Abstract
Background
To evaluate the outcome of surgical options in the management of Thiel-Behnke corneal dystrophy (TBCD). This is a retrospective case report.
Methods
A 52-year-old female with TBCD with a visual acuity of 0.50 LogMAR in both eyes underwent deep anterior lamellar keratoplasty (DALK) in her left eye (LE) and, 8 months later, phototherapeutic keratectomy (PTK) in her right eye (RE). Postoperatively, the presence of recurrence, uncorrected visual acuity (UCVA), best corrected visual acuity (BCVA), central corneal thickness (CCT), and spherical equivalent (SE) were assessed. Spectralis domain anterior segment optical coherence tomography was also performed to evaluate corneal morphology and reflectivity.
Results
At 1 year, the LogMAR UCVA and BCVA were +0.80 and +0.24, respectively, in the LE and +0.70 and +0.24 in the RE, respectively. CCT and SE were 741 microns (μm) and +4.25 diopters (D) in the LE, respectively, and 339 μm and +6.00 D in the RE, respectively. The cornea was clear in the LE. There was early recurrence of the TBCD and corneal haze in the RE.
Conclusions
The visual outcome of both DALK and PTK were similar for TBCD. No episodes of rejection or recurrence of dystrophy were noted in the eye that underwent DALK. However, postoperative hyperopic shift, persistent haze, and early recurrence were noted after PTK.
Introduction
Thiel-Behnke corneal dystrophy (TBCD), also called CDB2, is an autosomal dominant disease, which affects the Bowman layer and the superficial stroma. Two forms have been described; 1 is linked to the chromosome 10q24, and the other is caused by a mutation of the transforming growth factor beta-induced (TGFBI) gene on the chromosome 5q31 (1). This gene encodes keratoepithelin, which plays a major role in cell-collagen interactions by modulating cell adhesion as it represents a binding sequence for several integrins (2). TBCD is characterized by the accumulation of protein deposits in the cornea, forming bilateral, honeycomb-like, sub-epithelial opacities and increasing irregularity of the corneal surface. Such abnormalities are responsible for progressive decrease in visual acuity and recurrent painful erosions. When loss of corneal transparency becomes clinically significant, penetrating keratoplasty (PKP) is often undertaken (3). Phototherapeutic keratectomy (PTK) also has been reported as an alternative treatment (4). Recurrence of deposition is reported in both PKP and PTK (4, 5).
We report a 1-year intra-individual comparison of the functional and morphological outcomes of a patient with TBCD, who underwent deep anterior lamellar keratoplasty (DALK) in the left eye (LE) and PTK in the right eye (RE). Both treatments gave similar visual improvement, but the eye treated with PTK showed recurrence and postoperative haze.
Case presentation
A 52-year-old healthy woman presented with more than a 10-year history of slowly progressive blurred vision and episodes of ocular pain in both eyes. She had a family history of TBCD, which was detected in her 3 sisters and confirmed by gene testing. Her best-corrected visual acuity (BCVA) was 0.60 LogMAR in the RE and 0.80 in the LE. Manifest refraction (MRx) was +2.00 in the RE and +3.00 in the LE. The central corneal thickness was 661 in the RE and 656 in the LE (Pentacam, Oculus Optikgeräte, Wetzlar, Germany). Slit-lamp examination showed a bilateral, central, “honeycomb”-like pattern of opacities that were phenotypical of TBCD. Deposits were present within the anterior stroma (Figs. 1A and 2A). Spectral domain anterior segment optical coherence tomography (SD OCT) scans (HRA II, Heidelberg Engineering GmbH, Dossenheim, Germany) also confirmed an extensive sawtooth-like pattern of hyper-reflective material deposited along the Bowman layer (Figs. 1B and 2B). The deposits were irregular and localized mostly in the central cornea. The LE was treated first with DALK in which an 8.25 mm donor button was sutured into an 8 mm host bed. The thickness of the bed left was 80 microns (μm). The eye was treated with ofloxacin and dexamethasone 0.1% eye drops 4 times a day postoperatively. The antibiotic was stopped after 2 weeks and the steroid was tapered to once a day by 2 months. Sutures were removed 6 months postsurgery. BCVA was 0.24 and MRx was +2.75 + 3.00 × 130.

