Abstract
Abstract
Background
Assessment of lower extremity (LE) torsional profile using computed tomography (CT) imaging is a well-recognized imaging method that supplements the clinical examination. Magnetic resonance imaging (MRI) is another advanced imaging modality that can be used as an alternative, since there are many growing concerns of radiation exposure with traditional CT studies, particularly in the skeletally immature population.
Methods
Sixty-two patients between the ages of 7 and 19 years were included. Thirty-four had CT and 28 had MRI for assessment of LE torsional profile. All patients had clinical evidence of torsional malalignment. CT and MR images were randomized and de-identified. Two observers measured femoral anteversion and tibial torsion based on previously published methodologies. This exercise was repeated 2 weeks later and the data were tabulated and statistical analysis was performed. Radiation exposure for the patients studied by CT was estimated.
Results
The mean age of the patients was 14.4 years (range 9.5–18.9 years) and 13.8 years (range 7.3–18.9 years) for the CT and MRI groups, respectively. Inter-observer reliability for both CT and MRI studies were excellent. The intra-class correlation coefficient (ICC) for femoral anteversion and tibial torsion studied by CT and MRI for both observers at both times were excellent. The radiation exposure for CT examination averaged 0.3–0.5 mSv, compared to none with the MRI method.
Conclusions
MRI provides a reproducible method for assessing the torsional profile in children and adolescents using similar anatomic landmarks for measurements as those used on CT torsional profile. In circumstances where MRI methods are readily available (and affordable), the CT torsional profile can be replaced with MRI methods, in the current era of growing concerns of radiation hazards and increasing awareness about radiation safety.
Level of evidence
Diagnostic Level III.
Introduction
Torsional malalignment of lower extremities (LE) remains a common clinical problem in children and adolescents. Its spectrum of presentation varies from asymptomatic in-toeing gait at one end, to symptomatic gait abnormality and eventual severe symptoms related to prolonged compensation of foot and ankle pain, patellar pain and instability, and occasionally hip pain at the other end [1–3].
Traditional evaluation of torsional profile is via a thorough clinical examination to evaluate both the static and dynamic components. Torsional malalignment is common in both the idiopathic situation as well as neuro-muscular conditions such as cerebral palsy. Physical examination for determining femoral anteversion and the neck–shaft angle as measured on the internal rotation radiograph of the hips has been proved to be a clinically relevant method for evaluating the proximal femoral geometry and version in patients with cerebral palsy, and the results are as reliable as those obtained by computed tomography (CT) [4]. The radiological modalities to evaluate torsion include plain radiography [5–9], ultrasound [10, 11], CT [12–18], and magnetic resonance imaging (MRI) [18–21].
Subsequent to their initial usage for torsional assessment in the 1970s, CT scans quickly became the most common modality for the radiographic assessment of torsional profile. Although high-speed CT scanners allow studies to be performed with minimal radiation, in the current era of heightened awareness of radiation safety related to diagnostic imaging, many parents and physicians may seek, or insist on, other potential options when considering diagnostic assessment, while not compromising on the quality of data and information obtained [22–24].
Based on these considerations, we began to use MRI for the assessment of torsional profile in children and adolescents in our hospital over the past 3 years. We conducted this retrospective review to answer the following questions: (1) is it possible to obtain enough information from the MRI torsional profile to assess the degree of LE torsional malalignment in children and adolescents? and, (2) are MRI measurements reproducible?
Methods
Following Institutional Review Board (IRB) approval, electronic medical records were used to identify 61 patients as having either an MRI or CT evaluation of LE torsional malalignment. Thirty-two patients were evaluated via CT scan and 29 patients were evaluated with an MRI between January 2010 and March 2011. All patients included in this study had a clinical examination in their orthopedic consultation that identified the presence and severity of torsional malalignment, including contributions from the thigh (femur), leg (tibia–fibula), and ankle–foot complex. We excluded patients who had a past history of surgical intervention that could potentially distort the morphology of the femur/tibia.
