Abstract
A successful strategy in regenerative medicine over the last decade has been the translation of stem cell therapy to repair diseased or damaged tissue in a wide range of indications, despite limited evidence attributing any therapeutic benefit to cell survival or differentiation. Recent findings, however, have demonstrated that the conditioned media from stem cell cultures can produce similar efficacious effects compared to those observed for cells. This has led to the stem cell paracrine hypothesis, proposing that secreted factors released from the stem cells contribute significantly to their beneficial effects. It has been well documented that stem cells have the ability to release a range of growth factors, cytokines and chemokines relevant to their function; however, these factors are released at levels too low to account for the reported therapeutic effects. Further purification of the conditioned media has since identified that not only are small molecules released by the stem cells, but so too are a large quantity of membrane-bound vesicles, including exosomes, in a functionally relevant manner. In this review, we present our current understanding and explore the evidence supporting the development of stem cell-derived exosomes as a cell-free regenerative medicine.
1. Introduction
One major approach to regenerative medicine has been to replace lost tissue with new cellular material or facilitate the regeneration of damaged or diseased tissues by means of stem cell transplantation. Over the last two decades, therapeutic options have progressed from the grafting of whole tissue (such as bone marrow) to the injection of autologous or allogeneic stem cell products derived from adipose, blood, bone and brain tissue. More recently, pluripotent cells derived from embryonic stem (ES) cells or induced pluripotent stem (iPS) cells, using cellular reprogramming technologies, have been the source of new potential cell therapies. The translation of stem cell therapies from bench to clinic has been remarkable, with thousands of trials currently registered in the National Institutes of Health clinical trials database (www.clinicaltrials.gov). The investigations span a broad range of indications, from microbial diseases, cancers and neoplasms, congenital, heart and blood disorders, nervous system diseases, immune disease (graft versus host, multiple sclerosis, arthritis and colitis), wounds and injuries. Results from the early phase trials have demonstrated cell therapy as safe, feasible and - in a number of indications - potentially efficacious, for example, in cardiology [1], ischaemic stroke [2], peripheral ischaemia [3] and cancer [4]. However, for many of these therapies, evidence of a therapeutic benefit cannot be attributed to stem cell survival and/or differentiation [5–7]. The beneficial effects of cell implants without long-term cell survival together with observed trophic effects of the cell-conditioned culture medium suggest that secreted paracrine factors may be involved [8, 9]. Small molecules (i.e., growth factors, chemokines and cytokines) are secreted at too low levels to account for the therapeutic efficacy reported [10]. However, the paracrine hypothesis has been strengthened by the recent discovery that stem cells release not only soluble factors but also extracellular vesicles which elicit similar biological activity to the stem cells themselves [11–14].
The most prominent of the extracellular vesicles are exosomes. Exosomes have been shown to play a key role in cell-to-cell communication [15–20] and modulating cellular immunity [21–24]. Recent data suggest that exosomes may physically link beneficial outputs from stem cells to neighbouring diseased or injured cells through the delivery and transfer of protein, bio-active lipid and nucleic acid cargo, inducing phenotypic and functional changes in the recipient cells that promote the activation of regenerative programs [25–28]. The paracrine hypothesis has inspired an alternative approach in regenerative medicine: namely, translating the potential clinical applications based on exosomes secreted by the stem cells rather than the stem cells themselves, an approach underpinned by the discovery of the control system for the transport and delivery of cellular cargo for which E. Rothman, R.W. Schekman and T. C. Südhof received the 2013 Nobel Prize for Medicine (www.nobelprize.org).
2. Formation, release and function of exosomes
Stem cell-derived exosomes have now been identified and isolated from cell culture supernatants of several cell types with known therapeutic potential, including mesenchymal stromal (MSC) [29–31], (bone marrow stem cells) mononuclear (MNC) [32], immune cells (dendritic and CD34+) [33, 34] and human neural stem cells (hNSCs) [35, 36]. Exosomes (30–100nm) can be distinguished from microvesicles (MVs) (100 nm-1μm) and apoptotic bodies (1– 5 μm) by size and morphology [37–39]. Exosomes are lipid bilayer-bound vesicles, released from cells after stimulation [40], and they express specific biomarkers independently of the cell source that will be detailed below. Unlike MVs, which are derived from plasma membrane shedding, exosomes are secreted by multivesicular bodies (MVBs) [38, 41–44]. Exosomes produced from a single cell can comprise a heterogeneous population of vesicles that may feature different markers, compositions and, potentially, different functions [40]. The heterogeneity of their composition, along with their stable physicochemical features, has led to the idea of using exosomes as natural nano-devices for the development of new therapeutic applications [45–48].