Slit-lamp photomicrographs and Heidelberg Spectralis optical coherence tomography (OCT) images of the left cornea. (

Slit-lamp photomicrographs and Heidelberg Spectralis optical coherence tomography (OCT) images of the right cornea. (
The RE was treated 8 months later. A trans-epithelial PTK was proposed to the patient as an alternative treatment, with the rationale of achieving faster healing and refractive stabilization, avoiding the risk of rejection, and leaving the option open for a later transplant. Laser treatment was carried out by a Bausch and Lomb Technolas 217 z, with a 100 Hz repetition rate, 18 ns pulse duration, 120 mJ/cm2 fluence and eye tracking on, over an 8 mm area and in PTK mode. Starting with epithelium on, the treatment was frequently stopped for surface refilling with masking fluid (ialuronic acid 0.25%). During the dispensing of the masking fluid, the cornea was repeatedly examined for residual opacity using the laser microscope. The examination was done with direct light and the assistance of paraxial illumination of the lateral laser lights. As the deposits began to be less detectable, the patient was also shifted to the slit lamp for a more precise evaluation. The endpoint laser of laser treatment was visual scrutiny of barely visible opacities within the treated area. This was weighted against the theoretically calculated total ablation depth (including epithelium and stroma) of about 200 μm, and tissue dehydration. It was deemed not to leave a residual central thickness approximately less than 450 μm. However, this number had a limited reliability in terms of efficacy since the masking fluid alters the ablation rate. The eye was treated with ofloxacin eye drops four times a day for 1 month and dexamethasone 0.1% 4 times daily with gradual tapering over 12 weeks. A stromal haze appeared after 2 weeks and progressively decreased after the fourth month. At 1 year, BCVA was 0.24 and MRx was +5.25 + 1.50 × 90. At 20 months post DALK and 12 months follow-up post PTK, data were collected, and the results are detailed in Table I. Corneal graft in the LE was clear and the SD OCT scans did not show any clinical sign of recurrence (Figs. 1C, D, E). A mild residual haze and early signs of recurrence were seen in the right cornea at the slit lamp examination and at the SD OCT (Figs. 2C, D, E). The spherical equivalent was close to emmetropia in the LE, and the RE was more hypermetropic than it was preoperatively. The maximum BCVA was reached 7 months after surgery in the LE, and 4 months after surgery in the RE. There were no remarkable differences in total corneal wave aberrations (Pentacam) except for the root mean square of astigmatism Z(2,±1) which was higher in the LE. Nevertheless, the patient reported better visual quality in the LE.
Postoperative clinical information of the patient with Thiel-Behnke corneal dystrophy
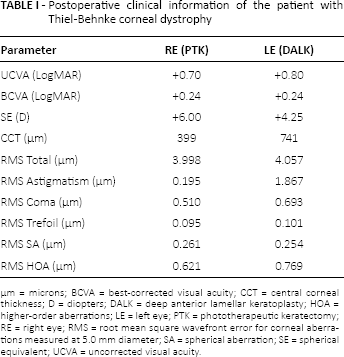
µm = microns; BCVA = best-corrected visual acuity; CCT = central corneal thickness; D = diopters; DALK = deep anterior lamellar keratoplasty; HOA = higher-order aberrations; LE = left eye; PTK = phototherapeutic keratectomy; RE = right eye; RMS = root mean square wavefront error for corneal aberrations measured at 5.0 mm diameter; SA = spherical aberration; SE = spherical equivalent; UCVA = uncorrected visual acuity.
