Abstract
Abstract
Introduction
In patients with cerebral palsy, the prevention of hip dislocation should be the “primum momens” of early surgery. The surgery consists of a myotomy of the adductor medium, mayor and gracilis, and, in non-ambulatory cases, a neurectomy of the second branch of the obturator nerve. The purpose of this study was to examine whether the adductor myotomy should be performed on the contralateral side at one sitting.
Materials and methods
In a study performed by our team on 1,474 patients, 792 patients (53.7%) had a unilateral procedure and 682 a bilateral procedure.
Results
The non-myotomized spastic adductors alter the movement of forces on the femoral head and, thus, 78.20% required a secondary contralateral procedure. The dislocation of the hip in patients whose operations were performed at two different sittings occurred in 20% of cases, and in those with a bilateral procedure at one sitting only in 1%. The increase in the cervicodiaphyseal angle occurred in 23.1% of patients with surgeries performed at two sittings and only in 10% of patients with bilateral procedures at one sitting.
Conclusions
Our results suggest that the bilateral surgical procedure at one sitting should be recommended to equalize the movements of force in spastic hips.
Introduction
The objective of orthopaedic surgery in the treatment of spastic hip is to prevent and/or correct deformities and improve function. It must be performed early, taking into consideration that gait ability reaches its maximum level at 7 years of age.
The hip is the second most affected joint in cerebral palsy (CP). Its stability will depend on the correct relationship of forces among flexors, adductors and internal rotator muscles on the one hand and extensors and abductor muscles on the other. In those with CP, the hip becomes at risk of a future dislocation when there is an abduction less than 45° and a head extrusion beyond 40° (Figs. 1, 2) [1]. At this stage, we must act surgically to avoid the progression to a dislocation, acting on spastic muscles forces that lead to it [2–4].
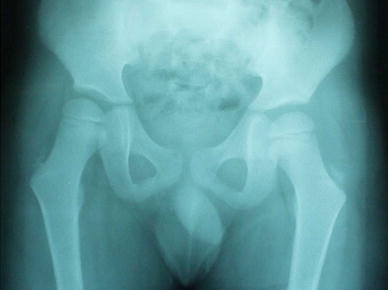
Observe valgus of the neck and the partial extrusion of the head in the right side
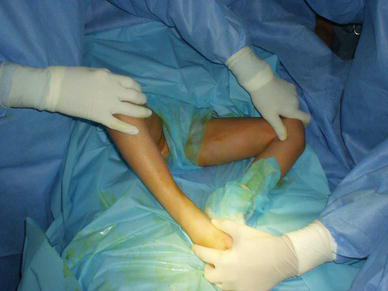
Limitation of hip abduction bigger in the right side
We must perform a myotomy of medial and great adductors, with or without myotomy of gracilis, depending on abduction limitation, and a psoas tenotomy [1, 5–7] (Fig. 4). We then immobilize for 15 days in a DuCroquet-type plaster of Paris. These procedures will improve function on diminishing the scissoring gait, thus preventing dislocation of the hip. The neurectomy of the second branch of the obturator nerve must be done only in those patients without gait possibilities, and for hygiene purposes (Fig. 3) [8–10].
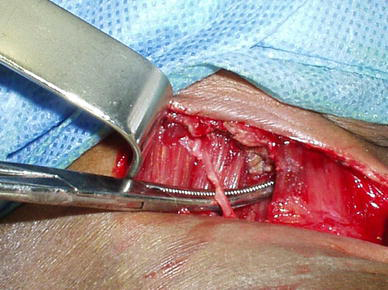
Dissection of the second branch of the obturator nerve, which must be waived except in patients without walking ability
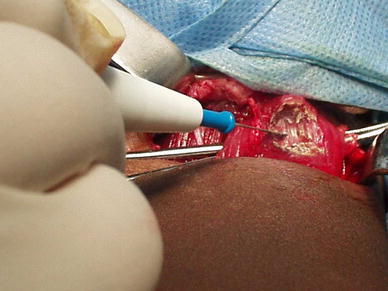
Myotomy of medial and major adductors
It has been widely reported that results of the medial translocation of adductor muscles, besides being a more difficult procedure, are not different from a plain myotomy [5, 7].
