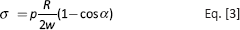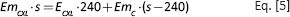Abstract
Background
The aim of this work was to evaluate the effect of cross-linking (CXL) on ex vivo porcine corneal elastic properties, using an inflation procedure.
Methods
Twelve corneas were subjected to standard CXL (370 nm, 3 mW/cm2, 30 minutes), while 12 were used as controls. Corneal thickness was measured by Visante optical coherence tomography, before and immediately after treatment, and before inflation test. Both intraocular pressure and radial apical cornea displacement were measured during inflation. Stress-strain curves were obtained by applying the linear shell theory. The elastic modulus was evaluated by calculating the slope of the stress-strain curves.
Results
Results showed a statistically significant increase in elastic modulus (p<0.0001), with a mean of 3,868 ± 502 kPa for cross-linked corneas and 2,727 ± 238 kPa for untreated corneas, when subjected to high pressure (40-60 kPa). CXL significantly increased porcine cornea stiffness by about 42%. Findings did not show any significant difference within the physiological range of pressure (2-4 kPa).
Conclusions
The inflation test has been proven to be a valuable tool for the investigation of corneal biomechanics, maintaining both integrity and geometry of corneal tissue.
Introduction
The cornea is the first transparent, thin-walled surface, and the most powerful refracting surface, forming the front of the eyeball. It acts as a protective covering and helps to focus or refract light waves onto the retina at the back of the eye. Anatomically the cornea consists of 3 main layers: epithelium, endothelium and stroma. The last forms about 90% of the cornea and is composed of about 200 flattened lamellae (collagen fibrils) superimposed one on the other (1). The physicochemical properties of corneal collagen do not differ from those of tendons or skin collagen (2).
Keratoconus is a noninflammatory ocular condition, usually bilateral, characterized by progressive changes in the shape of the cornea. In a keratoconic eye, a slowly progressive thinning of the cornea causes it to protrude forward in a conical shape, leading to blurry vision and other vision problems. In approximately 20% of patients, these impairments lead to cornea transplantation (3).
In recent decades, a new method for increasing the corneal stiffness using UVA and riboflavin (4-5-6-7) has been developed for the treatment of progressive keratoconus: corneal collagen cross-linking (CXL). To date CXL is considered less invasive than corneal transplant. Numerous studies have reported that CXL may delay or stop the progression of keratoconus acting on some pathophysiological mechanisms, thereby improving the corneal shape and producing a better quality of vision (8-9-10-11-12-13-14). Studies of rabbit and porcine eyes after CXL have shown a 70% increase in corneal stiffness in treated versus untreated corneas (6, 12-13-14). CXL has been demonstrated to strengthen the weak structure of corneas affected by keratoconus by increasing stromal collagen cross-links, thus bundling collagen fibers, and preventing cornea from bulging out and becoming irregular in shape (14).
From a biomechanical point of view, the cornea is a composite tissue that exhibits anisotropic nonlinear and viscoelastic properties (15). Its mechanical behavior, which depends on its shape, thickness, composition and microstructure (15, 16), is essential to maintain dimensional stability and thus a good vision (17). Load displacement as well as stress-strain curves are characterized by 2 distinct phases: a first phase in which a limited variation of pressure leads to a relatively small increase of corneal deformation, attributable to collagen fibers not yet completely stretched, and a second phase where a significant variation of pressure leads to a small increase of the corneal deformation, attributed to the tension of aligned collagen fibers.
Nowadays there are several clinical instruments capable of measuring in vivo corneal shape and thickness (i.e., ultrasound pachymeter, optical coherence tomography [OCT], etc), but investigations into the elastic properties of corneal tissue still rely on ex vivo procedures (16), with experiments involving corneas from human and animal donors (18-19-20). In particular, porcine corneas are often used due to their human-like behavior, although they have less stiffness and greater thickness (21). Several authors have performed tensile tests on corneal strips (11, 14, 20, 22-23-24-25-26-27-28) to characterize corneal stress-strain behavior. However, the procedure involves some intrinsic defects, which may reduce the reliability of the technique (29). Two of those problems are related to the corneal geometry: a strip of sample is indeed originally part of a spherical surface, whereas flattening produces bending stresses in addition to the fact that the length of the specimen along its longitudinal axis will be greater than along the sides (29). Furthermore, the analysis of the results obtained from tensile tests usually takes into consideration the central corneal thickness ignoring the natural increase in corneal thickness in the peripheral area (29). One additional problem is that strip tests are prone to extensive preconditioning effects, in which mechanical loading extensively alters the mechanical properties (30, 31). This causes the stress response of the ocular tissues to be stiffer in uniaxial strip tests than inflation tests (32). Therefore, tensile tests, despite their relative simplicity and low cost, have been replaced by inflation tests which allow the maintaining of the spherical corneal shape and solve the problems caused by tensile tests (16).
