Abstract
Abstract
Purpose
Reports on thoracic pedicle screw (TPS) constructs have demonstrated their safety and efficacy; however, concerns exist regarding their increased cost. This is a review of adolescents with main thoracic scoliosis surgically treated with anterior release and posterior fusion or posterior fusion only. The objectives were to compare the radiographic outcomes and financial data of two surgical treatments: anterior/posterior spinal fusion (APSF) versus posterior spinal fusion (PSF-TPS) alone with TPSs, in patients with large 70–100° main thoracic adolescent idiopathic scoliosis (AIS) curves.
Methods
We identified 43 patients with main thoracic Lenke type 1–4 AIS curves between 70 and 100° who had been treated with either APSF or PSF-TPS.
Results
Both groups had equivalent radiographic corrections postoperatively. The PSF-TPS group patients had higher implant charges, but the APSF group had higher surgeon procedural charges, operating room charges, anesthesia charges, and inpatient room charges. Total charges were $75,295 for the APSF group and $71,236 for the PSF-TPS group (P > 0.05). Analyses of two subgroups of the APSF group, anterior release via thoracotomy versus VATS and same-day versus staged surgeries, failed to change any of the above findings.
Conclusion
Based on this financial analysis, there was no statistically significant differences between the APSF and PSF-TPS groups, with equivalent radiographic corrections.
Keywords
Key points
Posterior-only spinal fusion utilizing thoracic pedicle screws has an equivalent degree of curve correction to combined anterior and posterior spinal fusions. Higher surgical implant charges in the posterior-only spinal fusion utilizing thoracic pedicle screws were due not only to the higher implant charge per unit but also to a greater number of overall implant fixation points. Posterior spinal fusions with thoracic pedicle screws were not more expensive than circumferential fusion for curves between 70 and 100°. The increased implant charges for the PSF-TPS group was offset in the circumferential group by higher surgeon's procedural charges, operating room charges, anesthesiologist charges, and inpatient room charges in the AP group.
Introduction
Surgical treatment of large, main thoracic adolescent idiopathic scoliosis (AIS) between 70 and 100° has often consisted of anterior and posterior fusion to improve correction and increase the fusion rate. However, the impact of chest wall violation on pulmonary function and the higher complication rates of circumferential fusion for AIS has been well documented [1–6]. Prior to the development and application of thoracic pedicle screws (TPSs), the limitations of posterior fusion-only constructs by hook-only or hybrid constructs theoretically translated into less correction of the scoliosis. With the use of TPSs, many centers have reported an improved ability to 3-dimensionally correct AIS curves due to the improved segmental fixation, better immediate correction of the coronal, sagittal and rotational deformity, less loss of correction, shorter fusions, avoidance of anterior spinal fusion, and less risk of neurological complications, when compared with posterior hook-only or hybrid constructs [1, 2, 7, 9–11].
Critics of TPS constructs cite the increased implant costs, need for specialized skill in TPS placement, and the lack of correlation of postoperative spinal alignment and patient outcome measures as barriers to more widespread application of TPS [10]. The higher overall implant costs can be due not only to the higher per-unit charge for each TPS but also to the trend by surgeons to use a greater number of fixation points during the AIS surgery. The purpose of this study was to compare the financial data and radiographic outcome of two surgical treatments: anterior/posterior spinal fusion (APSF) versus posterior spinal fusion (PSF-TPS) alone with TPSs in patients with large 70°–100° sagittal thoracic AIS curves.
Methods
A database search was completed to identify all patients with main thoracic AIS curves between 70 and 100° who had undergone spinal fusion (APSF or PSF-TPS) at one academic center between 1987 and 2001. Only Lenke type 1–4 main thoracic curve patterns were included for analysis [12, 13]. Patients were excluded from analysis if their follow-up was less than 1 year postoperative. Demographic and radiographic data collection were performed, tabulated and analyzed by individuals not directly involved with the patients’ care.
