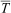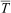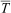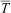Abstract
Introduction
The purpose of this work was to evaluate the effectiveness of 3 rewarming techniques to determine how warfighters, and perhaps other populations in wilderness environments, should prioritize field rewarming options after a brief accidental immersion in cold water.
Methods
As part of a cold weather military training exercise, 31 military personnel (mean±SD age: 26±5 y, height: 180±10 cm, weight: 83.2±10.9 kg) completed a 10-min immersion in cold (0°C) water and subsequently rewarmed for 60 min using 3 different field rewarming techniques (sleeping bag, sleeping bag + warm fluids, or exercise). Heart rate, core and skin temperatures, thermal and shivering sensations, and manual dexterity (intravenous setup and insertion) were measured during the training exercise.
Results
Cold water immersion decreased core temperature (pre: 37.4±0.4; post: 36.4±1.0°C; P<0.001) and mean skin temperature (pre: 27.9±1.3; post: 15.6±1.8°C; P<0.001) and impaired manual dexterity (intravenous insertion time, pre: 71±12, post: 166±48 s; P<0.001). Recovery from mild cold stress was similar among all 3 rewarming techniques for all measurements.
Conclusions
Findings suggesting similar rewarming responses in field settings are beneficial for the warfighter, and perhaps others, in that rewarming options exist and can be implemented with no compromise in recovery from cold stress.
Introduction
Accidental cold water immersion presents several challenges for those venturing into remote wilderness settings, ranging from minor inconveniences to full-scale rescue efforts to recover body temperature and preserve life. 1 Among warfighters specifically (ie, sailors, soldiers, and Marines), accidental immersion impairs operational performance and deteriorates mission readiness. 2 Fortunately, military leaders often require their warfighters to train for accidental cold water immersion. They are taught to anticipate the cold shock response, control breathing to avoid hyperventilation, self-extricate after falling through ice, and rewarm in the field using various techniques. 3 –5
Rewarming in wilderness settings may include spontaneous rewarming (ie, shivering), body-to-body warming, ingestion of warm fluids, and exercise, among others.6,7 Reasons for implementing different rewarming techniques depend on situational variables, such as cold stress severity, equipment availability, weather conditions, and, for the warfighter, the presence of hostile forces. The success of rewarming is often measured using core temperature, which can be difficult to accurately assess in combat or wilderness settings. 8 Other indicators such as mental status and functional performance may need to be used in operational settings to evaluate recovery from accidental cold water immersion.
The Marine Corps Mountain Warfare Training Center (MCMWTC), located in Bridgeport, California, conducts cold weather field training exercises in environments that are likely to be encountered by warfighters. These training environments offer unique opportunities to gather important information on warfighter recovery after cold water immersion. Given the scarcity of literature on rewarming investigations conducted in field settings, evaluation of the efficacy of rewarming techniques in actual conditions encountered by warfighters is needed. The purpose of this work was to evaluate the effectiveness of 3 rewarming techniques used by Marine Corps personnel to determine how warfighters, and perhaps other populations in wilderness environments, should prioritize field rewarming options after a brief accidental immersion in cold water. Of the rewarming techniques used, it was hypothesized that exercise, and not spontaneous rewarming (with or without warm fluid ingestion), would provide a stronger stimulus for overall rewarming success.
Methods
Research Participants
Active duty military members were recruited to participate in this study. Per course requirements, students enrolled in MCMWTC’s cold weather medicine course were required to participate in immersion and rewarming training exercises to successfully complete the course. Therefore, only students enrolled in this course were recruited to participate.
Study Design
During the immersion and rewarming training exercise, participants moved through different phases with fixed times for each phase. Phases were defined as “pre” (before entering water; 5 min), “immersion” (water immersion to neck; 10 min), “post” (after exiting water; 5 min), “start rewarm” (start of 60 min rewarming), and “end rewarm” (end of 60 min rewarming). MCMWTC medical staff monitored participants’ core temperature (Tc), mean skin temperature (
Body Temperature, Heart Rate, and Temperature Sensations
Ingestible Tc pills (Respironics, Bend, OR) were administered to participants by MCMWTC staff approximately 8 h before the start of the immersion and rewarming training exercise. Skin temperature patches (Respironics) were affixed to the chest (centered over the pectoralis major), shoulder (lateral aspect of the right deltoid, slightly above the lateral head of the triceps), thigh (mid-thigh; centered over the rectus femoris), and calf (centered over the gastrocnemius).
