Abstract
Introduction
Tissue engineering is a field which is currently under a great deal of investigation for the development and/or restoration of tissue and organs, through the combination of cell therapy with biomaterials. Rapid prototyping or additive manufacturing is a versatile technology which makes possible the fabrication of three dimensional (3D) structures from a wide range of materials with complex geometry and accuracy, such as scaffolds.
Aim
The aim of this study has been to investigate the interaction between mesenchymal stem cells with poly (ε-caprolactone) (PCL) biomaterials used for obtaining scaffolds through additive manufacturing.
Materials and Methods
Scanning electron microscopy, confocal microscopy and biological assays were performed to analyse the successful interaction between the cells and the biomaterials.
Results
As a result, the number of viable cells attached to the scaffolds was lower when compared to the control group; however, it was possible to observe cells in the scaffolds since day 1 of analysis, with regions of confluence after 21 days of seeding.
Conclusions
To conclude, these biomaterials are interesting if used as medical artifacts, principally in tissue with prolonged regeneration time and which requires 3D supports with good mechanical properties.
Introduction
The loss or failure of an organ or tissue represents frequent and devastating problems in health care. Thus, the need for substitutes to replace or repair tissue or problematic organs is overwhelming. Tissue engineering (TE), therefore, can provide a way of regenerating damaged tissue with the association of stem cells (SCs) with biomaterials (1, 2).
TE was first defined by Skalak and Fox (1998) (3) who defined it as the application of principles and methods of engineering and life sciences toward the fundamental understanding of structure-function relationships in normal and pathological mammalian tissues and the development of biological substitutes to restore, maintain, or improve tissue function.
Under these considerations, scaffolds used in TE must provide sufficient initial mechanical strength and stiffness for wound contraction forces and later for the remodelling of the tissue. Furthermore, scaffold architecture should enhance initial cell attachment and subsequent migration into the matrix; it must also enhance the mass transfer of metabolites and provide sufficient space for remodelling of the organized tissue matrix and development of a vasculature (4).
Several techniques for manufacturing polymer-based scaffolds are available today; however, additive manufacturing offers the possibility of strictly controlling complex details, such as pore geometry, size, and interconnectivity, as well as the spatial distribution of pores within the structure, providing a more suitable 3D scaffold for cell growth in order to mimic the extracellular matrix (5, 6).
Nowadays, 3D printing or rapid prototyping is transforming into a manufacturing focused process and a Committee (F42) of the American Society for Testing and Materials (ASTM) was established in 2009 to be responsible for this. This committee defined the official name of the technology as “additive manufacturing”. ASTM is also integrating its efforts with ISO (261 Technical Committee) in the area of test methods, processes, materials, terminology and design. It includes a new Standard Specification for Additive Manufacturing File Format (AMF) for a better and more complete representation of complex objects (7).
ASTM defined additive manufacturing by the “process of joining materials to make objects from 3D model data, usually layer upon layer, as opposed to subtractive manufacturing methodologies, such as traditional machining” (8). Moreover, this technique enables the production of patient-specific scaffolds that precisely match a patient's contours, in conjunction with non-invasive imaging technology and computer models.
The most popular polymers used to construct material are polylactic acid (PLA), polyglycolic acid (PGA) and poly (ε-caprolactone) (PCL) (9). PCL takes 2 to 3 years to degrade, owing to its hydrophobic nature but it displays relatively higher ductility (5). It could serve as a structural guide until tissue regeneration is completed and could also be a good option for the regeneration of large defects (5).
To facilitate these processes, mesenchymal stem cells are largely used in this field, due to their great plasticity, giving rise to several types of cells (10, 11). Moreover, these cells are easily cultivatable in laboratories for posterior implants in vivo.
With the aim of evaluating cell response for PCL 3D-printing scaffolds, mesenchymal stem cells from human dental pulp were seeded on the scaffolds and biological evaluations were performed.
Materials and Methods
Additive manufacturing
PCL moulds were fabricated by an extrusion process by additive manufacturing (AM) through a 3D printer called Fab@CTI (Fig. 1) (12, 13). It is an open-source design AM machine, based on the Fab@Home (14), and it was built and adapted at the Centre for the Renato Archer Information Technology (CTI) with the purpose of collaborating in research initiatives in the bioengineering and biomaterials fields, having partners in many research institutions. Thereby, being an open-source project, Fab@CTI facilitates applications that require wide flexibility of settings and the capacity of reproducing complex geometries, which are basic requirements in biofabrication. The PCL used was in wire format and the scaffolds were printed with five slices of polymer (Fig. 2) of approximately 0.6 mm diameter in a 3D printer. They were produced with different air gaps, which refers to the space found among successive layers, as follows: Group 1, 0.1 mm; Group 2, 0.15 mm; Group 3, 0.2 mm; Group 4, 0.3 mm, and; Group 5, 0.4 mm. For biological analysis the scaffolds were sterilised by UV radiation for 2 hours.