All the patients in this study had attended one of two independent children's hospitals, which are the two senior surgeon's main pediatric hospitals. The majority of the surgeries were performed at our pediatric charity hospital, where no financial database exists from which to derive financial information. Because of this, a novel financial analysis method was developed based on the main financial drivers of spinal fusion surgery: implant charges, surgeon procedural charges, anesthesiologist charges, operating room charges, and the inpatient room charges. To establish the implant charges, per-unit implant costs were obtained from the spinal implant manufacturer (rods, fixed-angle screws, multi-axial screws, hooks, cross-links, wires, set screws). For the APSF group, the implant mark-ups averaged 1.6 and for the PSF-TPS group 2.1; these were typical hospital financial mark-ups at our second children's hospital during the study time periods. A change in technique was represented in the two study groups due to the implementation of TPSs in 1999. Surgeon procedural charges were tabulated using 2004 CPT coding guidelines for each surgery and were reviewed by our orthopaedic surgery departmental coding specialists. Charges per CPT code were actual 2004 charge amounts, theoretically billable to third-party payers, which were 125% of medicare relative value units (RVUs), the current department of orthopaedic surgery standards in our institution. Anesthesiologist charges were based on the anesthesiologist surgical set-up charges for spine fusion (posterior-only or circumferential) and the actual “time” the anesthesiologist cared for the patient [preoperatively, operatively and in post-anesthetic care unit (PACU)] in 15-min increments. This second “time” charge was typically 15 min prior to entering the operating room, time in the operating room and the first 30 min of the PACU stay. Operating room charges are based on time the patient is in the operating room, in 15-min increments, and on the surgical disposables required for each type of spine fusion. Room charges were assessed by tabulating days in the pediatric intensive care unit (PICU) and on the regular inpatient floor. Per-day charges were generated from the billing office of our second pediatric hospital. Retrospective medical chart review documented length of anesthesia care, patient time in the operating room, surgical procedures, and length of inpatient stay (PICU and regular floor). Minor costs associated with the surgery, such as radiological studies, laboratory studies, and perioperative medications, were not tabulated based on the estimation that the remainder of the postoperative care would be similar between the groups.
All surgeries were performed by one of the two senior authors. Free-hand pedicle screw placement was performed using specific anatomical landmarks with multiple confirmatory steps to ensure intraosseous placement [14–17]. All TPSs were placed in a “straight-ahead trajectory”, paralleling the superior endplate as recommended by Kim and Lenke et al. [18, 19] and under tapped by 1.0 mm to optimize fixation [20]. Intraosseous TPS placement was confirmed with the use of triggered electromyograms, similar to those utilized in the lumbar spine [3]. Based on the type of posterior instrumentation, two distinct treatment groups could be identified: (1) anterior/posterior spinal fusion (APSF) with hooks-only or hybrid constructs (consisting of proximal hooks and distal pedicle screws) and (2) posterior spinal fusion (PSF-TPS) alone with TPSs. The use of different implant systems represents the evolution of AIS treatment performed by the senior authors from hook-only and hybrid constructs to the current pedicle screw-only constructs during the time frame of this study.
Preoperative radiographs for all patients routinely included a standing long cassette (36”), coronal and lateral, left and right side-bending views, and push-prone coronal radiographs. The Lenke classification system for AIS was utilized, which has been shown to be accurate and reproducible and correlates with treatment of surgically structural regions of the spine [12, 13, 21]. Multiple radiographic measurements were assessed on the preoperative, immediate postoperative standing, and final postoperative long cassette biplanar radiographs. Main thoracic curve data included the coronal Cobb measurements, and the upper and lower levels of the thoracic curve. Coronal flexibility of the main thoracic curve was assessed on supine side-bending AP radiographs over the extent of the thoracic curve and was expressed as a percentage [flexibility = {(preoperative coronal Cobb − side-bending Cobb)/preoperative coronal Cobb} × 100]. The number of fixation points (wires, hooks and pedicle screws) were counted and utilized to tabulate the number of fixation points per number of vertebral levels fused. To assess the relative ability of thoracic hook and TPS constructs to correct the thoracic curve, regardless of the number of levels fused, the overall main thoracic curve correction was divided by the number of fixation points per level fused (main thoracic curve percent correction /number of fixation points per level fused).
