Abstract
Objective
To explore the prognostic value of serum interleukin-17 (IL-17) and vascular endothelial growth factor (VEGF) levels in patients with small cell lung cancer (SCLC).
Materials and Methods
IL-17 and VEGF levels were determined by a commercially available ELISA method.
Results
Serum IL-17 and VEGF levels were higher in the SCLC group than the control group (p<0.001 and p<0.0001, respectively). In addition, there was a significant correlation between IL-17 and VEGF. The level of IL-17 showed significant correlations with tumor stage and tumor metastasis, while serum VEGF levels were significantly associated only with tumor metastasis. Univariate and multivariate analysis indicated that an elevated IL-17 level was an independent prognostic factor for shorter overall survival in SCLC.
Conclusions
IL-17 may play an important role in tumor dissemination in SCLC patients and measurement of IL-17 could have useful prognostic value for worse overall survival in patients with SCLC.
Introduction
Lung cancer is the most common cancer worldwide, accounting for 13% of all cancers. It is the leading cause of death due to cancer, with more than 1.4 million deaths worldwide each year (1). Small cell lung cancer (SCLC) accounts for 15%-18% of all lung cancers and its biological behavior is highly malignant (2). About 67% of SCLC patients are at an extensive stage of disease when diagnosed and the overall 5-year survival rate of SCLC is less than 15% in spite of systematic therapies (3). It therefore seems necessary to seek novel, independent prognostic factors to predict clinical outcomes and optimize the treatment of SCLC.
Angiogenesis, the process of the formation of new blood vessels, is an important biological prerequisite for tumor growth and metastasis (4). Various growth factors have been proved to promote angiogenesis in the tumor microenvironment (5). Vascular endothelial growth factor (VEGF) is considered one of the most important regulators of angiogenesis. VEGF has been reported to be associated with poor prognosis in a variety of human malignancies (6). IL-17 is a member of a group of proinflammatory cytokines which are primarily produced by a subset of CD4+ effector cells known as Th17 cells (7). It has been reported that metastasis is associated with increased levels of IL-17 via activation of the VEGF pathway (8). Recently, IL-17 has been demonstrated to synergize with VEGF during the process of angiogenesis and an IL-17-mediated paracrine network supports tumor resistance to anti-VEGF therapy (9).
Although increased levels of IL-17 have been found in advanced-stage non-small cell lung cancer (NSCLC) (10), little is known about its clinical significance in SCLC. To date, the potential prognostic roles of IL-17 and VEGF in serum have not been quantified and investigated for SCLC. Therefore, in this study we evaluated the serum levels of IL-17 and VEGF and their interrelationship in SCLC patients, and we assessed their potential prognostic value.
Methods
Patients
For this prospective study, we recruited 76 consecutive SCLC patients who were examined at the Affiliated Hospital of Putian University between September 2011 and April 2013. The cohort of patients included 52 (68.4%) men and 24 (31.6%) women with a median age of 51 years. All SCLC patients were newly diagnosed and the diagnosis was confirmed by pathologists. Patients were treatment-naïve when enrolled. As control subjects, 60 healthy volunteers (42 men and 18 women with a median age of 52 years) were enrolled in the same period. All patients received combination chemotherapy based on platinum agents such as cisplatin or carboplatin as first-line treatment for at least 1 cycle according to the NCCN guidelines. The clinicopathological characteristics of the patients were collected by review of their medical records. All patients were followed up by interview in the hospital or by phone contact. Overall survival (OS) was measured from the start of chemotherapy until death or loss of contact. This study was approved by the ethics committees of our institute.
Measurement of serum IL-17 and VEGF levels
Serum samples were obtained from each patient when the diagnosis was confirmed before any therapeutic measures. Samples were centrifuged at 2500 rpm for 15 minutes. The supernatants were immediately stored at −80°C until use. The IL-17 and VEGF concentrations were determined by enzyme-linked immunosorbent assay (ELISA) kits (R&D Systems, Minneapolis, USA) according to the manufacturer's instructions. Each sample was run in duplicate and the average was used. The technicians were blinded to the clinical data.
