Abstract
Abstract
Purpose
Osteogenesis imperfecta (OI) has been treated with bisphosphonates for many years, with some clear clinical benefits. In adults, there are reports of a new pattern of atraumatic subtrochanteric fractures with bisphosphonate treatment. This study assesses if bisphosphonate treatment leads to an altered pattern of femoral fractures.
Methods
Retrospective review of imaging for a cohort of 176 bisphosphonate-treated OI patients to identify the locations of femoral fractures over a two-year period, as compared to a historical control group managed pre-bisphosphonates.
Results
Sixteen femoral fractures were identified in this time period in the bisphosphonate-treated group. All but two were within the subtrochanteric region. In comparison, the historical group—composed of 26 femoral fractures—had a more widespread fracture pattern, with the most frequent location being the mid-diaphysis. Many of the subtrochanteric fractures in the treatment group occurred with minimal trauma.
Conclusions
It appears that concerns over the treatment of the adult osteoporotic population with bisphosphonates are amplified and mirrored in OI. It is possible that the high bending moments in the proximal femur together with altered mechanical properties of cortical bone secondary to the use of this group of drugs increase the risk of this type of injury, which warrants further modification of surgical management of the femur.
Introduction
Osteogenesis imperfecta (OI) is a condition characterised by bone fragility and multiple fractures, which causes considerable morbidity in affected individuals [1]. The many genetic defects in type I collagen that are generally responsible lead to a phenotypically broad spectrum of disease [2, 3]. The fracture risk arises from decreased bone density, abnormal mineralisation of extracellular matrix, disuse osteoporosis, and altered bone geometry, leading in most cases to transverse or short oblique patterns [4]. Lower limb fractures and in particular femoral fractures are most common due to their load bearing during normal gait patterns [5, 6].
The use of bisphosphonates has revolutionised the medical management of OI [7]. Their mechanism of action comes from a structure closely resembling pyrophosphate, which via its effects on surface lipoproteins ultimately results in the inhibition of osteoclast resorption of bone, altering bone turnover [8, 9]. There are other effects, including those on osteoblasts, osteocytes, and chondroblasts [10–15]. Indirect measures of bone quality (bone mineral density) increase with bisphosphonate use, as do cortical thickness and vertebral body size [16–20]. Randomized and controlled trials have also shown reductions in fracture rates and bone pain in some cases [21–24]. However, these findings are not universal [25], and not necessarily linked to a better quality of life [26], although BMD has been considered a guide to functional outcome [27]. Further studies are needed to confirm the reduction in long bone fracture incidence [28]—a difficult undertaking considering the rarity of this condition. There have been concerns raised regarding potential long-term complications, due to their effects on bone [29]. These include delayed remodelling during fracture healing [30, 31], reduced longitudinal growth [32], teratogenicity, and osteopetrosis [33].
Concern regarding the potential long-term effects of bisphosphonates has received increasing attention in the treatment of osteoporotic adults, with a number of cases where atypical subtrochanteric fractures have occurred in treated patients [34–37]. Many cases are bilateral and occur in those treated with bisphosphonates over a long period of time; there is an associated picture of thickening of the subtrochanteric bone which occurs in an elliptoid pattern associated with these fractures. Some studies suggest that the cortical thickening seen in these subtrochanteric fractures is due to repeated microfractures accumulating in this area, where bisphosphonate-mediated bone turnover effects lead to progressive failure under mechanical stress, often preceded by prodromal pain [38–40]. Recent population-based studies suggest an increased risk of subtrochanteric fracture in adults treated with bisphosphonates, which is, however, dwarfed by the overall reduced fracture rate in treated patients [41, 42]. This has not been corroborated in other population-based studies [43] and a review of three randomized controlled trials [44]. Some authors have suggested a treatment holiday to minimise potential complications [45].
Children treated with bisphosphonates may therefore be at increased risk of such fracture types. The aim of this study was to review a cohort of OI patients treated with bisphosphonates in order to assess the femoral fracture patterns seen.
Patients and methods
Approval from the Hospital Research and Audit Department was obtained. An existing database of patients currently under treatment with bisphosphonates was utilised to identify patients treated for OI. Using the digital radiograph archive, all imaging available for these patients over a two-year period from 2007 to 2009 was reviewed. Radiographs of femora as part of a skeletal survey or as isolated imaging were reviewed to assess the prevalence of acute femoral fractures in this time period. Other long bone or axial fractures were not assessed. Where fractures were identified, case notes were obtained for demographics on the patients and details of the fracture. The presentation, mode of injury, and length and type of bisphosphonate treatment were all recorded, as was the classification of the type of OI according to Sillence. Whether affected femora were rodded or not was also recorded, together with whether the mechanism of injury was high or low energy. Total body and spinal bone mineral density Z scores were also obtained for the time of injury.