The Fab@CTI 3D printer.

PCL 3D-scaffolds made by additive manufacturing.
Morphology and fibre diameter of the scaffolds
The morphology of the matrices was evaluated by scanning electron microscopy (SEM) model JOEL-JSM 6060, with acceleration voltage of 10 kV. The diameters of the fibres were evaluated by reading 10 fibres of the same sample in triplicate, resulting in 30 fibres being analysed per group by ImageJ software.
Isolation and cultivation of stem cells
For the study, mesenchymal stem cells (MSCs) isolated from tissue pulp from deciduous teeth were used. The teeth were extracted from children in good general health who were enrolled on the paediatric dentistry programme of the Faculty of Dentistry at UFRGS, after informed written consent of the parents/guardians (n° 296/08). The collection, isolation and characterisation of the pulp tissue MSCs were carried out in accordance with the established protocol described by Bernardi and coauthors (15). After isolation, the adherent cells were cultivated in a DMEM culture medium (
Seeding of the mesenchymal stem cells
For biological assays, the scaffolds were distributed in cultures plates (96 wells) and 5000 cells were seeded in each one. The cells seeded onto the scaffolds were maintained in culture for 21 days (the period of the experiments) and the medium was changed each 3-4 days.
Cellular viability test
The biological analysis consisted of a viability test, performed with WST-8 reagent (Sigma-Aldrich®). To perform this test, all the placement of the scaffolds was first changed, i.e. they were put in different wells to avoid erroneous reading of the test. The WST-8 reagent was added at this moment and left in contact with the cells for 2 hours, according to the manufacturer's instructions. Following this, the solution was read at 450 nm in a Wallac EnVision® plate reader (PerkinElmer). A control group, which consisted of cells directly cultivated on the well, was also evaluated by WST-8 assay. Three different cultures of MSCs from dental pulp were employed for this analysis and they were evaluated after 1, 4, 7, 15 and 21 days after the seeding process. The experiments were performed in triplicate.
Evaluation of the presence and morphology of cells on the scaffolds
The morphology of the cells was also evaluated by SEM. For this analysis, the scaffolds with the cells were first fixed with glutaraldehyde 3% (w/v) and then dehydrated with increased concentrations of ethanol. The matrices with the cells were then metalised and the analysis was performed.
Confocal microscopy (Olympus FV1000) was used to evaluate the morphology of the cells. For this test, the cells were fixed with parafolmadehyde 4% (w/v) and stained with DAPI (5 µg/mL) to observe the nuclei of the cells and with phalloidin (20 µg/mL) to stain the actin filaments. Cells directly seeded in the wells of the culture (control group) plate were also evaluated by confocal microscopy.
Both analyses were performed after 1, 4, 7, 15 and 21 days after the seeding process.
Statistical Analysis
Fibre diameter was compared using Student's t-test for unpaired samples. The cellular viability test was assessed by ANOVA for repeated measures with two classification criteria: time and group. P<0.05 was considered statistically significant.
Results and discussion
Morphology and fibre diameter
The analysis of the morphology of the scaffolds by SEM showed well-formed fibres. It is possible to see several layers of fibres in different arrangements. It is also possible to observe that there are differences in terms of fibre diameter and space between them, also known as air gaps, for the five groups considered (Fig. 3A-E). Group 1 showed the smallest space between the fibres, as was expected. The fibre widths were 645.42 ± 72.65, 596.80 ± 88.71, 648.93 ± 75.22, 581.28 ± 62.98, and 583.04 ± 75.03 micrometres, respectively, for groups 1, 2, 3, 4, and 5. There was no statistical difference among the groups (p>0.125 for all comparisons).

Morphology of the scaffolds analyzed by SEM. (
Cellular viability test
The viability assay showed that all the scaffolds demonstrated the same behaviour, with a little increase in the number of the viable cells after 21 days, represented by the increase in absorbance (Fig. 4). There was no statistical difference between these groups (p>0.550 for all comparisons).