Statistical Analysis
Statistical analyses were performed using SPSS 19.0 (SPSS Inc., Chicago, IL, USA). Continuous variables were expressed as means ± standard deviation. The Mann-Whitney U-test and chi-square test were applied to compare different groups for continuous variables and categorical variables, respectively. Spearman's correlation coefficient was used to test the correlations between 2 variables. OS was estimated using the Kaplan-Meier method and Cox regression analysis. The hazard ratios and corresponding 95% confidence intervals (CIs) were calculated with the Cox proportional hazards model. All p values were related to the results of 2-sided tests. P<0.05 was considered statistically significant.
Results
Serum Levels of IL-17 and VEGF in SCLC Patients
The 76 SCLC patients’ clinicopathological characteristics in relation to the serum IL-17 and VEGF levels are summarized in Table I. The serum levels of IL-17 in the patient group were significantly higher than those in the control group (24.30 ± 11.26 pg/mL vs.11.82 ± 4.16 pg/mL, p<0.001; Fig. 1A). Similarly, the levels of VEGF were significantly higher in patients than controls (292.86 ± 150.34 pg/mL vs.75.35 ± 20.99 pg/mL, p<0.0001; Fig. 1B). Moreover, there was a significant positive correlation between IL-17 and VEGF levels (r = 0.416, p<0.001; Fig. 2).
Mean values of IL-17 and VEGF of patients with SCLC according to their clinicopathological characteristics
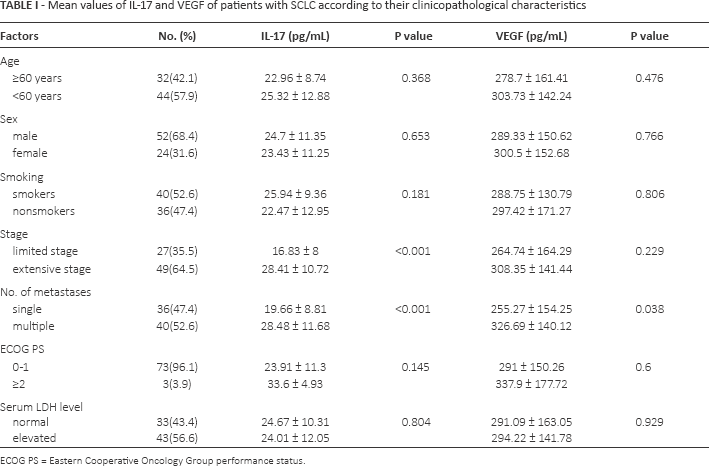
ECOG PS = Eastern Cooperative Oncology Group performance status.
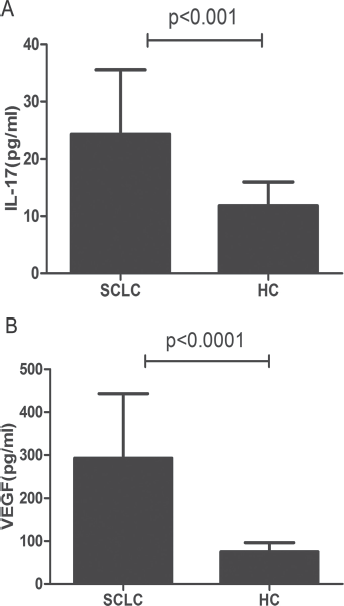
Serum levels of IL-17 in SCLC patients (n = 76) and healthy controls (n = 60), p<0.001
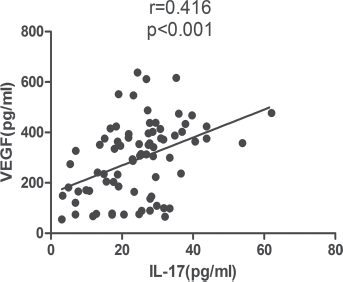
Correlation between serum levels of IL-17 and VEGF in SCLC patients.