Once released into the extracellular environment, exosomes may interact with recipient cells via adhesion to the cell surface mediated by lipid-ligand receptor interactions, internalization via endocytic uptake, or by direct fusion of the vesicles and cell membrane, which leads to the release of exosome content into the target cell [15, 49]. The net result of exosome-cell interactions is the modulation of the physiology of the target cell, induced through any of several different mechanisms, ultimately influencing the biology of tissue/the organism as a whole. The interactions involve many physiological processes, such as antigen presentation [50, 51], the transfer of RNA [28] and tissue repair [30]. Exosomes have been found to carry antigenic materials and express functional major histocompatibility (MHC) complexes, giving them the potential to mediate antigen-specific immune responses [52]. For example, tumour-derived exosomes captured by dendritic cells can induce the activation of antigen-specific T-cells not previously exposed to the tumour antigen [21, 23], and the function of follicular dendritic cells has been attributed to membrane-bound exosomes containing MHC class II [53].
Exosomes can also influence the biology of recipient cells via the delivery of bioactive content into target cells through the internalization of vesicles. The bilayer membrane encapsulation of exosomes provides a protected and controlled internal microenvironment, allowing cargo to travel long distances within tissues without degradation [27, 28, 54–56]. Most recent developments implicate a major role for the horizontal transfer of proteins and genetic materials (such as mRNA, microRNA (miRNA), pre-miRNAs, and other non-coding RNAs) in the reprogramming of recipient cells. ES cell-derived exosomes have been demonstrated to shuttle/transfer mRNA and proteins to hematopoietic progenitors [26]. Other studies have shown that adult stem cell-derived exosomes also shuttle selected patterns of mRNA, miRNA and pre-miRNA associated with several cellular functions involved in the control of transcription, proliferation and cell immune regulation [57–60].
3. Exosomal features
3.1 Membrane composition
Besides their characteristic morphology, exosomes are unique in their bilayer membrane protein and lipid composition compared to other extracellular vesicles. Exosomal membrane components have been proposed as playing pivotal roles, such as signalling molecules in the uptake/fusion of exosomes with target cells and propagation of signalling in immune responses. For example, Rab GTPase membrane proteins have been implicated in membrane trafficking and secretion [61,62].
3.2 Lipid rafts
Lipid rafts are structurally and functionally unique microdomains in the cell membrane surface which function as sites for key membrane activities, such as endocytosis, cell adhesion and membrane trafficking [63]. Lipid rafts, tightly packed areas of sphingolipids and cholesterol compared to the surrounding areas, have been reported in both cellular and exosomal (including stem cell-derived) membranes [64]. As a consequence of the lipids' composition and limited size, exosomes have a more rigid membrane than their parent cell [65]. High levels of ceramide (associated with biogenesis and release) have also been reported in exosomes [66]. Lipid rafts reflect the endosomal origin of exosomes and represent a distinctive feature, which may be useful for their differentiation and isolation from other secreted microparticles [65].
3.3 Proteins
Exosome membranes comprise both ubiquitous and cell type-specific proteins that cover numerous biological functions. A complete database of exosomal proteins can be found at ExoCarta (www.exocarta.org) [67]. Due to their endosomal origin, all exosomes contain membrane transport and fusion proteins (annexins, GTPases, flotillin), tetraspanins (CD9, CD63, CD81, CD82), heat shock proteins (Hsp70, Hsp90), proteins involved in multivesicle body biogenesis (Alix and TSG101), lipid-related proteins and phospholipases [29,68]. These proteins have been associated with lipid rafts. Due to their size, lipid rafts can contain only a few proteins at one domain. To engage in a membrane function, lipid rafts cluster together and sequester specific sets of signalling and other proteins which serve as platforms to execute functions such as membrane trafficking and signalling [61].
Proteins presented on the outer exoplasmic membrane layer are routinely used as identifying markers; however, there is wide variation in terms of protein profiles across exosomes from different cell sources. The most widely-used markers are tetraspanins, Alix, flotillin, TSG101 and Rab5b, which are detected using antibody-based techniques (such as Western blot or ELISA) for the rapid confirmation of the presence of exosomes.
3.4 Cargo contents
Exosomal cargo can contain a variety of cytoplasmic nucleic acids, lipids and proteins, reflecting both the condition and origin of the parent or producer cell. As a result, exosomes exhibit some commonly shared contents and express distinctive molecules identifying their originating producer cell, but they also possess unique mixtures of proteins and RNA. The complexity of cargo contents has been postulated as a significant factor of exosomal efficacy in treating complex tissue injuries such as those that affect multiple tissues and targets [69]. Individual components in the cargo may not be equally or sufficiently efficacious, and the therapeutic efficacy of exosomes in relation to a specific injury may result from the synergy of a select permutation of individual exosome components. One aim of translational research is to assess the biochemical activities of these contents and identify the optimal permutations of these activities for therapeutic targets.
There is a growing need for quick and easy methods for the analysis of exosomal cargo. The thorough molecular characterization of exosomes is hindered by the complexity of their composition, their high heterogeneity and their low abundance. To date, only a few studies have been conducted that have provided a systematic characterization of the protein and the genetic composition of stem cell-derived exosomes [29, 35, 57, 58, 69–71] (Table 1).