The statistical analyses were performed using the Pearson chi-square test to statistically test differences in the proportion of boys between the two groups (APSF versus PSF-TPS) and the Wilcoxon–Mann–Whitney test to test differences in the distributions of the other variables statistically. Because of the limited sample sizes in the groups, we used the exact P values for both tests as implemented in StatXact (version 5) (reference corporation CS) [22].
Results
A total of 43 patients who satisfied the criteria for inclusion were identified. Mean age of patients was 14.2 years (range 10.6–18.2 years), with 34 females and 9 males. Mean follow-up was 3.5 years (range 1.0–10.2 years). There were 18 patients in the anterior/posterior spinal fusion (APSF) group, with 14 undergoing open thoracotomy and release (open ASF) and 4 undergoing video-assisted thoracoscopic (VAT) release. There were 25 patients in the PSF-TPS group.
No statistically significant differences were observed between the groups with regard to gender, age at the time of surgery, number of levels fused, Cobb measurement of preoperative thoracic curve magnitude, curve flexibility, or intraoperative curve correction (Table 1). Statistical analysis of the APSF (n = 18) and PSF-TPS groups (n = 25) demonstrated the latter to have more implant fixation points used for correction (PSF-TPS 19.4 vs APSF 14.1; P < 0.0001) and more fixation points per number of vertebral levels fused (PSF-TPS 1.7 vs APSF 1.2; P < 0.0001). Interestingly, the APSF group demonstrated a higher percentage intraoperative curve correction per fixation points per vertebral level fused (P < 0.0001); hence, the anterior release increased the flexibility of the spine significantly, permitting the hook/wire constructs to have equal overall main thoracic curve correction to the PSF-TPS group.
Anterior/posterior spinal fusion (APSF) versus posterior spinal fusion (PSF)
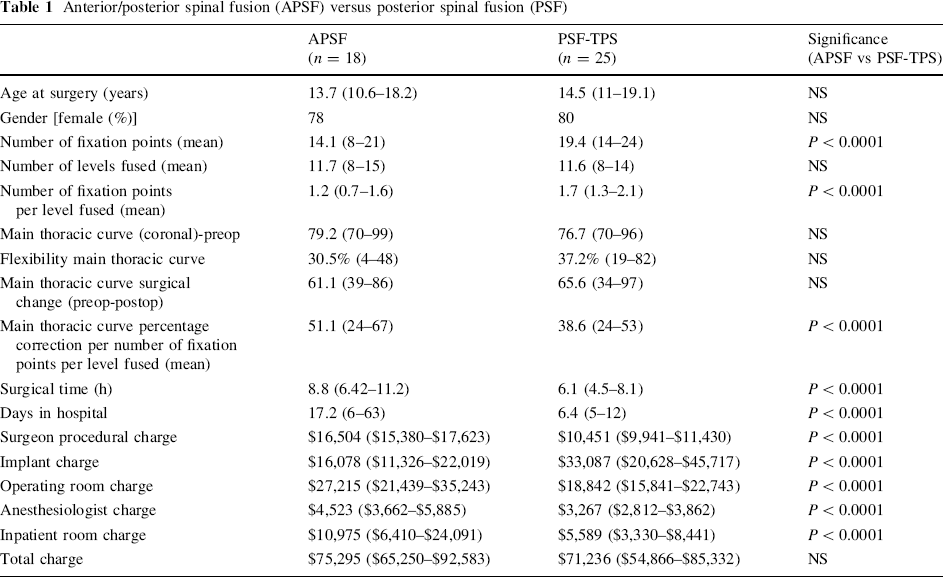
Overall, the total charge for the PSF-TPS group was $71,236 compared with $75,295 for the entire APSF group (n = 18) (P > 0.05; Table 1). The surgical time was significantly less in the PSF-TPS group (PSF-TPS 6.1 h vs APSF 8.8 h; P < 0.0001) as was true for the total number of days in the hospital (PSF-TPS 6.4 days vs APSF 17.2 days; P < 0.0001). Because six of the cases in the APSF group were staged, the mean number of days in the hospital was significantly higher than it was in the PSF-TPS group; to account for this, a sub-analysis was done to compare the PSF-TPS group and the APSF group (for which surgery was performed on a single day; SD-APSF) (Table 2). There was a difference between groups with regard to days in the hospital (PSF-TPS 6.4 days vs SD-APSF 7.9 days; P = 0.001) but total charges were not significantly different (PSF-TPS $71,236 vs APSF-same day $72,416; P > 0.05).
