Abstract
An experienced 24-y-old climber on Mount Everest presented to the Base Camp medical clinic with a friction blister on his right flank. The blister was filled with clear fluid and was located about 3 cm posterior and 3 cm superior to the highest point of the right iliac crest, the site where a climbing harness would support the climber while hanging. A diagnosis of friction blister caused by a climbing harness used while traversing between Camp 2 and Camp 3 of Mount Everest was made. The blister was managed with hydrocolloid dressing, and the patient resumed climbing after 1 wk. The lesion healed with scarring at 2 wk. Friction blisters of the feet are common in climbers wearing ill-fitting shoes, but friction blisters caused by climbing harnesses are unusual and have not been reported in the literature as far as the authors are aware. All existing guidelines for blister management pertain to blisters of the feet, and there are inconsistencies in recommendations made by various authors. This unusual case in an extreme environment provides a good learning opportunity.
Introduction
Friction blisters of the feet are common in climbers as they perform high-intensity activities often with improperly fitting shoes. Blisters can cause pain and loss of normal foot function and are prone to secondary infection. Additionally, patients with blisters of the feet have been reported to be predisposed to secondary injuries compared to those without blisters, likely owing to altered joint biomechanics as a pain-avoidant mechanism.1,2 As far as the authors are aware, climbing harnesses have not been reported to cause blisters. Existing guidelines describe management of blisters on the feet. There are inconsistencies among different guidelines. 3 –5 Development of a friction blister at an unusual location in an experienced climber provides a unique opportunity to discuss the mechanism of blister formation, blister management guidelines, and patient safety while climbing in extreme conditions.
Case presentation
An experienced 24-y-old climber with a painless blister over the area where his climbing harness rested on his right flank presented to the authors, who were working as physicians at Everest Base Camp medical clinic. The patient had been climbing from Camp 2 (6400 m) to Camp 3 (7100 m) of Mount Everest several hours earlier. The patient noticed the lesion only incidentally after climbing down to Base Camp. On examination, he had a 3 cm × 2 cm brownish blister with clear fluid about 3 cm posterior and superior to the most superior point of the right iliac crest. The blister was intact. There was no erythema or warmth surrounding the lesion to suggest infection. A clinical diagnosis of a friction blister possibly caused by the climbing harness was made, and no further investigations were done. Management involved cleaning the area with povidone iodine followed by application of a hydrocolloid dressing and advising the patient to avoid climbing until he could be re-examined. He presented 3 d later with spontaneous rupture of the blister with the dressing still in place (Figure 1). The major portion of the roof of the blister was intact. This was left in place, the wound was again cleaned with povidone iodine, and a hydrocolloid dressing was reapplied. The dressing was left in place for an additional 4 d. When the patient was re-examined after 1 wk, he reported no discomfort, and the dressing was intact. On examination, the wound was healing and was clean and dry. A new hydrocolloid dressing was applied for protection. The patient resumed climbing with a different climbing harness with the dressing in place and reported no discomfort. On day 14 after initial presentation, the patient climbed above Camp 4 (7950 m) of Mount Everest with a client. He was re-examined at the clinic after descent, and the wound was healing with minor scarring (Figure 2). Upon follow-up at 2 mo, the lesion had completely healed with some scarring (Figure 3).
