Abstract

The stark reality of hospital economics is undeniable today. Hospital administrators are justifiably concerned about the flow of resources, technology, and human capital that can shake the very foundations of the health care system. Among the many variables that can affect the efficacy of the health care environment, three in particular are prompting dramatic changes to clinical laboratory processes—and greater demand for automation:
The labor shortage: Staff vacancies are at a 12-year high, and job shortage rates range from 7 to 20%. An estimated 8000 vacant positions are generated annually. 1 The average lab tech is in his, or her, late forties, so the labor pool is both dwindling and aging. Laboratories must take steps to adopt new processes and systems to offset the labor shortage.
Medical errors and patient safety: According to the Institute of Medicine (IOM), medical errors lead to as many as 98,000 deaths and 1 million injuries per year in the United States. 2 Laboratory test results are an important determinant of a doctor's clinical decision in treating a patient, so quick turnaround time and accurate diagnostic results are vitally important. In fact, the laboratory provides as much as 80% of the information used by physicians to make important medical decisions. Laboratories are obligated to provide the right test for the right patient at the right time.
Length of stay: A hospital's economic well-being is contingent on positive patient outcomes and low length of stay. The sooner a laboratory provides physicians with valuable patient test results, the sooner physicians can diagnose and treat their patients. That, in turn, can mean a shorter patient length of stay and have an immense impact on a hospital budget. Laboratories must provide physicians with fast, accurate test results and decrease variability in test turnaround time to help lower patient length of stay.
These three change agents do not operate in a vacuum. A shortage of labor affects a laboratory's ability to meet physician demands for fast, accurate test results, which can affect patient safety and in turn result in an increased patient length of stay—all to the detriment of a hospital's bottom line.
Fortunately, laboratories have a powerful solution available to them in the form of automation—a tool that can be used to help the laboratory contribute to a hospital's economic viability. In rethinking the tenets of lab operations, a new archetype can emerge that serves economic imperatives without sacrificing our responsibilities for improved patient care.
The Road to Automation
It is a myth that only high-volume labs are fit for automation. Baptist Hospital of East Tennessee is a 349-bed community hospital in Knoxville, Tennessee. Since implementing automation in 2000, we have mitigated the effect of the growing labor shortage as well as helped reduce medical errors and improve patient safety. We also believe these improvements have had a positive impact on patient length of stay.
But the journey to automation did not begin overnight. It actually began several years ago in 1997 when we took steps to implement new processes and take advantage of advances in lab automation. Changing work processes was the initial focus. Like many laboratories, we were overwhelmed with increased demands for greater test volume and the need for faster, standardized test turnaround time. The lack of qualified technologists only added to our dilemma.
Simply put, manual processes were hurting our ability to perform optimally. The primary goal of our lab was the elimination of manual steps or “touches” a sample gets while being processed. The more touches, the more time it takes and the more opportunity for variability and human error. Eliminating these manual touches can be achieved through a variety of methods, spanning from traditional workstation consolidation to comprehensive automation. Regardless of the approach, automating processes helps the lab decrease variability while increasing quality and consistency.
In our mission to change work processes, three goals guided our project: (1) move the lab into a core lab or open lab environment; (2) consolidate workstations, and (3) make use of preanalytical robotic automation. After all, we were well aware that software enhancements and workstation consolidation were powerful tools of change that made a cleaner, more effective work environment.
But that quest for process improvement, in which automation was to play such a significant role, required one critical component: executive and senior management support. With that in mind, one of the first things we did was open a dialogue with executive and senior staff to let them know about the issues facing the lab and other health care departments. We also explained the tools that were needed to move forward.
Not surprisingly, one of the main issues administrators are dealing with at the executive level is not all that different from the main issue faced at the lab level: costs. Consequently, in our dialogue, we concentrated on cost improvements as well as opportunities for increased operational efficiencies and improvements in patient safety. This acknowledgment of “common ground” generated the support we needed to investigate improvement options—and put together a plan of action.
The plan of action was based on an analysis of work processes such as current performance, identification of specific processes that lead to potential errors and devising specific ways to reduce manual processes, decrease test turnaround time, and improve overall performance. We also took an in-depth look at the exact source of variability of patient test results, including sample arrival cycles, processing time, error tracking, resource availability, and the delivery of those test results.
This is crucial, because variability can have a profound impact on patient length of stay. For example, in a recent pilot study at a university health system, researchers examined the medical center's best practices with regard to patient length of stay. 3 Researchers determined that the hospital-wide average departure time was 3 p.m. They then implemented changes in specific pilot units to improve test turnaround times. This resulted in an average departure time of 11:45 a.m. among those pilot units—a savings of 3.25 h. Clearly, reengineering processes that improve test turnaround times supports a shorter patient length of stay.