A historical control group of OI patients, treated initially in childhood by surgical techniques, were used as a comparison. Case notes for this group were obtained and radiological reports for femoral fractures in those not treated with bisphosphonates were reviewed. Radiographs were also examined. Results for the locations of the fractures were plotted graphically for a direct visual demonstration of the trends.
Results
One hundred and seventy-six patients with moderate or severe OI in total were currently receiving treatment with oral risedronate or cyclical intravenous pamidronate during the two-year study period. These patients represent the entire bisphosphonate caseload at our unit treated during the two-year period described. The dose of pamidronate varied from 3 to 12 mg/kg/year given over 2–3 consecutive days with 1–4 treatments per year. Patients treated with risedronate received 0.2–2 mg/kg per week. Treatment holidays are not routinely used, except where surgery for long bone realignment is planned. Of these patients, 133 patients had imaging available for review, either as radiographic follow-up for surgical procedures, acute presentations, DEXA scans or skeletal surveys. A total of 43 had no imaging in this timescale.
Eleven patients had 16 femoral fractures on the radiographs available (Table 1). Of the 11, three were Sillence type III and the remainder type IV. Five had sustained bilateral fractures over the study period. All but two had been treated with bisphosphonates for more than six years. All fractures were either short oblique (25%) or transverse (75%). Figure 1 represents the location of each fracture in each of the patients in both the bisphosphonate-treated and control patients. In terms of the mechanism of injury, those classified as high energy made up 31% of all fractures. Those included in this group were injuries where a definite fall had occurred that could cause a fracture in an unaffected individual. Examples include a fall getting out of a swimming pool and a fall whilst dancing. Low-energy injuries included all fractures where the mechanism would not be associated with a fracture in an unaffected individual. In two cases there was no history of injury prior to the onset of pain, after which the fracture was diagnosed.
Demographics of femoral fractures in osteogenesis imperfecta patients treated with bisphosphonates
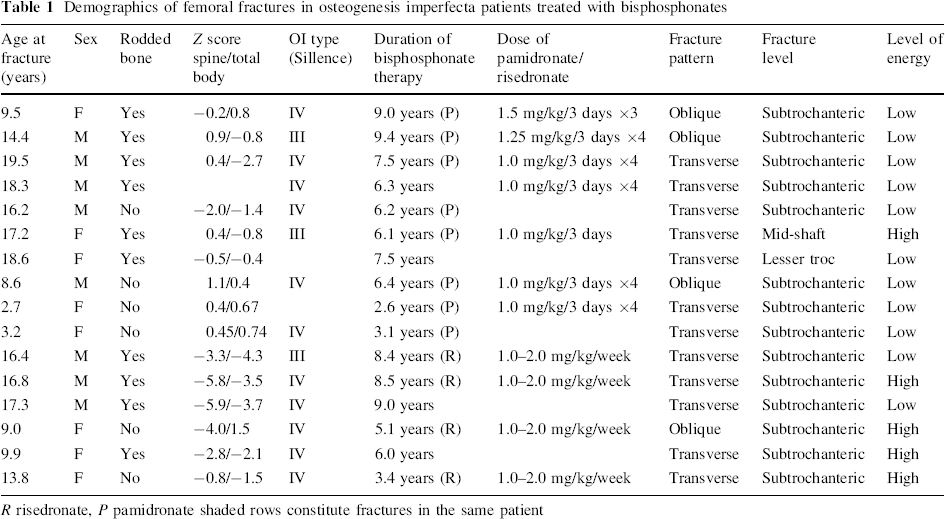
R risedronate, P pamidronate shaded rows constitute fractures in the same patient
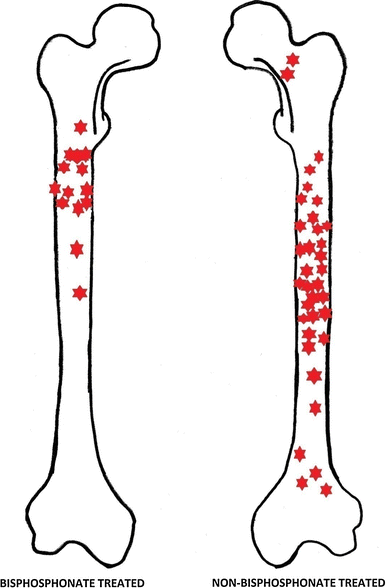
Graphical representation of fracture locations in bisphosphonate and non-bisphosphonate-treated patients
In three cases, the fracture occurred through a previous osteotomy with radiological evidence of union prior to the current fracture (union was defined as bridging callus visible on four cortices on an AP and lateral radiograph of the femur). One fracture had occurred through a mid-diaphyseal healed fracture. 38% of the fractures occurred in rodded femora. Fractures tended to be associated with pan-cortical thickening of sub-trochanteric bone, although—due to the small differences in the amount of thickening and despite standardised views—the absence of a calibration sphere meant that this could not be accurately measured (Figs. 2, 3). Ten of the 16 fractured femora had a telescopic rod in situ, and none had a pathological sagittal or coronal bow, although coxa vara was (as would be expected) a common finding.
