Abstract
Wild animal attacks are potential occurrences in rural areas of Turkey. Wolf attacks, however, are rare this century, but there are many anecdotal reports from previous times. Attacks by wolves are generally directed against animals, such as cows and sheep, and for feeding purposes. Wolf attacks on humans are a little known and unexpected phenomenon. A 60-year-old man was brought to the emergency department with facial injuries caused by a wolf emerging from a rural area and leaping at his face as he was sitting in his garden. During the incident, the patient strangled the wolf to death. Despite postexposure prophylaxis the patient likely died because of rabies.
Keywords
Introduction
Wild animal attacks are sometimes reported from rural areas of Turkey. Wolf attacks, however, are rare. An increase in instances of animal attacks on pets and humans indicates humans are encroaching on wild animals' habitats. This increase may also to some extent be associated with the unbalanced and uncontrolled breeding of animals that have been made the subjects of hunting bans. Rabies represents the most feared potential complication from animal bites. Rabies is a viral zoonosis that leads to fatal encephalitis in humans and other mammals. Most infections in humans originate from dogs, and the World Health Organization estimates that some 55 000 humans die of rabies every year. 1 A total of 247 human rabies patients were reported in Turkey between 1980 and 2006, for an average of 9.5 cases per year. Rabies postexposure prophylaxis was administered to 143 915 persons (218.7/100 000 population) in 2006, as reported by the Turkish Ministry of Health. 2 This report describes a patient who was admitted to the emergency department after an attack by a wild wolf, returning to the emergency department with a diagnosis of rabies despite being administered appropriate treatment, and dying 1 day later.
Case Report
A 60-year-old man was brought to the emergency department with facial injuries caused by a wolf attack as he was sitting in his garden. When the history of the case was taken, it was established that the wolf had bitten the patient's face and that he had strangled it to death. On arrival he was conscious, oriented, and cooperative, and his vital findings were stable. Physical examination revealed an oblique laceration of the face, approximately 5 cm in length, full-thickness as far as the mucosa, starting from the right oral commissure and extending laterally, and with irregular edges. There was a 0.5-cm vermillion defect at the right lateral commissure and a 1-cm skin cut at the left lateral commissure (Figure). The facial artery was exposed, and was thrombosed proximally. Facial nerve and sensation examination was normal. The patient was administered tetanus vaccine, tetanus immunoglobulin, rabies vaccine (human diploid cell vaccine: HDCV) 1.0 mL to the deltoid area, and rabies immunoglobulin (human rabies immunoglobulin: HRIG) 20 IU/kg around the wounds 2 hours after the attack. The lacerations were irrigated with saline and povidone-iodine solution for 15 minutes and sutured with the application of rabies immunoglobulin to the wound edges. The patient was given oral antibiotics (amoxicillin-clavulanate) and discharged. Vaccinations were performed on days 3 and 7 after discharge. Examination of the dead wolf's brain tissue revealed Negri bodies. The patient's vaccination program was continued. The patient was again vaccinated on day 14, but was brought back to the emergency department on day 25 with blurred consciousness. He had a Glasgow Coma Scale score (E3V4M6) of 13 and an oral temperature of 38.5°C, as well as increased salivation. Rabies was suspected. Respiratory difficulty developed 24 hours later. Endotracheal intubation was performed, and cardiac arrest occurred 4 hours later. Rabies was confirmed with autopsy and brain biopsy.