Operational Task
Operational performance was assessed at pre, post, and end rewarm using a manual dexterity task. Participants were given 5 min to complete an intravenous (IV) insertion on a manikin arm (Nasco, Fort Atkinson, WI). Six steps were required for IV insertion and consisted of 1) puncturing IV bag, 2) flushing IV line, 3) closing in-line clamp, 4) placing tourniquet on manikin arm, 5) performing needle stick into median cubital vein of manikin arm, and 6) opening in-line clamp (simulating fluid infusion). Participants were allowed 1 attempt to reposition the needle to ensure successful insertion into the vein. Research staff recorded the accuracy of the required steps and the total time to complete the IV insertion (successful insertion confirmed by research staff based on “red flash” of artificial blood). All participants were current military medical providers, were familiar with IV insertion techniques, and were given ample time to practice the steps and techniques before beginning the task.
Rewarming
After immersion, participants completed 5 min at post and then changed into dry clothing. After donning dry clothing, they were randomly assigned to 1 of 3 rewarming groups, which consisted of 1) entering a sleeping bag (SB), 2) entering a sleeping bag and consuming 1 L of warm broth during 60 min (SB+F), or 3) completing 12 rounds of an exercise circuit (EX). Exercises consisted of 20 body weight squats, 20 jumping jacks, 20 push-ups, and 20 bicycle kicks (completed on a deck free of snow and ice). Participants completed each round of exercises every 5 min.
Statistical Analysis
The effects of cold water immersion were determined using a repeated-measures analysis of variance (ANOVA) to analyze Tc,
Results
Participants
Thirty-one active duty military members (30 male, 1 female) participated in this study and self-reported their age, height, weight, and body mass index (Table 1).
Demographic information (mean±SD) for all participants and each rewarming group.
SB, sleeping bag; SB+F, sleeping bag+warm fluids; EX, exercise.
Environmental Conditions
The immersion and rewarming exercise began at 0700 onsite at the MCMWTC (2100 m altitude). A small pond was used for immersion. At the start of the exercise, ambient environmental conditions were as follows: air temperature (−5°C), wind speed (0 m·s-1), and water temperature (0°C). Participants wore military clothing consisting of utility uniforms (t-shirt, blouse, trousers, socks, and athletic shoes).
Effects of Cold Water Immersion
Cold water immersion significantly influenced all measurements (Table 2). Specifically, cold water immersion decreased Tc (P<0.001), 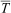
Physiological, perceptual, and dexterity responses (mean±SD) for pre, immersion, and post
HR, heart rate; SS, shivering sensation; Tc, core temperature; 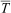
Different from pre (P<0.05).
Different from immersion (P<0.05).
Rewarming Evaluation
Rewarming groups were compared at start rewarm and end rewarm for each measurement. The change from start rewarm to end rewarm was also compared between groups for each measurement (Table 3). There were no differences among groups at start rewarm for Tc (P=0.807), 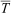
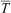
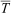
Physiological, perceptual, and dexterity responses (mean±SD) for start rewarm, end rewarm, and the difference (Δ) between start rewarm and end rewarm
EX, exercise; HR, heart rate; SB, sleeping bag; SB+F, sleeping bag+warm fluids; SS, shivering sensation; Tc, core temperature; 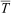
Different from SB (P<0.05).
Different from SB+F (P<0.05).
Discussion
This study evaluated the effectiveness of 3 rewarming techniques to determine how field rewarming should be prioritized in operational and other settings after a brief immersion in cold water. Findings indicate that 1) participants were mildly cold-stressed from cold water immersion and cold air exposure and 2) rewarming responses were similar among all rewarming groups for all measurements (Tc, 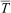
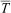
Cold water immersion severity, and the ensuing rate of body heat loss, is highly dependent on variables such as water temperature and movement, immersion duration, thermal protection, and depth of immersion (ie, partial vs full).