Relationship between Serum IL-17 and VEGF Levels and Clinicopathological Parameters
The relationships between serum IL-17 and VEGF levels and the clinicopathological characteristics of patients with SCLC are shown in Table I. The levels of IL-17 were significantly associated with disease stage (p<0.001) and number of metastases (p<0.001). However, there was no correlation between serum IL-17 levels and age (p = 0.368), sex (p = 0.653), smoking (p = 0.181), ECOG performance status (p = 0.145) or serum LDH level (p = 0.804). The serum levels of VEGF correlated only with the number of metastases (p = 0.038).
Survival Analysis
To evaluate the correlation of IL-17 and VEGF serum concentrations with survival, patients were dichotomized according to their median serum IL-17 and VEGF concentrations. As shown in Figure 3, OS analysis in the patient population showed a shorter OS for patients with IL-17 levels >24.93 pg/mL compared with those presenting with IL-17 levels <24.93 pg/mL (log-rank test, p<0.001; Fig. 3A). Interestingly, the OS of patients with VEGF levels above or below 313.43 pg/mL showed no significant difference (log-rank test, p = 0.051; Fig. 3B).
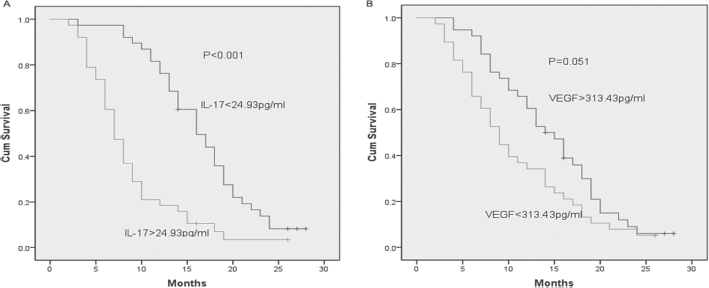
Kaplan-Meier survival curves for IL-17 and VEGF in patients with SCLC. The survival of SCLC patients with IL-17 levels <24.93 pg/mL was significantly longer than that of patients with levels >24.93 pg/mL (p<0.001)
Univariate and Multivariate Analysis
As shown in Table II, univariate analysis revealed that tumor stage (p = 0.018 for OS), serum LDH levels (p = 0.03 for OS), and IL-17 levels (p<0.001 for OS) were significantly associated with poor prognosis. All significant variables (p<0.05) from the univariate analysis were included in the multivariate regression analysis to identify independent prognostic factors. Our data showed that serum LDH levels (p = 0.02) and IL-17 levels (p = 0.002) were independent prognostic factors for OS.
Univariate and multivariate Cox proportional hazards for OS in SCLC patients
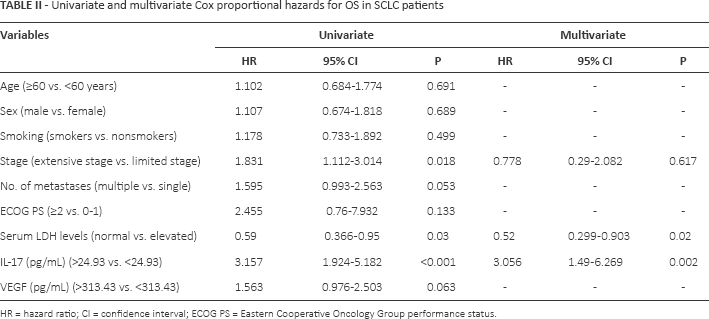
HR = hazard ratio; CI = confidence interval; ECOG PS = Eastern Cooperative Oncology Group performance status.