A number of proteins have been identified in the functional cargo of stem cell-derived exosomes which affect a variety of cellular functions [14, 18, 26, 49, 72, 73]. Recent developments in protein separation techniques, spectrometry, immunological methods and bioinformatics have enabled the systematic characterization of MSC-derived exosomes [29, 68, 69] (Table 1). These analyses have identified over 700 proteins that reflect: (1) the evolutionary conserved set of exosomal proteins (CD81, CD63, CD9 [tetraspanins], Alix, Tsg101) and those tissue or cell type-specific proteins; (2) integration of parental cellular processes and genes of self-renewal and differentiation; and (3) a list of proteins that can be associated with therapeutic potential [29].
Examples of functional components isolated from stem cell-derived exosomes
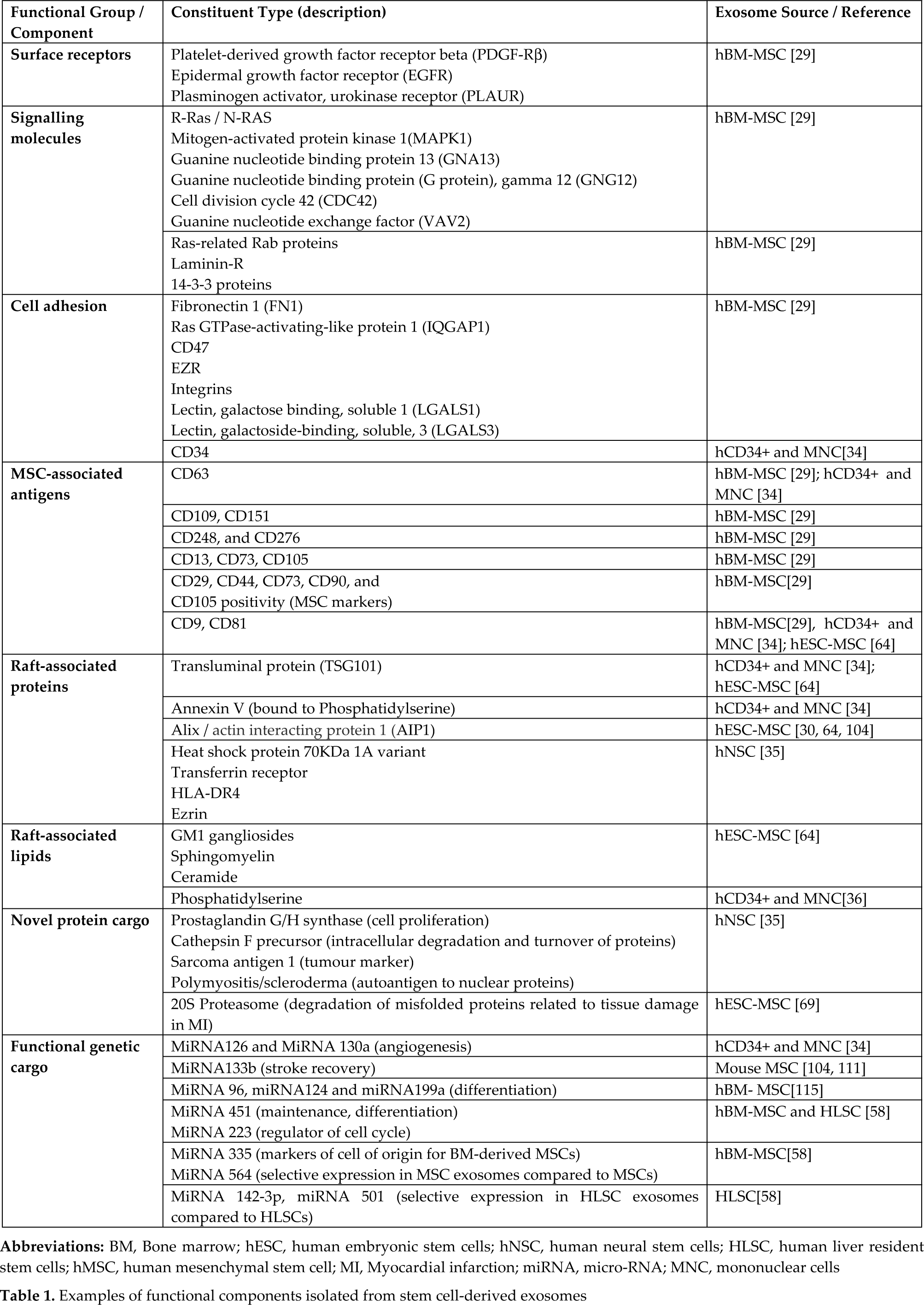
4. Proteomic characterization
Techniques such as Shotgun proteomic analysis of the peptide mixtures from exosomal fractions have been used to identify proteins from hNSCs [35]. A total of 103 proteins were detected in a sample of hNSC-derived exosomes, including previously reported heat shock 70 kDa, transferrin receptor, HLA DR4 and ezrin, and several as yet unreported such as anhydrolase-domain-containing-8, G protein-coupled receptor associated sorting protein 1, the 70 kDa heat shock protein 1A variant, and prostaglandin G/H synthase. Rarer proteins such as cathepsin F precursor and sarcoma antigen 1 which were also detected were uniquely present in only one fraction (Table 1).
