Abstract
Introduction
The effect of scaffold pore size and interconnectivity is undoubtedly a crucial factor for most tissue engineering applications. The aim of this study was to examine the effect of pore size and porosity on cartilage construct development in different scaffolds seeded with articular chondrocytes.
Methods
We fabricated poly-L-lactide-co-trimethylene carbonate scaffolds with different pore sizes, using a solvent-casting/particulate-leaching technique. We seeded primary bovine articular chondrocytes on these scaffolds, cultured the constructs for 2 weeks and examined cell proliferation, viability and cell-specific production of cartilaginous extracellular matrix proteins, including GAG and collagen.
Results
Cell density significantly increased up to 50% with scaffold pore size and porosity, likely facilitated by cell spreading on the internal surface of bigger pores, and by increased mass transport of gases and nutrients to cells, and catabolite removal from cells, allowed by lower diffusion barriers in scaffolds with a higher porosity. However, both the cell metabolic activity and the synthesis of cartilaginous matrix proteins significantly decreased by up to 40% with pore size. We propose that the association of smaller pore diameters, causing 3-dimensional cell aggregation, to a lower oxygenation caused by a lower porosity, could have been the condition that increased the cell-specific synthesis of cartilaginous matrix proteins in the scaffold with the smallest pores and the lowest porosity among those tested.
Conclusions
In the initial steps of in vitro cartilage engineering, the combination of small scaffold pores and low porosity is an effective strategy with regard to the promotion of chondrogenesis.
Introduction
A possible approach in the engineering of cartilage tissue is to expand seed and culture chondrocytes on synthetic porous biomaterial foams. An appropriate physicochemical environment that accounts for a physiological intracellular stress state deriving from the cell–biomaterial interaction may favor the recovery of a phenotypic cell expression (1, 2). The maintenance of such a physiological adhesive configuration, which is primarily related to the microarchitecture of the scaffold, allows the secretion of extracellular matrix (ECM) proteins specific to cartilaginous tissue, and thus a better quality of the engineered construct (3).
Therefore, the control of the scaffold pore structure, including the pore size and the pore interconnectivity and gradient, is crucial for an optimal development of the new tissue (4–5–6–7–8–9–10–11–12). The pore size should be in a range that facilitates cell penetration and migration during cell seeding, nutrient diffusion and removal of metabolic substances, and provides a 3-dimensional (3D) microenvironment inducing cell assembly and differentiation (13). The scaffold pore size, as well pore interconnectivity, were shown to influence osteochondral repair. In particular, both features seem to impair osteochondral repair in vivo (14, 15). Indeed, chondrocytes cultured on 3D microporous scaffolds have shown that small pore size can impair the infiltration of cells and may result in an uneven cell distribution throughout the scaffold (16). Accordingly, a significant enhancement in chondrocyte attachment and viability with increasing porosity was observed in poly-L-lactide scaffolds, in chitosan scaffolds, in poly(ε-caprolactone) (PCL) scaffolds, in collagen scaffolds and in polyurethane scaffolds (8, 12, 13, 17–18–19–20–21–22–23–24–25–26–27). However, some results have indicated that chondrocyte phenotype and biosynthetic activity improved in collagen matrices containing smaller pores (28, 29).
From a technological standpoint, there exist significant challenges in controlling the scaffold microarchitecture and pore size at the cell scale (10 µm). Relatively novel rapid prototyping techniques, such as fused deposition modeling and stereolithography, can be used to fabricate ordered microstructured scaffolds. However, these fabrication technologies are bound to layer-by-layer procedures or to the use of masks, and cannot be used to fabricate truly arbitrary geometries. Among stereolithography techniques, 2-photon laser polymerization (2PP) is a maskless 3D fabrication method with submicrometer resolution, which is not bound to a layer-by-layer procedure. This frontier technique has rendered it possible to fabricate ultraprecise ordered 3D scaffold structures, with a geometry controlled at the cell scale (10 µm) and with a very high spatial resolution (less than 1 µm) (30).