Discussion
This report describes a case of TBCD in which 2 different surgical approaches were undertaken. This case represents 2 well-known challenges in ocular surgery: the treatment of the epithelial-stromal TGFBI dystrophies and the yet unsolved issue of recurrence. The TGFBI gene is mutant in several other forms of corneal dystrophy, including Reis-Bücklers corneal dystrophy (RBCD), lattice corneal dystrophy type I and IIIA (LCD), granular corneal dystrophy type I and II (GCD), and epithelial basement membrane corneal dystrophy. Current strategies for the treatment of these types of dystrophy are based on tissue transplant or photoablation. The major limitation of both these treatments is the high recurrence rate of the primary disease. Therefore, the choice of surgical method in treating corneal dystrophies depends on typical characteristics of aggregates in relation to their location in the cornea, the morphology, the material composition, and the rate of recurrence after surgery.
PTK has been successfully used to remove deposits in corneal dystrophies. Ellies et al (5) examined the efficacy of PTK after PKP in patients with various types of TGFBI dystrophies. A significant number of treated eyes (85%) gained 2 or more lines of visual acuity. The most significant improvement in mean visual acuity was achieved in patients with RBCD who carried p.Arg124Leu and p. [Arg124Leu;ΔT125ΔE126] mutations, followed by patients with severe GCD and LCD who carried p.Arg555Trp and p.Arg124Cys mutations, respectively. Visually significant recurrent deposits were variably observed. Approximately 16% of the patients experienced a relapse in a mean follow-up period of 3.93 years (range 1.15-6.04 years).
In our case, PTK postoperative complications, such as persistent epithelial defects or corneal ulcers, were not observed. However, in the RE, the patient developed hyperopic shift (as expected), moderate haze, and recurrence of the disease. The postoperative thickness of 399 μm indicates that 262 μm were removed centrally; that is, 62 μm more than accounted for. The cornea dries during prolonged treatments, as in our case. Since the ablation rate increases as the cornea dries, significant stroma dehydration probably led to an ablation more than estimated intraoperatively. Caution in stopping the treatment was correct. The topical application of mitomycin-C (MMC) may have helped to reduce corneal haze after excimer laser surgery, but would not decrease the rate of recurrence, as has been reported by Ha et al (6), who found that MMC did not affect recurrence after PTK.
Keratoplasty provides a clear cornea and delays the natural process of disease progression and recurrence. However, symptomatic recurrence of the corneal deposits has been observed depending on the type of TGFBI mutations (3). Patients with p.Arg124Leu and p. [R124L;T125_E126del], which cause RBCD and an atypical variant of GCD, had the worst prognosis (significant recurrence of deposits occurred 5-8 years after the first procedure). Patients with LCD (p.Arg124Cys, p.H626R, and p.Ala546Thr) had an uncomplicated clinical course compared to patients with granular corneal dystrophy. For the LCD patients, symptomatic recurrence of the deposits after the first treatment was 5-7 years, and significant deposits recurred between 11 and 12 years. Patients with TBCD (p.Arg555Gln) also had a delayed recurrence (at 15-16 years). In our case, no recurrence or recurrent dystrophic erosions have appeared in the LE, which was treated with DALK, at 20 months follow-up.
Even though PKP has been mostly used for the treatment of severe TGFBI dystrophies, we believe that DALK may now be a more viable alternative, since it could minimize the risk of rejection, replacing the diseased stromal tissue and preserving the unaffected Descemet's membrane and endothelium.
Although DALK has been used successfully to treat several patients with other corneal stromal dystrophies, it has never been reported as a treatment of TBCD (7). To the best of our knowledge, this is the first report on the outcome of a TBCD treated with DALK in 1 eye, and PTK in the other. Visual acuity and quality appeared very similar for both procedures. On the whole, the patient was pleased with PTK, although it presented a faster stabilization at the expense of a greater hyperopic shift and slightly less clear vision. Furthermore, PTK, considering the increase in hyperopia, may be more reliably repeated for a significant visual recovery in less marked cases, as opposed to DALK. On the outcome of our case, it can be suggested that PTK may be proposed in early cases with central cornea involvement, leaving DALK for recurrences and advanced disease.
Footnotes
Financial support: No financial support was received for this submission.
Conflict of interest: None of the authors has a conflict of interest with the submission.