5. Genetic information in stem cell–derived exosomes
Mitochondrial DNA, mRNA and non-coding RNAs such as miRNA have been reported in stem cell-derived exosomes and may deliver horizontal gene transfer to target cells [11, 74, 75]. Exosomes derived from human stem cells have been shown in vivo to deliver human mRNA to mouse cells, resulting in protein translation [76, 77]. Exosomes derived from ES cells contain abundant miRNA and have been demonstrated to transfer a subset of miRNAs to mouse embryonic fibroblasts in vitro [60].
MiRNA is a class of small, non-coding RNA molecules consisting of 19 to 24 nucleotides that have a variety of cellular properties associated with both physiological and pathological processes. They are involved in homeostasis, the post-translational modification of gene expression, oncogenesis and tumour suppression, RNA and protein complex shuttling, and protection from RNase enzymatic degradation [20, 78–83]. Exosomes provide a protected and controlled internal microenvironment, allowing miRNA molecules to travel long distances within tissues without degradation [54]. Evidence suggests that miRNA packaging occurs non-randomly and that specific miRNA populations are preferentially sorted and shuttled into MVs [84], and secreted contents could vary in response to different stimuli [58]. Important questions, regarding how miRNAs are sorted into exosomes (shedding vesicles and high density lipoprotein (HDL) particles), whether there is regulated specificity in this process, how secreted vesicles are taken up by recipient cells and whether specific cells are targeted, need to be addressed.
The transfer of human mRNA via exosomes and its translation into protein have been observed both in vitro and in vivo in diverse experimental models [28]. RNA inactivation resulted in the significant loss of biological activities, suggesting that the transfer of nucleic acids has a relevant role [85]. However, exosomes also transfer regulators of transcription as they induce changes in the gene expression of the recipient cells, such as the up-regulation of the BCL family genes and the down-regulation of CASP1 (caspase 1), CASP8 (caspase 8) and LTA (lymphotoxin α) genes involved in the “execution” phase of cell apoptosis [80].
Moreover, the miRNAs present in exosomes are candidates for the post-transcriptional regulation and induction of epigenetic changes in the recipient cells. miRNAs shuttled by EPC-derived MVs are the main effectors of the pro-angiogenic and renoprotective activities of MVs [79]. In fact, the non-specific as well as the specific depletion of miRNAs in MVs obtained from Dicer- or miRNA126- and miRNA-296-knockdown EPCs modify their biological effects [79, 86].
The number of secreted miRNAs identified in stem cell-derived exosomes has been expanding (Table 1) and their role and biological/physiological significance is of considerable interest. Stem cell types and their derived exosomes have distinct miRNA profiles [34, 86, 87], and are listed in http://exocarta.org/mirna and http://www.mirbase.org.
5.1 Producer cells
To ensure the large scale supply required for clinical research and development, producer cell immortalization (either by natural selection or by genetic modification) and clonal isolation is a practical strategy to produce functionally bioactive exosomes for use as therapeutic agents or delivery vehicles [47, 88, 89]. Immortalization ensures production stability and reduces the equivalence testing of new production lots. Bioreactors and other specialized culture systems are also used for culture expansion and to increase the yields of exosomes and MVs [88, 90]. In respect of genetically modified producer cells, the immortalizing oncogene (e.g., c-myc) and its protein product are not trafficked into the exosomes [88].
While secreted exosomes from a range of cell types exhibit some common shared contents, they also express molecules that reflect their cells of origin [44, 58, 71] and their microenvironment (e.g., culture conditions) [37, 91–93].
Exosomes are released from producer cells with stable phenotypes. The possibility of changing the phenotype of the exosomes represents a novel therapeutic strategy for cell-free regenerative medicine. Pre-treating the producer cells with different cytokine cocktails, etc., to drive a specific response [94], or stimulating/exposing producer cells - in effect mimicking cells' responses to a local diseased/damaged environment after implantation - can result in exosomes therapeutically suited to specific indication, as in cancer vaccines [95].
5.2 Preparation, isolation and manufacture of stem cell-derived exosomes
Efforts to harvest purified exosomes in clinically significant quantities are limited by the lack of tools and methods to differentiate them from microparticles in general and isolate different subsets. Most cell types produce exosomes; those produced by cultured cells are isolated from the conditioned media (Figure 1). Additionally, the yield from different cell types varies significantly. Within MSCs, for example, the production of exosomes from ES cell-derived MSCs is up to seven-times that from cord blood- or bone marrow-derived MSCs, suggesting a direct correlation between the donor cell ‘immaturity’ and exosome yield [96].
