Abstract
This case report describes the use of a hydration bladder as an improvised air splint for a left forearm fracture in an austere environment. The literature regarding the use of air splints in the prehospital and wilderness environments is scarce, and it does not appear that this technique has been previously described in the literature. Given the widespread use of hydration bladders, the adjustable nature and overall comfort of the splint, and the anecdotal success of this technique without any complications or harm to the patient, the authors believe this is an important improvised splinting option to add to the quiver of any outdoor enthusiast or wilderness medical professional.
Introduction
Extremity injuries are common in many outdoor activities, and various improvised splinting techniques have been taught in wilderness courses and documented in the literature. Example techniques include the use of trekking poles, wooden sticks, foam sleeping pads, kayak paddles, and skis.1,2 Emergency medical services and search and rescue teams commonly carry medical equipment designed specifically for splinting, including flexible padded aluminum splits and air splints. In the austere and low-resource setting, these commercial products may not be readily available. In contrast, hydration bladders are common, readily available, and familiar to many outdoor enthusiasts.
The technique described in the following may be a useful improvised skill that is not currently documented in the literature or commonly taught in wilderness medicine courses. A wilderness care provider must be open minded and trained to use a multitude of materials to improvise a splint in an effective manner given a paucity of available resources.
Methods
A PubMed search was performed using the following keywords: “air splint,” “improvised splints,” “hydration bladder splint,” “improvised air splint,” “camelback splint,” “splint upper extremity improvised,” “air splint upper extremity,” and “improvised pneumatic splint.” In addition, well-known wilderness medicine texts were reviewed for any examples of hydration bladders being used as improvised air splints.1,2
Case
A 38-y-old woman riding a mountain bike had a fall at 8 km (5 mi) of a 16 km (10 mi) loop on the classic Slick Rock trail outside of Moab, UT, injuring her left wrist. There was an obvious distal forearm deformity concerning for a closed fracture. Given the surrounding environment of sandstone bedrock, dry dirt, and sparse low-lying plants, minimal natural materials were available to fashion an improvised splint (Figure 1). In addition, the group was traveling light for the mountain bike ride and had only basic first aid equipment. One of the group members, an author of this case report, was an emergency medicine physician and had undertaken additional training in wilderness medicine.

Two mountain bikers on the barren terrain, which has limited natural splinting material, outside Moab, UT. Photograph by Hans F. Hurt.
Given the nature of the injury and the obvious deformity, the patient required splinting and evacuation. An improvised splint needed to be fashioned because no formal splinting materials were available. In light of the surrounding environment, there were few options for providing splint rigidity: small sticks from the shrub bushes, small tube-style bike pumps, and bike seat posts. Options for appropriate splint padding were also limited because the weather was warm and the group members had minimal amounts of extra clothing available. Notably, all members had hydration bladders in their backpacks.
A forearm splint was created by placing an empty, deflated hydration bladder over the volar aspect of the hand and forearm. A jacket then was placed as padding on the dorsal aspect of the hand and forearm with the few available small sticks available as a rigid frame. Using 2.5 cm (1 in) silk tape from a first aid kit, the hydration bladder, padding, and sticks were secured around the hand, mid forearm, and upper forearm (Figure 2). With the hydration bladder and sticks secured in 3 places, the hydration bladder was inflated by blowing air into the bite valve until the bladder was firm enough to provide padding and support to the forearm with the tape connections sandwiching the injured wrist between the hydration bladder and the padded sticks (Figures 3–7). The bite valve mechanism was then locked, sealing the air in the bladder, and a sling was fashioned using another group member's jacket. The patient was able to adjust the hydration bladder air pressure for comfort by opening the locking mechanism and releasing or blowing air into the bladder. With the arm splinted, the patient was able to walk 3.2 km (2 mi) to an intersection with a motorized trail where she could be driven back to the parking lot. The patient was then transported to the local emergency department via personal vehicle.

The completed hydration bladder splint with a jacket as padding under the sticks, tape to secure the splint, and an additional jacket as a sling for support. Photograph by Hans F. Hurt.
