mg·kg-1·d-1 and cetirizine at 5 mg daily. Oral steroids are recommended for treatment of allergic reactions for a course of 2 to 3 wk to prevent rebound dermatitis. 17 The patient was also advised to continue calamine lotion and oatmeal baths for comfort. Pictures were sent to the dermatologist, who confirmed the diagnosis. The patient’s guardian reported significant improvement of erythematous areas after 24 h. The rash resolved in 5 d. The black dots disappeared after 2 to 3 wk.
At the time of the initial presentation, the differential diagnoses included: contact dermatitis, eczema herpeticum, scabies, skin trauma, foreign body, writing implement marks, foreign body, nevus, or skin melanoma. The areas were flat, nontender, and non-purulent. The black lesions did not appear to be superficial enough to be secondary to a writing implement. The areas of erythema and linear vesicles on the arm at initial presentation were consistent with the distribution of poison ivy or poison oak dermatitis. The element of linearity highly favors a plant dermatitis, with the linear lesions roughly corresponding to sites on the arm that could be physically brushed by the offending plant. The patient recovered well. If the black dots had persisted, a referral to a dermatologist and possible biopsy would be indicated.
Case 2
A 4-y-old boy with a history of developmental delay presented in the early summer for evaluation to the health care provider with a 1-wk history of a non-pruritic, black dot rash around his ankles bilaterally. The patient’s guardian noted he had black dots on his ankles and a black dot on his left elbow. The patient had no history of atopic dermatitis or other symptoms. He had no known exposure to insects, new foods, medications, or skin products. The guardian reported that because the patient had a developmental delay, it would be challenging to assess whether this rash was causing discomfort. The patient’s guardian reported that the older sibling had been diagnosed with poison ivy 1 wk prior by another health care provider. This improved with topical hydrocortisone. The guardian reported that the sibling may have been exposed to poison ivy from the day care center that both children attended.