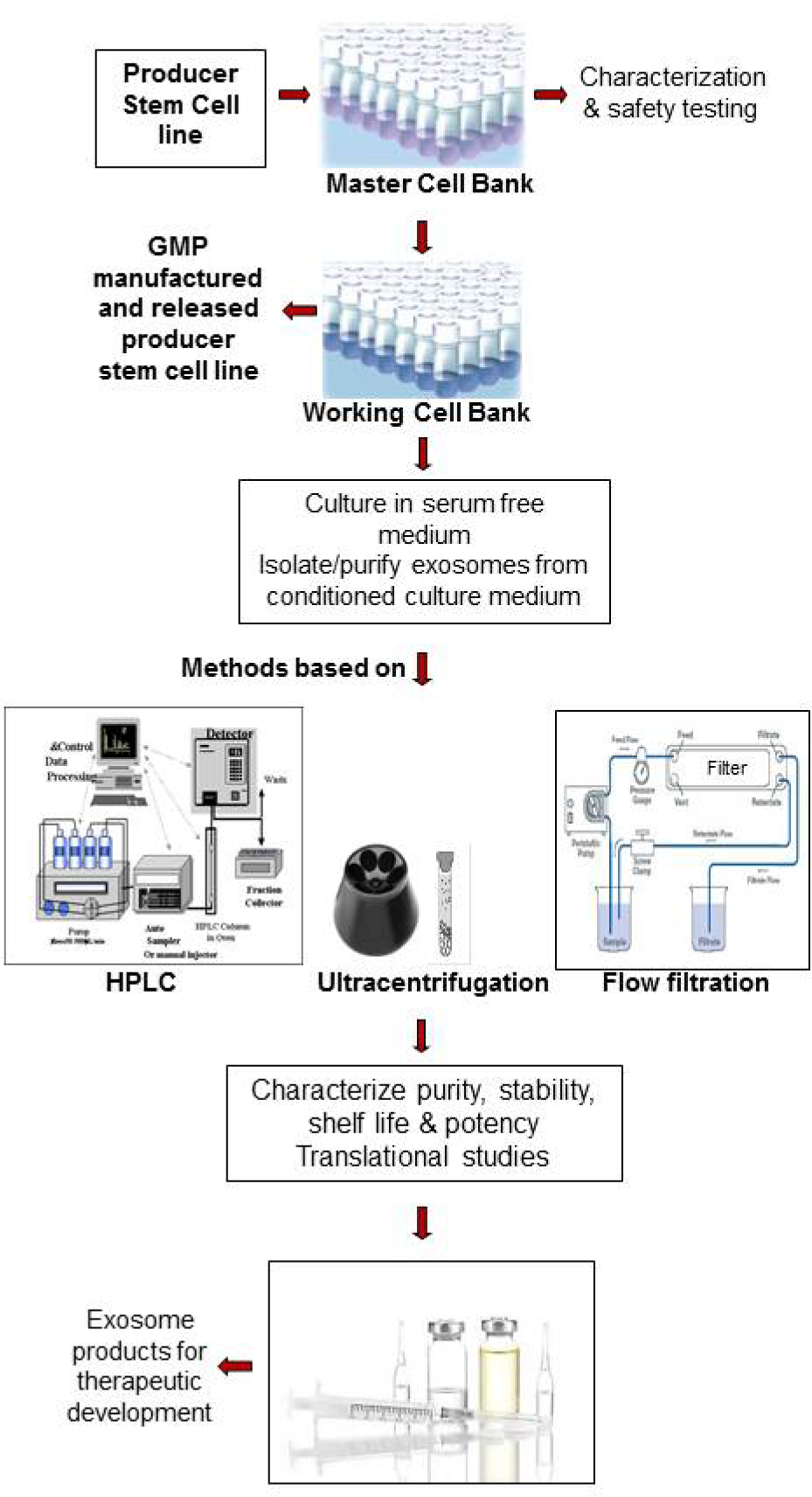
Overview of the isolation and manufacture of stem cell-derived exosomes
As yet, there is no agreed or standardized method for the preparation and purification of exosomes from cell-conditioned culture media (Table 2). MVs, exosomes, debris and culture media contaminants are all contained in the conditioned medium. Serum-free defined media may be used to reduce contamination with a serum or its components. Also, it is difficult to analytically distinguish exosomes from other membrane vesicles due to the limitations of commonly-used separation procedures, namely ultracentrifugation and flow cytometry [97]. The overall size of exosomes (<100 nm) has been an important criterion for distinguishing them from the other larger membrane-bound microvesicle secretions. Among current methods (differential centrifugation, discontinuous density gradients, immunoaffinity, ultrafiltration and high performance liquid chromatography (HPLC), differential centrifugation is the most commonly used for exosome isolation, which utilizes an increasing centrifugal force from 2000xg to 10,000xg to separate the medium- and larger-sized particles and cell debris from the exosome pellet at 100,000xg [33, 98–100]. Although crude and non-specific, this method has been reported to allow for the significant separation/collection of exosomes from a conditioned medium. However, protein aggregates, genetic materials, particulates from media and cell debris are common contaminants. To enhance the specificity of exosome purification, sequential centrifugation has been combined with ultrafiltration [98], or equilibrium density gradient centrifugation in a sucrose density gradient or Optiprep®, to provide for the greater purity of the exosome preparation (flotation density 1.1–1.2g/ml) [99] or sugar cushion [29, 33, 101].
