Abstract
Background
The aim of this study was to evaluate the clinical, biomechanical and morphological characteristics of a Kevlar®-based prosthetic ligament as a synthetic graft of the anterior cruciate ligament (ACL) in an experimental animal model in rabbits.
Methods
A total of 27 knees of rabbits randomly divided into 3 groups (control, ACL excision and ACL replacement with a Kevlar® prosthesis) were analyzed using clinical, biomechanical and morphological tests at 6, 12 and 18 weeks postprocedure.
Results
The mean displacement in mechanical testing was 0.73 ± 0.06 mm, 1.58 ± 0.19 mm and 0.94 ± 0.20 mm for the control, ACL excision and ACL replacement with synthetic prosthesis groups, respectively. The results showed an improvement in the stability of the knee with the use of the Kevlar® synthetic prosthesis in the biomechanical testing (p<0.05) compared with rabbits that underwent ACL excision, in addition to displacements that were larger but comparable to that in the control group (p>0.05), between the replacement group and the control group. The histological study revealed a good morphological adaptation of the synthetic material to the knee.
Conclusions
This study proposes a new animal model for the placement and evaluation of Kevlar®-based synthetic ACL implants. The studied prosthesis showed promising behavior in the clinical and biomechanical tests and in the histological analysis. This study lays the foundation for further basic and clinical studies of artificial ACL prostheses using this material.
Introduction
The rupture of the anterior cruciate ligament (ACL) is one of the most common pathologies in modern orthopedic surgery, especially in patients who participate in sports activities (1). There is an estimated annual incidence of ACL rupture of 1/3,000 inhabitants in the general population of the United States, which translates to more than 150,000 new ACL ruptures per year, with more than 100,000 surgical reconstructions reported per year (1-2-3). The direct cost of these reconstructions reaches approximately US $2 billion (4). This ligament shows a poor intrinsic capacity for healing because of its poor vascularity, given that it is enveloped by a synovial membrane; thus, surgical treatment is chosen in most cases (5).
Surgical reconstruction aims to reproduce the functions of the native ACL. However, due to its complex anatomy, biomechanics and function in stabilizing the knee in its multiple ranges of movement, it has not been possible to completely reproduce the functionality of the ACL (6).
Historically, the options for surgical repair have included primary repair with or without synthetic augmentation or reconstruction using allografts, autografts and prosthetic ligaments (7). Prosthetic replacements have traditionally been inadequate because of postsurgical complications from wear and degeneration (8). Therefore, autograft reconstructions using the calcaneal tendon, patellar ligament or the tendons of the semitendinosus and gracilis muscles are currently the most widely used procedures in the surgical treatment of these injuries (9-10-11). However, the interest in developing synthetic prosthetic ligament implants persists due to complications such as anterior knee pain, diminished functionality at the site of the removed structure, crepitation of the autografts or flexion contracture of the knee, with current procedures (12-13-14-15).
Currently no prosthesis has proven to be a viable alternative to autografts of the patellar tendon or hamstring tendons, which are currently used in over 90% of reconstructions (16-17-18). Multiple materials are used to manufacture a prosthetic ACL, such as silk, silver, polytetrafluoroethylene (PTFE), polyester, carbon, polypropylene and polyethylene terephthalate, among many others, with less than optimal results (19, 20). Previous studies have used rabbit animal models for evaluating different types of tissue as probable ACL grafts with varying results (21, 22).
However, the use of material proposed in this study has been poorly evaluated. There is no study that assesses morphologically, clinically and biomechanically at the same time the proposed material. Kevlar® aramid fibers by DuPont™ is an organic fiber in the aromatic polyamide family and has unique chemical properties that offer mechanical and resistance capacities that we hypothesize may be useful for the reconstruction of the ACL of the knee (23).
The objective of the present study was to propose and evaluate the clinical, biomechanical and morphological characteristics and the biocompatibility of the use of a Kevlar®-based ACL prosthesis in rabbit knees.
Materials and Methods
A randomized controlled clinical trial with a longitudinal, prospective and comparative laboratory experimental design was performed.