The remainder of the exam was normal except for the skin findings: non-tender, flat, black macules on the lateral portion of the ankles and the left elbow (Figure 2).
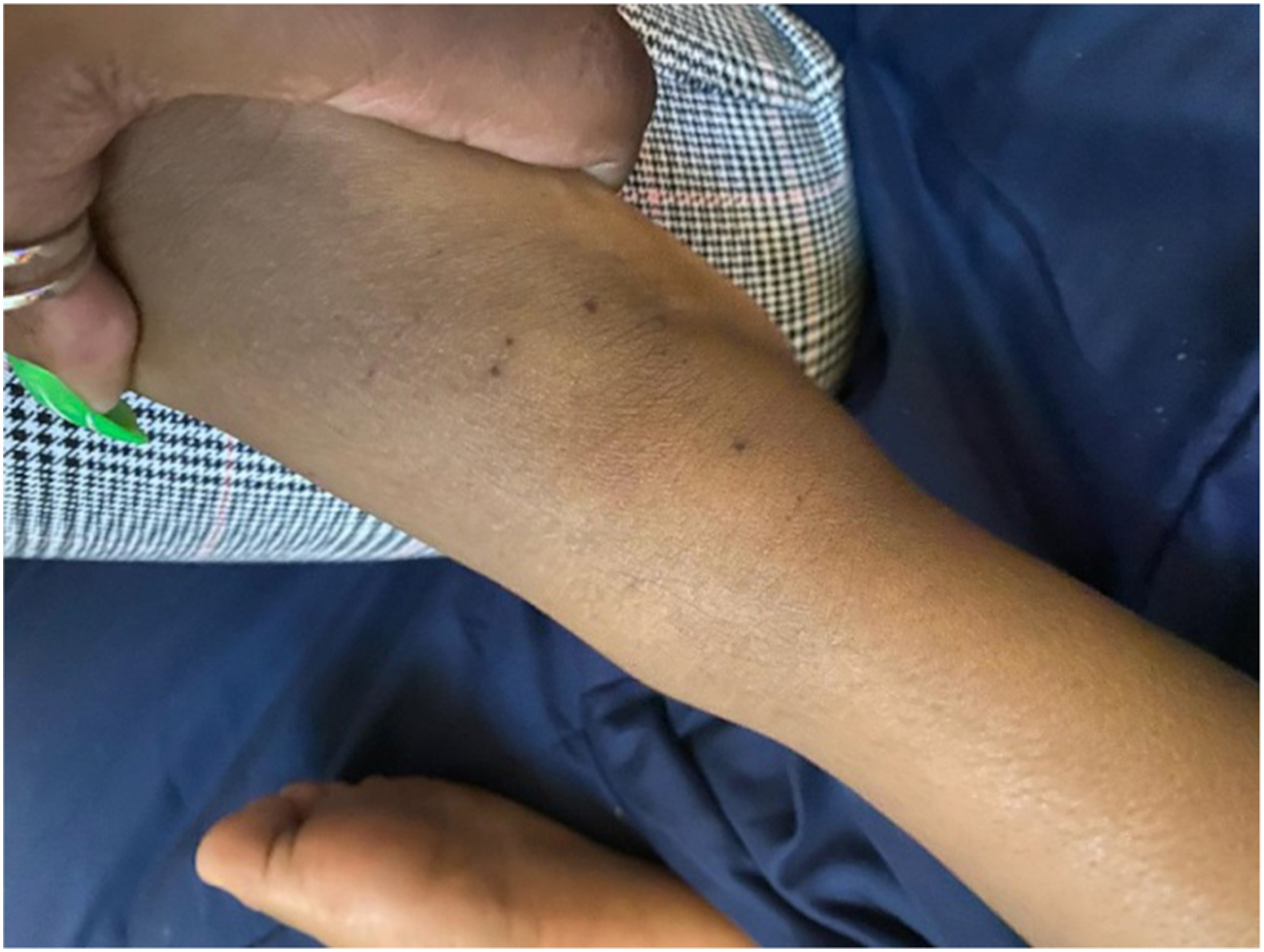
Case 2: Black lesions on right lateral ankle.
Because the black dots were a new presentation and the sibling had been diagnosed with poison ivy dermatitis 1 wk prior, black dot poison ivy dermatitis was diagnosed. The guardian was advised to follow up if the rash worsened or new symptoms developed. Because the rash resolved completely in 2 to 3 wk, the patient did not require further evaluation.
Discussion
Symptomatic treatment of black-spot poison ivy can include soothing topical treatments, oral antihistamines, high-potency topical corticosteroids, or oral glucocorticoids. Topical corticosteroids are most beneficial during the early stages of allergic contact dermatitis. 18 For severe dermatitis, particularly involving the face or inguinal region, oral glucocorticoids are indicated.19,20 Expected outcome of black dot poison ivy dermatitis with treatment is full recovery. Lesions should be monitored for secondary bacterial skin infection and treated with antimicrobial therapy if indicated. Measures to prevent further allergic reactions include wearing protective clothing and avoiding poison ivy or poison oak. For clothing, wool is most protective along with leather gloves.8,21 If a person comes in contact with poison ivy/oak, recommendations include washing the area with Zanfel 22 (a mixture of alcohol solubles and surfactants), Tecnu (a mixture of mineral spirts, propylene glycol, octylphenoxy-polyethoxyethanoal, and mixed fatty acid soap), or isopropyl alcohol. Clothing should be laundered, and tools should be washed with a dilute solution of bleach. 8
Black dot poison ivy typically resolves in 1 to 2 wk, although this can take longer, as in the cases we presented. Failure of the rash to resolve in 3 wk should prompt a dermatology referral. Time course of rash resolution may assist in determining if dermatology referral and biopsy are indicated and depending on the clinical evolution may be unnecessary.
Footnotes
Acknowledgements
Author Contributions: Clinical evaluation (ER, RA); drafting, critical revision, and approval of final manuscript (all authors).
Financial/Material Support: None.
Disclosures: None.