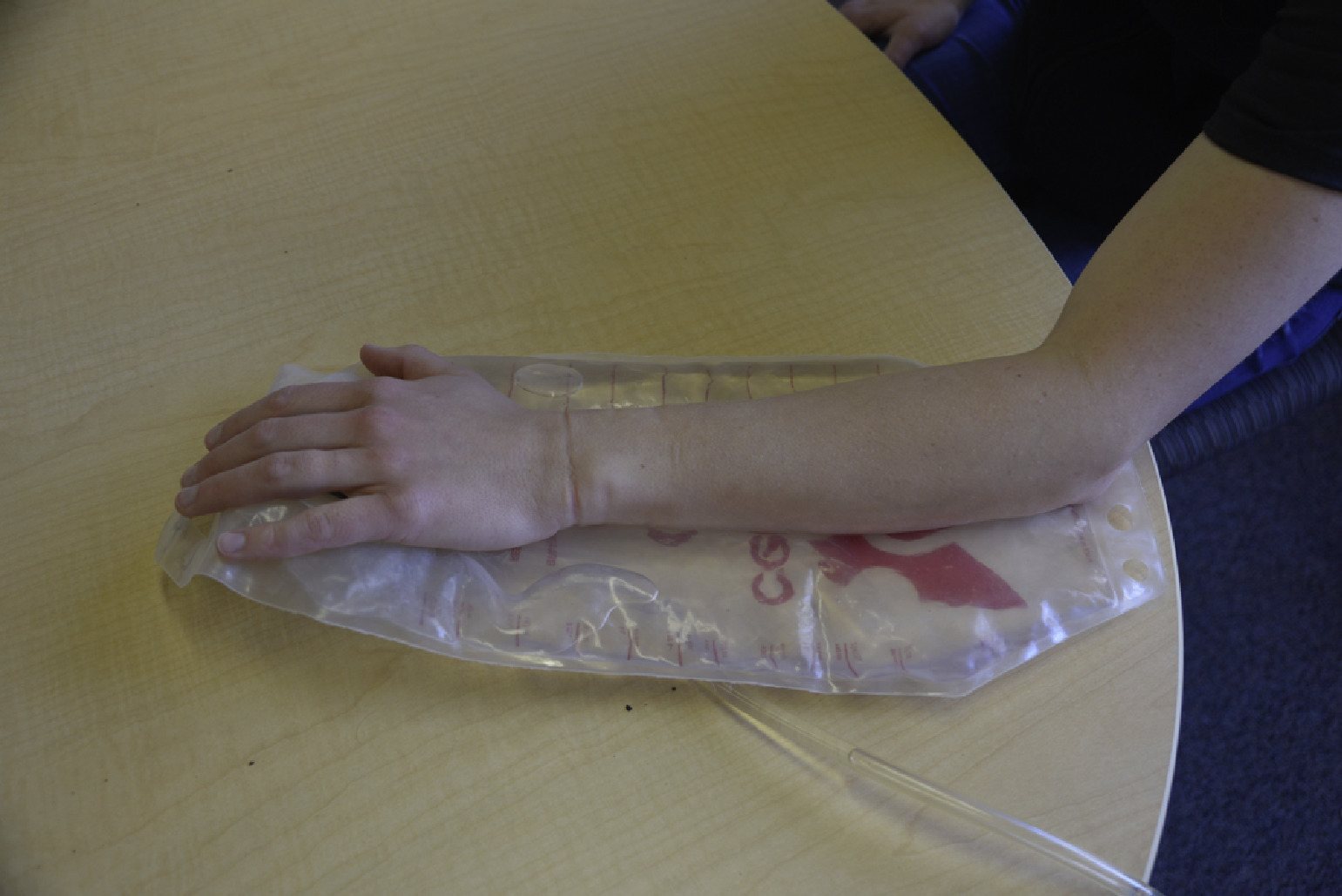
The arm was placed on a deflated hydration bladder. Photograph by Hans F. Hurt.

A jacket was placed as padding on the dorsal hand and forearm. Photograph by Hans F. Hurt.