Population characteristics
A total of 27 young adult (age range 5 to 6 months), male, white rabbits of the New Zealand species (Oryctolagus cuniculus), weighing between 3.5 and 4.5 kg, skeletally mature and clinically healthy were used. The calculation of the sample size was performed using a nonprobability sampling technique based on the disposition of laboratory animals. The rabbits were cared for and handled according to the International Review Board regulations and the Mexican Animal Protection Law (NOM-062-ZOO-1999). They were housed in light- and temperature-controlled rooms and fed a standard rabbit diet (8630 Tekland 15% rabbit food) and distilled water ad libitum. Every effort was made to minimize animal suffering and pain, as well as the number of animals used that were necessary to produce reliable scientific data.
Study groups
Using all of the experimental animals (n = 27), 3 experimental groups were designated into which the animals were randomly distributed. The control group (C) was composed of 9 rabbits in which no intervention was performed, and they were only followed during the time period. The excision group (E) was composed of 9 rabbits that had undergone surgical excision of the ACL in the right knee. The replacement group (R) was composed of 9 rabbits that had undergone surgical excision of the ACL and, during that procedure, reconstruction of the same was performed with a prosthesis of synthetic material consisting of ribbons of Kevlar® 49 by DuPont™ that were 3.0 cm in length and 0.5 cm in width, with a thickness of 200 denier, and with 1,000 filaments in a braided disposition for replacing the ACL in the rabbits.
Each of the 3 groups described above was subdivided into 3 proportional subgroups to conduct the clinical tests, histological analysis and mechanical tests at 6, 12 and 18 weeks postprocedure (Fig. 1).
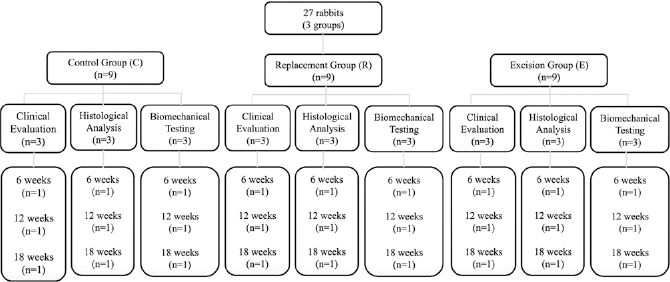
Distribution of the rabbits used in this study.
Study nomenclature
The first letter in the subject designations corresponds to the type of intervention: control (C), excision (E) and replacement (R). The first number corresponds to the type of test applied: clinical tests (designated as 1), histological analysis (designated as 2) and biomechanical tests (designated as 3). The second number corresponds to the time at which the tests were applied: 6 weeks (designated as 1), 12 weeks (designated as 2) and 18 weeks (designated as 3).
Surgical Technique
All of the surgeries were performed by the same surgeon (S.G.C.) who is a subspecialist in knee surgery, after the animal had undergone an 8-hour fast, under anesthesia using ketamine-xylazine (intramuscular 40 mg/kg) and sodium pentobarbital (intravenous 50 mg/kg) according to the animal's weight. Once under the anesthetic, trichotomy of the right knee was performed, and asepsis of the surgical area was performed through exhaustive washing with chlorhexidine. Using a sterile technique, sterile fields were placed to isolate the right knee. Once the procedures above were performed, the surgeon proceeded to perform an anterior arthrotomy of the right knee in a supine decubitus position, starting with an anterior incision on the right knee 4 cm in length.
Dissection was performed by planes up to the articular capsule, which was incised medially 2 cm proximal to the insertion of the quadriceps tendon into the patella and was extended to the insertion zone of the patellar tendon on the anterior tibial tuberosity. Then, an open partial synovectomy was performed, and the infrapatellar fat pad was also partially resected, subsequently performing a lateral luxation of the patella to enable greater visibility of the intercondylar notch (Fig. 2A). Subsequently, the ACL was identified, taking as reference its inclusion into the medial surface of the lateral condyle of the femur in its proximal portion in addition to its insertion into the anterior tibial spine in the center of the tibial plateau. Once located, the ACL was resected with cutting instruments (Fig. 2B).