The isolation of exosomes based on size is another option. Ultrafiltration can be used to purify exosomes without compromising biological activity. Membranes with different pore sizes - such as 100 kDa molecular weight cut-off (MWCO) and gel filtration to eliminate smaller particles - have been used to avoid the use of a non-neutral pH or non-physiological salt concentration [33, 100]. Currently available tangential flow filtration (TFF) systems are scalable (to >10,000L), purify and concentrate the exosome fractions [29] (www.pall.com), and are less time consuming than differential centrifugation. HPLC can also be used to purify exosomes to homogeneously-sized particles and preserve their biological activity as the preparation is maintained at a physiological pH and salt concentration [68, 88]. Although the purity of the exosome preparation is high, this method has poor scalability.
Exosome isolation methods from cell culture media
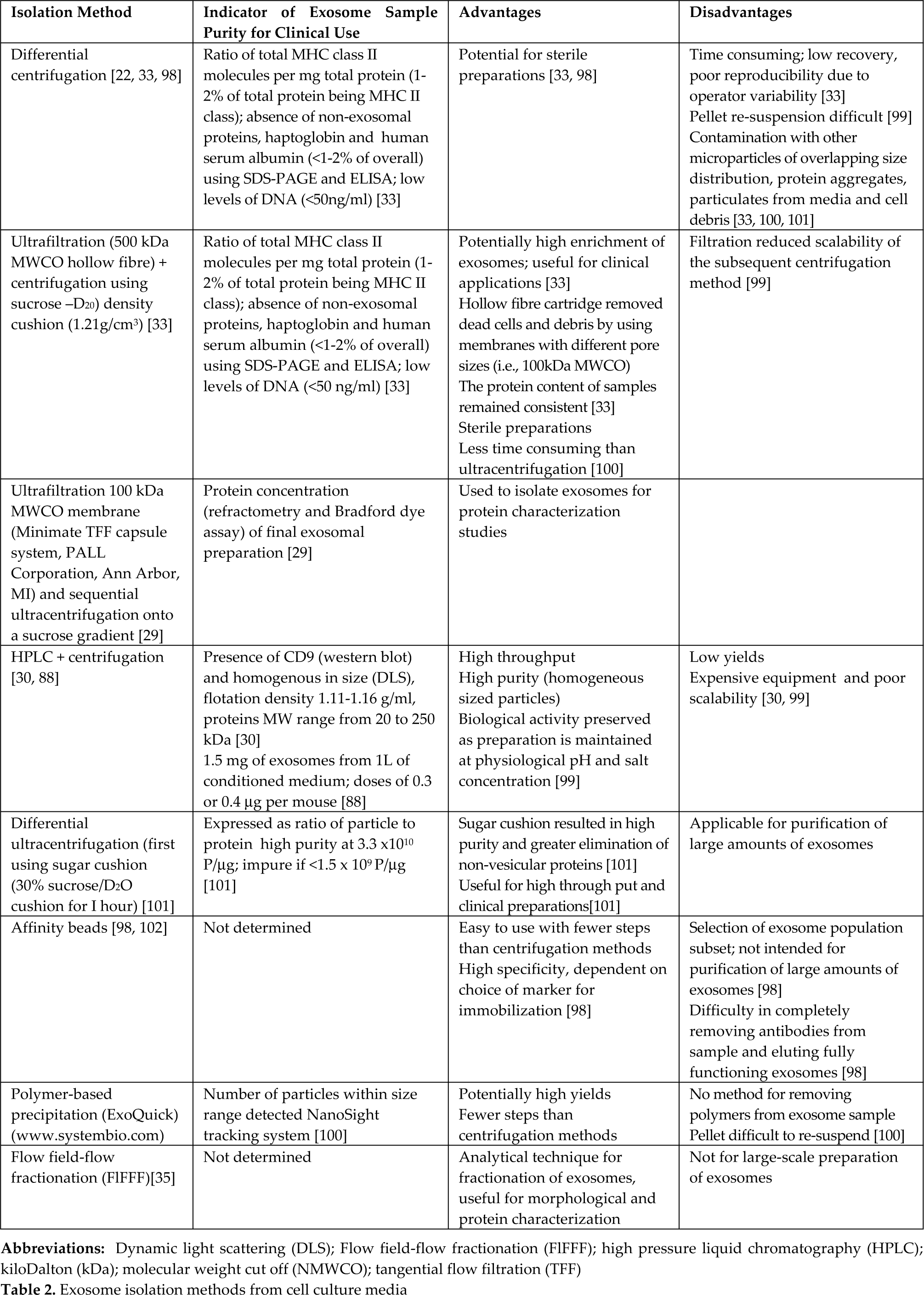
Immunoaffinity is a highly scalable technique using antibodies recognizing exosome-associated antigens conjugated to magnetic beads, chromatography matrices, plates or microfluidic devices [67, 88, 98, 102]. The antibodies can be used by themselves or in combination. For example, ExoTest® kits feature anti-CD63, -CD81 or - CD9 antibodies immobilized on 96 well plates for exosome capture and characterization (www.HansaBioMed.eu). Other affinity-capture methods use lectins which bind to specific saccharide residues on the exosome surface (www.AethlonMedical.com). The targets or markers for affinity capture need to be identified to optimize the high specificity offered by this technique.