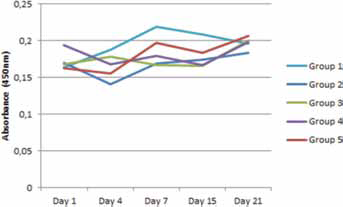
Viability test of mesenchymal stem cells in the scaffolds groups.
The number of viable cells on the scaffolds was smaller when compared to the control group (Fig. 5). The control group presented more viable cells (p<0.001 for all comparisons) than the other groups.
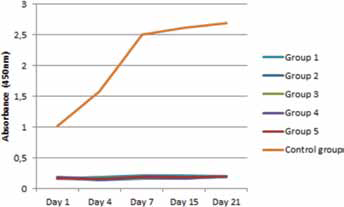
Viability test of mesenchymal stem cells on the scaffold groups and control group.
At the same time, the absorbance of the well, where the cells were seeded on the scaffolds, was measured in the absence of the scaffold; high absorbance was observed, which was almost comparable to the control group (Fig. 6).
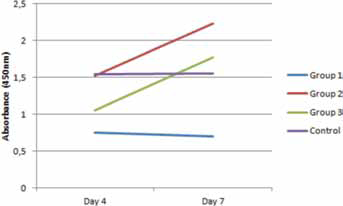
Viability test of mesenchymal stem cells for groups 1, 2 and 3 on days 4 and 7 after seeding the cells on the scaffolds. This analysis evaluated the absorbance of the cells attached on the wells in which the scaffolds were removed before cellular viability analysis.
In relation to time, there was statistical (p<0.001) difference between the number of viable cells over time, i.e. the cells on the scaffolds in all the groups were proliferating and increasing in number.
Evaluation of the presence and morphology of cells on the scaffolds
Although the absorbance of the WST-8 assay on the scaffolds was very low in comparison with the cells seeded on the scaffolds, it was possible to observe cells distributed on the fibres, which formed matrices in all the groups since day 1 (Fig. 7A-D1).
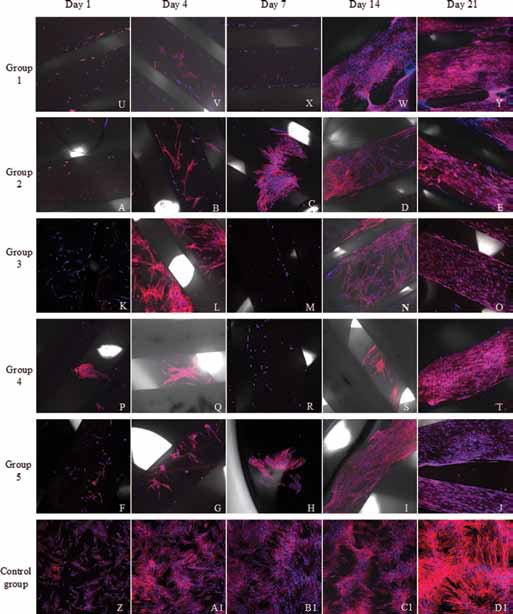
Cells stained with DAPI and phalloidin.
Figure 8A-F shows confocal images of day 1 after seeding for all the groups. These analyses were performed in the wells where the cells were seeded on the scaffolds, but after the removal of the matrices. The control group was also evaluated. From the photographs, it can be observed that the cells that adhered to the wells where the scaffolds were deposited are more grouped, while the cells in the control group are more dispersed.
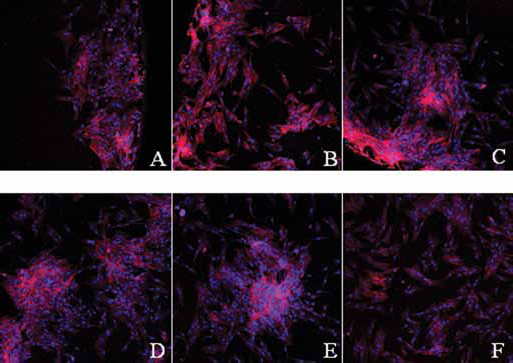
Cells attached on the wells of the culture plates. (
In relation to the results obtained by SEM, it was difficult to see cells on the first days of analysis. From day 14 it was possible to see some cells attached to different fibres (Fig. 9A-C) in groups 1 and 4. On day 21 it was already possible to note the formation of some colonies of cells attached between the fibres (Fig. 10A-B).