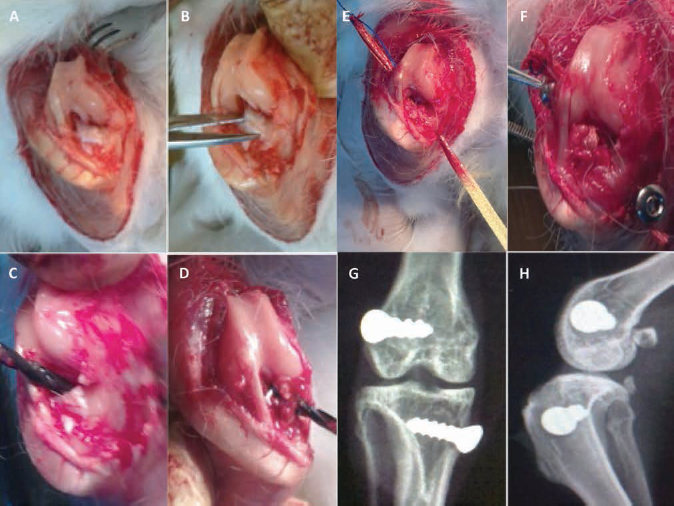
(
The anterior instability of the knee was corroborated transsurgically, performing a transoperative Lachman's test. Once the anterior instability of the knee was corroborated in the 9 rabbits belonging to group E, articular washing was performed, and the capsule was sutured with absorbable material (Vicryl 4-0), in addition to the subcutaneous cellular tissue and the skin, terminating the procedure.
In the 9 rabbits of the replacement group, the procedure was continued with the completion of the bone tunnels for the placement of the prosthetic ligament, as described below. Maintaining the knee in flexion of 100°, the insertion zone of the ACL was identified in the medial surface of the lateral femoral condyle of the knee, and through the intercondylar notch, a femoral tunnel was bored with a drill of 2 mm in diameter, in a medial to lateral and distal to proximal direction, until perforating the lateral cortex of the femur (Fig. 2C); then, the tibial tunnel was made, taking as reference the anterior tibial spine, from where a tibial tunnel was bored with a 2-mm drill, in the direction from the center to the medial cortex and from proximal to distal, until perforating the medial tibial cortex (Fig. 2D). Subsequently, the Kevlar®-based ACL prosthesis was passed through the tunnels, starting with the tibial tunnel, then emerging toward the intercondylar notch and then through the femoral tunnel toward the lateral cortex of the femur (Fig. 2E).
Once the prosthesis was positioned, it was manually tensed and secured to the tunnels with 3.5 × 12 mm cortical compression screws (Synthes, USA), unicortically, in the manner of interference screws (Fig. 2F). Once the procedures above were performed, the stability provided by the prosthetic knee ligament was checked transoperatively, and the capsule and skin were sutured with absorbable material. Proper screw placement was confirmed postprocedure with anteroposterior (AP) and lateral projections of the right knee (Fig. 2G, H).
The animals were managed with antibiotic and analgesic immediately postoperative over a period of 5 days using cephalothin (13 mg/kg intramuscularly every 6 hours) and metamizole sodium (50 mg/kg subcutaneously every 8 hours).
Clinical evaluation
Nine rabbits were evaluated through clinical tests at 6, 12 and 18 weeks from the start of the protocol that included gait analysis and Lachman's test. The gait analysis was subjectively evaluated with regard to whether it was normal or abnormal, considering a degraded or claudicant gait as abnormal, by running the rabbit over a smooth surface that was 10-m long and 50-cm wide. Lachman's test was performed on all of the knees studies and was compared with the contralateral knees of the same experimental animal. To perform the test, the knee was flexed at 30° with the animal in supine position. The examiner placed one hand behind the tibia and the other grasping the animal thigh. The examiner's thumb was on the tibial tuberosity. The tibia was pulled forward to assess the amount of anterior motion of the tibia in comparison with that of the femur. The maneuver was performed by 2 different observers independently to ensure the reliability of the method.
