Abstract
Abstract
We describe a new anchoring method for tarsal tendon transfers in myelomeningocele patients to protect the sole of the foot from pressure sores and skin necrosis and to loosen the tension of the transferred tendon.
Tendon transfer procedures were performed in 51 feet (33 patients) with myelomeningocele. We transferred tibialis anterior tendons to the second or third cuneiform in 19 with equinovarus deformities, and transferred tibialis anterior tendons to the calcaneus through the interosseous membrane in 32 with talipes calcaneus. Clinical results were evaluated with the muscle power of transferred tendons using manual muscle testing 6 months after surgery. The muscle test result was classified as good, fair, and poor.
After passing the tendon through the bony hole, a 2.0-mm Kirschner wire was inserted from the sole to the tibia through the ankle joint at neutral. (It extended from the sole through the posterior cortex of the tibia.) The remaining part of the wire was bent and formed into a loop shaped like the Greek letter “zeta” (ζ). The thread was then tied to the loop of the wire as tightly as possible. In this way, there was no contact with the sole during anchoring, thus avoiding ulcers. In addition, the transferred tendon could be kept stable because the patient's ankle was fixed by the Kirschner wire.
No cases of wound infection or skin necrosis of the sole occurred. In 49 of the 51 cases, transferred tendons were firmly anchored to tarsal bones. Muscle strength was good for 83%, fair for 13%, and poor for 4%. Consequently, 45 feet could obtain plantigrade pattern during their walking with shoe inserts or occasional use of ankle-foot orthoses.
Our anchoring method has the advantage of protecting the sole of the foot from pressure sores and skin necrosis, as well as maintaining tension on the transferred tendon until it settles down in an anchor hole.
Introduction
Muscle imbalance in the lower extremity induces dynamic deformities of the foot. Thus, patients with myelomeningoceles associated with muscle imbalance often suffer from dynamic deformities of the feet. Good results have been reported for tendon transfers, which can effectively correct dynamic deformities by re-routing the deforming force induced by the loss of antagonist [1, 3, 4, 6, 8]. The technique of lateral tendon transfer of the tibialis anterior was first described by Garceau [5] and modified by Ponseti and Smoley [8]. Peabody first described the posterior tendon transfer of the tibialis anterior [7], and this procedure was modified by Geogiadis [4]. With both approaches, Cole's pull-out button method is usually used to anchor the transferred tendon as it is drawn tightly into the bony hole. However, this button often causes an ulcer of the foot due to the button exerting pressure against the skin [6]. Ulcers occur more frequently in myelomeningocele patients because of sensory loss. They cause the button to sink, loosening the tension of the transferred tendon, which in turn will lead to poor surgical results. Moreover ulcers themselves may cause serious problems, such as skin defects and superficial or deep infections.
We describe a new anchoring method to solve these problems that has yielded good results in our trials.
Patients and methods
We performed tendon transfer procedures in 51 feet (33 patients) with myelomeningocele: 22 patients had deformities of both feet—5 with equinovarus deformities of both feet, 13 with talipes calcaneus of both feet, and 4 with an equinovarus deformity of one foot and talipes calcaneus of the other; 11 patients had deformities of just one foot—9 with equinovarus deformities and 2 with talipes calcaneus.
We transferred tibialis anterior tendons to the second or third cuneiform in 19 feet (16 patients) with equinovarus deformities (lateral transfer) and tibialis anterior tendons to the calcaneus through the interosseous membrane in 32 feet (19 patients) with talipes calcaneus (posterior transfer). The average age at the time of operation was 6 years and 9 months (range 3 years and 6 months to 17 years). The average term of follow-up was 8 years and 4 months (range 6 months to 17 years and 9 months). In some patients, lengthening of the Achilles tendon, tibialis posterior tendon, or flexor hallucis longus tendon was performed concomitantly with the tendon transfer.
Clinical results were evaluated with respect to wound conditions on the soles during post-operative care and the muscle power of transferred tendons using manual muscle testing (MMT) 6 months after surgery. The muscle test result was classified as good (MMT = 5 or 4), fair (MMT = 3), or poor (MMT = 2, 1, or 0).