Same-day anterior/posterior spinal fusion (SD-APSF) versus posterior spinal fusion (PSF)
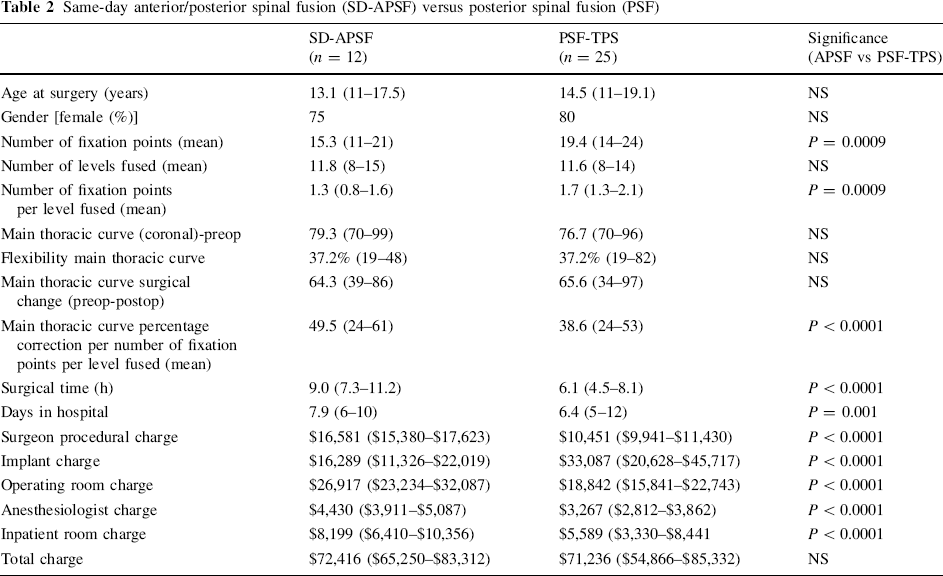
The overall differences between the two groups for the surgeon procedural charges, implant charges, operating room charges, anesthesiologist charges and hospital inpatient room charges were all statistically significant (P < 0.0001) (Table 1). There were no differences in the data between the two hospitals, such as longer stays at the charity hospital. A previous report on VATs demonstrated that surgical disposables and operating room equipment charges were significantly higher than open ASF (57). Because of this, a second sub analysis was completed to compare PSF-TPS with the APSF group for which anterior release was performed through an open thoracotomy (O-APSF) (Table 3). The overall charges for the PSF-TPS group were not statistically different from the O-APSF ($71,236 vs $75,983, respectively; P > 0.05). The APSF subgroup with the lowest charges was done on a single day with an open thoracotomy ($70,089).