Using these types of analyses, labs have the information they need to justify the investment in automation and other process improvement tools. Our lab installed automation in July 2000 and is equipped with a Power Processor automation system and two SYNCHRON LX®20 clinical systems (Beckman Coulter, Fullerton, CA) for general chemistry testing. The Power Processor allows our lab to automate sample centrifugation, cap removal and sample sorting. This allows our staff to focus on work that requires critical analysis, such as interpreting patient test results.
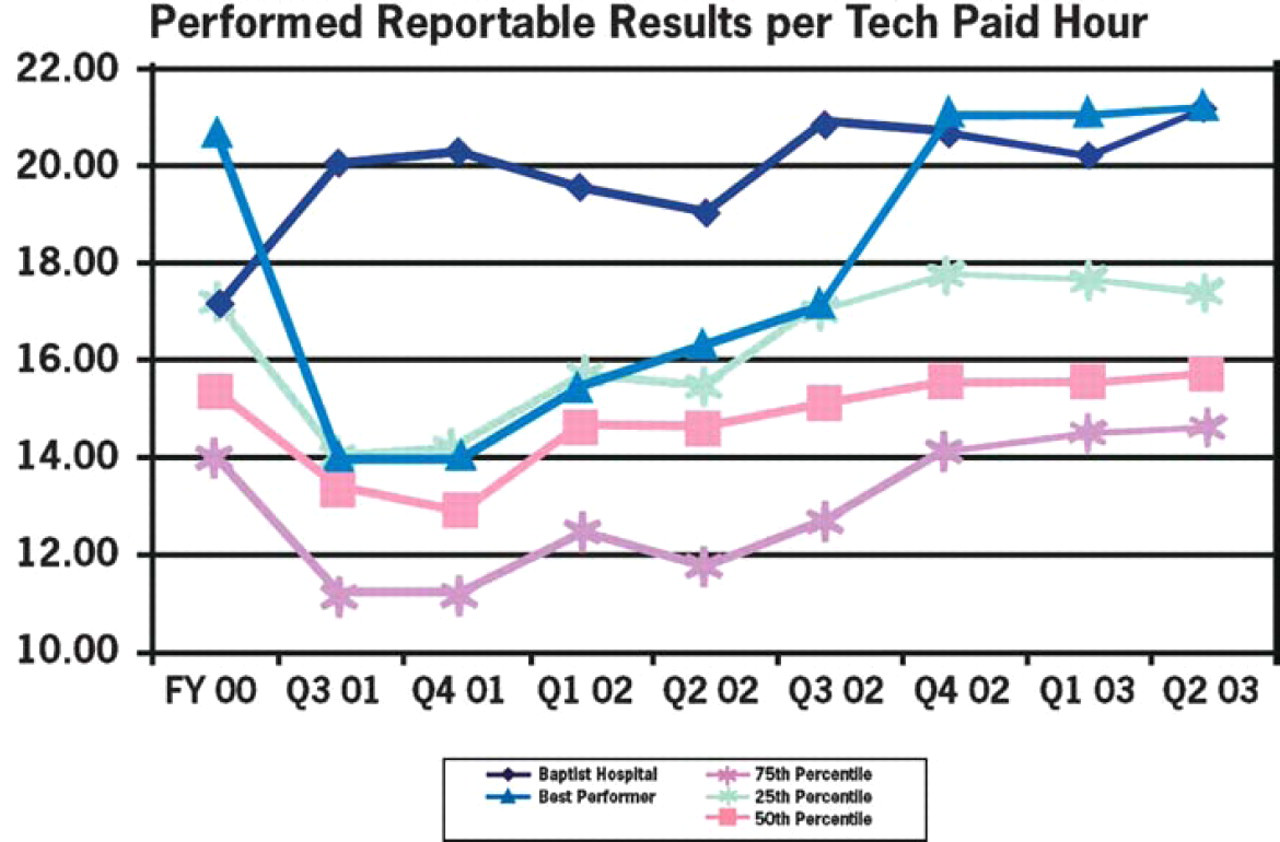
Performed reportable results per technical paid hour. A national benchmarking study involving up to 25 laboratories from 2001 through 2003 indicates that Baptist Hospital of East Tennessee was a leading performer in technical productivity.
After adopting these automation technologies and improved processes, we continued to monitor and evaluate our progress in lab improvements. To this day, we continuously look at total expense per performed reportable result as well as total cost per performed reportable result. We also track other information, such as technical productivity and consistently across multiple quarters (Figure 1). This method helps us not only illustrate our improvements in productivity, but also improvements in costs.
