Abstract
Purpose
To investigate the influence of at least 12 hours of fasting followed by acute water ingestion on macular choroidal thickness in eyes of healthy subjects.
Methods
Prospective case series study including healthy volunteers from April 1, 2015 to May 31, 2015. Macular choroidal thickness was measured on enhanced depth imaging optical coherence tomography (EDI-OCT) and on swept-source (SS)-OCT after 12 hours of fasting, and 60 minutes after acute water ingestion (750 mL in 5 minutes).
Results
A total of 52 eyes of 26 healthy volunteers were included in this study. The mean age for participants was 32 years old. After 12 hours of fasting, the mean (±SD) subfoveal choroidal thickness was 335.43 (±104.82) μm on EDI-OCT and 286.16 (±80.32) μm on SS-OCT. The mean (±SD) subfoveal choroidal thickness after acute water intake was 352.32 (±120.36) μm and 290.5 (±85.86) μm, respectively. There was no significant difference between the mean subfoveal thickness at baseline and 60 minutes after acute water ingestion for any of the choroidal imaging techniques (p = 0.1386 for EDI-OCT and p = 0.0659 for SS-OCT).
Conclusions
These results suggest that choroidal circulation can physiologically quickly adapt to systemic vascular changes in healthy eyes. Choroidal thickness did not depend upon the hydration status for the subjects participating in this study.
Introduction
The choroid has multiple physiological functions in the eye; supplying oxygen and metabolites to the outer retina and to the retinal pigment epithelium (RPE) are vitally important.
Choroidal thickness has recently become a subject of increasing interest since the advent of enhanced depth imaging optical coherence tomography (EDI-OCT) (1) and swept source (SS)-OCT, which allow for high-definition imaging of the posterior pole and its structures beyond the RPE (2). There is evidence that that some choroidal thickness changes are related to pathological conditions. Choroidal thickening is associated with central serous chorioretinopathy (3), polypoidal choroidal vasculopathy (4), and cuticular drusen (5). Choroidal thickening also may be observed in choroidal inflammatory diseases, and rapidly decreases after the treatment of inflammation (6). On the contrary, choroidal thinning is associated with atrophic age-related macular degeneration (7) and high myopia, among others (8).
In healthy eyes, it has been shown that choroidal thickness can be influenced by sex, axial length, and age (9-10-11-12). Moreover, variations in choroidal thickness of eyes of healthy subjects have been described after the water drinking test (WDT). Mansouri et al (13) measured the choroidal thickness of 56 eyes of 28 patients before and after the WDT (1,000 mL of water within 5 minutes) using automated segmentations on SS-OCT. They found a significant increase in choroidal thickness after the WDT.
The aim of this study was to investigate the influence of the hydration status of subjects on choroidal thickness, with a protocol of at least 12 hours of fasting followed by acute water ingestion (750 mL in 5 minutes).
Methods
Setting
The study was conducted in the department of Ophthalmology of the Centre Hospitalier Intercommunal de Créteil, France, a referral center specialized in the diagnosis and treatment of macular diseases.
Methods
This was a monocentric, prospective, case series study conducted from April 1, 2015 to May 31, 2015. Healthy volunteers were included in this study if they met the following inclusion criteria: a refractive status between −6 D and +6 D (14), no previous significant medical history, and no history of ophthalmological diseases or surgery. Subjects had to have normal visual acuity results, open angles, and a deep anterior chamber, normal intraocular pressure, and no clinical signs of glaucomatous optic neuropathy on slit-lamp fundus examination.
Choroidal thickness was measured for all participants after 12 hours of fasting, and 60 minutes after acute water intake (750 mL in 5 minutes) at 8:00 am and 9:00 am, respectively.
Choroidal thickness measures were done with EDI-OCT (HRA Spectralis, Heidelberg Engineering) and with SS-OCT (Atlantis, Topcon Inc.). The parameters used with EDI-OCT were 1 horizontal and 1 vertical cross scan 30° (9 mm) centered on the fovea. Measurements were performed by one of the authors, specialized in retinal diseases (R.B-G), with the caliper tool embedded in the provided software. Limits of choroidal tissue were defined as the distance between the outer border of the RPE and the scleral-choroidal interface. On SS-OCT, two single-line 12 mm horizontal and vertical scans centered on the fovea (composed of 1024 A-scans for each of 96 B-scans) were obtained. The automated choroidal segmentation was performed with the manufacturer's viewing software. The resultant choroidal thicknesses for each sector of the Early Treatment Diabetic Retinopathy Study (ETDRS) grid were displayed. We manually measured the subfoveal choroidal thickness at the central point of the ETDRS grid.
