Abstract
The incidence and prevalence of congestive heart failure are actually increasing worldwide, especially in Western countries. In Europe and the United States, congestive heart failure represents a disabling clinical disease, accountable for increased hospitalization and health care costs. European guidelines have underlined the importance of pharmacological treatment to improve both patients' outcomes and quality of life. The latest clinical trials to evaluate ivabradine's efficacy have underlined its usefulness as a stand-alone medication and in combination with conventional congestive heart failure therapy, including in chronic kidney disease patients.
Introduction
Chronic heart failure (CHF) represents a major cardiovascular morbidity and mortality factor in Western countries. Mortality rates are about 50% in people aged over 65, despite undeniable advances in pharmacological treatment with the introduction of beta-blockers, angiotensin-converting enzyme inhibitors (ACEis) and angiotensin receptors blockers (ARBs) during the last 2 decades.
The incidence of heart failure (HF) is actually increasing in line with the population's age: from 2.5/1,000 person-years for those aged between 55 and 64, to 44/1,000 person-years for older patients (over 80). At present, the prevalence of heart failure (HF) is approximately 0.4%-2% in people aged between 50 and 65 years, up to 10% in people aged over 75. CHF is much more common among those patients with systolic or diastolic dysfunction than in those with normal ventricular function. However, even among those with moderate or severe diastolic or systolic dysfunction, less than half have recognized CHF (1).
Based on these data, it becomes clear that heart failure (HF) is accountable for the majority of incident hospital admissions in people aged over 65. Health care costs etc etc for CHF are about 1%–2% of the entire health care budget in Western countries.
CHF etiopathogenesis is multifactorial, but coronary syndrome (both acute and chronic) still represents the main cardiovascular disease leading to heart failure (HF) (1). Heart failure's (HF) pharmacological treatment has gradually been developed during the last 3 decades for both acute (i.e. levosimendan) and chronic (beta-blockers, ACEis and ARBs) disease (1).
Recent trials have highlighted the importance of cardiac heart rate as a negative prognostic factor in cardiovascular diseases (including heart failure) (2–5). Based on this evidence, beta-blockers represent ideal pharmacological agents because of their effects on heart rate and myocardial oxygen consumption, especially in those patients with chronic ischemic heart disease (2, 3).
Low beta-blockers dosages can induce significant clinical improvement in left ventricular systolic function (40% reduction in mortality and hospitalization rates, and about a 30% increase in left ventricular ejection fraction), also providing progressive reduction of cardiac chamber diameters (2–4).
Clinical data from major randomized clinical trials (MDC, CIBIS-II, MERIT-HF) suggest that all patients with stable mild to moderate systolic heart failure (NYHA class I-III) should take advantage of beta-blocker therapy (5). Unfortunately, about 25% patients with CHF cannot receive beta-blockers, due to diabetes, multivessel disease and chronic obstructive pulmonary disease (4). Beta-blocker therapy also involves side effects such as the development of asthenia and heart rate impairment, which limit its widespread administration (4, 5).
The first evidence of heart rate's prognostic significance in cardiovascular disease outcomes was in Levy's results published in 1945 (6). More recent evidence has underlined the close association between heart rate and cardiovascular events (especially fatal events such as sudden cardiac death) in patients with acute coronary syndrome and heart failure.
Mortality rates increase together with heart rate, especially for heart rates between 70 and 90 beats per minute bpm) (7–10); therefore, a resting heart rate increase represents an independent cardiovascular mortality factor and is accountable for fatal cardiovascular events in patients with chronic and stable ischemic cardiopathy (11, 12).
Ivabradine: pharmacological profile and clinical application
Ivabradine is an inhibitor of mixed Na+-K+ current that can combine with hyperpolarization-activated cyclic nucleotide-gated (HCN) channels to reduce the transmembrane velocity of funny current (I
Ivabradine is a selective and specific I
Ivabradine is mainly used for the treatment of several cardiovascular diseases, including CHF and stable angina pectoris in adults with heart rate at rest above 70 bpm, with beta-blocker intolerance; alternatively, ivabradine can be added to standard beta-blocker therapy in NYHA class II to IV patients with systolic dysfunction and heart rate at rest above 75 bpm (20).
Ivabradine treatment seems not to interfere with renal function in CHF patients, and all cardiovascular outcomes improve both in patients with impaired renal function and in those without renal damage (21).
