Abstract
Purpose
To report the association of polyneuropathy, organomegaly, endocrinopathy, monoclonal gammopathy, and skin changes (POEMS) syndrome with bilateral papilledema and bilateral choroidal neovascularization (CNV) in a 61-year-old man and to compare our findings with data from a review of the literature.
Case report
Diagnosis of POEMS syndrome was based on paraproteinemia immunoglobulin A lambda associated with progressive sensorimotor peripheral neuropathy and increased serum vascular endothelial growth factor (VEGF) levels. Shortly later, loss of vision of the left eye (LE) was noted and bilateral papilledema was observed with peripapillary hemorrhages and papillomacular subretinal fluid. Lenalidomide 25 mg daily and weekly dexamethasone 20 mg were administered and the patient was followed up closely. The systemic complaints initially were controlled and peripheral neuropathy improved. Regression of the papilledema and hemorrhages was observed as well as regression of the papillomacular edema in the LE. However, after a few months, the systemic VEGF levels increased, and an active CNV was diagnosed in the LE. Melphalan and prednisone were administered systemically, and the CNV was treated with bevacizumab intravitreal injections and these treatments proved to be effective.
Conclusions
Optic disc edema is reported frequently in POEMS syndrome but complication with CNV is rare, this being the second reported case.
Introduction
Polyneuropathy, organomegaly, endocrinopathy, monoclonal gammopathy, and skin changes (POEMS) syndrome is a rare paraneoplastic disorder secondary to an underlying cell dyscrasia. Recently, criteria for the diagnosis of POEMS syndrome have been reported (1). Mandatory criteria are polyneuropathy, typically demyelinating, and monoclonal plasma cell proliferative disorder, almost always lambda. Additionally, to confirm diagnosis of POEMS, patients have to present with at least one of the other major criteria and at least one of the minor criteria (1, 2; Tab. I). The most common ocular abnormality is bilateral optic disc edema, being present in half of the patients with POEMS who underwent an ocular examination (3, 4; Tab. II). We describe the ocular findings in a patient who fulfilled the criteria for POEMS syndrome and report bilateral papilledema and unilateral active choroidal neovascularization (CNV), a complication described only once previously (5).
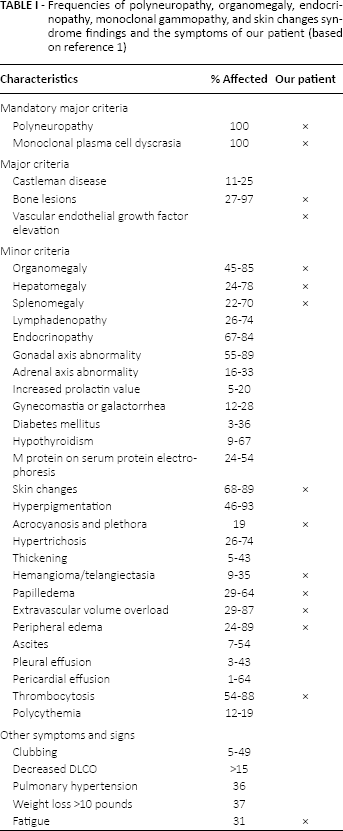
Frequencies of polyneuropathy, organomegaly, endocrinopathy, monoclonal gammopathy, and skin changes syndrome findings and the symptoms of our patient (based on reference 1)

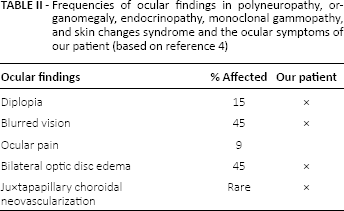
Frequencies of ocular findings in polyneuropathy, organomegaly, endocrinopathy, monoclonal gammopathy, and skin changes syndrome and the ocular symptoms of our patient (based on reference 4)
Case presentation
A 61-year-old man had a 1-year history of progressive demyelinating polyneuropathy and a monoclonal plasma cell proliferative disorder, responsible for loss of sensitivity in limbs, pain, weakness, and walking problems. Several weeks later, he developed malleolar edema, dermal angiomas, hepatomegaly, and splenomegaly. Based on the presence of the mandatory criteria as well as a number of other major and minor criteria, the suspected diagnosis of POEMS was confirmed (Tab. I), and treatment consisted of plasmapheresis (without result), lenalidomide 25 mg daily (Revlimid), and weekly dexamethasone 20 mg.