Following patient selection, one investigator de-identified and randomized all examinations and printed them on paper. The methodology of measuring the torsional profile was reviewed by the entire group and landmarks to be utilized were agreed upon. Previously published methods for assessing torsional profile from Weiner et al. [12] and Jakob et al. [13] were used in this study. Two board-certified, fellowship-trained orthopedic surgeons then completed the first set of readings on all images. They drew necessary lines to measure LE torsion at the proximal femur, distal femur, proximal tibia, and distal tibia. A third investigator (orthopedic, non-physician, MPH researcher) independently measured and recorded all angles.
Femoral anteversion and tibial torsion were then calculated and corroborated with the clinical documentation of increased femoral anteversion with or without internal torsion of the tibia. One week later, the radiographic examinations were randomized and the entire exercise was repeated, thereby, allowing for intra-observer comparisons.
Clinical examination
Clinical examination was performed in all patients in sitting, supine, prone, and standing positions and while walking. Findings noted on clinical examination included: internal and external rotation of the hip in sitting position, assessment of tibio-fibular torsion, thigh–foot axis measurement, assessment of metatarsus adductus, and foot progression angle during walking. Clinical examinations were conducted by multiple clinical providers using bedside goniometers, but there was no means of confirming true standardization of measurements amongst these providers (>10). Clinical examination findings were merely used to corroborate the finding of increased femoral anteversion and/or decreased tibial torsion in individual cases. Clinico-radiographic correlation and stratification based on individual clinical providers was beyond the focus of this study. The accuracy/reliability of individual aspects of the clinical examination and their correlation to the imaging study was also beyond the focus of this project.
CT examination (technical details)
The examination was performed with the patient supine with the legs extended. It was ensured that both patellae were facing forward. The scan was carried out using a 64-slice multi-detector CT Scanner (VCT64, GE Healthcare, Milwaukee, WI, USA). Five-millimeter-thick axial images were acquired through the hips, knees, and ankles. The scan time was 10–20 s, depending on the size of the patient. The amount of radiation exposure was estimated for each patient based on standardized CT radiation data per scan time and area studied (hip, knee, ankle) [25].
MRI examination (technical details)
The examination was performed utilizing the method outlined by Koenig et al. [26]. The scans were carried out using 1.5 T unit (Signa HDxt, GE Healthcare, Milwaukee, WI, USA). From the coronal localizer sequence, transverse T2 FSE (TR 4,100 ms; TE 82 ms, 256 × 224, 2 NEX) non-fat-saturated images were obtained through the acetabula and proximal femurs, knees, and ankles. A total of approximately 20 slices were required to cover the required anatomy, with each slice being 5 mm thick, with a 1-mm interslice gap. No gadolinium contrast or breath-holding was required. Acquisition at each level took 2 min and 50 s, and the total scan time was approximately 10 min.
Statistical methods
The intra- and inter-observer reliability of both the CT and MRI examinations were evaluated using the intra-class correlation coefficient (ICC) statistic in SPSS (version 12, IBM, Armonk, New York, USA). The ICC generally has a value between 0.0 and 1.0. Values closer to 1 represent stronger agreement [27]. The two-way mixed model (absolute agreement) was used because our observers were not selected at random and were measuring identical images [27]. Although there is not a set standard range of values that indicate acceptable agreement [27], for the purposes of this study, an ICC of 0.7 was chosen as the cut-off point between acceptable and unacceptable.
Results
The patient population consisted of 29 males and 32 females. The CT group had 17 males and 15 females, while the MRI group had 12 males and 17 females. Sixteen patients were being followed by orthopedics for cerebral palsy or a syndromic diagnosis (10 in the CT group, 6 in the MRI group). Fourteen patients were being followed for idiopathic angular or rotational deformity (10 in the CT group, 4 in the MRI group) and 31 patients were being followed for other orthopedic conditions, such as patellar instability, developmental dysplasia of the hip (DDH), and clubfoot (12 in the CT group, 19 in the MRI group). The mean age of the patients was 14.4 years (range 9.5–18.9 years) and 13.8 years (range 7.3–18.9 years) for the CT and MRI groups, respectively. Clinical examination findings in all patients were consistent with the findings obtained on torsional profile via advanced imaging (both CT and MRI).
