Abstract
Background:
The 6-minute walk test (6MWT) is crucial for lung transplants, but traditional testing has limitations. Patients needing high oxygen requirements may not be suited for the pulmonary function testing lab, while physical therapy prioritizes mobility issues. This delays 6MWT administration, hindering transplant evaluation. This project trained respiratory care staff to perform 6MWTs, ensuring efficient and equitable access to this vital test and potentially improving transplant access for critically ill individuals.
Methods:
To address the bottleneck caused by limited PT and PFT lab availability for 6MWTs, we implemented a two-pronged approach. First, we trained respiratory care staff in proper 6MWT administration, equipping them with the necessary expertise. Second, we developed clear protocols to identify patients most suitable for respiratory care-led 6MWTs, ensuring efficient allocation of testing resources. This combined strategy aimed to increase capacity, improve wait times, and ultimately expedite lung transplant evaluation for critically ill patients.
Results:
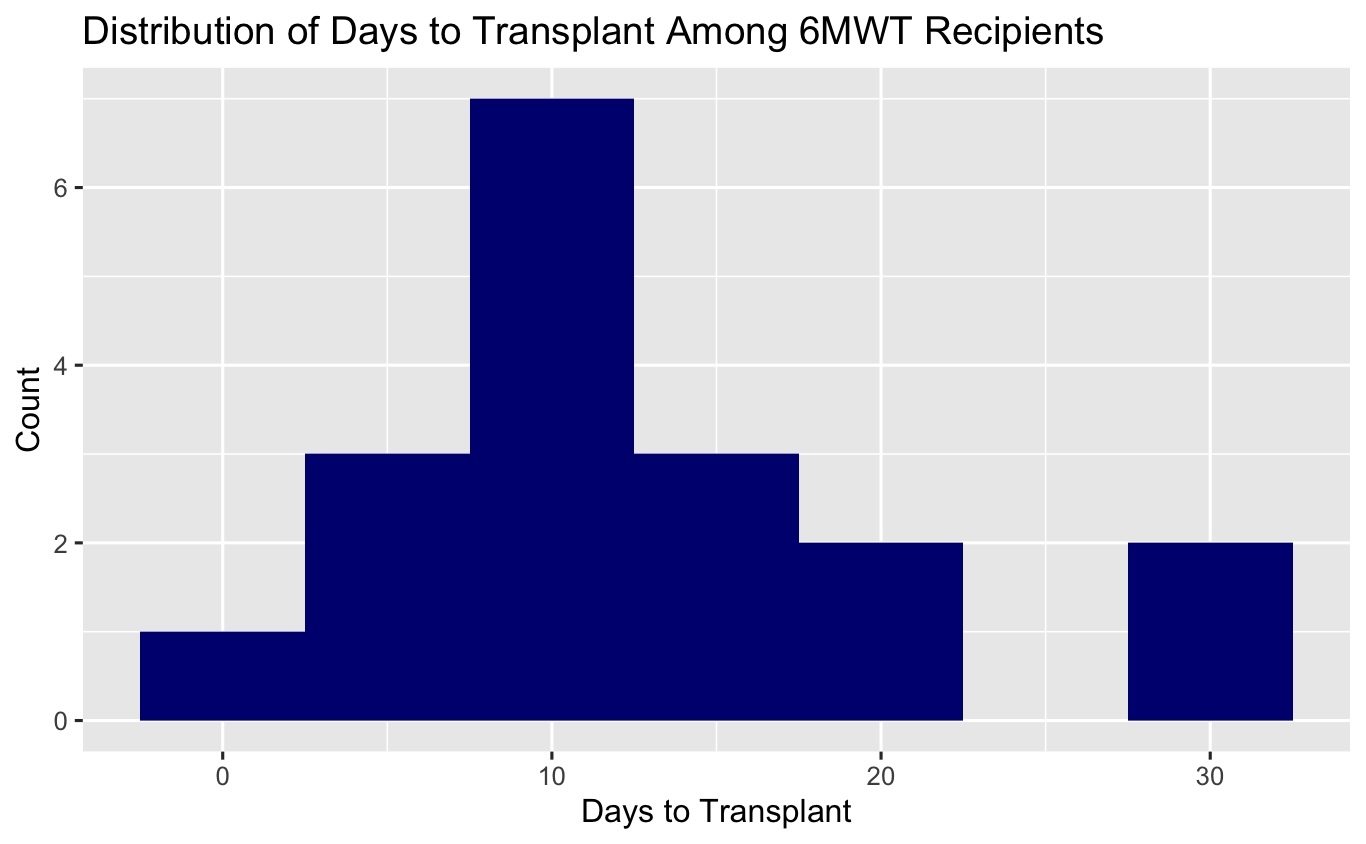
Respiratory care staff were trained to perform 6MWTs, tackling delays caused by limited PT and PFT lab access for lung transplant patients. This expanded our testing capacity and potentially expedited transplants. The average wait time after a respiratory care 6MWT was 12.7 d, highlighting the project’s effectiveness. This approach shows promise for expediting evaluations in other transplant settings.