A few small sticks were placed on top of the jacket to help stabilize the dorsal aspect of the splint. Photograph by Hans F. Hurt.
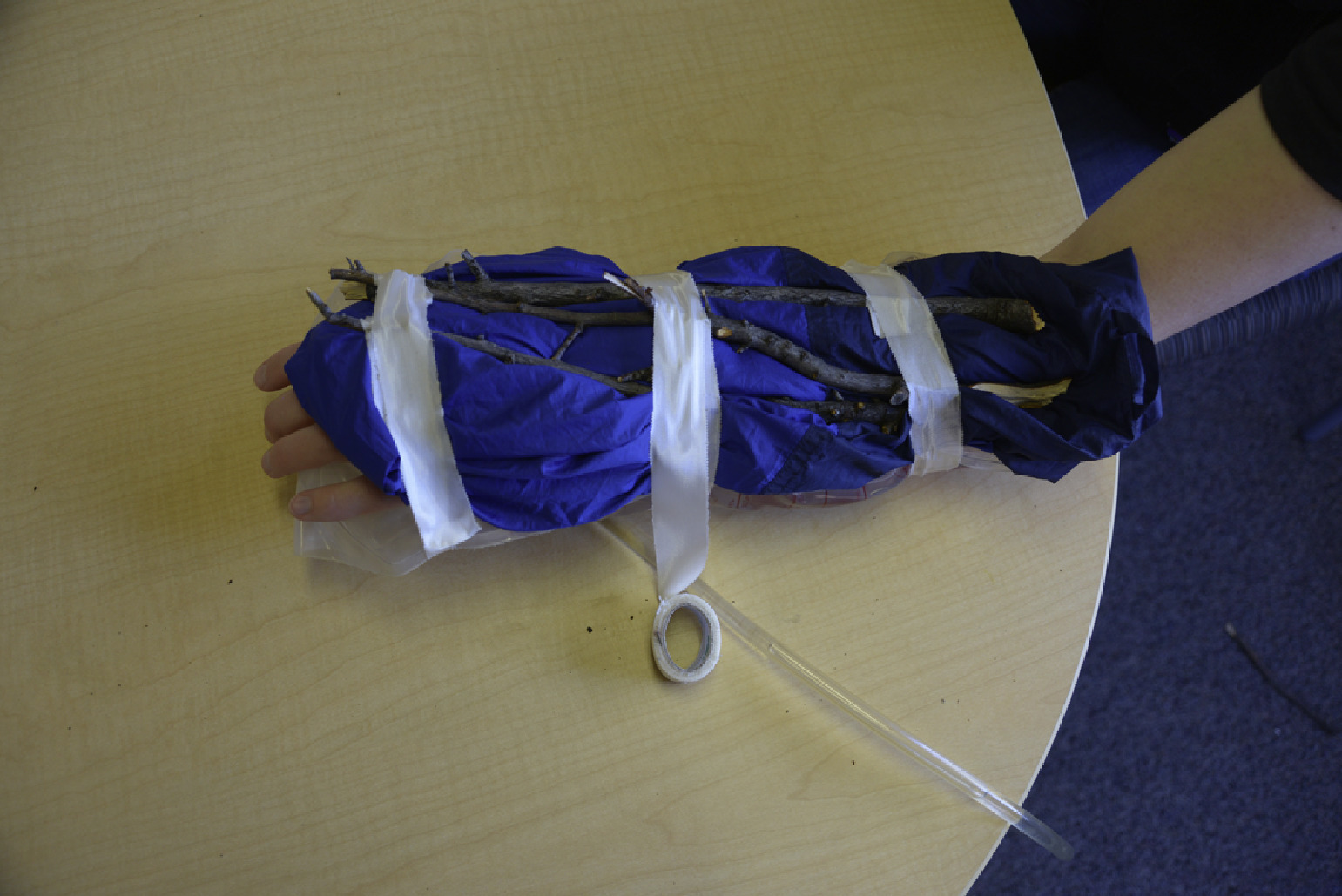
A 2.5 cm (1 in) silk tape was used to secure the pieces of the splint together in 3 places. Photograph by Hans F. Hurt.