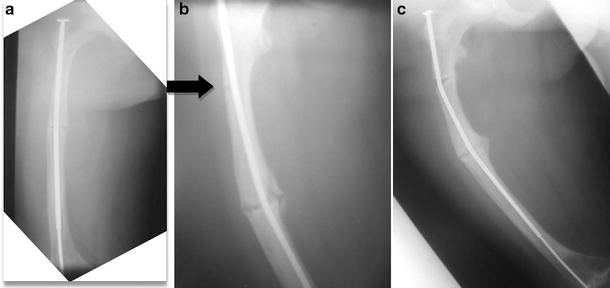
A type IV adolescent OI male patient.
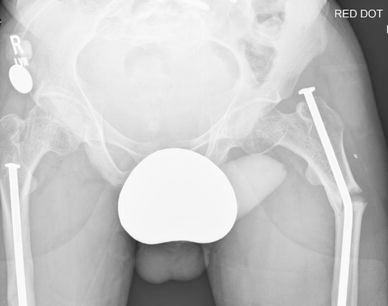
A subtrochanteric fracture in an adolescent Sillence type IV OI patient sustained whilst dancing. The elliptoid thickening in the region of the fracture corresponds to similar findings in adult bisphosphonate-treated patients
The comparison group consisted of a historical group of OI patients treated prior to the advent of bisphosphonates. A total of 45 were identified with complete data, all with moderate or severe OI. All had reached skeletal maturity at the time of this study. Fractures were recorded from the original treatment until discharge from the children's hospital to the adult sector at 18 years of age. This cohort consisted of patients referred for consideration of surgical treatment of OI, with either acute fractures, recurrent fractures, or deformity. The radiographic review therefore consisted of unrodded femora without significant deformity, or rodded femora for the indications mentioned above. Over the course of treatment within our institution, a total of 34 femoral fractures occurred in the 26 patients. Apart from one segmental midshaft fracture, all injuries were short oblique or transverse fractures. Two femoral neck and four distal fractures were included in the group, although the majority were in the mid-diaphyseal region. 73% of the fractures occurred in patients already treated with intramedullary rodding of the femur; these were telescopic rods in nearly all cases (Table 2). Due to the retrospective data available and the small number of historical cases with complete data to allow a comparison, this cohort consists of similar cases of moderate and severe OI that in the present era would qualify for treatment with bisphosphonates, but which differ from the treatment group in that all fractures sustained were recorded during the entire treatment, and are therefore similar only in the underlying severity of bone disease.
Non-bisphosphonate-treated OI patient classification and fracture details
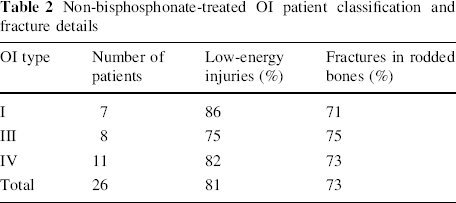
Statistical analysis was not possible based on existing classification systems, primarily because the Pediatric Comprehensive Classification of Long Bone Fractures only differentiates on fracture location by describing the proximal and distal metaphysis and the diaphysis; this would not allow any differences in the location within the diaphysis to be differentiated. For this reason, and due to the small numbers within the study, only trends are inferred from the resultant fracture patterns (Fig. 1).
Discussion
The benefits of bisphosphonates are not in doubt, either in adult populations or in the various clinical situations where children require treatment. Experience in our institution certainly suggests that treatment has reduced OI fracture rates and bony pain in treated patients [46]. OI is a different clinical entity compared to osteoporosis, the main indication for the use of bisphosphonates in adult populations. For this reason, identifying a change in the pattern of femoral fractures within a relatively small cohort is a finding of concern, and warrants further investigation. This adds to an already controversial topic; current issues include the choice, dose, and method of administration of bisphosphonate, as well as the perioperative medical treatment regime that is least likely to interfere with osteotomies and fracture healing.
The length and method of treatment is in itself a subject of debate in the care of osteoporotic adults. At present there is insufficient research to guide on whether “drug holidays” may be of benefit in reducing the rate of atypical fractures. These treatment holidays may themselves put patients at risk of further fractures.