Exosomes can also be purified by using differential solubility in volume-excluding polymers, such as polyethylene glycols (PEGs) and low-speed centrifugation or filtration. Based on this concept, System Biosciences has released a proprietary reagent called ExoQuick® that can be added to the conditioned cell media to precipitate the exosomes (www.SystemBio.com). The procedure has been reported as being fast and straightforward. However, it is not specific for exosomes and pellet re-suspension is difficult [100].
Flow field-flow fractionation (FlFFF) is an elution-based technique that is used to separate and characterize macromolecules (e.g., proteins) and nano- to micro-sized particles (e.g., organelles and cells) and which has been successfully applied to fractionate exosomes from hNSCs culture media [35].
Defining the purity of an exosomal preparation is critical to defining the product prior to any translational development [101]. The production of clinical-grade exosome products would require current Good Manufacturing Practice (cGMP). Exosomal products are more stable and easier to store and transport to the clinical site than stem cells [47]. The use of clinical-grade immortalized stem cell lines can reduce the time required for cell production, allowing cell banking and scalability, and thereby reducing production costs, and can also be of value in a strategy for GMP manufacturing [68, 88]. Also essential for the development of exosomes products are release assays, required for establishing the storage, shelf life and stability of the exosome products prior to clinical trials [46, 103].
6. Developing a stem cell-derived exosome product
6.1 Therapeutics
For clinical translation to be realized, it is necessary to characterize the physiochemical properties/phenotype of the purified exosome population along with the content and/or cargo of these vesicles in terms of proteins and small RNAs (Table 1). By addressing in an unbiased manner the genomic and proteomic content of the purified exosomes, it may be possible to predict the cellular targets and pathways that may be influenced.
Therapeutic approaches based on the delivery of miRNAs are currently being explored for cerebrovascular, myocardial and peripheral ischaemia. MSC-derived exosomes have been found to increase the miRNA-133b level when exposed to middle cerebral artery occlusion (MCAo) brain extracts [104]. MiRNA-133b is substantially down-regulated in the rat brain after MCAo. The therapeutic approach is to increase miRNA-133b in the brain tissue via exosomes to stimulate neurite outgrowth and improve functional recovery after stroke. Similarly, MSC-derived exosomes were also able to provide protection against myocardial ischaemia and treat myocardial infarction through the expression of higher levels of precursor forms of hsa-let-7b and hsa-let-7g miRNAs. CD34+ stem cell-derived exosomes are described as inducing angiogenic activity in isolated endothelial cells and in murine models of vessel growth. The benefit of CD34+ cell therapy for functional recovery after ischaemic injury could be induced by the exosome-mediated transfer of angiogenic factors to surrounding cells. Preliminary data on the mechanism that may mediate the enhanced potency of CD34+-derived exosomes have shown that the pro-angiogenic miRNAs 126 and 130a were highly expressed in CD34+ exosomes compared with other unselected MNCs [34].
In another study, protein profiling led to the identification of 20S proteasome using the ExoCarta database as a candidate exosome protein, with the therapeutic potential to ameliorate tissue damage after myocardial infarction [69]. Exosomes - as active components of conditioned medium from human ES cell-derived MSCs - injected into swine and murine models of ischaemia /reperfusion injury reduced the infarct size [30]; from bone marrow-derived MSCs, they accelerated repair in mouse models of acute kidney injury [77]; and from liver-derived stem cells, they induced proliferation and apoptosis resistance in cultured human hepatocytes [76]. Many more detailed functional studies are required to discover other candidate proteins and their therapeutic potential.