Based on available data, ivabradine can enable a strong reduction of cardiovascular mortality and hospitalization rates in CHF patients, together with reduction of mortality rates and rehospitalizations for acute heart failure (21).
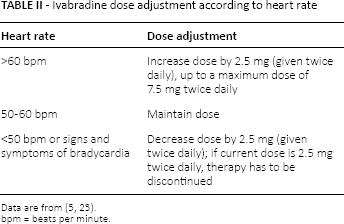
The European Society of Cardiology (ESC) has suggested administration of ivabradine (as stand-alone medication or added to standard beta-blocker therapy) in both chronic coronary heart disease patients with heart rate ≥70 bpm and CHF patients with heart rate ≥75 bpm (22). Tables I and II show standard ivabradine's dosage and adjustments according to heart rate.
Standard ivabradine dosages in management of heart failure patients
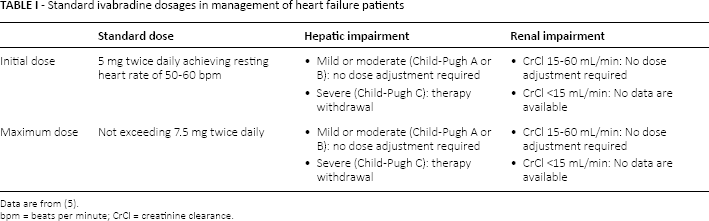
Data are from (5).
bpm = beats per minute; CrCl = creatinine clearance.
Ivabradine and clinical trials
The BEAUTIFUL trial
The Morbidity-Mortality Evaluation of the I
Inclusion criteria were verified stable chronic coronary disease in the last 3 months, echocardiography-assessed left ventricular dysfunction, heart rate at rest of ≥60 bpm and presence of normal sinus rhythm. The primary end point was a composite of cardiovascular mortality, hospitalization for acute myocardial infarction and hospitalization for incident or worsening of previous heart failure. Secondary end points were global mortality, cardiovascular-related mortality, hospitalization for heart failure, acute myocardial infarction or unstable angina and coronary revascularization surgery outcomes.
The aim of the study was to assess efficacy of heart rate reduction on the above described cardiovascular end points by ivabradine therapy.
The BEAUTIFUL trial's conclusions were that reduction in heart rate with ivabradine does not improve cardiac outcomes in all patients with stable coronary artery disease and left-ventricular systolic dysfunction, but could be used to reduce the incidence of coronary artery disease outcomes in a subgroup of patients who have heart rates of 70 bpm or greater. Therefore a post hoc analysis was proposed that ivabradine may reduce major cardiovascular events in patients with stable coronary artery disease and left ventricular systolic dysfunction who present with limiting angina. The results also suggested that there is no indication for treating patients with a heart rate less than 70 bpm with ivabradine if they have significant left ventricular dysfunction (ejection fraction 40%) and do not have symptoms of limiting angina (24).
The SIGNIFY trial
The Study Assessing the Morbidity-Mortality Benefits of the I
After a median 27.8-month follow-up period, the authors concluded that addition of ivabradine to standard background therapy to reduce heart rate did not improve outcomes among patients who had stable coronary artery disease without clinical heart failure.
There are several hypotheses to explain the lack of benefit with ivabradine in the SIGNIFY trial; it is possible that ivabradine decreased the heart rate too much, or there may be a J-shaped curve for the relationship between heart rate and outcome (25).
The SHIFT
The Systolic Heart Failure Treatment With the I
Patients who received ivabradine showed significant primary (18%) and secondary end point reduction (26%), supporting the importance of heart rate reduction with ivabradine for improvement of clinical outcomes in heart failure and confirming the important role of heart rate in the pathophysiology of this disorder (26).
A subgroup analysis indicated that the effects of ivabradine on the primary clinical outcome of SHIFT, and its components, were not significantly impacted by beta-blocker dose. Any borderline nonsignificant trends were significantly weakened by adjustment for the previously identified interaction between baseline heart rate and ivabradine treatment. This suggests that any impact of background beta-blocker treatment on the effects of ivabradine are, if anything, marginal and that the critical factor driving the benefits of ivabradine treatment is heart rate (23).