Once the pieces were secured in place, the hydration bladder was inflated for comfort and support as guided by the patient. Photograph by Hans F. Hurt.
The hydration bladder splint was removed and radiographs were done, showing a distal radius fracture (Figure 8). The patient was then placed in a temporary moldable padded aluminum splint at the hospital after the radiographs were done. The patient noted that the new splint, made from a commercial splinting product, was very uncomfortable, to the point of requiring opioids for pain control. In comparison, the patient stated the hydration bladder splint had been much more comfortable during the 3 to 4 h it took to reach the hospital, without any need for pain medication.
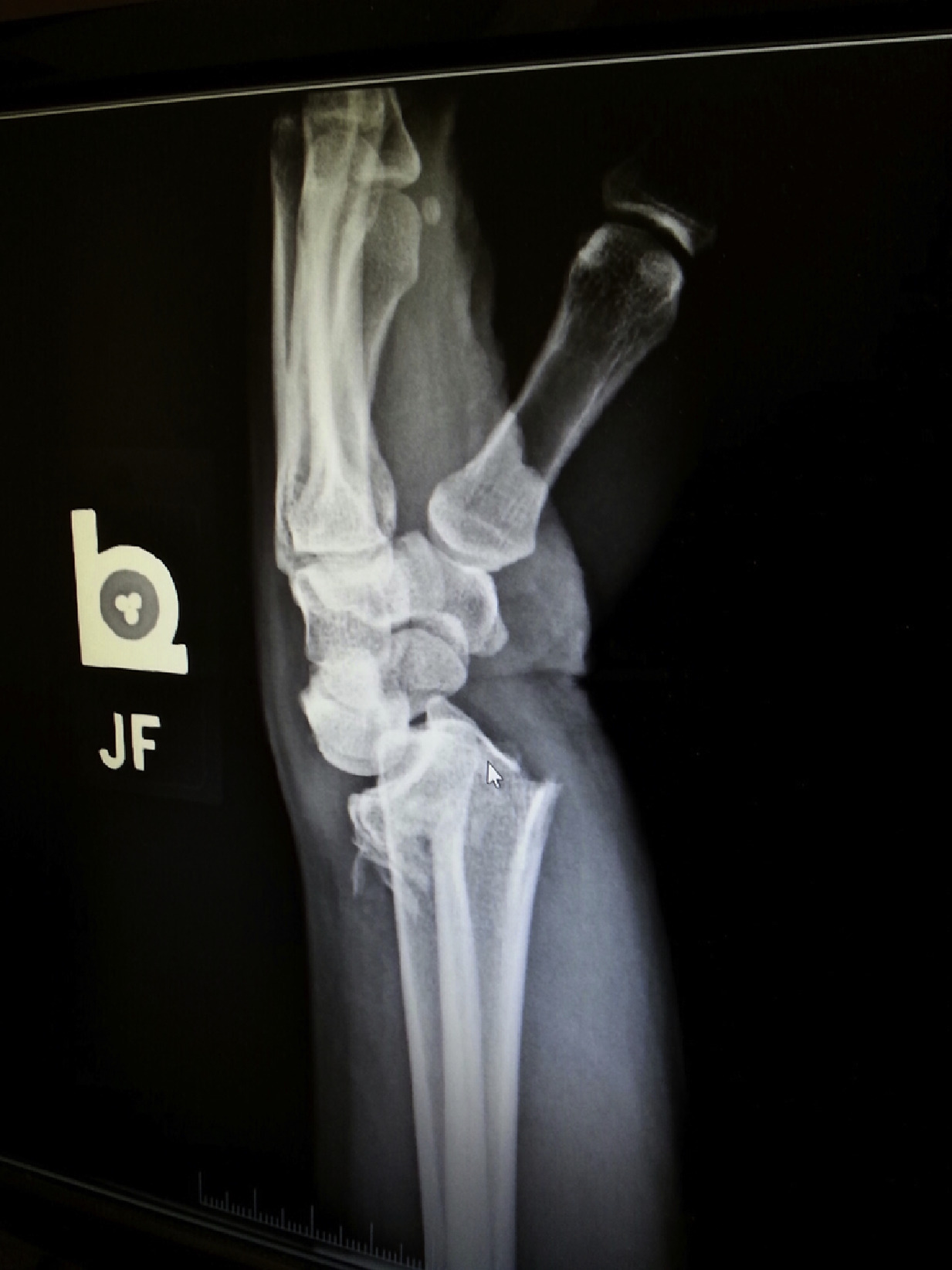
Radiograph demonstrating the patient's left distal radius fracture. Photograph by Hans F. Hurt.