Intra-observer reliability
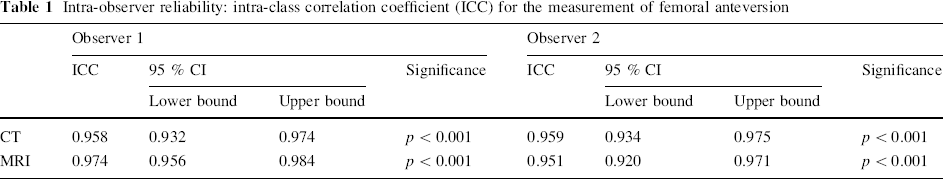
The ICC values for measurements of femoral anteversion and tibial torsion using CT and MRI by both investigators are shown in Tables 1 and 2. The ICC values for all measurements were greater than 0.800. The mean difference in femoral anteversion noted between time periods was 2.5 ± 0.19° (range 0°–10°) for observer one and 2.8 ± 0.20° (range 0°–12°) for observer two. The mean difference in tibial torsion noted between time periods was 3.4 ± 0.36° (range 0°–25°) for observer one and 3.0 ± 0.28° (range 0°–21°) for observer two.
Intra-observer reliability: intra-class correlation coefficient (ICC) for the measurement of femoral anteversion
Intra-observer reliability: ICC for the measurement of tibial torsion
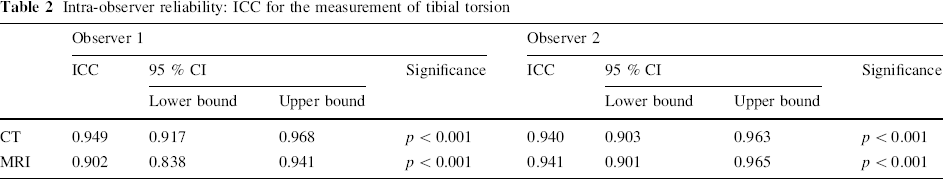
Inter-observer reliability
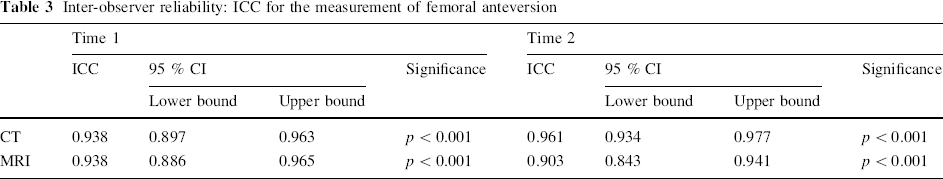
The ICC values for measurements of femoral anteversion and tibial torsion using CT and MRI at both times are shown in Tables 3 and 4. The ICC values for all measurements were greater than 0.800. The mean difference in femoral anteversion noted between observers was 3.2 ± 0.26° (range 0°–18°) at time period one and 3.3 ± 0.27° (range 0°–19°) at time period two. The mean difference in tibial torsion noted between observers was 4.1 ± 0.36° (range 0°–30°) at time period one and 4.5 ± 0.36° (range 0°–19°) at time period two.
Inter-observer reliability: ICC for the measurement of femoral anteversion
Inter-observer reliability: ICC for the measurement of tibial torsion
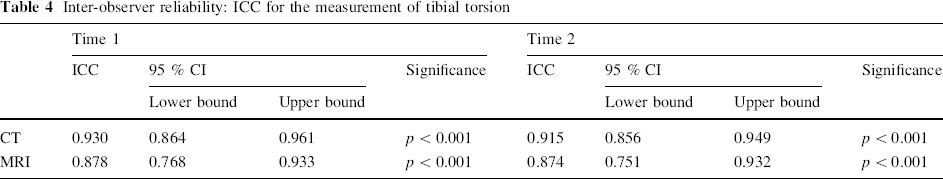
It was possible to obtain enough anatomic information from MR torsional profile to clarify the extent of femoral and tibio-fibular malrotation. These readings were comparable to the ones noted on the clinical examination (as were those obtained via CT). The MRI torsional profile measurements were reproducible between different observers.
Radiation exposure
Radiation from the CT study was between 0.3 and 0.5 mSv per patient, based on published norms for estimating radiation exposure [25]. This value was according to the protocol and necessary adjustments tailored to each patient.