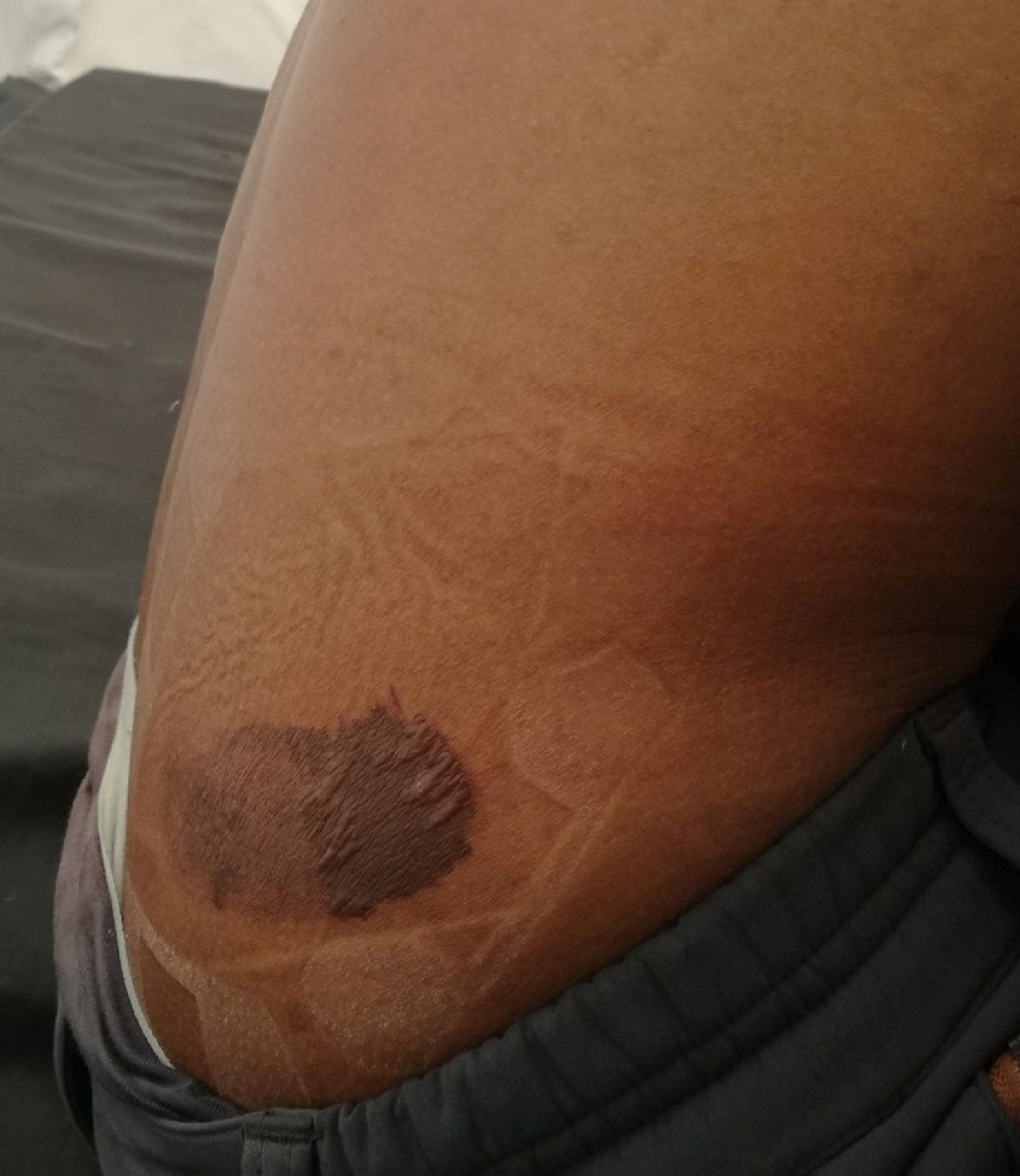
Blister at 3 d.