The aim of this work was to evaluate the effect of CXL treatment in terms of corneal stiffness, by comparing the elastic properties of treated corneas and controls by means of an inflation procedure.
Methods
Samples
Twenty-four fresh porcine eyeballs were used in this study (Fig. 1A). Collection of samples, taken from animals aged 9 months, was accomplished within 4 hours post mortem. Among the 24 eyes, 12 were treated with CXL, while the other 12 were used as controls. All samples were cut to obtain a central disc including both cornea and 2-3 mm of sclera, as shown in Figure 1B, C. In cases of corneas subjected to CXL, cutting was done after the treatment.
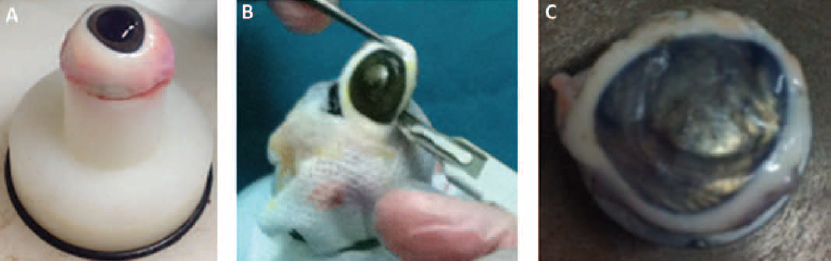
A typical fresh porcine eyeball (
All corneas were kept in a refrigerator in a storage medium (Eusol C; AL.CHI.MI.A. s.r.l, Italy) for 48 hours to prevent their dehydration and allow an uniform cross-linking distribution, and then brought to room temperature before being tested.
Corneal thickness measurement
Corneal thickness was measured by using high-resolution, noncontact optical coherence tomography (OCT) with a Visante (Carl Zeiss Meditec, Jena, Germany), with an optical axial resolution of 18 µm and a lateral resolution of 60 µm.
Corneal thickness measurements were performed before and after treatment, as well as before inflation test. A scanning protocol was chosen for the thickness evaluation (33). OCT images were considered to be of adequate quality according to a good demarcation of both anterior and posterior corneal boundaries and the absence of artifacts. Figure 2 shows a typical OCT image of the cornea.

Example of a typical optical coherence tomography (OCT) image of the cornea.
Corneal cross-linking treatment
All CXL treatments were performed by the same surgeon in accordance with standard clinical procedures (5). The whole epithelium was removed from the cornea with a metal spatula to allow the photosensitizer solution to diffuse into the stroma. Prior to irradiation, the cornea was soaked with a riboflavin 0.1%–dextran 20% solution (Ricrolin Sooft Italia, Montegiorgio Fermo, Italy) for 20 minutes to facilitate the UVA absorption. Then the cornea was exposed to UVA emission for 30 minutes (370 nm, 3 mW/cm2), while dropping the riboflavin 0.1%–dextran 20% solution every 2.5 minutes. CXL treatments were completed within 6 hours of collection of the eyeballs.
Equipment
In this study, inflation test equipment, schematized in Figure 3, was used in order to inflate ex vivo porcine corneas and measure the anterior cornea apex displacement as a function of the inlet pressure. The main components of the equipment were an inductive displacement transducer (W50; HBM, Germany) with loose plunger and full scale of ± 50 mm; a strain gage pressure transducer (P3M; HBM, Germany) with a full scale of 10 bar; an acquisition board NI SCXI-1000 (National Instruments, USA) connected to a PC by means of a NI SCXI-1200 USB module. Specifically, the acquisition board was composed of a conditioning module for strain gages NI SCXI-1121 with terminal block NI SCXI-1321 and a conditioning module for LVDT sensors NI SCXI-1540 with terminal block NI SCXI-1315.
