Abstract
Purpose
To report the first case of a one-eyed child with micro-cornea, coloboma of iris and acute hydrops without any other disorder of the cornea or systemic disease.
Methods
Intracameral injection of perfluoro propane (C3F8) gas was performed under general anaesthesia.
Results
Resolution of the hydrops was observed at 1st week of follow-up, which was confirmed by anterior segment optical coherence tomography. Patient was subsequently lost to follow-up.
Conclusions
Intracameral injection of perfluoro propane gas is an effective way to quickly resolve acute hydrops. In this specific case, the patient presented with micro-cornea and no other corneal abnormalities.
Introduction
Hydrops denotes an abnormal accumulation of fluid in a body tissue or cavity. Acute corneal hydrops occurs due to a disruption in the Descemet's membrane secondary to an ectatic disorder of the cornea, leading to fluid accumulation in the corneal stroma and epithelium. It has also been reported in cases of post-laser-assisted in situ keratomileusis (LASIK) and post-radial keratotomy (RK) ectasia and after deep anterior lamellar keratoplasty (DALK)/penetrating keratoplasty (PKP) for keratoconus (1, 2). Male preponderance is seen (1, 3). Eye rubbing is an important risk factor (3).
Patient Presentation
A 9-year-old boy presented to the cornea clinic of our hospital with complaints of profound loss of vision in right eye along with pain, redness and watering for the past 3 days. The left eye of the child was phthisical following a similar episode 2 years previously, as described by the father of the child. Visual acuity of right eye was hand movement only with accurate projection of rays.
Slit lamp examination of the right eye revealed a small cornea measuring 8.8 mm horizontally and 8.6 mm vertically. There was diffuse oedema in the cornea and dense oedema centrally. Further examination revealed it to be an acute hydrops with coloboma of the iris. Anterior segment photography (ASP) (Fig. 1) was performed with great difficulty, the child was unable to co-operate for anterior segment optical coherence tomography (AS-OCT).
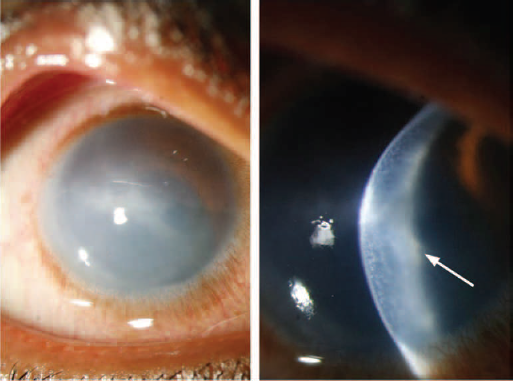
Anterior segment photography (ASP) of the cornea showing diffuse oedema and slit section showing Descemet membrane tear (white arrow).
Systemic examination of the child did not reveal any abnormalities. Past systemic history was non-contributory. There was no history of eye rubbing.
The child was born of a consanguineous marriage and there were no significant ocular complaints in the siblings. The child was un-cooperative for corneal topographic examination.
The child was advised to undergo immediate intracameral injection of per fluoropropane (C3F8) gas (1, 2, 4). The child underwent the procedure under general anaesthesia.
Pre-operative topical application of 2% pilocarpine nitrate was done to achieve pupillary constriction and prevent lens injury. Anterior chamber (AC) paracentesis was performed with a 15-degree side port and 0.1 mL of aqueous was aspirated. 14% nonexpansile concentration of C3F8 was achieved by diluting 0.1 cc of C3F8 with 0.7 cc of sterile air. This mixture was injected into the AC with the help of a cannula attached to a 1 mL syringe – 70% air fill of the AC was achieved.
Post-operatively supine position was advised and topical antibiotics and hypertonic saline were given along with a tapering dose of loteprednol. Topical timolol maleate was prescribed to counter any rise in the intraocular pressure.
Follow-up at 1 week revealed improvement of visual acuity up to 20/200 with resolution of the hydrops with a central scar, which was documented on slit lamp photography (Fig. 2) and AS-OCT (Fig. 3). No complications due to intracameral C3F8 injection were noted. However, the child was lost to follow-up after that.
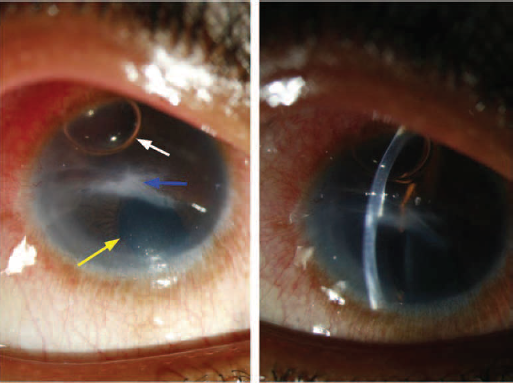
Anterior segment photography (ASP) of the cornea at 1 week post-op showing corneal scar (blue arrow), iris coloboma (yellow arrow) and per fluoropropane gas bubble in the anterior chamber (white arrow).
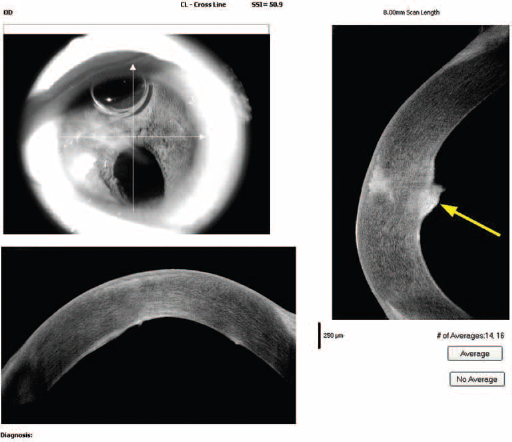
Anterior segment optical coherence tomography (AS-OCT) of the cornea at 1 week post-op showing resolution of the hydrops with Descemet membrane scarring (yellow arrow).
Conclusions
We report the first case of a child having micro-cornea with iris coloboma and acute hydrops without any other corneal abnormalities. No other systemic abnormalities were detected in the child. Extensive literature search did not reveal any similar case. Micro-cornea and acute hydrops have been reported earlier in a case series of Ehlers-Danlos type VI syndrome (5). However, this child did not have any systemic features of the same.
Footnotes
Financial support: No grants or funding have been received for this study.
Conflict of interest: None of the authors has financial interest related to this study to disclose.