Discussion
Hydration bladders are frequently used in many outdoor and athletic endeavors and are commonly available even when participants are traveling with minimal equipment. Although there are examples of pneumatic air splints dating back to 1944, no examples of improvised splints describing a hydration bladder as an effective way to improvise a splint were found in the current literature. 3 In this case of a forearm fracture, the patient reported that the splint was extremely comfortable when compared with a padded aluminum splint placed at the hospital. The hydration bladder splint could be easily adjusted by the patient with a single free hand and functioned for 3 to 4 h without causing any abrasions, tissue breakdown, or limb ischemia. The sticks were used to distribute the force of the tape that was used to secure the splint but may have aided in providing stability as well. When used without an additional rigid structure, the hydration bladder alone with an elastic wrap still provides stabilization that is likely adequate to reduce movement and pain, but because this was placed on a noninjured limb for the purpose of demonstration, the exact effect on an injured limb cannot be clarified (Figures 9 and 10).
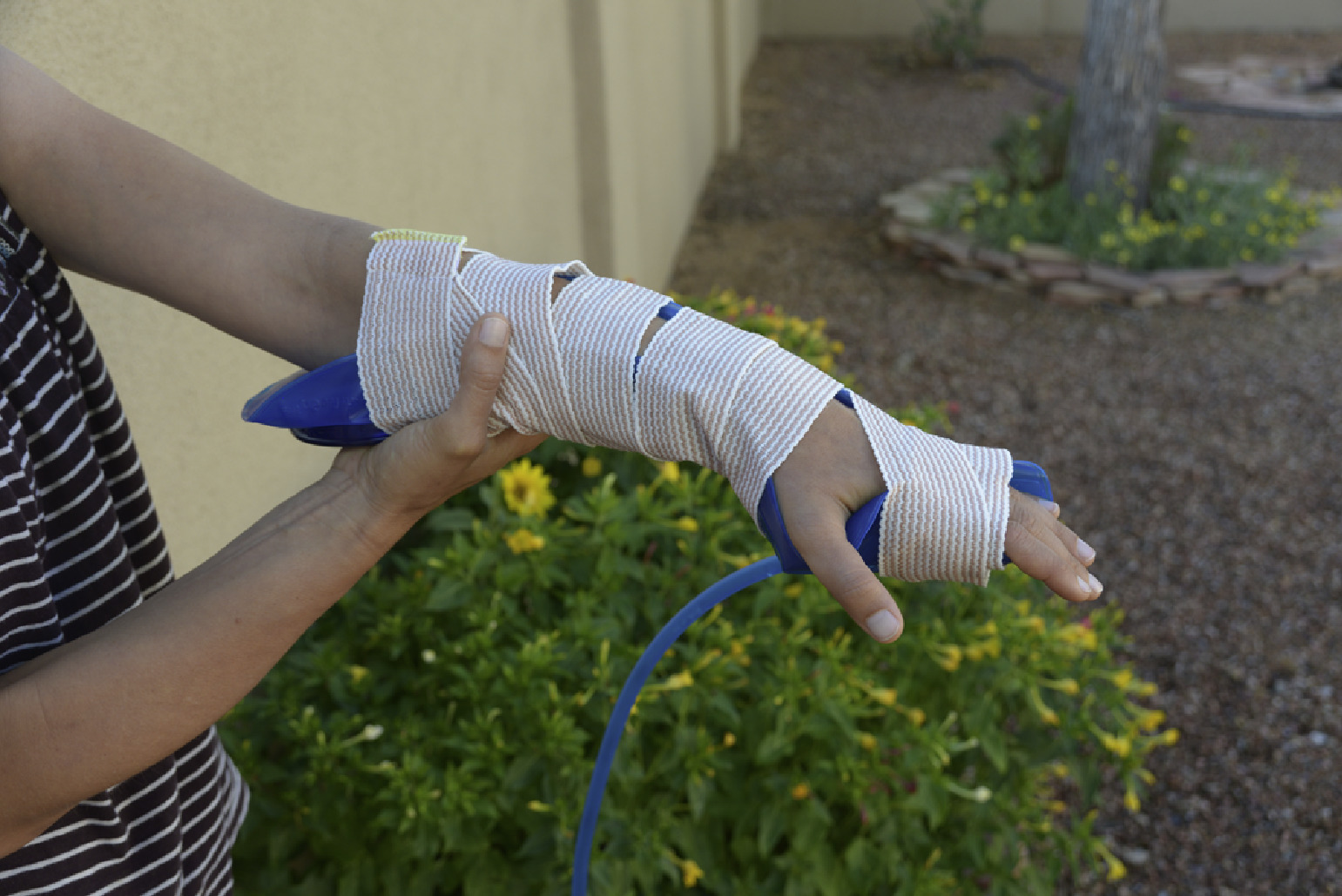
Hydration bladder with elastic wrap, not inflated. Photograph by Hans F. Hurt.
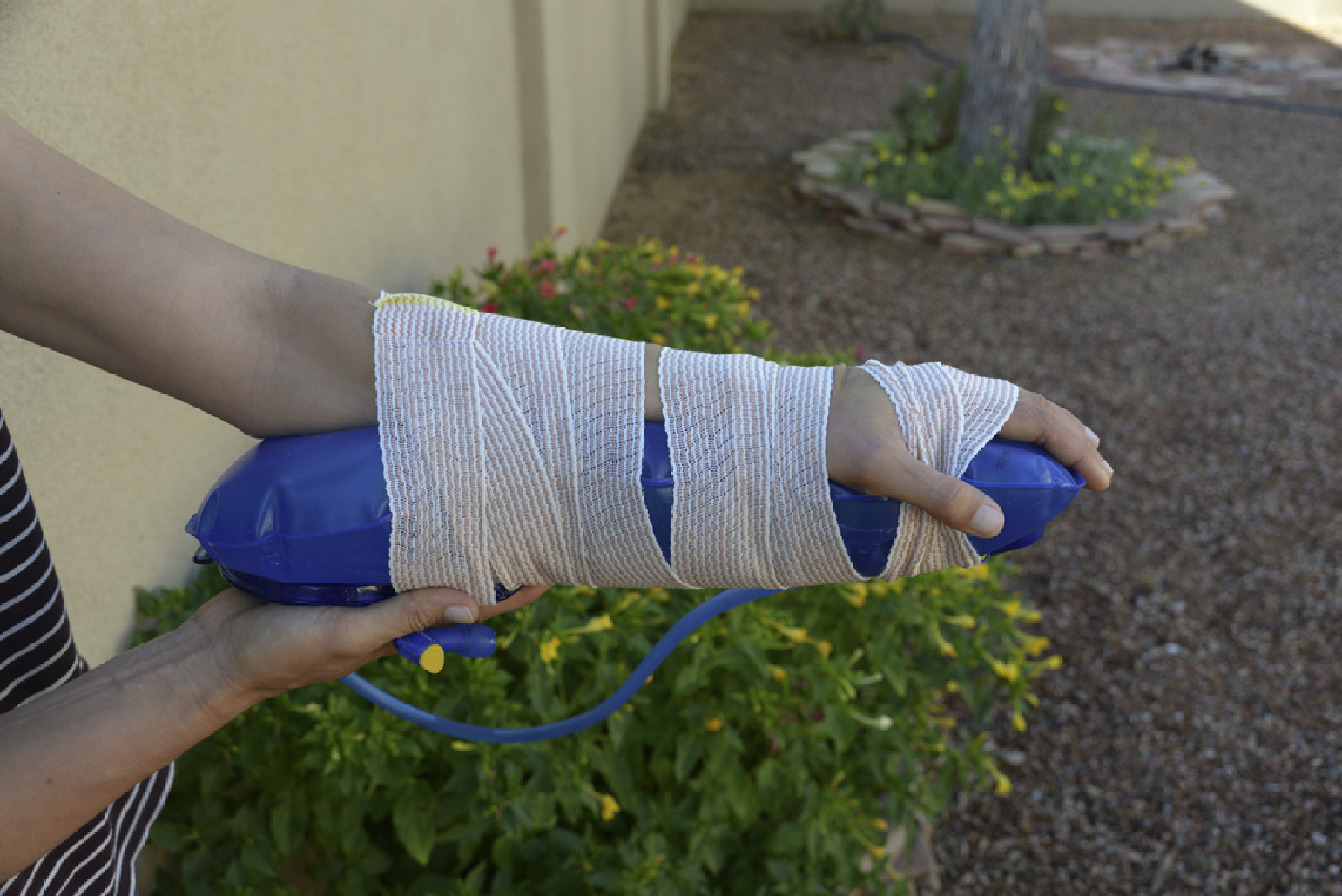
Hydration bladder with elastic wrap, inflated and providing stability without additional rigid structure. Photograph by Hans F. Hurt.