The rabbits from the 3 groups were sacrificed at 6, 12 and 18 weeks by inhalation of CO2 emitted by a cylinder of compressed gas in a closed chamber, and the knees were obtained for subsequent analysis.
Biomechanical tests
The biomechanical tests were conducted on a Shimadzu® Universal tensile and compression Testing Machine (Model AG-20 kN/50 kNX plus). The extremities of the rabbits were mounted on the machine through clamps that were specifically designed for the study. Each right knee was tested in the machine with the anterior drawer test at 90° of flexion. The machine was programmed for a movement speed of 15 mm/min and with a progressive force of 20 N (representing approximately 45% of the weight of the rabbit) (Fig. 3). Graphs of the displacement obtained with respect to the force applied were produced with a computer program adapted to the testing machine.

Photograph of the experimental knee placed in the clamps and mounted on the tension-compression machine for the performance of the biomechanical tests.
Morphological analysis
A total of 9 knees were evaluated. To that end, the specimens were fixed in 10% formaldehyde for 24 hours and then decalcified in a 20% solution of trichloroacetic acid for 72 hours. Immediately afterward, sagittal sections of the femur and of the tibia were made every 5 mm from the group C and group E knees. Sagittal, coronal and axial sections were made in the femur and tibia of the group R knees at the height of the bone tunnel. Samples of 1 × 1 cm were obtained for inclusion in cassettes. Subsequently, conventional histological technique was applied, the pieces were included in paraffin blocks and longitudinal and transverse histological sections 4-μm thick were obtained by microtomy and stained with hematoxylin and eosin (H&E). Seven lamellae were prepared in group R (tissue around the bone tunnels bored into the tibia and into the femur, synovial tissue of the articulation, and tissue of both menisci and adjacent articular cartilage at both of the bone tunnels). In groups C and R, lamellae were prepared of the native ACL, articular cartilage and subchondral bone, synovial membrane and menisci. The lamellae were analyzed with a bright-field light microscope (Nikon Eclipse 50i) and a digital image analysis system (Digital Sight dDS-2Mu). The morphological analysis was performed by a medical doctor with a PhD in morphology and a pathologist. In the sections corresponding to the insertion tunnels, the following were evaluated: the surface of the articular cartilage, the existence of integration of the prosthetic material into the host bone and the presence of ossification of the prosthetic material. Other findings, such as fibrosis, inflammation and vascular congestion, were evaluated. In the sections corresponding to the menisci, the state of the cartilage and the collagen fibers was evaluated. In the sections corresponding to the capsule, the presence of synovial hyperplasia and inflammatory reaction was evaluated. In the sections of the knees in groups C and E, the morphology of the native ligament, the articular cartilage and subchondral bone, and the synovial membrane and menisci was evaluated.
Ethical considerations
The present protocol was approved by the Ethics Committee and the Research Committee with the registration number OR10-007 and the Institutional Committee for Care and Use of Laboratory Animals. The animals used for experimentation were handled according to current international regulations and the Mexican Official Norm for the handling of experimentation animals (NOM-062-ZOO-1999). There were no financial or commercial earnings for the performance of this study, and therefore, the authors declare they had no conflicts of interest.
Statistical Analysis
The statistical analysis was performed using the Excel® 2010 computational program for Windows® XP. An analysis of the frequency distribution for the results of the gait analysis and Lachman's test was performed. The mean and standard deviation for the displacement shown in the biomechanical analysis of the knees were determined. Parametric 2-tailed correlation tests (Student's t) for independent variables were applied to determine the significance of the differences between the mean results of the displacements obtained in the biomechanical tests at 6, 12 and 18 weeks in the different groups studied (C vs. E, C vs. R, and E vs. R), considering as significant a value of p≤0.05. All of the results are presented in graphs and tables.