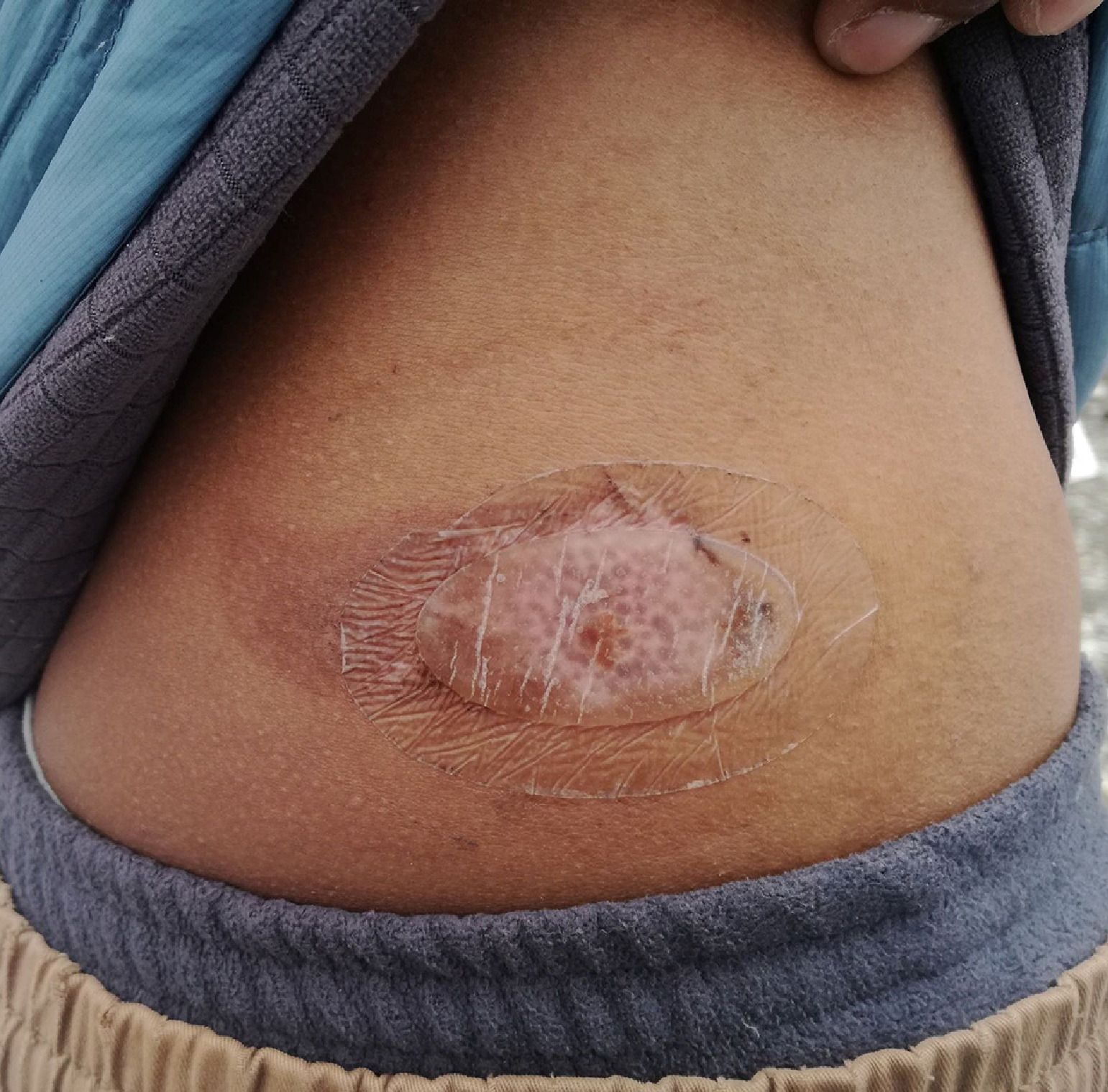
Blister at 2 wk with dressing.