In contrast to such techniques, microporous scaffolds made of synthetic biodegradable polymers (e.g., based on polylactic acid, polyglycolic acid and hyaluronic acid) can be manufactured using established techniques, such as gas foaming, solvent casting with particulate leaching, and electrospinning (31). These techniques produce highly porous scaffolds with interconnected pores or random fiber networks.
In this context, the aim of this study was to examine the effect of pore size and porosity on cartilage construct development in different scaffolds seeded with articular chondrocytes. Poly-L-lactide-co-trimethylene carbonate scaffolds with different pore size were fabricated, using a solvent-casting/particulate-leaching technique. On these scaffolds, bovine articular chondrocytes were seeded, cultured for 2 weeks and examined with regard to morphology, viability and cell-specific production of cartilaginous ECM proteins.
Materials and Methods
Scaffold fabrication
The scaffolds used for cell experiments were biodegradable structures made with well-defined spherical pores. Poly-L-lactide-co-trimethylene carbonate (PLA-co-TMC) was chosen as scaffold material because copolymerization of L-lactide with trimethylene carbonate allows improved material flexibility and control of the degradation rate. Compared with plain polylactide (PLA), the acidity of degradation products – particularly detrimental in poorly vascularized implant sites – is reduced. Furthermore, the in vitro cytocompatibility of PLA-co-TMC was found to be significantly higher than that of PLA (32, 33).
The fabrication technique used to control scaffold pore size and geometry – i.e., solvent casting/particulate leaching – was detailed in a previous work (34), together with a preliminary biocompatibility assessment. Briefly, spherical gelatin particles were prepared from soybean emulsion and sieved to the desired diameter intervals. Microspheres were then leveled in a mold and allowed to adhere by controlling temperature and humidity before casting polymer solution. After complete solvent evaporation, gelatin was leached out in warm deionized water. The technique was shown to enable the preparation of scaffolds with well-defined spherical pores and with a discrepancy between total porosity and open porosity of less than 5%, as measured by air expansion porosimetry. The scaffold preparation technique actually allows the controlling of interconnections by regulating the particle adhesion in the mold (by simply increasing time and temperature). Here, the chosen condition was optimized to guarantee a very large open porosity, while preserving scaffold mechanical integrity and a well-defined spherical shape of pore. A representative image of the microgeometry that the technique allows us to obtain is shown in Figure 1A. A microdomain of this geometry can be idealized as made of single pore units arranged in a honeycomb pattern (Fig. 1B). By controlling particle size and optimizing adhesion conditions – i.e., the degree of packing – 3 different scaffold geometries were prepared: the first with pore diameter ranging from 50 to 100 µm (average 75 µm), the second with pore diameter 100 to 150 µm (average 125 µm) and the third 150 to 200 µm (average 175 µm). Scaffold porosity, calculated as the ratio of void volume to total volume, was 71%, 83% and 87% for scaffolds with mean pore size of 75, 125 and 175 µm, respectively (Fig. 1C).

Scaffold of variable pore dimensions used in the study. (
Cell culture
Articular cartilage was harvested aseptically from the metacarpophalangeal joints of 8-month-old calves slaughtered at an abattoir supplying food producers. Approval by an institutional board was not required since experimental animals were not used. There were no ethical issues for human and animal rights. Chondrocyte isolation was achieved by enzymatic digestion with collagenase (35). The reagents used were from Sigma-Aldrich s.r.l. (Italy). The complete medium contained Dulbecco's modified Eagle's medium (DMEM), sodium pyruvate, HEPES buffer, antibiotics (penicillin/streptomycin), L-glutamine, L-ascorbic acid, insulin and 10% fetal calf serum (FCS). Viable cells were counted with trypan blue exclusion and used for scaffold seeding.
Three independent experiments were carried out. The scaffolds employed were 5-mm-diameter, 1-mm-thick discs. For each experiment, 18 discs were positioned in a culture cluster, 6 for each scaffold mean pore size (75, 125 and 175 µm), and seeded with cells at a density of 102,000 cells/mm3. The discs were incubated for 24 hours at 37°C to allow cells to adhere. The disks were then transferred to culture flasks and incubated for 2 weeks, with medium freshly replaced every 3 days.