Conclusions:
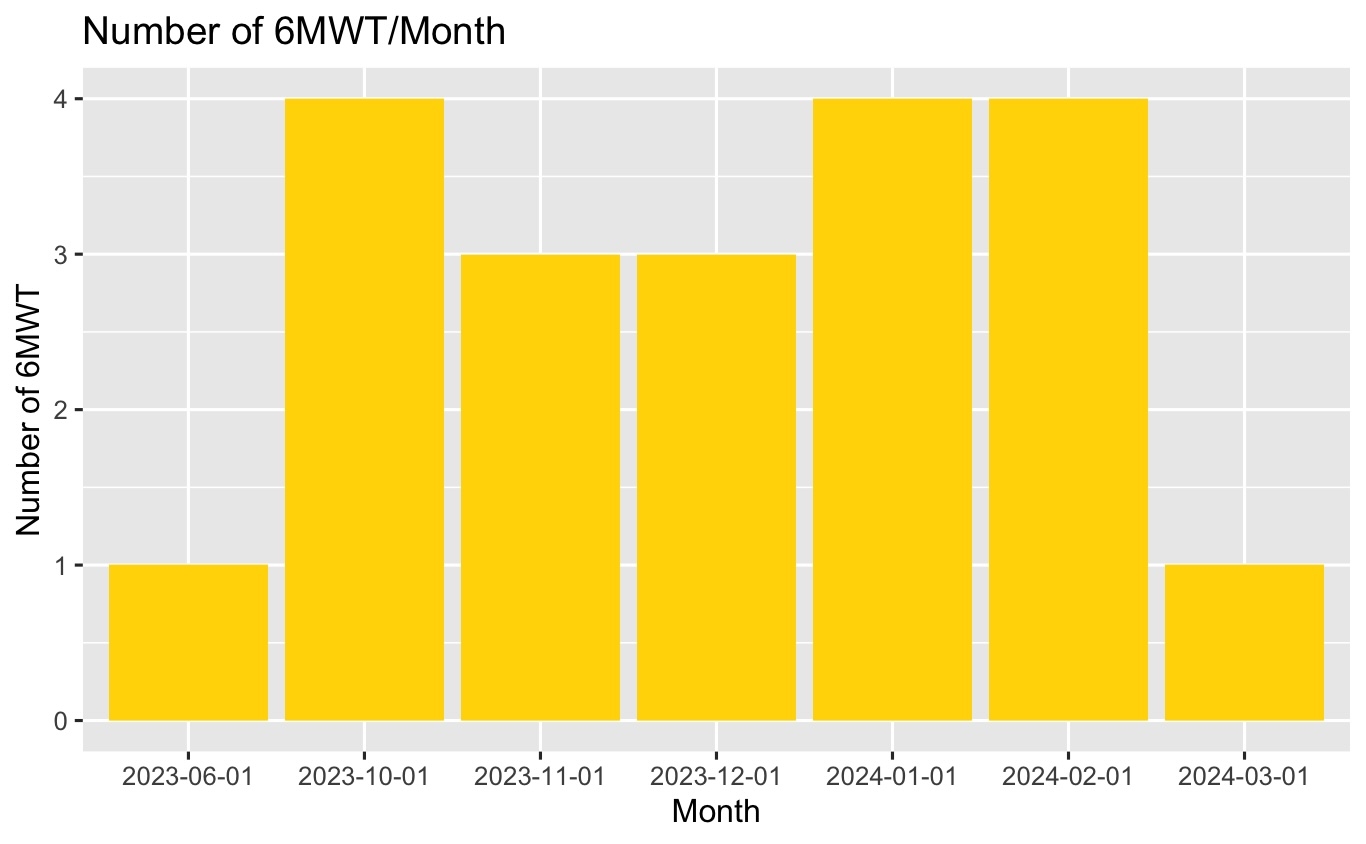
This project addressed the challenge of delayed 6MWTs for lung transplant patients due to limitations in physical therapy and pulmonary function testing lab availability. By training respiratory care staff in 6MWT administration and establishing clear protocols, we significantly increased testing capacity. This resulted in 44 timely 6MWTs performed by respiratory care, with an average wait time for transplant after the test of only 12.7 d. These findings suggest that expanding the role of respiratory care in 6MWTs can improve efficiency and potentially expedite lung transplants for critically ill patients. This approach holds promise for broader application in other transplant settings, warranting further investigation.
Get full access to this article
View all access options for this article.
