Abstract
Introduction
To report a case of central serous chorioretinopathy (CSC) associated with a retinal pigment epithelium detachment in a myopic patient with marked pachychoroid.
Patient presentation
Case report of a 37-year-old male patient with relatively high myopia (-5.00D in OD/-5.75D in OS), unilateral CSC, and bilateral retinal pigment epithelial detachments, pachychoroid, and choroidal hyperaemia. Standard ophthalmological examination and multimodal imaging, including fundus photography, fundus autofluorescence, spectral-domain and enhanced depth optical coherence tomography, and indocyanine green angiography were performed.
Conclusions
Findings characteristic for the spectrum of CSC/pachychoroid pigment epitheliopathy can be observed in patients with relatively high myopia. Based on the outcome of complete ophthalmological examination, this clinical picture can be discerned from other diseases, which is important for the optimal therapeutic approach.
Keywords
Introduction
Central serous chorioretinopathy (CSC) is a chorioretinal disease, presumably occurring due to choroidal congestion and hyperpermeability, subsequently leading to fluid leakage through a dysfunctional retinal pigment epithelium (RPE), resulting in an accumulation of subretinal fluid (SRF). The aetiology of CSC is poorly understood. The disease is observed approximately six times more often in men than in women, and especially occurs in middle-aged individuals. CSC is associated with the use of corticosteroids, hypercortisolism, and possibly with stress and type A personality (1-2-3). Recently, genetic factors have been found to play a role in CSC (4, 5).
CSC is typically seen in hyperopic or emmetropic eyes, in which a thickened choroid (pachychoroid) can often be detected (6, 7). However, the combination of fundus characteristics associated with this thickening, RPE abnormalities, but absence of SRF in ophthalmological history should lead to a suspicion of pachychoroid pigment epitheliopathy (PPE) (7). Occurrence of CSC has only been described in a few myopic patients. In these patients, a thick choroid in relation to the refractive error but no pachychoroid has been found (8). Choroidal thickness in highly myopic patients is usually lower compared to emmetropic patients (9, 10). Moreover, myopia has been suggested to serve as a protective factor for CSC (11).
Thus far, little is known about the occurrence of findings characteristic of PPE/CSC in (highly) myopic patients. We describe a patient with relatively high myopia in whom findings of CSC and pachychoroid were detected using multimodal imaging, including digital colour fundus photography (Topcon Corp., Tokyo, Japan), fundus autofluorescence (Spectralis HRA + OCT; Heidelberg Engineering, Heidelberg, Germany), spectral-domain and enhanced depth optical coherence tomography (EDI-OCT; Spectralis HRA + OCT), and indocyanine green angiography (ICGA; Spectralis HRA + OCT).
Patient presentation
A 37-year-old Caucasian male was referred to our tertiary referral centre, because of reading difficulties in his left eye for a period of 9 months. The patient had an ophthalmological history of a moderate-to-high myopia, with a refractive error of −5.00 dioptres in the right and −5.75 dioptres in the left eye. Besides a history of deep venous thrombosis, for which the patient used vitamin K antagonists, general medical history revealed no abnormalities. The patient had never used steroids. The best-corrected visual acuity at presentation was 20/13 and 20/44 in his right and left eye, respectively. Slit-lamp examination was unremarkable. Ophthalmoscopy revealed small RPE detachments temporally and superiorly in the macula of the right eye and a central RPE detachment in the fovea of the left eye (Fig. 1E-F). The OCT (RTVueXR Avanti device; Optovue Inc., Fremont, CA, USA) from the referring hospital showed these RPE detachments in both eyes, with serous SRF in the fovea of the left eye (Fig. 1A-B). When the patient presented at our centre, the SRF had disappeared spontaneously on spectral-domain OCT. In both eyes, the RPE detachment was still present (Fig. 1C-D). The choroidal thickness (distance from Bruch's membrane to the hyperreflective line of the inner surface of the sclera, on EDI-OCT) was 496 µm in the right eye and 758 µm in the left eye (Fig. 1C-D). Because of minimal visual complaints in binocular circumstances, the patient was scheduled for repeat examination including ICGA 3 months later. At that visit, his complaints and the outcome of ophthalmological examination had not changed. Mid-phase ICGA showed focal areas of choroidal hyperpermeability in the right and the left eye (Fig. 1K-L). In both eyes, large choroidal vessels that appeared densely packed on the posterior pole and appeared to show early hyperfluorescence on ICGA were detected, (Fig. 1I-J) without evidence of choroidal haemangioma on multimodal imaging (Fig. 1). Because of the absence of SRF at this moment and the stable clinical picture during these last 3 months, no therapeutic intervention was indicated, and the patient was scheduled for ophthalmological follow-up after 1 year, with the instruction to come earlier if experiencing new or worsening of visual symptoms.