Open anterior/posterior spinal fusion (O-APSF) versus posterior spinal fusion (PSF)
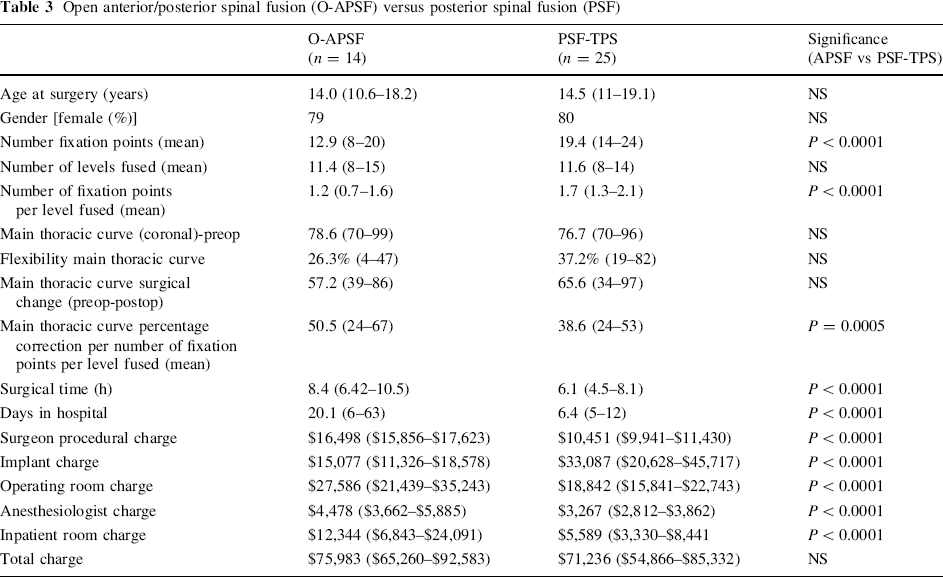
Discussion
The treatment of AIS has undergone an evolution since the introduction of the Harrington rod system. First-generation CD instrumentation, and its clones, supplanted the Harrington rod system as the “gold standard” for scoliosis implant systems due to improved curve correction, maintenance of long-term correction, improved overall spinal motion, and a low frequency of pseudoarthroses and neurological deficits [23–28]. The introduction and application of lumbar pedicle screws enhanced the ability to correct the scoliosis deformity through better three-column bony fixation in the lumbar spine [29]. However, in order to accommodate the shortcomings of hook fixation in the thoracic spine, anterior releases were additionally performed to improve the flexibility of the thoracic spine and permit a greater surface area for fusion, especially for larger and stiffer curves [4, 30–34]. The downside of anterior release at the time of posterior spinal fusion has been well documented, with increased time under general anesthesia, increased patient cost, higher complication rates, and the negative impact on pulmonary function, both perioperatively and long-term [1, 3–6, 30, 32, 34–38].
The improved three-column fixation of TPS, which permits direct apical vertebral derotation, has been demonstrated in cadaveric studies and clinical case series [2, 7, 9–11, 39]. However, the application of pedicle screws in the thoracic spine was slow to gain acceptance due to the challenges of safe, intraosseous placement in AIS secondary to implant constraints and to the size, orientation and morphology of the thoracic pedicles. Various insertion techniques have been reported to safely guide the placement of TPSs, from the free-hand technique to image-guided systems, making TPS placement possible in nearly all patients, including those with severe curves [8, 14, 16, 17, 21, 40–49]. Several centers with significant experience in TPS use have documented a low frequency of screw-related complications [14, 50, 51]. In 2001, Suk et al. [51] reported on 462 surgically treated AIS patients with 4,604 TPSs. A total of 67 screw malpositions (1.5%) were documented, with screw-related neurological complications in only 4 patients (0.8%): 1 transient paraparesis and 3 dural tears. In 2004, Kim et al. [14] reported on a retrospective analysis of 233 AIS patients at a single center with 2,653 TPS. There were no postoperative insertion-related neurological complications in this patient series. Despite this encouraging data on the safety of TPS placement, neurological sequelae attributable to TPS have been reported [6, 52, 53].