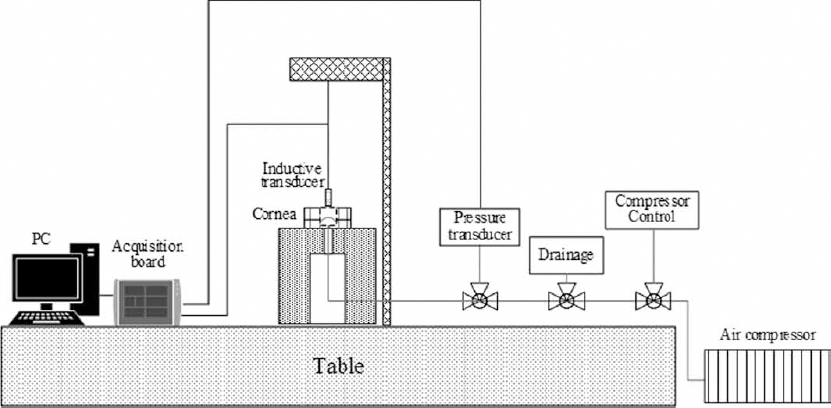
Diagram of the instrumentation used during inflation tests.
The compressed air circuit consisted of an air compressor with pressure tank (Kraft, USA), a tap serving as control valve to regulate air pressure in the test circuit, a T junction connecting the air circuit with the pressure transducer, and a pressure relief tap. All of these components were linked to the cornea holder by means of plastic piping and quick release couplings.
Experimental procedure
The cornea was placed in a metal seat consisting of 2 rings with edges about 4 mm in height. The cornea was then clamped between the 2 rings along the sclera, so that there was no risk of cutting the cornea surface during tightening. The holes in the 2 rings allowed the passage of compressed air and the positioning of the displacement transducer (Fig. 4).

Cornea placed in the bottom circular seat (
A rocker arm system (Fig. 5) was built to apply the same constraint condition on the entire edge of the sample. The 2 threaded bars were first placed in equilibrium, and then, with a key and an appropriate reference, they were alternately tightened so as to perform every time a quarter turn for both bars. The force imposed on the edge of the sample had to be sufficient to keep the cornea at its initial position without compromising its integrity. Indeed, excessive pressure would cause damage to the sclera-corneal edge and affect the reliability of the test. For this reason, a torque measurement was employed: the right tightening was achieved when a contact pressure of 12 MPa was registered.

Details of the equipment. Plunger and corneal seat (
The tip of the displacement transducer – centered with respect to the hole of the upper ring holding the cornea – was in contact with the center of cornea, and this position was set to zero. Furthermore, the pressure inside the piping was checked to be practically zero before starting the experiment. The control tap was carefully operated allowing the air gradually to inflate the cornea while reaching the maximum testing pressure (about 0.8 bar).
A program made with LabVIEW (2009; National Instruments, USA) was used for balancing the forces acting on the cornea seat and recording both pressure and corneal displacement during the inflation test. The sampling frequency was set to 1,000 Hz.
Mechanical model of cornea
A simple theoretical model based on linear shell theory was used for processing the experimental data (18, 34). Furthermore, it was assumed that the cornea had negligible bending stiffness (35).
The corneal geometry could be approximated to a homogeneous shell with both known geometry and load distribution acting on it, as represented in Figure 6A. The radius of the shell curvature R and the angle α were calculated as:
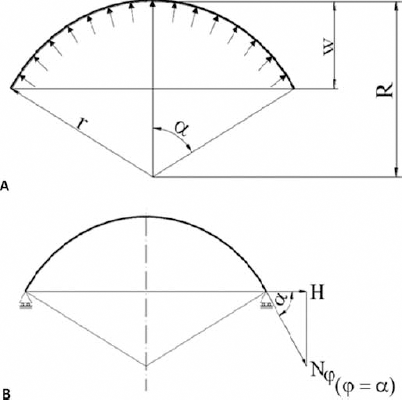
Schematic representation of the circular thin shell used in the analytic calculations.
where r is the radius of cornea subjected to inflation, and w the displacement measured by the transducer.
By taking into account the constraint conditions imposed on the cornea (sealed between 2 rings), the force schematization, shown in Figure 6B, was applied for data evaluation. Force H was calculated by applying the equilibrium on the membranal forces acting on the cornea. According to the membranal theory (36), stress (σ) and strain (ε) can be expressed as follows:
where p is the inlet pressure.
Elastic modulus evaluation
The elastic modulus was then calculated as the slope of the stress-strain characteristic (loading curve) in 2 pressure intervals: 2-4 kPa (physiological range of intraocular pressure [IOP]) and 40-60 kPa.