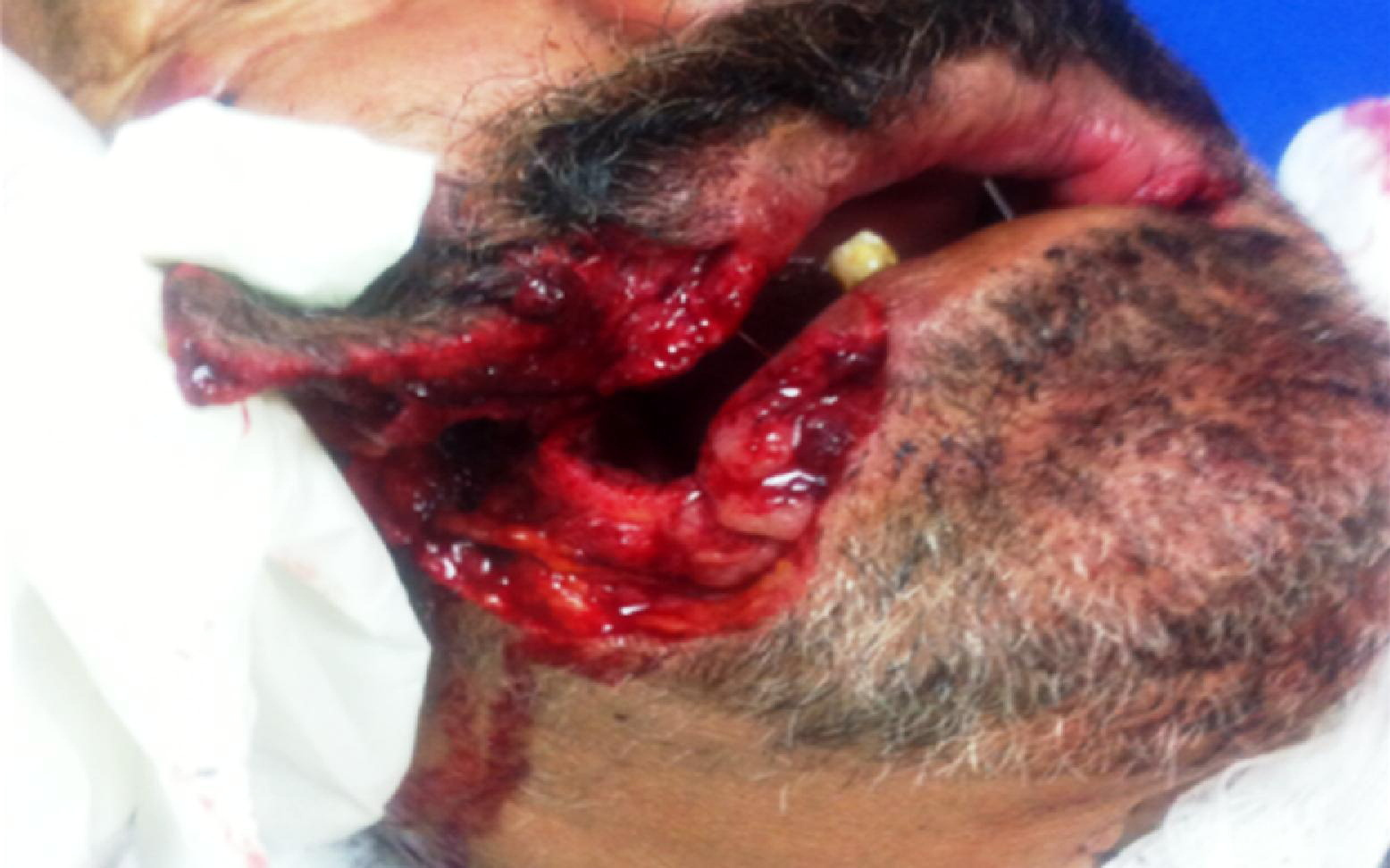
Photograph of facial wound resulting from a wild wolf bite.
Discussion
Most emergency department visits related to rabies are caused by dogs, especially in developing countries. Such injuries may give rise to local wound infections, and also to systemic complications such as lymphangitis, local abscess, septic arthritis, tenosynovitis and osteomyelitis or endocarditis, meningitis, brain abscess, or sepsis with disseminated intravascular coagulation.3,4
Rabies is a fatal disease, although death is preventable. Rabies-associated deaths mainly occur in Asia and Africa, where animal control, vaccination programs, and effective postexposure prophylaxis for humans are not widely available. In developed countries, rabies is largely found in wild animal hosts. In those parts of the world rabies passes directly from wild animals such as raccoons, foxes, skunks, and bats to humans without passing through a domestic animal.5,6 The incubation period in humans ranges from 5 days to 1 year, with an average of 1 to 2 months. The length of incubation decreases if the bite is on the head or neck. The patient in this report was injured in the facial region, and in spite of postexposure prophylaxis, rabies symptoms appeared some 26 days later. In this case postexposure prophylaxis likely did not work because of the location of the wound.