One month later, in August 2016, the patient was referred to our department because of complaints of diplopia and metamorphopsia. On examination, the best-corrected visual acuity was 20/33 in the right eye (RE) and 20/67 in the left eye (LE). No abnormalities were noted in the anterior segment. Ocular examination revealed a left divergent strabismus. Ocular motility was normal as well as pupillary reaction. Funduscopic examination showed bilateral papilledema with peripapillary hemorrhages and in the LE papillomacular subretinal fluid (Fig. 1, A-D). Ocular motility was normal, as was pupillary reaction, and no anterior segment abnormalities were noted. Fluorescein angiography (Heidelberg HRA 2-KT-00725) and optical coherence tomography (Zeiss Cirrus HD OCT model 5000) confirmed the papilledema with prominent disc leakage and showed papillomacular abnormalities with serous subretinal detachment and masking due to hemorrhages (Fig. 1, C-H).
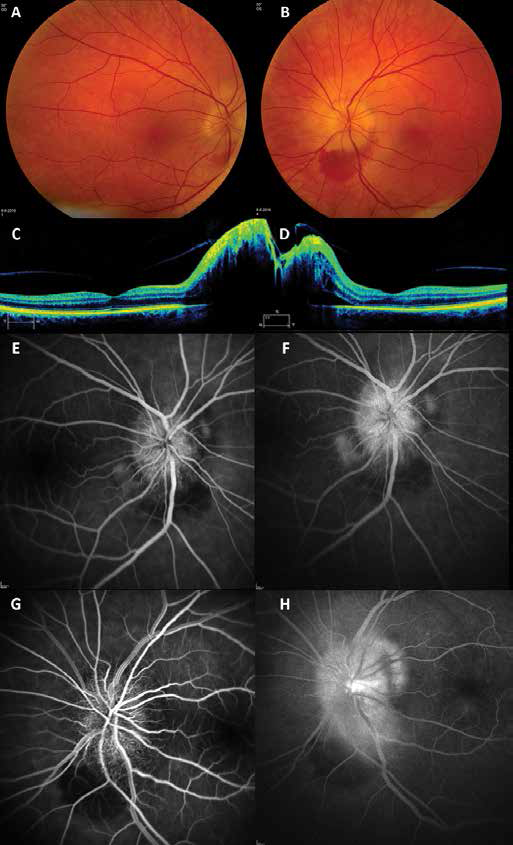
First visit, August 2016. (
Cranial computed tomography (CT) and magnetic resonance imaging did not show optic nerve infiltration or intracranial pathologic findings.
Over the following months, we observed spontaneous partial regression of the papilledema and a resolution of the hemorrhages. The patient received 7 treatments with Revlimid and dexamethasone; then the systemic therapy was changed to melphalan and prednisone as the systemic complaints did not resolve and vascular endothelial growth factor (VEGF) levels had increased.
A follow-up visit in February 2017 showed bilateral peripapillary retinal pigment epithelial (RPE) changes and these changes were marked in the papillomacular area, where CNV was suspected (Fig. 2, A-B; Topcon TRX-50DX Type IA). Fluorescein angiography and spectral-domain optical coherence tomography (Heidelberg Spectralis OCT) (Fig. 2, C-H) showed a localized CNV in the RE, without edema of the overlying retina, and this CNV was observed closely without anti-VEGF treatment. In the LE, the CNV was active with retinal and subretinal fluid and leakage of dye and treatment with bevacizumab intravitreal injections was instituted. Two injections with bevacizumab were given.