Analyses comparing TPS with other fixation constructs have reported thoracic curve corrections with TPS constructs to be 56–71% and hooks to be 49–52% [2, 7, 9, 49, 50]. Kim et al. [2] reported a matched cohort analysis of surgically treated AIS patients comparing segmental hook to segmental pedicle screw constructs. The TPS constructs had a better ultimate major curve correction (43 vs 71%) and apical translation (63 vs 41%), with shorter construct lengths by an average of 0.8 levels, than hook constructs. In a study on large main thoracic curves between 70 and 100°, Luhmann et al. [54] demonstrated PSF with TPS constructs to have equal correction of the main thoracic curve when compared with APSF with hook and hybrid constructs (APSF 47.2°, 58.5% vs PSF-TPS 45.9°, 58.3%; P > 0.05). These studies demonstrate the utility of segmental TPS fixation, and raise the question as to the necessity of anterior releases for all curves, regardless of flexibility, up to 100°.
The costs of TPS implants and the justification of their use has been the topic of significant debate [10]. The previously mentioned matched cohort study of Kim et al. [2] reported the implant costs (hospital purchase costs) for TPS constructs to be US $11,508, approximately double the cost of hook-only constructs (US $5,816). In an era of rising healthcare costs and the institution of cost containment policies by third-party payers, this cost differential, taken as an isolated cost, may be viewed as an unnecessary expense. However, as demonstrated by this study for curves from 70 to 100°, TPS constructs permit equal correction to APSF with hook and hybrid constructs, while avoiding the increased morbidity of chest wall violation. The mean increased implant costs associated with TPS constructs of US $17,009 are offset by eliminating the surgeon procedural charge for an anterior release, lower anesthesiologist charges, and lower operating room and inpatient room charges. Because the APSF group had some of the anterior release performed with VATs and others were staged surgeries, both of which can drive up hospital charges, sub analyses were performed to isolate the APSF done via thoracotomy and that on the same day as the posterior fusion. These same-day APSF with thoracotomies were similar in cost to the PSF-TPS constructs (TPS US $71,236 vs APSF $70,089, P > 0.05). In addition, it should be noted that the length of stay is similar between our children's hospital and our charity hospital (P > 0.05).
In this study, of the 18 patients that underwent a circumferential fusion (APSF), only 4 had hybrid constructs. The use of sublaminar wires is a significantly less expensive option (Luque wires, US $5 in 2004; Wisconsin wires, $96 in 2004) than hooks ($696 in 2004) or screws ($872–$1,232 in 2004). Because the use of wires is an adjunctive method of treatment in our institution, very few wires (average of four per patient) were utilized in any of the constructs. If the surgical plan is to utilize a substantial number of wires (Luque or Wisconsin) in place of screws or hooks then the implant costs can be lowered significantly. To accomplish cost neutrality between the two study groups, the APSF implant construct must be lowered by US $4,059 (Table 1; $75,295 − $71,236 = $4,059), which means using wires instead of 3.3 multi-axial screws or 4.6 fixed-angle screws or 5.8 hooks. If one was to construct the least-expensive construct [2 rods, 2 cross-links, 8 hooks (claw constructs at top and bottom of construct) and 10 Luque wires], the implant costs would be US $11,186 or a decrease in the mean APSF construct costs in this study of US $5,318.
Another often overlooked financial issue in scoliosis surgery is that due to revision surgery. Kuklo et al. [55] recently presented data on the surgical revision rates of 1,428 patients from 2 medical centers after fusions for AIS over a 14-year period. Overall revision rates were 4.5% (64 of 1,428 patients). Hook and hybrid constructs had overall higher surgical revision rates (6.4 and 5.7%, respectively) when compared with TPS constructs or APSF (2.4 and 2.5%, respectively; P < 0.05). The 4% difference in revision rates between all-hook and TPS constructs calculates into roughly 40 more revisions cases per 1,000 primary cases. The financial costs of revision spine surgery, the impact on ultimate outcome and patient satisfaction have not yet been described in the literature, but are likely significant. The benefits of TPS and their lack of complications makes TPS constructs attractive and will likely lead to fewer revisions [10, 55].