Results
Clinical test
The results of the clinical tests of the 3 groups of animals are shown in Table I. The rabbits in group C always showed normal results in the evaluation of gait and Lachman's test. The rabbits in group E presented abnormal results in gait and positive Lachman's tests at 6, 12 and 18 weeks postprocedure. In the rabbits in group R, an abnormal gait test was demonstrated at 6 weeks postprocedure, with the gait normalizing itself at both 12 and 18 weeks. The Lachman's test was negative at all 3 time points of evaluation. There were no differences between the results reported by the 2 observers.
Condensed results of the clinical tests

C = control group; E = excision group; R = replacement group.
Morphological analysis
Normal histological characteristics could be observed in the sections of the knees in group C at 6, 12 and 18 weeks; collagen fibers with a regular and well-organized disposition were observed. Between fibers, cells with fusiform nuclei between them were also observed, in addition to the absence of inflammatory cells (Fig. 4A, B). The most superficial layer of articular cartilage attached to the subchondral bone plate with normal cellular characteristics. Underneath the cartilage, zones of compact bone and sections of unaltered trabecular bone were observed (Fig. 4C). Furthermore, the synovial cells presented a linear disposition, with no evidence of inflammatory process at the level of the synovial membrane (Fig. 4D). The articular cartilage showed no type of morphological alteration, given that chondrocytes, isogenic groups and cartilaginous extracellular matrix of normal appearance were observed (Fig. 4E).
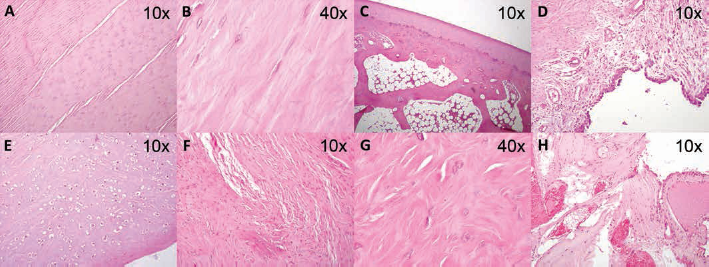
Micrographs of the morphological analysis of the knees of groups C (
In contrast with the results described above, in sections of the knees of group E at 6, 12 and 18 weeks, alterations in the alignment of the collagen fibers of the ACL were observed, distributed in a disorganized and irregular manner, with spaces between the fiber bundles. The loss of normal cellular architecture was also observed (Fig. 4F, G). The presence of extensive areas of hemorrhage and vascular proliferation with fragmentation of collagen fibers in the sections next to the sites of tibial and femoral insertion draws attention (Fig. 4H). In this group, the synovial membrane and the menisci showed no alterations.
In all of the analyzed sections of the knees in group R, it was possible to identify the synthetic implant, with a regular disposition among its components. An inflammatory process was observed around the implant in this group, with the presence of abundant large mononuclear cells with hyperchromatic nuclei at 6 weeks (Fig. 5A, B), small bone sections were also observed. At 12 weeks, the prosthetic ligament was observed to be surrounded by inflammatory cells and fusiform cells similar in appearance to fibroblasts, in addition to indications of the initiation of ossification or integration into the adjacent bone in which small vessels were also observed in the trabeculae (Fig. 5C, D). It is important to highlight that at 18 weeks, complete prosthetic ligament ossification was observed with the invasion of the entire channel by compact bone and a decrease in the inflammatory process. Bone tissue with normal histological characteristics was observed in the zones of ossification around the prosthetic implant, characterized by haversian systems or osteons with well-organized concentric laminae and with cells similar in appearance to osteocytes between them. The laminae were observed to be organized around a central conduit or haversian canal covered by endosteum (Fig. 5E, F).