In the present work, a simple procedure for evaluating the average elastic modulus of the cross-linked portion of cornea was developed. To obtain an estimation of the cross-linking effect, some hypotheses were made on the distribution of corneal elastic properties. Specifically, the elastic modulus of the cross-linked portion (240 μm (14)) was considered constant along its depth, as well as that of the non-cross-linked portions. It was thus possible to schematize the cornea as made of 2 layers. By knowing the elastic moduli of both treated and untreated corneas, the following equation was obtained:
where s is the corneal thickness measured by OCT, ECXL the mean elastic modulus of the cross-linked layer, EmCXL the mean elastic modulus of cross-linked corneas and EmC the mean elastic modulus of normal corneas.
Statistical Analysis
One-way ANOVA was applied to assess the difference in thickness among the measurements done before and after CXL, and 48 hours after CXL. A 2-sample t-test was used to compare treated corneas and controls in terms of elastic modulus. A p value ≤0.05 was chosen to indicate a significant difference.
Results
A significant reduction in corneal thickness, up to 34%, was found immediately after CXL (p<0.001). Specifically, an average decrease of 345 ± 21 µm was found, referring to the initial thickness which varied between 814 µm and 1,189 µm for cross-linked corneas, and between 825 µm and 1,171 µm for controls (Tabs. I and II). However, corneal thickness returned to approximately the initial values after immersion in Eusol C for 48 hours. Indeed, no statistically significant difference (p = 0.147) was found when comparing thickness before treatment and after immersion in the storage medium.
Thickness of corneas subjected to CXL treatment
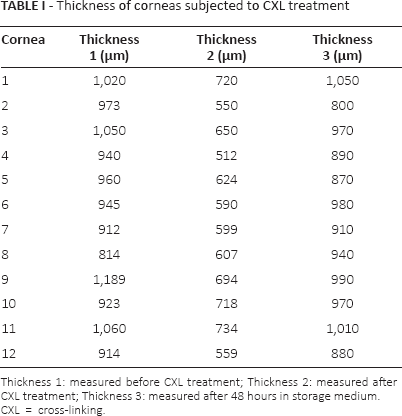
Thickness 1: measured before CXL treatment; Thickness 2: measured after CXL treatment; Thickness 3: measured after 48 hours in storage medium.
CXL = cross-linking.
Thickness of control corneas
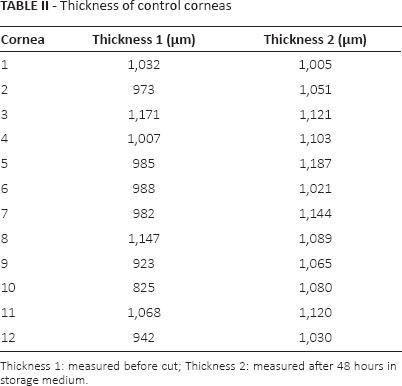
Thickness 1: measured before cut; Thickness 2: measured after 48 hours in storage medium.
Figure 7 shows the typical pressure-corneal apex displacement curves as well as stress-strain for controls (black curve) and treated corneas (gray curve), obtained by inflation tests. The pressure-apical displacement curve of the cornea shows a first part with low stiffness and then, corresponding to a pressure of 0.05 bar, a subsequent stiffening, as shown in Figure 7A.
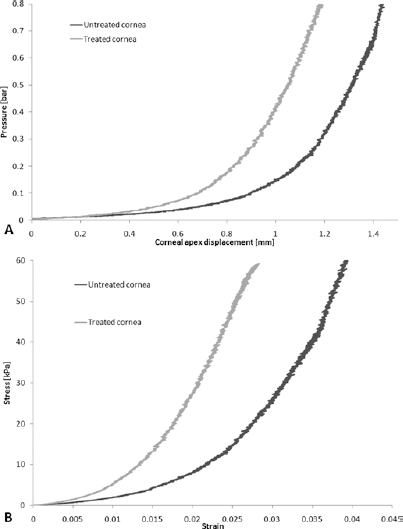
Typical load–corneal apex displacement (
The results showed that there was no statistical significant difference (p = 0.058) between the average elastic modulus of treated corneas (356 ± 159 kPa) and controls (247 ± 169 kPa), calculated in the range of 2-4 kPa. A significant increase (p<0.0001) was found when operating in the range of 40-60 kPa, with a mean of 3,868 ± 502 kPa for cross-linked corneas and 2,727 ± 238 kPa for untreated corneas, an average increase of about 42%.
By applying the 2-layer model and Equation 5, with an average thickness of 900 µm and a cross-linked portion of 240 μm, it was possible to estimate the elastic modulus of the cross-linked layer (656 kPa), which was 84% more than the mean value found for the whole cross-linked cornea. This method allowed the estimation of an increase of the elastic modulus of human corneas subjected to CXL treatment of about 55%.