6.2 Clinical experience
Only one stem cell-derived exosome product has been used clinically to date [105]. In this first attempt, the administration of escalating doses of exosomes derived from donor bone marrow MSCs into a patient suffering from severe therapy-refractory cutaneous and intestinal graft-versus-host disease grade IV was found to be well tolerated and led to a significant and sustainable decrease of symptoms. A small number of clinical trials are currently investigating dendritic cell-derived exosomes for immunotherapy or vaccination in severe cancers, such as non-small lung (Phase II, NCT01159288) [106], glioma (Phase I NCT01550523) [107] and gastric (Observational, NCT01779583), and with Phase I trials in non-small lung small lung ([108], colorectal [109] and melanoma [110] completed. Interestingly, the use of plant-derived exosomes as vehicles to deliver curcumin to treat colon cancer is also under scrutiny (Phase I, NCT01294070).
6.3 Advantages/limitations of exosome therapeutics
The research to date indicates that stem cell-derived exosomes potentially have significant clinical utility. Exosome-based, cell-free therapies - in contrast to cell-based therapies in regenerative medicine - can be generally easier to manufacture and prima facie safer, as they are non-viable and will not form tumours. By replacing the administration of live cells with their secreted exosomes, many of the safety concerns and limitations associated with the transplantation of viable replicating cells could be mitigated.
Stem cell-derived exosomes have generally been found to be less immunogenic than parental cells, as a result of a lower content of membrane-bound proteins, such as MHC complex molecules [10]. Thus, ‘off-the-shelf’ products may be readily developed using exosomes with negligible alloimmunogenicity.
Cell-free products offer a number of advantages compared to cell transplantation. Exosomes – in a manner similar to conventional biopharmacological products - can be standardized and tested in terms of dose and biological activity. Exosomes can be stored without potentially toxic cryopreservatives at −20°C for six months with no loss to their biochemical activity [100].
An important feature of exosomes is the encapsulation and protection of their contents from degradation in vivo, thereby potentially preventing some of the problems associated with small soluble molecules such as cytokines, growth factors, transcription factors and RNAs, which are rapidly degraded [28].
The durability of exosomes in culture allows for the acquisition of large quantities of exosomes through their collection from a culture medium in which the exosomes are secreted over periods of time.
Scalable systems for exosome production to support large-scale commercially viable manufacturing processes need to be developed.
While exosomes exhibit several attractive features as a therapeutic agent, there are also potential limitations to be considered as well. Exosomes contain a mixture of biologically active molecules, some of which seem to have beneficial effects, whereas others might have detrimental (e.g., proinflammatory) effects under certain conditions. Whether exosomes will turn out to be superior to angiogenic drugs or purified recombinant growth factors and other peptides within the context of cell-free approaches to tissue regeneration remains to be seen.
In addition, these naturally-occurring secreted membrane vesicles are better tolerated in the body, as evidenced by their ubiquitous presence in biological fluids, and have an intrinsic homing ability. In contrast to cell-based therapy, stem cell-derived exosomes provide an ‘off-the-shelf’ therapeutic product and will incur less manufacturing and storage costs.
Similarly, most stem cells can be readily genetically modified, either by integrating viruses or episomal transfection. It is known that the overexpression or knock-down of miRNAs can result in similar over- or under-expression in exosomal cargo [79, 104, 111–113]. This has been exploited in preclinical studies where genetically modified exosomes have shown relevant therapeutic outcomes [78, 104, 111–114].
6.4 Clinical and regulatory considerations
While the application of stem cell-derived exosomes remains largely untested by regulatory authorities in advance of clinical trials, it is likely that these products will be seen in a similar way to their parent cells.
Safety testing will focus on systemic bio-distribution, toxicity/tolerability and half-life studies. Compared to stem cell therapy, exosomal products can be delivered more readily by less sophisticated and more conventional delivery devices as the formulation and stability will be similar to biologics. Repeat administration and even self-administration may also be possible in the future due to more straightforward product presentation. In addition, the much lower cost of such goods will be attractive to healthcare funders.
7. Future scope
The number of peer-reviewed publications focusing on exosomes has increased exponentially over the past decade. The newly founded International Society for Extracellular Vesicles (ISEV) is seeing a rapid rise in the number of presentations on the therapeutic use of exosomes. Much excitement and promise has been generated around the use of exosomes in cell-free regenerative medicine, which offers the potential for safer, low risk products to cover a wider range of applications. Databases such as ExoCarta have facilitated the sharing of data regarding the genomics and proteomics of exosomes. As this data continues to accrue, it will become important to determine which factors are most relevant to exosome functions. Also key to exosome product translation will be advances in GMP supply and the production of clinical grade products, product characterization and potency assays, preclinical proof of efficacy and the identification of target populations. Although some exosomal preparations are already being administered in the clinic, the regulatory road map for stem cell-derived exosome product translation to clinical application will need to be established soon so as to keep pace with research demands.
Footnotes
Conflicts of interest: I. Vishnubhatla, R. Corteling, L. Stevanto, C. Hicks and J. Sinden are ReNeuron employees. No part of this study was performed on any human or animal subjects.