With increasing bisphosphonate use, there appears to have been a change in the pattern of fractures seen in our cohort of patients, with more proximal fractures seen in the femur, and some developing insidiously without any history of trauma. In the adult osteoporotic population, a review of over 14,000 patients in three randomized trials treated with bisphosphonates identified no significant increase in atypical fractures, although firm conclusions could not be drawn because it was felt to be underpowered [44]. A further population-based case–control study has identified that there is an increase in subtrochanteric fractures in those treated with bisphosphonates for more than five years [42]. The trend demonstrated in our cohort highlights a trend that far exceeds that seen in the adult population, and the underlying OI abnormalities are the likely cause (Fig. 4).
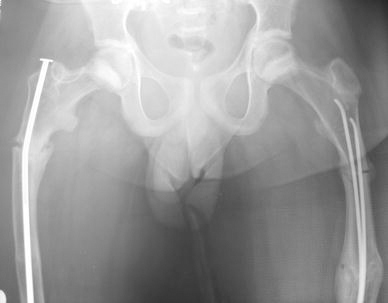
A type IV adolescent male patient who sustained bilateral sequential atraumatic subtrochanteric fractures. One side was treated with elastic nailing. Zebra lines from bisphosphonate use are visible around the proximal femora and pelvis
A possible hypothesis for this altered pattern can be inferred from animal studies, and the basic science of developing bone growth. OI is a condition associated with high bone turnover. Although the main effect of bisphosphonates is modifying the osteoclastic resorption of bone, they also affect osteoblasts [10–15] and chondroblasts [47], and in vivo studies suggest better longitudinal bone growth [48, 49]. How exactly the risk of fracture may be reduced with bisphosphonate treatment is not fully understood. The bone of patients with untreated OI is hypermineralised, but despite this, treatment with bisphosphonates appears to increase bone mass by cortical and trabecular thickening; it may alter the cross-sectional geometry, but it does not alter the material properties of bone [50]. Intramembranous ossification, such as that involved in appositional growth of cylindrical bones such as the femur, are mainly osteoblast mediated, with some evidence to suggest that bisphosphonates affect the quality of the organic matrix, leading to bone with weaker mechanical properties [51, 52]. Studies of OI patient iliac bone samples have suggested that intrinsic properties are unaffected [53]. There is also evidence to suggest bisphosphonates bind selectively to areas of increased bone turnover, which may result in patchy areas of uptake. This may also play a role, and may be exacerbated, if there is an element of stress shielding in rodded bones.
A recent study looking at the effect of bisphosphonates on the BRTL mouse OI model corroborates that the brittleness of bone is not altered by treatment; histological analysis of mid-shaft and proximal bisphosphonate-treated bone identified areas of weakness secondary to unmineralised cartilage. Altered osteoblast function was also identified, and an overall reduction in bone strength with continued treatment was noted; the stiffness, toughness, Young's modulus, and moment of inertia remains the same with treatment [54, 55].
It is likely that weakness to bending moments within the proximal femur due to the mechanisms explained above result in this altered fracture pattern.
We believe that the findings of this study identify concerns regarding the long-term use of bisphosphonates and a changing pattern of fractures, amplifying as well as mirroring the findings of other groups among adults. OI is a completely different disease entity when compared to the main clinical indications for bisphosphonate use in adults, and the response of bone to the use of this group of drugs would be expected to demonstrate similar trends, but not a large increase in the incidence of pathological fractures. The findings suggest that there is a much increased risk of fracture pattern alteration in this skeletal dysplasia, which warrants further investigation including clinical trials and histological analysis of cortical bone from treated OI patients.
It also warrants an altered attitude towards surgical management of the femur. As this particular region appears at increased risk of fracture, efforts should focus on maintaining a mechanical axis that is as normal as possible. In particular, excessive coxa vara, which is commonly seen in more severely affected OI patients, increases the moment arm at the subtrochanteric level, which may in turn allow lateral microfractures to develop. In addition, corrective osteotomies at this level, if possible, should be avoided when planning corrective surgery, as healing in this group of patients treated with bisphosphonates is known to be altered in a deleterious manner. Any patient reporting pain in the upper thigh should have the proximal femur imaged and radiological changes described previously should be sought. Screening radiographs may be indicated to assess and predict fracture occurrence in this area.
There are limitations to this observational study. It does not compare fracture incidence in bisphosphonate-treated patients to untreated patients. A review of radiographs is not guaranteed to identify all femoral fractures, as some patients may have been imaged in other hospitals because the centre is a tertiary referral unit. There is matching of the underlying OI type with the historical comparison made, although the use of a method based on available historical data and the small number of femoral fractures sustained in the treatment group only allow a trend to be demonstrated. However, we do believe that, as a comparison, it does highlight a different pattern of fractures (Fig. 1) which must be considered together with the other controversies regarding the medical management of OI.