Assays
At culture day 14, constructs were prepared for viability assays, histology, biochemical assays and electron microscopy.
Cell viability was determined using mitochondrial dye inclusion. For each scaffold pore dimension, 1 cell construct and 1 cell-free scaffold were washed twice in sterile phosphate-buffered saline, placed in microtiter wells with DMEM containing 0.5 mg/mL of thiazolyl blue (Sigma Chemical, St. Louis, MO, USA) and incubated for 3 hours. The color crystals were dissolved using 10% dimethyl sulfoxide (DMSO) in isopropanol. Absorbance of the converted dye was measured in triplicate with a DU-65 spectrophotometer (Beckman Instruments GmbH, München, Germany) at a wavelength of 570 nm, and with a background subtraction at 630 nm. The absorbance obtained from the cell-free scaffolds was set as the zero reference.
For histological analysis, samples were fixed in 1:1 methanol:acetone overnight at 4°C. Paraffin-embedded samples were sectioned at 5 μm using standard procedures. The histological sections were stained with Mayer's hematoxylin-eosin to determine cell distribution and with 1,9-dimethylmethylene blue to determine glycosaminoglycan (GAG) content. In addition, staining was performed on histological preparations obtained from acellular scaffolds, to verify the reliability of the method in distinguishing newly synthesized matrix from the original scaffold material. Digital images were acquired from stained sections using a light microscope (Leica Ltd., Cambridge, UK).
Portions used for biochemical analysis were digested with papain and assayed for DNA, GAG and hydroxyproline (HYP) content. DNA was assessed by Hoechst 33258 dye binding (36), while GAG content was assessed by 1.9-dimethylmethylene blue chloride (37). Hydroxyproline content was evaluated by alkaline hydrolysis of the tissue homogenate and subsequent determination of the free hydroxyproline in hydrolysates (38).
For scanning electron microscopy (SEM), seeded construct samples were fixed with 2.5% glutaraldehyde in 0.1 M cacodylate buffer (pH 7.4) for 4 hours at 4°C, rinsed in cacodylate buffer and postfixed in 1% osmium tetroxide for 1 hour. After an additional rinse in cacodylate buffer, samples were dehydrated through a graded series of ethanol. Prior to SEM observation, samples were vacuum dried and sputter-coated with gold. The observations were carried out at 10 keV using a Stereoscan S360 electron microscope (Leica Cambridge Ltd., Cambridge, UK).
Statistical analysis
The mean and standard error of the mean were calculated for each experimental group (of average pore size 75, 125 and 175 µm, respectively). The groups were compared with 1-way ANOVA, and with Tukey tests for matched pairs, and differences were considered to be significant for a p value <0.05.
Results and discussion
Understanding the effect of scaffold pore size and interconnectivity is undoubtedly a crucial factor for most tissue engineering applications. Within this context, gelatin microsphere leaching appears to be a powerful tool to investigate the influence of porosity parameters on cell fate. Indeed, gelatin microsphere leaching allows manufacturing scaffolds with well-defined spherical pores with a controlled dimension and distribution by simply sieving particles with a specific size. Finally, this technique can be applied to virtually any degradable polymer suitable for tissue engineering. For all of the scaffolds, SEM observation (Fig. 2) showed chondrocytes with a phenotypic spherical morphology, with smooth membranes and very small areas of adhesion between each other and to the scaffold. Cell distribution at culture day 14 can be better appreciated from the histological sections in Figure 3 (scale bar equals 20 µm in all images). All constructs showed a homogeneous distribution of round cells throughout their thickness, although in some cells, the nucleus was condensed and pyknotic, indicating apoptosis (Fig. 3A–B–C). ECM showed positivity to GAG in all constructs (Fig. 3D–E–F). The total DNA content was found to be the lowest for 75-µm constructs and increased significantly with scaffold pore size (Fig. 4A, B). The cell metabolic activity significantly decreased with pore size (Fig. 4C). Concerning the total content of phenotypic matrix proteins, we observed that the GAG content was the lowest for 75-µm pore size constructs and increased significantly with the pore size (Fig. 5A), whereas, the collagen content was found to be significantly greater in 125-µm pore size constructs (Fig. 5B). The matrix proteins GAG and collagens normalized to the DNA content showed a significant decrease with increasing pore size (Fig. 5C, D, respectively).