Discussion
Tumor angiogenesis and metastasis are among the most important prognostic factors for patients with SCLC. When they occur, this often results in treatment failure and poor prognosis (11). IL-17 is a proinflammatory cytokine that is mainly produced by Th17 cells (7). Th17 cells have strong proinflammatory activity in the tumor microenvironment and play a role in cancer progression (12). Angiogenesis is necessary to supply nutrient and structural substrates in amounts to meet the increased metabolic requirements both in physiological and pathological conditions, especially tumor development and metastasis (13). VEGF is one of the angiogenic polypeptides identified in tumor tissue.
In the present study, we showed for the first time that the serum levels of IL-17 and VEGF in patients with SCLC were significantly higher than those of control subjects. IL-17 expression was previously found to be elevated in various cancer types including colorectal cancer (14), breast cancer (15), ovarian cancer (16), and NSCLC (17). Most notably, a recent study has uncovered a network of paracrine signaling in the tumor microenvironment driven by IL-17 secreted by infiltrating Th17 cells (9). The increased levels of IL-17 contribute to cancer proliferation through stimulation of glycolysis and growth factor production, which is a process accompanied by activation of the VEGF pathway (18). These studies and our data suggested that high levels of IL-17 and VEGF could be risk factors for SCLC and emphasized the necessity to inhibit IL-17 and VEGF expression simultaneously.
We further analyzed the correlation between the serum IL-17 and VEGF levels and the clinical features of our patients, and the results suggested that the expression levels of IL-17 were positively associated with tumor stage and number of metastases, whereas the level of VEGF was positively associated only with the number of metastases. In line with our results, most of the literature reported that IL-17 promoted angiogenesis in tumor models and IL-17 expression correlated well with the accumulation of blood vessels in a variety of cancers (19, 20). The acceleration of angiogenesis may contribute to the advanced stage of SCLC. Moreover, cancer cells could spread to distant locations with the aid of new blood vessels. These results suggested that IL-17 plays an important role in tumor progression and dissemination. Furthermore, we reported for the first time that serum levels of IL-17 and VEGF were significantly correlated (r = 0.416, p<0.001). Our results provide evidence that IL-17 might be a protective factor which is favorable for tumor progression as well as a potential therapeutic target to limit both angiogenesis and tumor spread.
To explore the clinical relevance of serum IL-17 and VEGF levels in SCLC, we correlated their concentrations with OS in our patients. In the Kaplan-Meier survival analysis, the OS of patients with high serum IL-17 levels was significantly shorter than that of patients with low IL-17 levels. SCLC patients in the high serum VEGF group had a poorer prognosis than patients in the low VEGF group, but the difference was not statistically significant (p = 0.051). Our study yielded similar results to the study by Tas et al in SCLC (21), whereas other reports suggested VEGF was a prognostic factor in cancer. The different inference may be due to the heterogeneity of different types of cancer. We further carried out univariate and multivariate analysis to investigate the potential prognostic values of IL-17 and VEGF. Our results demonstrated that serum IL-17 levels predicted poor prognosis in both univariate and multivariate regression analysis. Thus, serum IL-17 might be an independent prognostic factor for SCLC patients and could be conventionally measured in clinical practice. Meanwhile, it also could be a good indicator in the follow-up of patients.
In summary, our study demonstrated that the levels of IL-17 and VEGF were significantly elevated in sera of patients with SCLC and showed a significant correlation. IL-17 and VEGF levels correlated significantly with tumor metastasis and IL-17 levels also correlated with tumor stage. Furthermore, high IL-17 levels predicted shorter OS in SCLC and could be used as an independent prognostic factor. Thus, IL-17 may be a new prognostic biomarker in SCLC and a promising target to limit both angiogenesis and tumor metastasis.
Footnotes
Financial support: This work was supported by grants from the Ministry of Science and Technology of China (973 projects) (No. 2012CB917104), the National Natural Science Foundation of China (Nos. 81101833 and 81201605), Shanghai Municipal Commission of Health and Family Planning (No. XYQ2011040), and the Natural Science Foundation of Fujian Province (No. 2013J01390).
Conflict of interest: The authors of this article do not have any potential conflicts of interest.