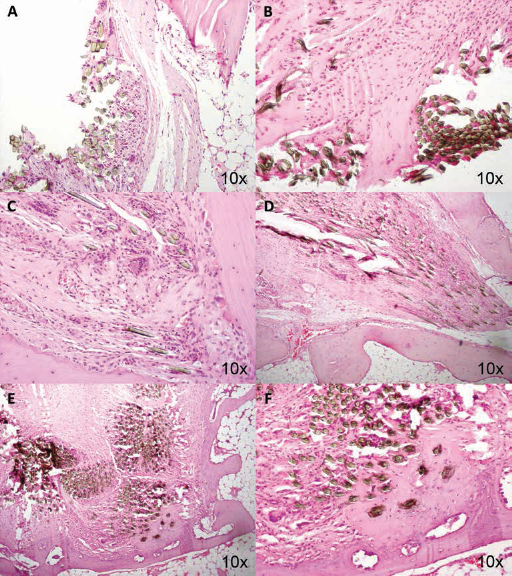
Micrographs of the morphological analysis of the knees of group R. (
Biomechanical tests
The rabbits that made up group C showed no anterior instability of the knee, as would be expected in a knee with the ACL intact, showing a mean displacement of 0.73 ± 0.06 mm with an applied force of 20 N and a lower displacement at 1 mm, which is considered to be a stable knee (Fig. 6A).
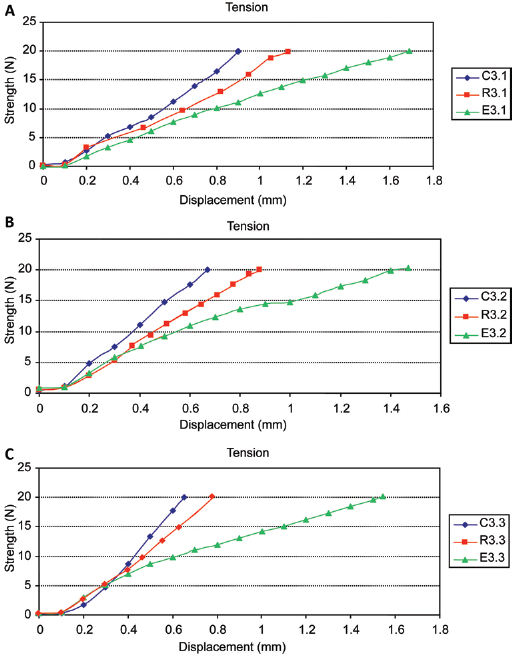
Graph showing the displacement observed at 6 weeks in the knees of the control group (C3.1), the excision group (E3.1) and the replacement group (R3.1). Similar behavior was observed between the normal knee and the knee with the implant. An important difference was observed in comparison with the rabbit in which the anterior cruciate ligament (ACL) excision was performed. (
The rabbits in group E showed important anterior displacement of the tibia with respect to the femur. The mean displacement shown by the knees of the rabbits in this group was 1.58 ± 0.19 mm with an applied force of 20 N (Fig. 6B).
Group R showed no significant differences (p = 0.19) in terms of the above knee stability in comparison with the rabbits of the group that underwent excision of this ligament, showing displacement similar to that of the control group. The mean displacement shown by the knees in this group was 0.94 ± 0.20 mm, which was similar to that in group C.
However, in analyzing the behavior of the movement of the knees of this group, the individual mobility that was shown by each of the knees was noteworthy. The knee of the rabbit in group R that was sacrificed at 6 weeks showed a final displacement of 1.180 mm; the knee of the rabbit that was sacrificed at 12 weeks showed a terminal displacement of 0.875 mm; and the knee of the rabbit that was sacrificed at 18 weeks showed a terminal displacement of 0.784 mm (Fig. 6C).
Significant differences could be demonstrated by means of Student's t-test comparing the mean values obtained from group C vs. group E (p = 0.001) and group C vs. group R (p = 0.02). Comparing the mean results of the displacements obtained between the rabbits in group C vs. group R, no significant differences were demonstrated (p = 0.19).
Discussion
This study is the first to describe the clinical, biomechanical and morphological evaluation at the same time of the use of a Kevlar®-based ACL prosthesis in a rabbit model. The samples from the study groups were analyzed at 6, 12 and 18 weeks, observing an increase in knee stability, improvement in gait and a good morphological adaptation of the synthetic material to the knee in the group receiving the Kevlar® implant. These findings were in contrasted to those in the group with excision of the ACL that showed abnormality in gait and positive Lachman's tests. No biomechanical, clinical or morphological alterations were observed in group C. Thus, the results of the present study demonstrate the use of a Kevlar®-based artificial ACL prosthesis in an animal model. Based on the consulted literature, this material has not been previously used as a material for any type of prosthesis in humans. However, it possesses certain physical properties, such as its tensile strength, flexibility and thermal and chemical stability, that might be of great value as an ACL prosthesis.