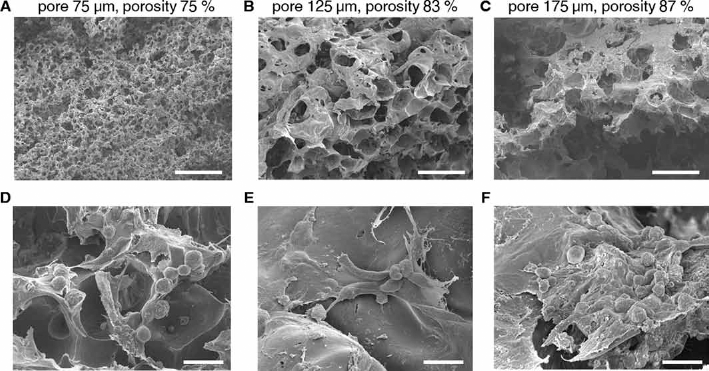
Representative scanning electron microscopy (SEM) images of the chondrocyte-seeded constructs at 14 days of static incubation, showing that cells maintained a phenotypic spherical morphology and secreted abundant extracellular matrix: (
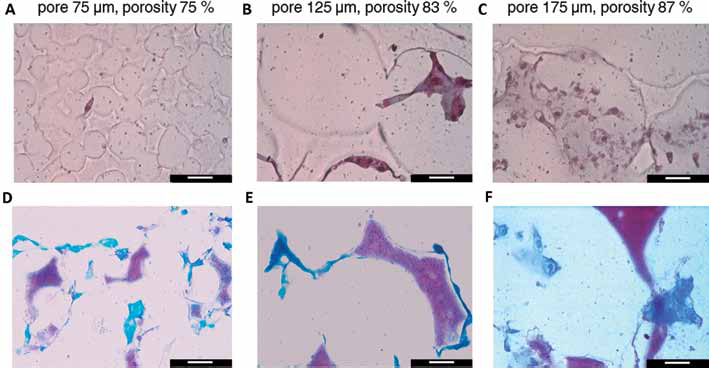
Representative images taken from histological sections of the chondrocyte-seeded constructs at 14 days of static incubation. The scaffold pore geometry is clearly visible in section in all images. (
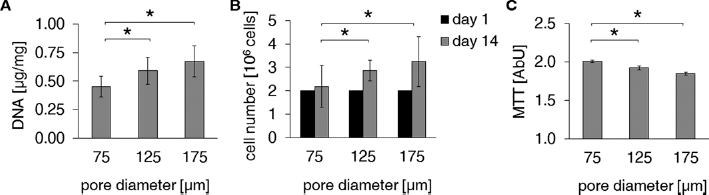
Results of cell growth and of biochemical assays on the chondrocyte-seeded constructs at 14 days of static incubation, as a function of the different scaffold pore sizes. (
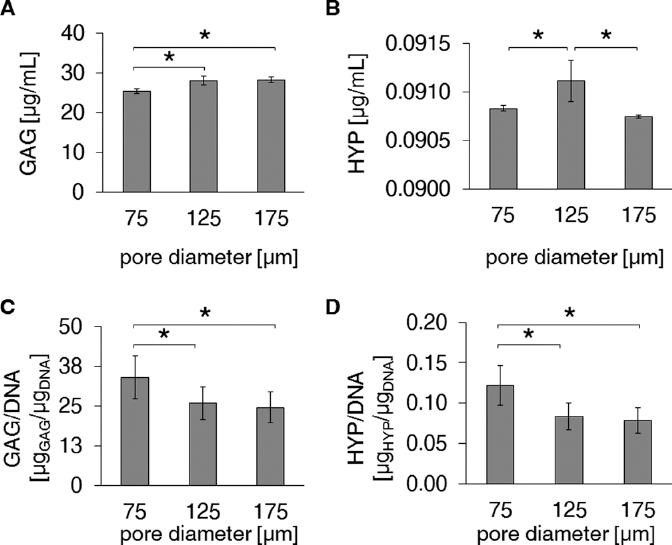
Results of biochemical assays on the chondrocyte-seeded constructs at 14 days of static incubation, as a function of the different scaffold pore sizes: (
Our results are in general agreement with those reported in previous studies (8, 12, 13, 17–18–19–20–21–22–23–24–25–26–27) with reference to the increasing cell density, DNA content, GAG and collagen-specific constituents found in constructs, with increasing scaffold pore size. Our results refer to different scaffold materials and to pore diameters ranging between 75 and 175 µm, instead of 10 and 120 µm (8) or even greater 50 and 500 µm seeded with different cell populations (12, 18, 19). However, some published results have indicated that chondrocyte phenotype and biosynthetic activity improved in collagen matrices containing smaller pores (28, 29). The contradictory results may be due to the complexity of factors in 3D culture, which may affect cell penetration, distribution and nutrient diffusion (8, 12, 13, 17–18–19–20–21–22–23–24–25–26–27).
In this work, the highly controlled pore geometry adopted allowed us to measure a cell-specific decrease in metabolic activity, GAG and collagen-specific constituents, with increasing pore diameter, with statistical significance. Cell density significantly increased with scaffold pore size and porosity in our study, indicating a better general viability of cells in this condition, likely due to increased mass transport of gases and nutrients to cells and removal of catabolites from cells that was allowed by the scaffolds with the lowest diffusion barriers. However, smaller pores induced a more 3D adhesion configuration for cells in smaller pores, where cells have a limited surface on which they can proliferate in monolayer and are thus stimulated to aggregate