New anchoring method
We performed the modified procedure of lateral tendon transfer described by Ponseti and Smoley and the modified procedure of posterior tendon transfer described by Geogiadis since 1989, in conjunction with a new anchoring method to hold the transferred tendon effectively and safely. After passing the tendon through the bony hole, which is made in either the second or third cuneiform in the lateral transfer or in the calcaneus in the posterior transfer, a 2.0-mm Kirschner wire was inserted from the sole to the tibia through the ankle joint at neutral. It was inserted at a point approximately 3 cm anterior to the pulled-out thread on the sole and extended through the posterior cortex of the tibia. Approximately 1 cm below the sole skin, the wire was bent and formed into a loop shaped like the Greek letter “zeta” (ζ) (Fig. 1). The thread was tied to the loop of the wire as tightly as possible (Fig. 2), creating rebound force along the loop drawing the transferred tendon into the bony hole more tightly. To prevent proximal wire migration, the wire has to be inserted in an oblique fashion to pass it through two tarsal bones (calcaneus and talus) and the posterior cortex of the tibia.
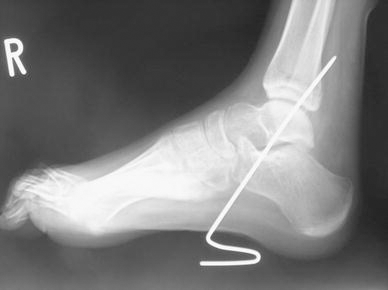
The Kirschner wire was inserted obliquely to pass through calcaneus, talus, and the posterior cortex of the tibia. Approximately 1 cm below the sole skin, the wire was bent and formed into a loop shaped like the Greek letter “zeta” (ζ).
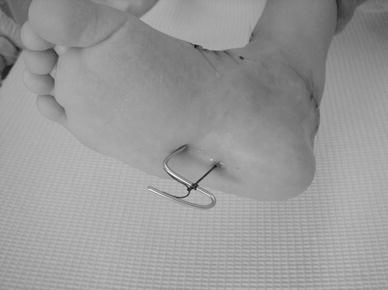
The Kirschner wire was inserted at a point approximately 3 cm anterior to the pulled-out thread on the sole. The thread was then tied to the loop of the wire as tightly as possible not to make the transferred tendon loosen
A short-leg plaster cast was applied for 6 weeks. At the end of the fifth week, it was cut to be bivalve and to remove the Kirschner wire and thread, modeling an ankle-foot orthoses (AFO). After modeling, the plaster cast was put on again. We removed the cast and permitted patients to stand up with the AFO after the end of the sixth week and to walk after the end of the eighth week.
Results
No cases of wound infection or skin necrosis of the sole occurred. In 49 of the 51 cases, transferred tendons were firmly anchored to tarsal bones. In 7 cases, we had to repeat the operation: 2 required postoperative extraction of the tendon from the bony hole due to persistent rigid equinus or non-adhesion; 3 developed a secondary deformity; and in 2 cases the deformity recurred. Of the 51 feet, 47 were assessed by means of MMT. Muscle strength was as good for 39 feet, fair for 6, and poor for 2. One of the poor results occurred in a foot that was one of the two cases that required postoperative extraction of the transferred tendon. The cause of the other poor result is unknown. Consequently, 45 feet were able to obtain a plantigrade pattern during their walking with shoe inserts or occasional use of AFO.
Discussion
Conventional tendon transfer methods have utilized a button tied tightly to the sole to keep the transferred tendon positioned firmly in an anchoring hole. However, foot ulcer formation from skin pressure exerted by the button represents one of the most serious problems for patients with sensory loss in the lower extremities [1, 2, 6]. Prevention of foot ulcers is difficult, even if the button is made from a soft material such as silicon [3]. The anchoring method described by Peabody involves burying the transferred tendon under an osteoperiosteal flap on the calcaneus at the insertion of the Achilles tendon [7]. However, this method results in the development of trophic ulcers at the site where the transferred tendon is buried [1]. In contrast, our anchoring method has the advantage of protecting the sole of the foot from pressure sores and skin necrosis, as well as maintaining tension on the transferred tendon until it settles down in an anchor hole. Furthermore, even if a transferred tendon were too short to perform the bound-up method around the anchoring hole, the tendon could still be anchored using our method, thereby avoiding the necessity of employing the bound-up method.
Our purpose here is to introduce the new anchoring method for tendon transfers in myelomeningocele patients, rather than report the long-term clinical result, although this is a very important issue. In discussing long-term results, many influencing factors would have to be considered, such as progression of paralysis, muscle weakness, increase of body weight, and social conditions. In this study, we assessed the short-term clinical result, which was affected purely by the surgical procedure itself. Thus, we examined the function of transferred tendon 6 months after surgery. Further long-term results will be reported at the next stage.