Several drawbacks of this study exist. The financial analysis methodology utilized in this study was driven by the absence of financial data from our charity children's hospital, which forced us to create a novel cost analysis model. The five main financial drivers chosen to analyze are the main drivers in spine fusion surgery; due the lack of accounting of all hospital charges, our figures will underestimate the overall charges incurred by the patient and insurance carriers. Also it should be noted that the financial data derived by our analysis are actually the theoretical charges and not the hospital purchase costs or resource utilization. Though most cost analyses use resource utilization as a methodology (as a proxy for social costs), we chose to highlight the impact onto the purchasers of healthcare, the patient and third-party payers, which can be perceived as a limitation of this study. In order to validate this analysis method, the actual charges from our children's hospital were compared with our calculated charges. A total of 14 patients (6 in the APSF and 8 in the PSF-TPS groups) had sufficient financial data available to compare with our model. After adjusting for inflation, using a consumer price index calculation (http://www.minneapolisfed.org/Research/data/us/calc/hist1800.cfm), the mean actual charges for the APSF group were US $80,323 and for the PSF-TPS group $77,109 (P > 0.05). The differences between the actual and calculated charges were $5,028 for the APSF group and $5,873 for the PSF-TPS group, which represents an increase of 6.7% and 8.2%, respectively, over the calculated financial analysis method. The variances are expected because minor hospital charges related to the surgery and postoperative care were not included in the financial analysis model. It is also necessary to point out that the costs at our institution may vary significantly from that obtained at other centers around the world.
Newton et al. [56] reported a comparison of ASF using an open thoracotomy or VATs performed from 1993–1994 over a 12-month period. Actual hospital charges for the VATs were US $54,910 ± $15,546, and for the open thoracotomy $48,025 ± $19,836. Adjusting for inflation to 2004 levels would increase the hospital charges for VATs to $71,782 and for open thoracotomy to $62,788, which are relatively in line with our findings. Another potentially perceived limitation of this study is the follow-up of 1 year postoperative. Due to this study focusing on the immediate perioperative medical financial data, we wanted to maximize our sample sizes for a more applicable analysis. Studies with longer follow-up on hook, hybrid, and TPS constructs have been reported previously and have demonstrated minimal loss of correction [23, 26–28].
Over the last 8 years, pedicle screws have become the favored method of spinal fixation in the treatment of spinal deformity at our institution. When pedicle screws can be safely placed, they are preferred over hook or wire fixation. However, certain situations exist that preclude safe placement of pedicle screws, such as small or absent pedicles, or in the presence of dural ectasias in Marfan's disease. It is in this situation we must resort to other construct configurations and spine fixation methods. Despite these issues, no anterior release has been performed at our institution for scoliosis less than 100°. In addition, with the improved ability to correct sagittal and coronal alignment that pedicle screw constructs can produce, it is essential to preoperatively plan the amount and type of deformity correction to correctly balance the patient.
This study analyzed the financial data relating to two methods of treatment for main thoracic curves between 70 and 100°: APSF with hook/hybrid constructs and PSF with TPSs. Despite higher surgical implant charges, the PSF-TPS group had equivalent charges when compared with the APSF group, due to lower anesthesiologist charges, operating room and inpatient room charges, and surgeon procedural charge. The concern about costs of TPS constructs does not appear valid when a circumferential fusion is avoided. While the use of circumferential fusion (APSF) is usually recommended for severe scoliosis, the use of TPS constructs in PSFs for AIS curves 70°–100° appears to be a safe and effective technique which, based on this analysis, is also financially equivalent.