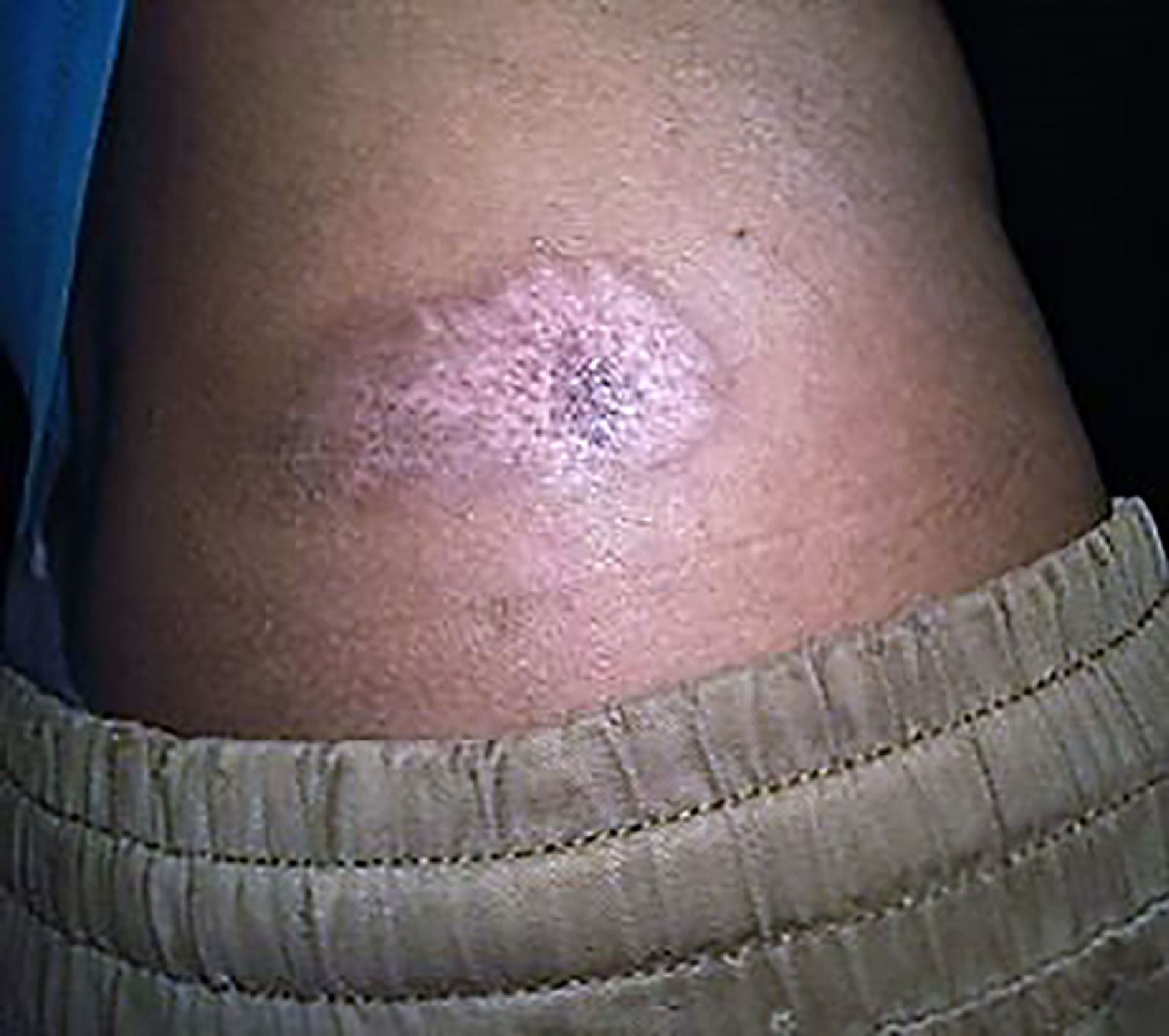
Blister at 2 mo.
Discussion
Friction blisters of the foot are a common problem associated with activities such as hiking, trekking, and climbing; they increase sweating and friction on the skin surface.6,7 Blisters are more common on the hands and feet than on other parts of the body. On the hands and feet, because of the increased thickness of the stratum corneum, surface shear forces result in differential movement of the upper and lower epidermal layers, causing a space to form. The space between the layers then becomes filled with fluid. 5 In contrast, elsewhere on the body, the stratum corneum is naturally thinner, and abrasions tend to occur rather than blisters as the top layer is rubbed off. 8
In addition to causing localized discomfort, friction blisters are susceptible to secondary infection. As patients with blisters of the foot alter their gait biomechanics to avoid pain, they can develop further injury.2,9 In a study of military trainees, 53% of those who developed friction blisters on the foot developed another overuse injury of the lower limb. The incidence of overuse injuries was significantly higher in those with friction blisters compared to those without. 2 Based on our experience at the clinic, we have observed that climbers will often continue to climb with foot blisters that have adequate dressings. However, the patient in this report discontinued climbing while the blister healed, principally because of the unusual location on the torso. He was able to return to climbing after 1 wk. The presence of the dressing at 1 wk did not affect his function and was helpful in preventing pain, according to the patient.