(
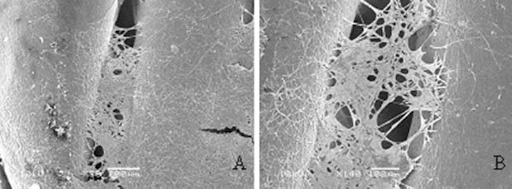
(
For scaffolds to be used in tissue engineering is vital that they meet structural, mechanical, and nutritional requirements. The additive manufacturing technique offers innovative ways to produce these scaffolds with biomaterials; however, this approach is limited by the properties and parameters of the materials, depending on the biomaterial under consideration. In this study, it was possible to construct PCL scaffolds by rapid prototyping with five different air gaps, maintaining similar fibre diameter and morphology.
The choice of MSCs to be used in combination with the constructed biomaterials was based on the fact that these cells can be easily isolated, cultured and expanded in a laboratory and have the advantage of not being immunogenic (16, 17). There are also numerous reports demonstrating that MSCs can repair tissue by directly differentiating towards mesenchymal lineages. Recent works have established that these cells can also enhance the differentiation of other progenitor cells into functional somatic cells. In addition, they may contribute to other aspects of local tissue repair, via paracrine mechanisms (18, 19).
With a view towards the benefits of the use of MSC in tissue engineering, these cells were seeded on PCL scaffolds which were constructed by additive manufacturing for up 21 days. The viability test showed that the cells adhered and proliferated on the scaffolds, although much less than the control, which is the gold standard in cell culture. However, it was also observed that the number of viable cells in the scaffolds increased throughout the period of analysis.
The feasibility of these scaffolds supporting cell growth was also evaluated by image analysis. Using confocal microscopy it was possible observe that the MSC density increased over a 21-day period in all the groups. Moreover, the cells had spread morphology, typical of MSCs in culture, which confirms the affinity of these cells with the biomaterial. Scanning electron microscopy was also used to evaluate the presence and morphology of the cells. By this technique, it was difficult to see the cells on the first days of analysis, but it became easier over time, mainly on day 21 when the formation of some colonies of cells attached between the fibres were observed in group 1. These colonies have the appearance of extracellular matrices, arranged in fibres with each cell being in contact with each other.
As the groups in which the cells were seeded on the scaffolds showed lower absorbance than the control group, it was decided to make an investigation at the place where these cells were attached. This was evaluated by WST-8 assay and also by image analysis. The WST-8 assay of the wells where the scaffolds of groups 1, 2 and 3 were deposited on day 4 confirmed the suspicion that the cells passed through the pores of the matrices and adhered to the plastic of the wells. To visualise the cells on the wells, confocal microscopy was performed. From the photographs, it is notable that the cells that adhered to the wells with deposited scaffolds are more grouped, while the cells in the control group are more dispersed. This is probably due to the fact that in the wells with the scaffolds, the cells passed through the scaffold pores and adhered in more specific places.
To overcome the problem of pore size, which was determined as being the originator of the smaller number of MSCs found on the scaffolds when compared to the control group in this study, different approaches are being used. Infiltration of the printed moulds with another polymer scaffold (5, 20) and also performing a hybrid fabrication by combining electrospinning with additive manufacturing techniques (21, 22) are some examples.
In such cases as those mentioned above, the scaffold acquired a 3D architecture. The matrices which developed operated more as a 2D environment for the cells, since most of the cells adhered and proliferated above the fibres and not between the fibres. Although within a 2D environment, the cells appeared to be comfortable in this structure, as observed by the spread morphology and also by the improvement in the number of the viable cells over the passing of time. Moreover, this structure is a good alternative to be used in tissue engineering for tissue that requires material with strong mechanical properties, as in the case of bones, which take months or years to be healed. We are of the belief that the cells can adhere and proliferate like a 3D tissue if some improvements, as those detailed above, are implemented.
Conclusions
Although the viability test showed a low number of viable cells in the scaffolds, it was possible to visualise cells interacting with the biomaterial and with each other. In addition, the biomaterial worked principally as a 2D environment as the cells attached more to the surface of the fibre and only to a small degree with the 3D architecture of the matrices. It can be concluded, therefore, that the 3D biomaterial structure developed by additive manufacturing with PCL is an interesting artifact to be used in tissue engineering for interaction with cells and for the replacement of tissue which requires long periods of regeneration.
Footnotes
Financial support: This work was supported by CNPq, FAPESP and Stem Cell Research Institute.
Conflict of interest: The authors declare no conflicts of interest.
