Abstract
We report a case of late detachment in a patient with Descemet membrane (DM) microperforation following a deep anterior lamellar keratoplasty (DALK). Late detachment of the DM in this case occurred 5 months after DALK because of the flattening pressure during the retinal exam with scleral depression. In patients with a history of microperforation during DALK, we suggest that the retinologist and patient avoid rubbing or applying pressure over the eye to minimize the risk of late detachment of the DM.
Introduction
Deep anterior lamellar keratoplasty (DALK) is a safe and effective technique for patients with stromal corneal pathology without the involvement of the endothelium and the Descemet membrane (DM) (1).
The most common intraoperative complication during DALK is DM perforation, which may occur in 0%-50% of eyes undergoing this operation (2).
The purpose of this manuscript is to report the case of late detachment of the DM that occurred after a retinal exam with scleral depression in which the cornea regained transparency and remained transparent for 5 months.
Case report
A 28-year-old male underwent DALK in his left eye due to keratoconus in December 2013 using the Pachy-Bubble technique (3). During the operation, a microperforation of the DM occurred in the superior area. Nonetheless, the surgery was considered a success without residual stroma. The 8.25 mm donor corneal button was sutured with 16 interrupted 10-0 mononylon stitches, without removing the endothelium from the donor corneal button. An inferior iridectomy was performed and SF6 was injected at 20% until 95% of the anterior chamber was filled.
Eight days after the transplant, the patient had a transparent corneal button with slight superior detachment surrounding the microperforation, which measured approximately 2.0 × 2.0 mm and was stable during further follow-up visits. The cornea was transparent in the visual axis, and the DM adhered to the entire extension, except in a small upper area, so we chose not to perform a rebubble.
Five months after the transplant, the patient developed photopsy and floaters that were evaluated by a retinologist. The cornea was clear with no edema, which was exactly as it had been at the eighth postoperative day. A peripheral retinal exam with scleral depression was normal. However, 3 hours after the exam, the patient returned complaining of a significant decrease in visual acuity. His uncorrected visual acuity (UCVA) test worsened from 20/70 to 20/400, and complete detachment of the DM from the corneal button was noted with grade III stromal edema (4). We injected air into the anterior chamber, which was unsuccessful in reattaching the DM. We then opted to leave the double chamber and maintain observation.
Nine months after DALK, the patient showed a UCVA of 20/400 with a transparent corneal button in the double chamber (Fig. 1), fibrosis of the detached DM, and 1 mm anterior subcapsular cataract on the axis. Removal of the stitches was performed. Fourteen months after DALK, the patient had a transparent corneal button, but significant opacity of the detached recipient DM. We created a 3 mm opening in the detached recipient DM over the visual axis with a YAG laser. Endothelial counting was not performed.
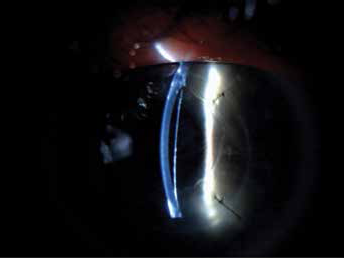
Transparent corneal button with double chamber 9 months after DALK.
After 1 month, the patient returned to the office with significant worsening of UCVA (counting fingers at 40 cm). The detached DM was open along the visual axis, but the DM flap was in contact with the endothelium in the paracentral region, which was causing central and paracentral edema. An endothelial count was attempted, but we were unable to obtain images. We removed the detached DM during surgery for phacoemulsification with implantation of a monofocal intraocular lens. Two months later, the corneal button showed grade II stromal edema (4), and we performed a successful Descemet membrane endothelial keratoplasty (DMEK).
Discussion
Microperforations or larger lacerations following DALK are the major risk factors for early postoperative DM detachment; nonetheless they are not rare (1, 2, 5-6-7-8-9-10). However, despite these complications, most surgeons continue to perform the lamellar corneal transplantation while avoiding converting it into the penetrating technique. We were unable to find a case report similar to ours in the literature. The detachment likely occurred due to the flattening pressure during the retinal exam with scleral depression.
Notably, the corneal button regained its transparency despite the detachment 5 months after DALK. The patient lived about 450 miles from the hospital, so he did not return until 4 months after the rebubble. Therefore, it was not possible to determine how long it had taken the cornea to become clear after detachment. A possible explanation is that part of the endothelium in the donor corneal button can survive in the adherent interface and in the small 2 × 2 mm region, which remained detached in the periphery.
Perhaps in these cases, the recipient DM is not entirely attached to the donor endothelium. There may be areas that maintain virtual spaces without real adherence, where the donor endothelium can survive for longer in the interface. This could also be responsible for the reduced adherence of the donor button to the DM from the recipient, facilitating a late detachment; however, there are no data in the literature to support such a claim.
We prefer to keep the donor's DM because it results in less surgical time. Also, if an early detachment occurs (on the first or second postoperative day) due to a surgical perforation, which does not have a good response to rebubble, it is common for the button to remain transparent. In addition, there are studies that show no significant advantage in removing the DM from the donor (11, 12).
Another important aspect to emphasize is our bad experience using the YAG laser to open the detached DM in the visual axis in a double chamber situation with a clear cornea. A high amount of energy is necessary, as well as a high number of shots, which often occur near the donor endothelium. In this case, although we were able to open the recipient DM, one of the flaps was curved anteriorly and was touching the endothelium, which was already suboptimal. Our current practice has been to open the detached DM surgically, and in cases of significant detachment of the DM, we suggest treatment with rebubble as soon as the diagnosis is obtained (5). After a few days, the DM contracts and opacifies, which makes the detachment untreatable.
In patients with a history of microperforation during DALK, we suggest that the retinologist and the patient avoid rubbing or applying pressure over the eye to minimize the risk of late detachment of the DM. Because late detachment is a rare event, there is not enough evidence to recommend always using a donor corneal button with endothelium. However, the fact that the corneal button regained transparency warrants future studies of the endothelium in similar cases.
Footnotes
Financial support: No grants or funding have been received for this study.
Conflicts of interest: None of the authors has financial interest related to this study to disclose.