ACL rupture is one of the most common knee injuries in sports, resulting in AP laxity, which often leads to an unstable knee (24, 25). Traditional ACL reconstruction is performed with an autograft; disadvantages of this technique are donor site morbidity and a long rehabilitation period (26-27-28). In the 1980s, artificial ligaments became an attractive alternative to biological grafts. The initial enthusiasm surrounding their introduction stemmed from their lack of donor morbidity, their abundant supply and significant strength, immediate loading and reduced postoperative rehabilitation (27).
Synthetic grafts made of different materials such as carbon fibers, polypropylene, Dacron and polyester have been utilized either as a prosthesis or as an augmentation for a biological ACL graft substitute (26). Nevertheless, every material has presented serious drawbacks: cross-infections, immunological responses, breakage, debris dispersion leading to synovitis, chronic effusions, recurrent instability, and knee osteoarthritis (26, 27). Although many experimental studies have been conducted and much effort has been made, currently, no ideal prosthesis mimicking natural human tissue has been found.
The surgery required for the placement of the prosthesis in this study showed no major problems in this animal model. This result indicates that if necessary, current arthroscopic techniques may be adapted for its use. However, we recognize that performing arthroscopic studies on cadavers is necessary to corroborate the ease of the placement of this material.
Moreover, the results of the biomechanical tests employed in the study determined that the mean displacement obtained from the knees in group R presented superior results. However, these values showed no significant differences compared with those for group C. Similarly, it was evident that these displacements showed a pattern of decline over the passage of time, a fact that may be related to the integration and ossification of the prosthesis into the biological tissue of the knee as the weeks elapsed. A longer follow-up may demonstrate that the Kevlar®-based prosthesis can become fully integrated and therefore increase stability in the long term.
The morphological study revealed good tissue adaptation to the environment of the knee. Although the graft was shown to provoke an inflammatory foreign body reaction, it was favorable because it permitted the integration of the ligament into the host bone. Nevertheless, this inflammatory reaction had a downward trend in relation to time. The intraarticular tissues of the knees, such as the menisci, cartilage, articular capsule and synovial membrane, showed no significant alterations before the presence of the foreign material in the intracellular environment. In experimental studies that have employed materials such as polyvinylpyrrolidone mixed with collagen, an improvement in the quality and response time of healing has been observed in the lesions in which it has been evaluated. It has also been observed that it decreases many proinflammatory factors (29-30-31-32).
An important finding of our study was the presence of a larger amount of collagen fibers in the group with the prosthetic implant, which showed greater organization in the late stages of the analysis. These results suggest an increased synthesis of this protein compared with the group with excisions, in which large areas were observed with large spaces, in addition to areas of hemorrhage. Previous studies have described that the application of certain synthetic compounds can modulate collagen synthesis in the fibroblasts and, in addition, can act on the process of wound repair (33-34-35-36-37). These studies may support our results that a larger amount of collagen fibers were observed in the group with the Kevlar®-based prosthesis. The organization of the collagen fibers in the areas of ossification that showed a greater organization of the collagen fibers in the concentric laminae of the osteons is also noteworthy. Other studies have shown that various chemical compounds can be used as a vehicle for the cells and growth factors for bone tissue regeneration (38).
Another important aspect of our study was that, although a synthetic material was applied and an inflammatory response at 6 weeks following implantation of the Kevlar® was observed, it showed a gradual decrease over time. These results correlate with what was described in a double-blind clinical trial, in which a hyaluronic acid-based gel was applied to the gingival mucosa in patients with periodontal disease and a significant decrease was observed in the rate of proliferation of inflammatory cells (Mesa et al, 2001, unpublished data). Henderson et al (39) was the first to make an experimental animal study which concluded that the test material corresponded to a biocompatible material (39).