12
-15 In the current study, a 10-min immersion to the neck in a static, cold pond with minimal thermal protection lowered body temperature and caused participants to feel colder and perceive greater shivering. The immersion also deteriorated performance in a manual dexterity task; time to complete an IV after immersion took more than twice as long as before immersion. Deterioration of manual dexterity is expected with the skin temperatures reported, considering dexterity loss is noted by others when hand temperatures fall below 15°C.16,17 Although not measured in the current study, it is likely that hand temperatures were reduced below 15°C, given the observed 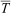
Investigations evaluating the efficacy of actual field rewarming are scarce, 18 but controlled laboratory studies suggest no difference in recovery times from hypothermia using spontaneous rewarming (shivering), exercise (treadmill walking), or external heat application. 19 Using cold water immersion, Giesbrecht et al. cooled participants to Tc 33°C and subsequently evaluated Tc recovery. They noted a large Tc afterdrop with exercise but found no final differences between shivering or external heat application rewarming techniques. Similar to findings from the current study, all 3 rewarming techniques provided a similar recovery. 19 Rewarming rates reported in the literature for shivering and exercise are 3 to 4°C·h-1 and 5°C·h-1, respectively,7,20,21 but this assumes hypothermia and not mild cold stress. In the case of mild cold stress, we report rewarming rates of only 1°C·h-1 for both shivering and exercise. Hence, the stimulus for faster rewarming rates appears to be influenced by lower Tc. Several concerns are raised when using exercise as a rewarming option in moderate to severe hypothermia in that the risk of cardiac irritability increases along with both time and magnitude of afterdrop.22,23 These concerns, however, are rarely raised for individuals who have only experienced mild cold stress. Exercise therefore remains a viable option for those who experience mild cold stress resulting from cold water immersion.
Warfighters represent a unique population; their actions for cold stress recovery could be highly dictated by dynamic military situations. For example, warfighters may not have the freedom to exercise in the open or access to stoves for heating warm broth. Instead, they may be engaged with hostile forces or require covertness to remain undetected.24,25 Findings suggesting similar rewarming responses in field settings therefore are beneficial for the warfighter, and perhaps others, in that options exist and can be implemented with no compromise in recovery from cold stress.
Limitations
Several limitations are present in the current study that require attention. The population studied consisted of primarily young male military personnel. All were fit for full duty and aware of the procedures that would take place during the field training exercise. In true accidental immersion, health status and age can vary greatly and victims are likely unaware of impending immersion, which may negatively influence physiologic and psychological responses to cold water immersion. 26 –28 Additionally, recommendations for field rewarming are typically focused on recovery from hypothermia and not mild cold stress. Although several participants did experience hypothermia, rewarming procedures started with each group near Tc 36.0°C. Had rewarming been evaluated from a Tc below 35°C, it is possible that the rewarming outcomes may have differed. Large variations in Tc were also observed in this population and are likely attributed to individual differences in subcutaneous fat amounts, vasoconstrictor and blood flow responses, and metabolic heat production.29,30 It is not anticipated that variations in Tc would greatly influence IV insertion time because dexterity performance is related more to finger/hand temperature and less to Tc. 31 For the EX rewarming group, exercises such as jumping jacks, bicycle kicks, and squats used at frequent intervals during rewarming included large muscle groups. However, it is possible that other exercise types and intensities could influence rewarming rates, and this should be taken into consideration in future investigations. 32 Lastly, warm broth provided to students was heated, but the temperature or timing of ingestion was not measured. This, too, could have influenced rewarming rates for the SB+F group.
Conclusions
The Wilderness Medical Society recently published clinical practice guidelines for hypothermia and addressed field rewarming recommendations. 6 Strong recommendations for shivering, shivering with ingestion of warm fluids, and exercise were presented, with shivering supported by high-quality evidence and shivering with ingestion of warm fluids and exercise supported by low-quality evidence. Findings from the current study, perhaps only relevant to mild cold stress and not true hypothermia, add to this growing body of knowledge and indicate that body temperature, perceptual measurements of temperature and shivering, and functional performance recover similarly among different field rewarming techniques.
Footnotes
Acknowledgements
Acknowledgments: The authors thank the staff at the Marine Corps Mountain Warfare Training Center for their support during this study.
Author Contributions: Study concept and design (DJ, JB, JH); acquisition of the data (DJ, DB, CC, KR, CP, JH); analysis of the data (DJ, DB, CC, KR, CP); drafting of the manuscript (DJ); critical revision of the manuscript (JB, JH); approval of final manuscript (DJ, JB, DB-T, CC, KR, CP, JH).
Financial/Material Support: This study was supported by the US Navy Bureau of Medicine and Surgery under work unit no. N1804.
Disclosures: None.