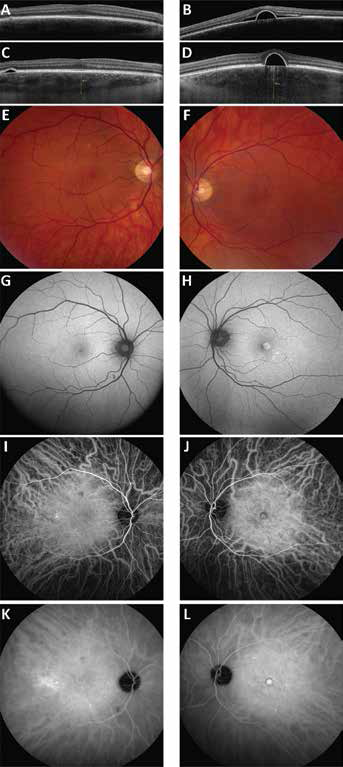
Unilateral central serous chorioretinopathy and bilateral retinal pigment epithelial detachments, pachychoroid, and choroidal hyperaemia in a relatively highly myopic patient. (
Discussion and conclusions
This is the first paper describing a relatively highly myopic patient in whom findings characteristic of PPE/CSC were detected. Active SRF leakage due to CSC was detected unilaterally in this patient, and spontaneous resolution occurred without therapeutic intervention. The RPE detachments, which were detected bilaterally in this patient, did not disappear spontaneously. Due to the fact that no treatment has been conclusively proven to be needed and effective for such RPE detachments, we decided not to schedule a treatment for this patient.
EDI-OCT in this patient revealed a markedly thickened choroid bilaterally, with the eye initially affected by CSC displaying the more thickened choroid. Pachychoroid has seldom been observed in myopic patients (9, 10). In general, in high myopia, choroidal, retinal, and scleral thinning and stretching can be caused by the enhanced elongation of the eye (12). This thinning and stretching have been described to possibly reduce the retinal metabolic demand and to increase the oxygen transport through the retina, together with a thinner and less congested choroid, leading to a decrease in the risk of occurrence of CSC (11). The relatively thick choroid in this myopic patient could have occurred due to the fact that the patient was relatively young, and a choroidal developmental anomaly may have also been present, together with vascular regulatory factors that could have influenced choroidal thickness (13, 14). Moreover, a greater choroidal volume has previously been described in healthy male subjects, compared to that of female subjects (15).
The clinical picture of PPE can be discerned from choroidal haemangioma by indirect ophthalmoscopy, fluorescein angiography, and ICGA. These vascular tumours are usually unilateral, round or oval, elevated, orange-red, and do not have a clear border. The fluorescence that appears during angiography could indicate the existence of large blood vessels. PPE may also resemble acute retinal pigment epitheliitis. Despite similar clinical features, only solitary pigmented lesions in the foveolar area, no RPE detachments, and no thickened choroid have been described in relation to this disease (16). Moreover, the accumulation of SRF in myopic patients can occur in cases of choroidal neovascularization, optic disc pit, and in serous maculopathy in inferior staphyloma associated with tilted disc syndrome (17). The presence of one of these diseases would have led to different findings on multimodal imaging. The hyperautofluorescent abnormalities on fundus autofluorescence imaging of this patient are also most typical for the spectrum of PPE. For CSC, both hyper- and hypoautofluorescent changes have been described, that could occur either unilaterally or bilaterally (18-19-20). Above all, differentiating between these diseases is important to select the optimal therapeutic approach. CSC should be treated with photodynamic therapy with reduced settings, whereas full-setting photodynamic therapy is the indicated treatment for choroidal haemangioma (21-22-23). When a serous maculopathy occurs in patients with an inferior staphyloma associated with tilted disc syndrome, no treatment has yet been proven to be beneficial (24).
We conclude that findings characteristic of the spectrum of PPE/CSC can also be detected in relatively highly myopic patients. Based on the outcome of complete ophthalmological examination including multimodal imaging, this clinical picture can be discerned from other diseases, which is important for the optimal therapeutic approach. Further studies are needed to gain knowledge on the occurrence of PPE/CSC in this specific patient group and on the consequences of this combination.
Footnotes
Financial support: This research was supported by the following foundations: MaculaFonds, Retina Netherlands, BlindenPenning, and Landelijke Stichting voor Blinden en Slechtzienden, that contributed through UitZicht, as well as Rotterdamse Stichting Blindenbelangen, Haagse Stichting Blindenhulp, ZonMw VENI Grant, and Gisela Thier Fellowship of Leiden University (CJFB). The funding organizations had no role in the design or conduct of this research. They provided unrestricted grants.
Conflict of interest: None of the authors has financial interest related to this study to disclose.