Statistical analysis
Quantitative variables were described by their mean with standard deviation. Comparisons were performed using the standard T-test. P values <0.05 were retained as significant. Statistical analysis for sensitivity and specificity was performed using the online available MedCalc Software Version 15.2.2 (MedCalc Software bvba).
Ethical issues
Informed consent was obtained from all subjects participating in the study. All examinations and investigations of this study followed the tenets of the declaration of Helsinki. Approval to conduct the study was obtained from the independent review board/ethics committee of the Federation France Macula.
Results
A total of 52 eyes of 26 healthy volunteers were included in this study (17 women [65.4%] and 9 men [34.6%]). Their mean age was 32.1 years old (range 20-48, SD ± 7.1). The mean spherical equivalent was −0.8 D (range, −4 to +0.75, SD ± 1.5). All subjects successfully performed the acute water ingestion within the required 5 minutes. No adverse events relative to acute water ingestion were recorded.
EDI-OCT images of sufficient quality were available in 84.6% of included eyes (44 eyes) and SS-OCT images of sufficient quality were available in 92.3% of eyes (48 eyes). Low-quality images could not be measured; therefore, these were excluded from the statistical analysis. The mean (±SD) central subfoveal choroidal thickness after 12 hours of fasting was 335.43 (±104.82) μm on EDI-OCT, and 286.16 (±80.32) μm on SS-OCT. The mean central (±SD) subfoveal choroidal thickness 60 minutes after acute water ingestion was 352.32 (±120.36) μm on EDI-OCT, and 290.5 (±85.86) μm on SS-OCT. There was a mean increase in subfoveal choroidal thickness after water intake in this population, which was evidenced by both methods: 14.07 (±26.76) μm in EDI OCT, and 4.83 (±16.47) μm in SS-OCT. However, the difference between subfoveal choroidal thickness before and after acute water intake was not statistically significant for any of the choroidal imaging techniques (p = 0.1386 for EDI-OCT and p = 0.0659 for SS-OCT). An example of measurements before and after water intake is shown in Figure 1.
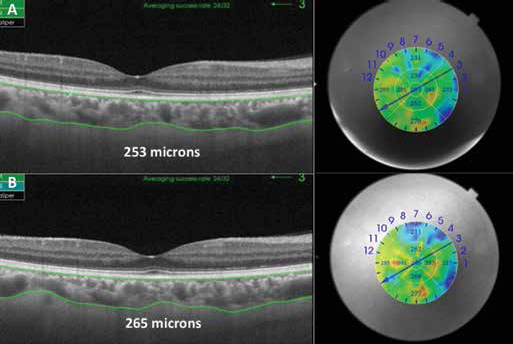
Subfoveal choroidal thickness before and 60 minutes after acute water ingestion (example 1). Right eye of a 34-year-old woman with a spherical equivalent of −0.5 diopters. Horizontal swept source optical coherence tomography scans show a subfoveal choroidal thickness of 253 μm after 12 hours of water and food intake restriction (
Discussion
In this study, we found that subfoveal choroidal thickness 60 minutes after a WDT (750 mL of tap water in 5 minutes) was not significantly increased compared to that at baseline after 12 hours of fasting measured with both EDI-OCT and SS-OCT.