As far as the authors are aware, climbing harnesses have not been reported to cause blisters. Additionally, the literature review by the authors found articles discussing friction blisters of the feet but none describing blisters around the back and flank region. Guidelines exist for the management of foot blisters but not for blisters on other parts of the body. The Wilderness Medical Society wound care guidelines recommend that blisters larger than 5 mm should be drained but the roof left intact. The blister should then be covered with a hydrocolloid or hydrogel patch or equivalent, such as petrolatum or antibacterial ointment covered with gauze or moleskin. 4 A review of burn blisters recommended leaving blisters intact when possible to allow gradual absorption of blister fluid in an attempt to maximize healing and reduce patient discomfort. 3 Another study reported better outcomes in terms of healing and patient satisfaction with adhesive tape over fixation dressings in patients with foot blisters. 10 We agree with the Wilderness Medical Society guidelines that larger blisters are more likely to rupture spontaneously. We could not, however, find evidence in the available literature to support the 5 mm cutoff. In our patient the blister was at a location that would not affect his general mobility, and the injury occurred early in the season, so postponement of climbing was feasible. Therefore, we chose to manage the blister conservatively without drainage or deroofing. However, the blister ruptured spontaneously while the dressing was still intact and in place. We continued to adopt a conservative approach by keeping the roof intact, cleaning the wound with povidone iodine, and applying another dressing.
The climber was experienced with multiple previous successful summits of Mount Everest (8848 m). He developed a blister at an unusual site despite his extensive experience with harness use. The authors theorize that while the patient was climbing with the harness, he had not noticed displacement of his inside layer of clothing. The frictional force of the harness may have contributed to the formation of the blister at this unlikely location. It is also possible that the blister may have been caused by friction from his clothing, backpack, or other equipment.
One limitation of this report is that we do not know the exact mechanism by which he acquired the blister. Another limitation is that findings of an isolated case study may be difficult to generalize to other similar cases. Because we do not know the exact mechanism by which the patient acquired the blister, other differential diagnoses must be considered. Although it is possible that the patient may have sustained frostbite because of exposure to extreme cold, the torso is an unlikely location for frostbite. Insect and bedbug bites are unlikely in this cold, dry climate. Other dermatological conditions such as bullous fixed drug eruptions, epidermolysis bullosa, bullous tinea, and stasis bullae can be ruled out in this patient with an isolated nonhemorrhagic asymptomatic blister without a history of previous similar lesions, drug intake, or any other medical condition.
The lesson from this case is that even experienced climbers with knowledge of safety measures may sustain unusual injuries. Based on our experience, climbers are usually familiar with self-management of foot blisters and can often safely continue to climb with adequate dressing. However, blisters at unfamiliar locations raise safety concerns for the individual and the team by making it difficult for the climber to adhere to safe climbing techniques. If this patient had continued to climb without proper management of the blister, he would have felt uncomfortable in the climbing harness. That discomfort could have affected his performance, jeopardizing the safety of the entire team. Blisters at unusual locations require consultation with physicians familiar with the condition and its management.
Footnotes
Acknowledgments
We express our gratitude to Dr Buddha Basnyat for his assistance in manuscript write-up and invaluable comments to help finish the article. We express our gratitude to Dr Sarah Kemp for her contributions in editing and critical review of the manuscript for grammar and language.
Author Contributions: Study concept and design (SA); drafting of the manuscript (SA, JU); critical revision of the manuscript (SD); and approval of final manuscript (SA, SD, JU).
Financial/Material Support: None.
Disclosures: None.