Recent studies have focused on improving the biocompatibility of Kevlar® aramid fibers in human tissue by adding chemical and biological compounds, obtaining very promising advances in the use of this material as a substitute for bone tissue (40). Suchý et al (40) determined that the addition of 15 vol% of nano hydroxyapatite additive to a composite material based on a polyamide fabric (aramid) and a polydimethylsiloxane (PDMS) matrix is an optimum amount for final application of the composites as substitutes for bone tissue: in this case, both the mechanical properties and the biological properties are optimized without distinct changes in the inner structure of the composite (40). The use of this additive in an animal model similar to ours could improve the adaptive response of synthetic implant to native tissue.
Passuti et al (15) explored the possibility of replacing an ACL with an aramid fiber (Kevlar) implant. This study was performed in at the intraarticular site in 9 dogs, and the average implantation period was 5 months. Studies were carried out by macroscopic, photon microscopy and electron microscopy examination of the samples obtained at the time the animals were sacrificed. Clinical and radiographic studies of the knees were performed to assess functional consequences. Overall, the results showed a partial or complete rupture of 10 neoligaments out of the 17 ligaments studied; on the other hand, osseous anchorage and reintegration in the intraarticular zone appeared satisfactory. That study concluded that fiber only partially meets the performance specifications for an artificial ligament intended to serve as an ACL substitute. Some positive results have encouraged those authors to carry on further this experimental study (15). Similarly, previous studies have evaluated the use of ACL prostheses based on Kevlar. The length change and tension patterns from multiple insertion locations of an ACL substitute were studied in cadaver knees in different ranges of motion (41, 42). However, the primary objective of these studies was not to evaluate the biocompatibility of the graft. Even so, the results of these studies could be valuable for future research in humans.
Wening et al (43) mentioned that neither native X-ray, computed tomography (CT) or magnetic resonance imaging (MRI) allow the evaluation of intraarticular implantation results of Kevlar® directly. In animal trials, the course of an artificial ligament may only be presumed from connective tissue ingrowth. Although soft tissue structure appears much better on MRI than on CT, direct proof of ligament continuity is still impossible. As soon as the connective tissue becomes continuous, it appears clearly and allows indirect evaluation of the prosthesis, as integrity can be judged by its being shaped like natural cruciate ligament. Anatomic preparations show that connective tissue fills up the small space between the 2 cords of a Kevlar® 2-bundle prosthesis 8 weeks after implantation, so that imaging systems show only 1 intraarticular bundle (43). Our study extended to 16 weeks, as we hypothesized that in this period the implants could be assessed using imaging techniques. This was not done in our study and is a limitation to our study.
It is noteworthy that during the present study, biological coatings were not used on the implanted synthetic material, which may represent another limitation. However, the observed results open the door for performing major basic and clinical research on this type of Kevlar®-based prosthetic ligament. One future extension of our study would be to evaluate, through clinical, biomechanical and morphological tests, the response of this material to periods of time longer than the 18 weeks analyzed in our study, in addition to considering a larger number of samples.
In conclusion, our study describes comprehensively evaluating a Kevlar®-based ACL prosthesis showed promising performance in clinical and biomechanical tests and in the morphological analysis. Thus, the results of this study lay the foundation for further basic and clinical studies of an artificial ACL prosthesis using this material in animal models, with longer monitoring times and larger sample sizes, as well as for new studies comparing the proposed material in our study against other synthetic or autologous materials.
Currently, in our research group, in vivo studies are being conducted with the purpose of evaluating the before mentioned perspectives, in addition to identifying the immunomodulatory mechanisms of the body's response to the use of a Kevlar®-based artificial prosthesis and the cellular sequences and/or tissue changes that occur at the site of implantation of the prothesis, and to use biological additives to enhance the biocompatibility of synthetic grafts using the same animal model as that in this study.
Footnotes
Acknowledgements
The authors wish to acknowledge the assistance of Jaime A. Cisneros Rios in preparing the graphical material presented in this study.
Financial support: No grants or funding have been received for this study.
Conflict of interest: None of the authors has any financial interest related to this study to disclose.