in 3D, as shown in Figure 2D. Cell aggregation is an important cue for phenotypic expression of chondrocyte markers in most published reports in the literature (3, 14–15–16, 27). In addition, hypoxia is recognized as a stimulus leading to an increased expression of the cartilage phenotype in chondrocytes. We propose that the association of smaller pore diameters, causing 3D cell aggregation, to lower oxygen levels, caused by increased diffusion barriers, could have been the condition favoring the synthesis of cartilaginous matrix proteins in the scaffold with the smallest pores and the lowest porosity, among those tested.
The main limitation in our study was the technical difficulty in characterizing the pore microgeometry in the scaffolds. It would have been useful to select a more precise technique for pore size and porosity evaluations, such as microcomputed tomography (µCT). Unfortunately, μCT was not available to us at the time when the experiments were performed. Nevertheless, we assessed open porosity by gas expansion porosimetry while optimizing the scaffold preparation technique, and the difference between total porosity and open porosity was less than 5%. Despite this limitation, this study is the first in which the polymers evaluated do not differ either in composition or in microgeometry, except for the pore size. This favorably affected our ability to distinguish the influence of this factor on the promotion of chondrogenesis.
Conclusion
In conclusion, in engineered cartilage constructs, the pore diameter correlates positively with the cell density, in accordance with the published data in all previous reports. However, here we additionally showed that the pore diameter correlates negatively with cell metabolic activity and ECM synthesis, consistent with the fact that a greater production of ECM by the cells requires a more intense anabolic activity. This implies that cartilage cells synthesize less matrix when they are stimulated to proliferate in larger pores, where they can spread on the pore surface while maximizing the tensional state of their cytoskeleton. We suggest that, at the beginning of culture, maintenance of a (nonspread) roundish shape in smaller scaffold pores is more effective with regard to the promotion of chondrogenesis.
Footnotes
Acknowledgement
We are grateful to Matteo Moretti for his contribution to the hydroxyproline analyses.
Financial support: No grants or funding have been received for this study.
Conflict of interest: The authors have no financial conflicts of interest.