Symptoms in rabies are usually typical. The disease generally begins with mental depression, restlessness, aches, fever, lack of appetite, and sensory changes around the bite site. After this prodromal period, the patient develops an acute neurologic phase. The acute neurologic phase has 2 forms: furious and paralytic. The furious form is the most seen presentation. Hyperactivity, disorientation, hallucinations, bizarre behavior, and autonomic dysfunction may occur. Confusion, lethargy, and increased salivary gland secretion appear within a few days. Attempts to drink fluids result in severe spasms in the pharynx, larynx, and diaphragm and are known as hydrophobia. Half of patients may have hydrophobia. The paralytic rabies form is noted in 20% of patients. Paralysis is symmetric and diffuse. Fever and nuchal rigidity may accompany this form.7,8
Rabies is still a global threat, despite widespread vaccination programs for domestic pets. As the disease is generally fatal, rabies postexposure prophylaxis (RPEP) should be considered for all victims of unprovoked dog and cat bites. Ten-day quarantine periods have only been established for dogs, cats, and ferrets, and quarantine for rabies is not appropriate for any other species. When animal quarantine is appropriate, victim prophylaxis may not be necessary, but should be initiated at the first clinical sign of the disease in the quarantined animal. 9 If the animal is a dog or a cat and has escaped, initiation of RPEP should be based on the local epidemiology of rabies. Bites from any wild animal can potentially pose a risk of rabies to humans, depending on the level of rabies transmission in local wildlife populations. When wild animals are not available to be tested for rabies, immediate RPEP should be given. 10
Two other conditions as well as rabies should be borne in mind in wild animal or domestic pet bites, and prophylaxis for these should not be neglected. These are local wound infections and tetanus infections. Antibiotic prophylaxis is important in such injuries. All cat, human, or monkey bites, deep dog bite puncture wounds, hand or foot wounds, bites in immunosuppressed patients, and any injury undergoing surgical repair have a high risk for infections, and these wounds require prophylactic antibiotics. When antimicrobial prophylaxis is considered worthwhile, the empiric regimen should primarily be active against Staphylococcus aureus, streptococci, Haemophilus species, anaerobes, and Pasteurella multocida (in canine and especially feline bites) or Eikenella corrodens (in human bites, and especially clenched-fist injuries). First-line antibiotic agents recommended in wild animal bites are amoxicillin-clavulanate or cefoxitin/cefotetan. Alternative therapy of clindamycin plus either fluoroquinolone or trimethoprim-sulfamethoxazole is also recommended.9,11
All bites are regarded as tetanus-prone injuries. Standard treatment includes the administration of tetanus toxoid if no booster injection has been given during the preceding 5 years. Tetanus immunoglobulin should be given if the victim's immunization status is unknown, or if fewer than 3 doses of adsorbed tetanus toxoid have been administered. 12
Wild animal attacks on humans are encountered only infrequently. Research shows 3 underlying reasons for wolf attacks: the wolf may be rabid, it may regard human beings as prey, or, third, the attack may have been provoked by a human. 13 Rabies was investigated in the wolf strangled to death by our patient during the attack, and the animal was confirmed as rabid.
Wolves and human beings seldom interact, although tragic incidents may sometimes occur. A wild wolf attacking a human sitting in his garden and the human suffering lacerations to the face is a very rare phenomenon. There are no previous reports of a wolf being strangled to death by the human involved. The attacking wolf being rabid, and the injured patient also contracting rabies despite being given appropriate treatment is again an unexpected tragic outcome. Wound cleaning in wild animal attacks of this kind must be performed very accurately; the possibility that the animal may be rabid must be borne in mind, and both tetanus and rabies prophylaxis must be administered without delay.14,15 In addition, antibiotic prophylaxis must not be forgotten.
Rabies continues to represent a significant public health problem in developing countries. Wild animal attacks, as with all attacks by uncontrolled mammals, continue to bear a risk of rabies in such countries. Unexpected attacks by wild animals in particular should raise serious suspicions of rabies. In addition to other attendant dimensions, in the presence of such injuries the physician caring for the patient must absolutely consider the possibility of the animal concerned being rabid. Domesticated animals (especially dogs, cats, and ferrets) should be vaccinated to prevent them from becoming infected and transmitting rabies to humans. Wild animals should not be handled; wildlife behaving abnormally should particularly be avoided. Bats should be kept out of houses and public buildings.
Footnotes
Conflict of Interest: None