The WDT is a provocative test that indirectly provides information about different parameters of the eye physiology and outflow. In 2009, De Moraes et al (15) studied the variations in choroidal thickness after a WDT in 30 eyes with primary open-angle glaucoma. They measured a composite of retina-choroid-sclera-episcleral tissue on ultrasonographic A and B scans 7 mm nasal to the optic disc. They found a significant increase in the composite thickness. The peak of choroidal thickness increase was at 15 minutes after the WDT. Since the advent of EDI-OCT and SS-OCT, the choroidal thickness has been more precisely measured. The difference in the technique used to analyze the choroidal thickness (ultrasonographic A and B scans vs. EDI-OCT and SS-OCT), the localization of the measures (7 mm nasal to the optic disc vs. subfoveal area), the tissues measured (a composite of retina-choroid-sclera-episcleral tissue vs. choroid/choriocapillaris) and the subjects analyzed (glaucoma vs. healthy volunteers) could explain the discrepancy between their results and ours. In 2012, Arora et al (16) studied the mean macular choroidal thickness variation on EDI-OCT after a WDT (1L of tap water in 15 minutes) in 88 eyes with open-angle and angle-closure glaucoma. Thirty minutes after the WDT, there were no significant changes in mean choroidal thickness in all 88 included eyes. Thus, the WDT seemed to induce no significant variations in choroidal thickness. However, they found a significant choroidal thickness increase after the WDT only in the 40 eyes in the angle-closure subgroup. In another study, Nongpiur et al aimed to evaluate changes in choroidal thickness after a WDT (10 mL/kg of tap water in 5 minutes) in fellow eyes of acute primary angle-closure and in primary angle-closure glaucoma (17). They did not find a significant increase in mean macular choroidal thickness using EDI-OCT at 30 and 60 minutes after the WDT.
Concerning healthy eyes, Mansouri et al (13) analyzed the peripapillary and macular choroidal thickness and volume changes after a WDT (1L of tap water in 5 minutes) in 56 eyes of 28 healthy volunteers. They used automated segmentations on SS-OCT. They found a significant increase in choroidal thickness and volume in the peripapillary area (5.7%; p<0.001 and 6.4%; p<0.001, respectively, at its maximum) and in the macular area (4.3%; p<0.001 and 3.9%; p<0.001, respectively, at its maximum). At the peak of intraocular pressure (15 minutes after the WDT), they also found an increase in choroidal thickness and volume in the peripapillary area (2.6%; p<0.001 and 2.6%; p = 0.007, respectively) and in the macular area (1.2%; p = 0.201 and 1.9%; p<0.01, respectively). They measured the choroidal thickness and volume at different time points, and their peak was found to be variable between 15 minutes (26% of eyes) and 120 minutes (19% of eyes). In our study, we did not find an increase in subfoveal choroidal thickness 60 minutes after the WDT either in EDI-OCT or in SS-OCT, as they did, up to 120 minutes after the WDT. Nevertheless, we do not know if the increase found in their study at 120 minutes after the WDT was statistically significant.
In our study, we aimed to reveal profound changes in choroidal thickness by restricting water ingestion 12 hours prior to baseline measurements and before the WDT. We found an increase in subfoveal choroidal thickness with both OCT techniques but, surprisingly, it was not significant as described by other authors (13, 15). This suggests that the choroidal circulation could physiologically quickly adapt to systemic vascular and osmotic changes in the eyes of healthy subjects.
The present study has several limits. First, we analyzed a relatively small sample; thus, our results need to be confirmed by a larger cohort. Second, we measured the choroidal thickness in a single subfoveal point manually on EDI-OCT. Other authors have also manually analyzed choroidal thickness (15, 17). Both techniques did not find a significant increase in choroidal thickness, but we have only reported results for subfoveal choroidal thickness. We speculated that choroidal thickening changes would be distributed proportionately throughout the choroid. Thus, it is possible that we might have missed choroidal thickness changes in other areas. Third, the peak of choroidal thickness could have occurred before the time point, at 60 minutes after the WDT, in which case those changes are transient and should not affect the final conclusions of our study.
Conclusion
To the our best knowledge, this is the first report analyzing subfoveal choroidal thickness changes in healthy eyes between baseline (corresponding to a measure after 12 hours of fasting) and 60 minutes after the WDT, in both EDI-OCT and SS-OCT. This study highlights that choroidal circulation can physiologically quickly adapt to systemic vascular changes in healthy eyes without significant or persistent changes in choroidal thickness after acute water ingestion. It also suggests that choroidal thickness could be independent of hydration status in healthy subjects.
Footnotes
Financial support: No grants or funding have been received for this study.
Conflict of interest: None of the authors has a financial interest related to this study to disclose.