Discussion
The ability to understand and predict the corneal response to pathological conditions and to new surgical therapies like cross-linking is of great clinical importance. However, corneal material properties reported in the literature vary widely, almost by orders of magnitude (17), and the variation seems to be related to a number of factors such as the different test methods, corneal viscoelastic behavior, IOP and velocity of the applied load.
The aim of this study was to assess the effect of CXL treatment on ex vivo porcine corneas in terms of elastic properties, by inflation tests. Such tests were performed on corneas of circular shape, surrounded by 2-3 mm of sclera acting as a clamping and sealing area. This solution allowed proper tightening during the test.
The mechanical model used in this study describes the corneal behavior taking into account the dimensions involved (thickness to radius ratio of the specimen less than 10), the characteristics of the material and the type of test performed. This model is similar to that of previous inflation studies (16, 18-19-20, 35, 37) although with further assumptions due to the constraints acting on the sample.
Although several other studies on the subject of this present study have been carried out in the last decade, only one (Kling et al in 2010 (37)) investigated the stiffening effect of cross-linking on ex vivo porcine corneas. In their experimental system, the whole porcine eye was inflated with saline solution by means of a needle. This experimental setup allows the maintaining of the integrity of the eye, but the procedure cannot be used on human donor corneas; in clinical practice, it is known that only corneas surrounded by a thin ring of sclera are available from donors. Both the equipment and procedure applied in the present work are, in contrast, easily usable for all kind of corneas, as well as reproducible.
All corneas were inflated with air to a pressure up to 0.8 bar (far above the physiological IOP), and the corneal apex displacement was measured by a displacement transducer. The pressure variation was manually regulated by the same operator to keep the same loading velocity, as this feature influences the repeatability of the experimental procedure.
The relationship between pressure and corneal deformation was found to be highly nonlinear, with 2 distinct phases, and significant stiffening over a pressure of about 0.02-0.04 bar. This result is in agreement with previous studies (15, 16, 25, 34, 35, 38, 39).
The first finding of this study was a significant reduction in corneal thickness, up to 35%, obtained immediately after CXL. This is due to the strong dehydrating effect occurring during the treatment, as previously reported by other authors (37, 40-41). However, the effect was completely reversible as corneal thickness returned to the initial values after immersion in the medium storage. Indeed, the change of thickness due to changing hydration may also influence the biomechanical results (42), but this study eliminated these changes of thickness by immersing corneas for 48 hours in Eusol C.
The most significant result was the stiffening of porcine corneas subjected to CXL treatment by 42% in comparison with untreated corneas. This finding confirms the ability of CXL treatment to modify the internal corneal structure by bundling collagen fibers. As a consequence, the passage between first and second phase in the stress-strain curves was at lower loads, so that the range of physiological pressure was dominated by collagen with higher stiffness (Fig. 7).
The literature shows that the combined effect of UVA and riboflavin is concentrated in the first 240 µm of corneal thickness (14) which accounts for about 60% of the total thickness in humans. In porcine corneas, however, CXL treatment involves only 25%-30% of the corneal thickness, thus the stiffening effect will be less evident than that on human corneas.
The different average thickness between human and porcine corneas (550 µm vs. 900 µm) and the higher UVA coefficient of absorption for human corneas (i.e., a greater portion of the human cornea can be cross-linked), indicate that the stiffening effect due to CXL may be much higher in human corneas (7, 9). Indeed, reports in the literature have shown that the CXL effect is more evident on corneas affected by keratoconus (14).
The 2-layer model, developed in this work, allowed the evaluation of the elastic modulus of the cross-linked portion of cornea which was nearly twice the elastic modulus of the whole cross-linked corneas. By hypothesizing that human and porcine cornea have the same elastic modulus for the cross-linked portion (it is not possible to use any reports in the literature as a reference for human elastic modulus due to the high variability in the results (10)) and considering a mean thickness of 550 μm, the stiffening effect due to cross-linking can be calculated to be up to 55% for human corneas (11).
Inflation tests have been proven to be a valuable tool for investigating corneal elastic properties and assessing the efficacy of CXL treatment in porcine corneas.
Footnotes
Financial support: No grants or funding have been received for this study.
Conflict of interest: None of the authors have any proprietary, financial, professional or other personal interest of any nature or kind in any product, service and/or company that could be construed as influencing the position presented in, or the review of, the present manuscript.