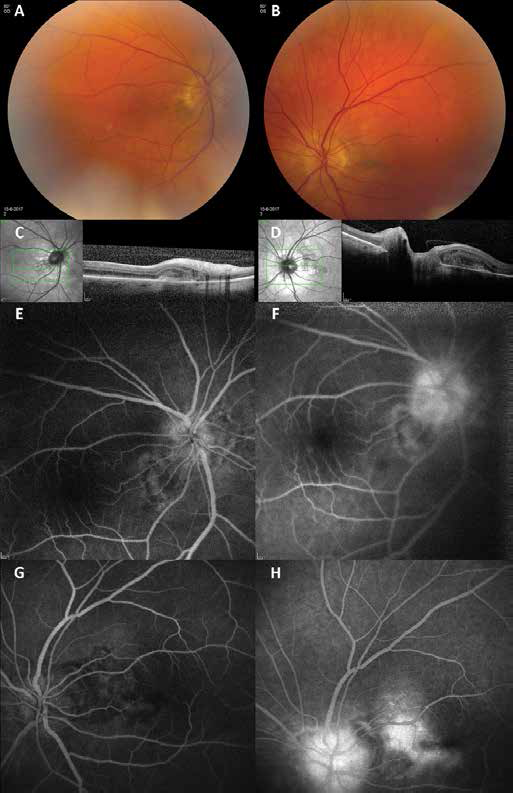
Follow-up visit in February 2017. Fundus photograph of the right (
At the last visit, 3 months later, in May 2017, the optic disc showed leakage but the CNV appeared inactive on both sides. Positron emission tomography CT showed an isolated osteosclerotic bone lesion, treated with radiotherapy.
Discussion
As POEMS syndrome is a multisystem disorder with variable clinical expression, its identification can be delayed or missed. The diagnosis is based on clinical suspicion of the syndrome and confirmation is based on obligatory criteria, major criteria, and minor criteria (1) (Tab. I). The pathogenesis of POEMS syndrome is complex and not fully understood. Several systemic factors are involved but VEGF hyperproduction is considered to be a major contributor to the development of POEMS. On the other hand, systemic anti-VEGF treatment has not been very effective and overall showed variable results, indicating that VEGF is probably only one component of many in a complex cytokine process (6, 7). Treatment of POEMS syndrome usually consists of radiotherapy and/or systemic therapy. For up to 3 isolated plasmacytomas, radiation is the preferred treatment, and for widespread lesions, chemotherapy is indicated (1, 2).
Ocular abnormalities (4) (Tab. II) can be subtle and overseen, or the patient can complain of diplopia as a result of intracranial pressure causing oculomotor abnormalities. The ophthalmic findings that have been reported in POEMS syndrome are papilledema, cystoid macular edema, serous macular detachment, infiltrative orbitopathy, and venous sinuous thrombosis (4). Papilledema occurs in more than 50% of cases, is mostly bilateral, and results from elevated intracranial pressure, but infiltration of the optic nerve, elevated VEGF, and interleukin-6 causing vascular hyperpermeability could be contributing factors. Systemic VEGF might alter optic nerve head vascular permeability via the choroidal blood flow (7). A significant correlation between serum level of VEGF and subfoveal choroidal thickness was present in patients with POEMS syndrome (8).
The initial clinical presentation of papilledema varied, with 73% of patients having blurred vision and 29% of patients being asymptomatic (4). Loss of vision noted by some patients seems to result from chronic papilledema and papillomacular retinal edema. The patient we report had persistent papilledema despite a combination of treatments. As a complication of the chronic papilledema, RPE lesions and a CNV developed. Aside from these RPE lesions predisposing to CNV growth, elevated VEGF levels may have been predisposing to CNV development.
An ocular examination is indicated in patients with suspected or proved POEMS syndrome as chronic papilledema and subsequent loss of vision occurs in more than 50% of patients with POEMS. The chronic papilledema can also predispose to peripapillary RPE abnormalities and to growth of CNV. In the literature, there is only one report of the development of a peripapillary CNV, and the authors suggested that this supports the role of elevated VEGF levels in the pathogenesis (5). Choroidal neovascularization can remain localized in the peripapillary area with limited activity not requiring anti-VEGF treatment, as shown in the RE of our patient, or can be large, active, and responsible for marked edema and visual loss, as shown in the patient's LE. Anti-VEGF intravitreal injections are useful to induce inactivation of active CNV and could also have benefit to limit other complications of the papilledema. Knowledge of the ocular complications of POEMS is required to allow timely identification and treatment of papilledema and CNV.
Footnotes
Financial support: No financial support was received for this submission.
Conflict of interest: None of the authors has conflict of interest with this submission.