Discussion
The debate on what constitutes the truly relevant torsional profile analysis, i.e. clinical examination and dynamic assessment versus an advanced imaging work-up with objective torsional assessment, remains unresolved. Although clinical methods [28] and intra-operative image intensifier [29] studies provide extensive information regarding LE torsional abnormalities, some clinicians have less faith in these methods. Also, more complex torsional problems may require a more objective determination as to location (tibia vs. femur) and severity of the torsional abnormality. CT methods for assessing torsion have been proven to give accurate values for femoral anteversion and tibial torsion as studied on dried specimens [13–15]. Similar results have been confirmed in clinical studies [28]. Together with the simplicity of the procedure, CT has been regarded as the standard method for torsional profile studies over the past three decades. Although studies in children and young adults with cerebral palsy have proved the validity and reliability of measuring femoral anteversion on physical examination as well as the femoral neck shaft angle on plain internal rotation radiograph of the femur, comparing it to data obtained via CT [4], other studies have proven that there is not an excellent correlation between the physical examination assessment of torsional profile and that obtained via CT imaging [30].
In the current era of heightened awareness of radiation safety, both the scientific literature and the media have redirected their focus towards the availability and feasibility of non-radiation-based diagnostic imaging that continues to provide clinicians with equally valuable (non-inferior) information. Because of continuing concerns about radiation exposure from CT in the pediatric population [22–24], several authors have started to look into other non-ionizing imaging modalities, such as MRI, to study torsional profile [18–21, 26]. Despite its questionable inferiority in demonstrating bony landmarks, MRI generates adequate information that is comparable to CT [18, 26].
This study is not without its limitations. Due to its retrospective nature, this study could not control for potential confounders and made no attempt to standardize the goniometers used to evaluate clinical rotation. Another limitation to this study is that none of the patients enrolled had both an MRI and CT to evaluate torsion. The lack of objective correlation of either modalities with single-observer-based clinical examination findings with adequate standardization also remains a limitation of this study, although that was not the focus of the paper. Previous literature that has proved the poor correlation between CT and clinical examination findings decreases the need to re-examine the issue though [30].
Our findings support that MRI is reliable (as compared to information obtained on clinical assessment related to the existence of femoral anteversion/abnormal tibial torsion) and can be utilized for obtaining torsional profile values in children. We have found that using MRI to study torsional profile gives adequate data needed to calculate the torsional value for each bone and that multiple observers will produce measurements that are not significantly different from each other.
Guenther [20] performed a study on anteversion of the femoral neck measured by MRI in 19 children (37 hips) preoperatively before femoral rotational osteotomies. The results were compared with values for anteversion obtained by CT scanning and ultrasound. There was a high correlation (Pearson's correlation coefficient) between the MRI results and CT scanning (r = 0.77), as well as MRI and sonography (r = 0.81). They concluded that MRI allows precise anatomical measurement and reliable results.
The radiation exposure estimated from CT for torsional profile was between 0.3 and 0.5 mSv per scan [22, 23], in contrast to radiation-free MRI. The current projected risk from childhood imaging studies remains unclear and is difficult to assess when replacement imaging (MRI) is often more time-intensive and more expensive. Special MRI sequences have been described which can bring the study time down to approximately 10 min [26, 31], and, in some cases, as short as a breath hold [32]; however, these may not be readily available. The life-long mSv exposure risk versus the current economic cost to a family (or a society) has not been established. Because of equipment availability, economic limitations, and poor understanding of the risk–benefit ratio, an MRI profile will not be available, or selected, in much of the world. However, it is clear that exposure to radiation via diagnostic imaging for a variety of medical conditions is increasing rapidly [23, 33–35], and, in our practice, parents are increasingly concerned about their child's exposure to radiation and it is important to increase the awareness of radiation-free techniques available to evaluate torsional abnormalities.
In summary, we conclude that MRI is able to produce reliable information on torsional profile evidenced by excellent inter- and intra-observer correlation. Therefore, we recommend that, whenever feasible, MRI should be utilized for torsional profile, especially in children, where exposure to low-dose radiation poses concern.
Footnotes
No funding was received for this study and none of the authors have any conflicts with this research project.