Ivabradine and chronic kidney disease
Clinical trials on ivabradine use in chronic kidney disease are lacking at present time. In 2008, data regarding the role of heart rate as a mortality prognostic factor in hemodialysis patients were published by Cice et al (27). Four hundred and seven normotensive end-stage renal disease (ESRD) patients (mean age 56.6 ± 3.3 years) without coronary artery disease or left ventricular systolic dysfunction or on antiarrhythmic therapy were enrolled. Baseline electrocardiography (ECG) at rest, 48-hour ambulatory Holter ECG monitoring and standard echocardiography were performed. After a mean follow-up of 46 months (range 12–60 months), cardiovascular and sudden death were considered as primary composite end points. Echocardiogram showed a normal left ventricular ejection fraction in 91% patients and left ventricular hypertrophy in 71%. Mean heart rate by 48-hour Holter ECG was 81 ± 10.6 bpm. During the follow-up, the all-cause mortality rate was 12%, while 9.8% patients died from cardiac causes (4.9% by sudden cardiac death). By univariate analysis, age, diabetes, left ventricular hypertrophy and increased mean heart rate by 48-hour Holter ECG were all significantly related to global, cardiovascular and sudden death. Receiver operator characteristic curve analysis identified optimal cutoff points for heart rate at >85 bpm and age >65 years associated with increased cardiovascular risk (p< 0.001). The authors concluded that in normotensive ESRD patients, increased mean heart rate detected by 48-hour Holter ECG is an independent determinant of global and cardiovascular mortality. Therefore, increased mean heart rate is directly related to left ventricular systolic dysfunction, easily assessed by color Doppler echocardiography, which provides transmitralic flow and left ventricular refilling pressure data. ESRD patients present severe diastolic dysfunction due to left ventricular hypertrophy (and consequent myocardial fibrosis), chronic ischemic coronary disease, calcium overload and storage leading to diastolic filling impairment and myocardial fibers abnormally relaxing, together with abnormalities in heart rate and rhythm (27).
In 2006, ivabradine was tested (7.5 mg twice daily) in hemodialysis patients with higher heart rate at rest, and heart failure, both diastolic (54%) and systolic (46%) (28). After 6 months of therapy, weekly mean heart rate was lower in patients treated with ivabradine both predialysis and postdialysis. When ivabradine was added to therapy for hemodialysis patients with congestive heart failure and preserved ejection fraction, it showed positive effects on left ventricular diastolic dysfunction, as underlined by decreased left ventricular isovolumetric relaxing time (Tab. III).
Ivabradine: effects on left ventricular diastolic function
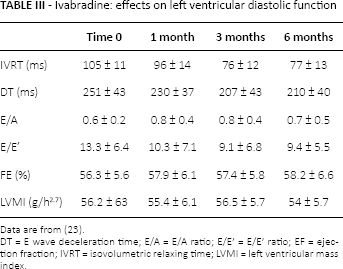
Data are from (23).
DT = E wave deceleration time; E/A = E/A ratio; E/E' = E/E' ratio; EF = ejection fraction; IVRT = isovolumetric relaxing time; LVMI = left ventricular mass index.
Ivabradine therapy also led to an improvement of left ventricular systolic function, with an increase of mean ejection fraction and shift toward lower NYHA classes, according to the SHIFT results (21, 28).
Ivabradine can also be helpful in treating inappropriate sinus tachycardia (1ST) characterized by unexplained tachycardia (heart rate >100 bpm) and related symptoms at rest. IST can be observed in ESRD patients and renal transplant recipients. Ivabradine can be used as an alternative to beta-blockers and calcium channel blockers for management of IST when these agents are not tolerated or an overdose is to be avoided (29).
Conclusions
The benefit of a decrease in heart rate for patients with chronic coronary artery disease and CHF is a reduction in cardiovascular mortality rates. Beta-blocker agents have improved patients' outcomes, but they are often administered at unsuitable doses.
Ivabradine, as stand-alone medication or in association with beta-blockers, seems to be more effective in improving patients' quality of life in the presence of coronary artery disease or CHF with heart rates above 70 bpm. In heart failure patients, ivabradine decreases cardiovascular mortality and heart failure hospitalization rates. The beneficial effects of ivabradine therapy become evident in both ischemic and nonischemic disease–related heart failure.
In chronic kidney disease patients with glomerular filtration rates (GFR) above 15 mL/min per 1.73 m2, no dose adjustment seems to be required. At present, no data for patients with GFR <15 mL/min per 1.73 m2 are available, although efficacy and safety may be preserved in these patients too; more trials are needed, and ivabradine should be used carefully or avoided in ESRD patients.
Footnotes
No grants or funding have been received for this study.
None of the authors has any financial interest related to this study to disclose.