In this study, we intended to evaluate whether a bilateral adductor myotomy at one sitting would give better results, avoiding a later hip dislocation, than when the procedure is performed in two stages.
Materials and methods
Between 1975 and 1995—with more than 10 years follow-up—we performed adductor surgery in 1,474 patients. Unilateral and bilateral procedures were performed in 790 (53.7%) and 682 (46.3%) patients, respectively. Patients were operated as soon as a limitation of abduction in one side was observed on clinical examination, regardless of age—the youngest was operated on at 2 years of age. The procedure performed was a myotomy of adductor mayor and medium; in cases of patients with an Ely-positive sign, a gracilis myotomy was also performed. The follow-up periods are explained during evaluation of the results when a requirement of a new, different procedure, such as contralateral myotomies or osteotomies at different levels, were required at such a follow-up stage. Analyzing these results at the final follow-up—more than 10 years—we can observe whether these further surgical procedures required were somewhat useful. Due to the great number of patients and the clear difference between the two groups, we did not perform the statistical analysis.
Results
Among 792 patients with unilateral procedures, 619 (78.20%) needed adductor surgery in the contralateral side a mean of 3.6 years after initial surgery. A unilateral hip dislocation developed in 123 patients (20%). In 115 (93%) of these 123, the dislocation occurred a mean of 1 year post-operation in the side of the second surgery.
Among 619 patients, 143 (23.1%) developed Coxa valga of more than 155° (23.1%) at a mean of 6.6 years of age, and 3 years after the second surgery. In 102 of 143 (71%), it was necessary to perform a derotation and varus osteotomy of the proximal femur in the hip, where the second adductor surgery was performed and, in 20 of 102 (20%), the end result was a hip dislocation.
The bilateral myotomies at one sitting were performed in 682 patients (46.30%). Only 7 patients (1%) developed a unilateral dislocation in a mean 2 years post-operation, and 68 of 682 (10%) required a varus plus derotation proximal femur osteotomy at a mean age of 6 years; of these 68, 20 (3%) ended in a hip dislocation.
Of the total 130 dislocations seen, 72 (55%) were quadriplegics, 28 (21%) diplegics, 21 (16%) hemiplegics and 1 (1%) was triplegic.
Conclusion
The adductor spastic muscle non-myotomized alters the movements of force on the femoral head and, thus, 78.20% of patients required a further contralateral operation. Dislocation occurred in 20% of cases that had undergone surgery at two sittings, but only in 1% of those that were operated on bilaterally at one sitting. The augmentation of the cervical diaphyseal femoral angle occurred in 23.1% of cases operated on at two sittings and only in 10% of those operated on bilaterally at one sitting.
With regard to the results obtained using the two-stage operation and the method proposed by us of a single-stage bilateral myotomy at one sitting, in view of the size of the group studied (1,474 patients) and the length of the follow-up (more that 10 years), we think that medicine based in evidence allows us to draw the final conclusion that a bilateral adductor myotomy at one sitting should be the technique of choice. In our opinion, it is necessary always to operate on the adductors bilateral at one sitting, regardless of the clinical spasticity and the unilateral affection, in order to equalize the sum of moments of forces at hip level (Fig. 5).
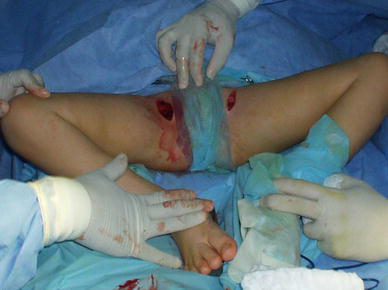
Observe the identical bilateral abduction obtained after the bilateral procedure
