Abstract
Aim
To describe a novel technique of tube placement in the anterior chamber.
Methods
In this technique, the extra cut piece of the tube is used to provide a hinge/fulcrum such that the main tube entering the anterior chamber would be angulated posteriorly away from the cornea.
Results
The tube entering the anterior chamber is angulated posteriorly.
Conclusions
Using a fulcrum beneath the tube would assist in posterior positioning of the tube and prevent long-term tube endothelial touch.
Introduction
Glaucoma drainage devices like the Ahmed Glaucoma valve, the Baerveldt or the Molteno are being increasingly used in the surgical management of recalcitrant glaucoma (1). Proper placement of the tube of a glaucoma drainage device (GDD) is important to prevent long-term corneal endothelial damage. We report a novel and simple technique of implantation of a GDD, in which a part of tube is used as hinge/fulcrum to achieve a posterior placement in the anterior chamber, thus avoiding the corneal endothelium.
Methods
A 16-year-old patient presented with bilateral aphakia and having had a prior vitreoretinal surgery done in both eyes for subluxated crystalline lenses and retinal detachment. His intra-ocular pressure (IOP) was 32 mm Hg on maximum tolerated medical therapy in right eye. The decision to implant Ahmed Glaucoma valve (AGV) was taken in view of his aphakic status, prior vitreoretinal surgery, presence of scleral thinning and fibrosed conjunctiva that could cause failure of the conventional trabeculectomy. The challenge in the case was to place the tube in such a way that chances of post-operative corneal endothelial touch could be minimized along with bypassing the area of scleral thinning.
A fornix-based peritomy was performed in the inferotemporal quadrant. After the priming of the valve with 2 mL fluid, the plate of AGV was put in the conjunctival pocket and anchored to the sclera with 6-0 silk sutures. A 4 mm × 4 mm partial thickness scleral flap at the limbus was made. The excess tube was cut with an anterior bevel. The anterior chamber was entered with the help of a 23-gauge needle and the tube inserted into the anterior chamber. The tissues in the area where the tube entry was made were fragile, and the tube while being inserted in the anterior chamber with the standard technique of insertion rose up and pointed towards cornea. It was decided to angulate it posteriorly by using the cut remnant of the tube, which was trimmed to 3 mm and placed below the main tube, horizontally at the limbus (sutured to the underlying sclera with two fixed 10-0 nylon sutures) (Fig. 1). This cut piece of the tube provided a hinge/fulcrum such that the main tube entering the anterior chamber would be angulated posteriorly away from the cornea (Fig. 2). The angulation of the tube inside the anterior chamber was such that it was parallel to the iris. The partial thickness scleral flap was sutured with 10-0 mono-filament nylon sutures and the peritomy was closed with 8-0 vicryl sutures. The patient was followed-up regularly and his IOP ranged from 12 to 16 mm Hg after 12 months’ follow-up on a combination of brimonidine and timolol twice a day. The tube was in the anterior chamber pointing posteriorly and the cut end of tube that was used as hinge was in place with no evidence of any extrusion or displacement.
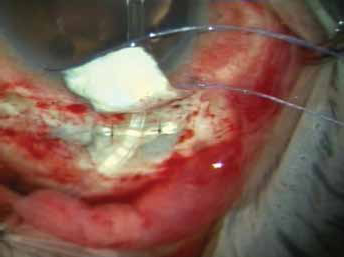
Cut end of tube used as hinge (placed horizontally under the main tube) that facilitates a posterior angulation of the tube in the eye.
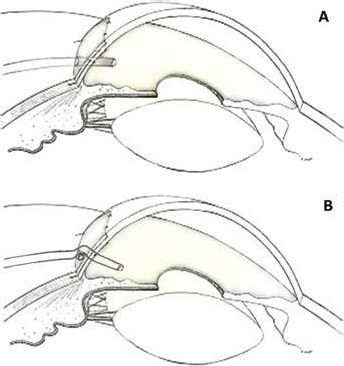
Diagrammatic representation of tube placement without the underlying hinge (
Discussion
Tube corneal touch is a rare but dreaded complication of any GDD implantation (2, 3) as not only it may cause corneal decompensation but it can also result in blockage of the tube. Once a tube endothelial touch occurs or is suspected, techniques to keep the tube away from the cornea have been described (4, 5). However, the best option remains proper intraoperative positioning of the tube in the anterior chamber. This may not always be possible. With the technique described here, however, the cut end of the tube (that is usually discarded) can be used to provide a fulcrum for proper positioning of the tube away from the cornea. Also, neither the angulation of the tube to avoid path through thin sclera nor the small tube segment over which it was passed, caused any hindrance to the function of tube. With the underlying tube support it is unlikely that the tube in the eye will move anteriorly. However, the technique described may not alter the position of the entry site of the main tube into the anterior chamber. Moreover, this is only one case report and further study on a larger number of cases would establish the efficacy of the technique.
The position of the underlying tube piece can be varied (anterior or posterior) depending on the angulation required. This angulation is especially desired in vitrectomized eyes, such as in this report, where the tissues are softer and more likely to result in postoperative movement of the tube in the anterior chamber (6) as also in eyes with post-keratoplasty glaucoma. This procedure can also be adopted in repositioning the tubes that are already causing endothelial touch to position them away from the cornea.
Footnotes
Financial support: No grants or funding have been received for this study.
Conflicts of interest: Conflict of interest: None of the authors has financial interest related to this study to disclose.