Commercial pneumatic air splints are documented in the literature since 1944 and are recommended to have 10 to 25 mm Hg of pressure to allow adequate blood flow.3,4 Oral inflation can achieve pressures up to 60 to 80 mm Hg, but if inflation is halted as slight resistance is felt and the material creases disappear, then pressures of 20 to 25 mm Hg can be obtained reliably.4,5 Caution is warranted because pressures above 25 to 30 mm Hg could lead to increased tissue pressure and ischemic damage.4,5
As with any splint, monitoring of distal circulation, sensation, and motor function is important. The height and width of a 2 to 3 L hydration bladder makes it ideal for splinting forearms, but if combined with a longer rigid structure and multiple hydration bladders, this technique could be adapted for larger extremity splints as well. The ease of adjusting the air pressure to comfort and stability via a bite valve makes for an ideal padding and support system around bony or soft tissue structures. A lock-off system behind the bite valve can be beneficial to seal the air at the desired pressure and minimize leakage. Interestingly, the authors of an article from 1984 could not find any documented complications from air splint use in the 20 y before the article's publication. 5 An additional possible use of the hydration bladder splint could be to optimize hemorrhage control or to optimize a pressure dressing for a severely bleeding wound without having to apply pressure by hand, allowing a rescuer to focus attention on evacuation or other injuries, as this has been documented with commercial inflatable splints. 6
Conclusion
The hydration bladder splint technique described can be adapted to many situations and may be a useful option for outdoor enthusiasts and medical personnel to add to their quiver of improvised splinting techniques. Caution is warranted because overinflation with high pressures could cause tissue ischemia, and periodic neurovascular examinations are warranted to avoid iatrogenic harm. Although air and gel splints are used for ankle sprains with little concern for tissue injury or ischemia, further studies could be performed to evaluate this theory of safety for air splints of the forearm. Wilderness medicine textbooks and outdoor medical courses should consider adding this technique in future editions and course curricula.
Footnotes
Acknowledgments
The authors thank the International Mountain Medicine Center and the University of New Mexico Department of Emergency Medicine for supporting their work in the field of wilderness medicine education. They also thank Jon Femling, MD, PhD, and Darryl Macias, MD, for their efforts in the review process.
Author Contributions: Drafted the manuscript (HH); contributed the photographs (HH); critical revisions of the manuscript (HH, AR); approval of the final manuscript (HH, AR).
Financial/Material Support: None.
Disclosures: None.