Automation Boosts Accuracy, Efficiency
After automating the pre-analytical process, we successfully standardized the work environment and put more time back into the hands of our technologists, so they were not making as many errors. For example, in our hospital-based clinical laboratory, we process approximately 1200 tubes a day. Once we calculated the economic impact of the changes to our preanalytical processes, we were astounded. We had eliminated 7 out of 14 manual processing steps. If you consider the seven steps that were eliminated multiplied by the 1200 tubes a day, the result is 8,400 manual processing steps eliminated daily. Multiply that by 365 days per year, and the result is more than 3 million manual steps eliminated annually.
Automating processes also helped us isolate and significantly reduce the problems that lead to misidentification of patient samples, the likelihood of performing the wrong test on the wrong patient, and other errors. Whenever there are repetitive, manual procedures, there is always a risk of human error, and this often occurs in the preanalytical stage of sample testing. However, with automation, many of these manual, error-prone steps are no longer required. Thus, you can eliminate the opportunity for error.
At Baptist Hospital of East Tennessee, we reduced manual handling of samples by 50%, thereby reducing manual process variances that contribute to errors. Process variations, such as failure to document the calling of a medical alert value or having to issue a corrected report, were reduced by up to 68% (Table 1).
Reduction in lab variances

It is estimated that medical errors contribute $17 billion to $29 billion in added costs to our health care system every year. 2 According to the IOM, diagnostic mistakes are identified as a key source of medical errors. Automating pre- and post-analytical tasks—which is where most errors in the lab occur—can play a significant role in the reduction of medical errors and in the improvement of patient safety.
Meanwhile, relabeling has been diminished or eliminated. The establishment of a database, and the monitoring of database elements such as stat turnaround times and lab errors, were instituted. We also eliminated about 90% of our aliquotting, another area of opportunity for errors.
In addition, through interaction between our laboratory information system and our analytical analyzers, we now auto-validate our results, which significantly affects patient safety. For instance, before we began auto-validating, every sample had to be manually reviewed at a workstation. Now, 80 to 85% of samples are auto-validated, and the results are released automatically. This has dropped turnaround time on five of our most frequent tests from 49.2 to 18.9 min, an improvement of more than 60%. More importantly, at the 90th percentile, our test turnaround times on the same test mix were reduced from 72.2 to 33 min, a 55% improvement (Table 2).
Stat test statistics

The open lab design makes it possible for us to process nearly all of our work in one space instead of passing it around the hospital from one specialty lab to another. Reducing manual handling of samples reduces opportunities for error. And, all of our design elements have worked together to help improve turnaround time, a key component of lowering patient length of stay as well as supporting efforts to improve patient safety.
While these advancements have improved patient safety, they have also helped our hospital's bottom line. Thanks to our automated workplace, we were able to slash $340,000 in personnel costs through the reduction of 11.2 FTEs (full-time equivalents), since we no longer require manual processing of most samples. The monetary value of eliminating manual processing steps in our laboratory was $0.10 to $0.11 per step. Overall, laboratory process automation has resulted in a 7% reduction in total cost per total reportable result. Year-to-year savings of this nature add up, and the impact on a hospital's profit-and-loss statement is obvious.
Direct Cost Savings While Offsetting the Labor Shortage
But automation has done more than make the lab a more cost-effective health care department. The elimination of manual processes has become a powerful employment benefit that we tout when recruiting lab personnel—and that has also helped offset the labor shortage. Indeed, our automated lab has helped us recruit and retain top medical technologists who want to work in a safer, more high-tech environment.
New demands for higher productivity are coming at a time when there is a critical shortage of lab technologists. Qualified laboratory technologists will naturally migrate to hospitals that allow them to concentrate on the tasks they do best: analyze patient test results. Automation takes over the most tedious and labor-intensive processes. The less tedious work one has to do, the more attractive the job will be. Recently, two medical technologists resigned their positions to take jobs elsewhere at a higher dollar rate. However, within two weeks of resigning, they withdrew their resignations because they preferred working in our high-tech environment.
Our lab is now a safer place because a standardized workflow using automation helps mitigate risks. In an age of HIV, hepatitis, and other bloodborne pathogens, the issue of safety is on every health care professional's mind. Automation means that tubes are handled less frequently. Technologists have less chance of a sharps injury or splash from opening a sample tube. Consequently, in the lab at Baptist Hospital, exposure to biohazards such as splashed or spilled samples or broken test tubes has been reduced 25%.
New Frontiers
These examples illustrate the return on investment realized when Baptist Hospital redesigned its lab. New technology created a “work-smart” environment, enabling our lab to do more with less.
Thus, using automation as a tool is in alignment with administration's goal of offering superior health care while reducing costs. For physicians and other health care professionals, it means more accurate test results with faster and less variable turnaround times. For laboratory personnel, it means a more standardized and work-friendly environment. For patients, it means less chance of medical errors and improved patient safety. And, for the medical profession as a whole, it means that laboratories can play a significant role when it comes to offering better patient care at optimal efficiency.
