Abstract
Background:
Asthma exacerbations (AE) present a significant burden on emergency departments (EDs). Vibrating mesh nebulizers (VMNs) have been shown to increase aerosol deposition leading to decreased admission rates and ED length of stay (LOS), but research specific to VMNs effects on AE patients in the ED is limited. We aimed to improve patient disposition and decrease ED LOS and admission rates by improving VMN accessibility in our 59 bed ED (766-bed Adult Level-1 Trauma, Academic Medical Center).
Methods:
An IRB exempt, retrospective review assessed VMN utilization and patient disposition for ED-diagnosed AE cases between October 2022 and April 2024. VMNs were introduced in the ED in March 2022 with limited utilization due to controller accessibility. Subsequently, VMN controllers were installed in all ED patient rooms in September of 2023. Data metrics for the same 7-month period in subsequent years included total ED encounters, ED LOS and boarding hours per patient for all populations, as well as specific metrics for patients diagnosed with AEs.
Results:
Following VMN controller installation, VMN utilization among asthma patients surged from 11.3% to 53.5%, driven by enhanced accessibility (P < .001). Patient outcomes improved, with a 10.3% increase in ED discharges (P = .04). ICU admissions decreased substantially from 3.1% to 0.8% (P = .03). Although ED LOS increased (271 min vs. 297 min; +9.6%), this trend paralleled that of all patient populations (306 min vs. 333 min; +8.8%), with a 4.6% year-over-year increase in total ED encounters. An increase in boarding hours per patient (2.49 to 3.58; +44%) significantly affected ED throughput, further influencing ED LOS for AE patients.
Conclusions:
The implementation of VMNs in our ED, facilitated by VMN controller installation in patient rooms, has yielded promising outcomes for AE patients. Our study demonstrates a substantial increase in VMN utilization, correlating with higher ED discharges and reduced ICU admissions. While a modest increase in ED LOS was observed post-implementation, consistent trends across all patient populations suggest broader systemic factors influencing ED throughput. The observed rise in boarding hours per patient underscores the ongoing need to optimize ED workflow and resource allocation. Overall, our findings underscore the potential of VMN integration to enhance asthma care in the ED, emphasizing the need for continued evaluation and refinement to improve patient outcomes and ED efficiency.
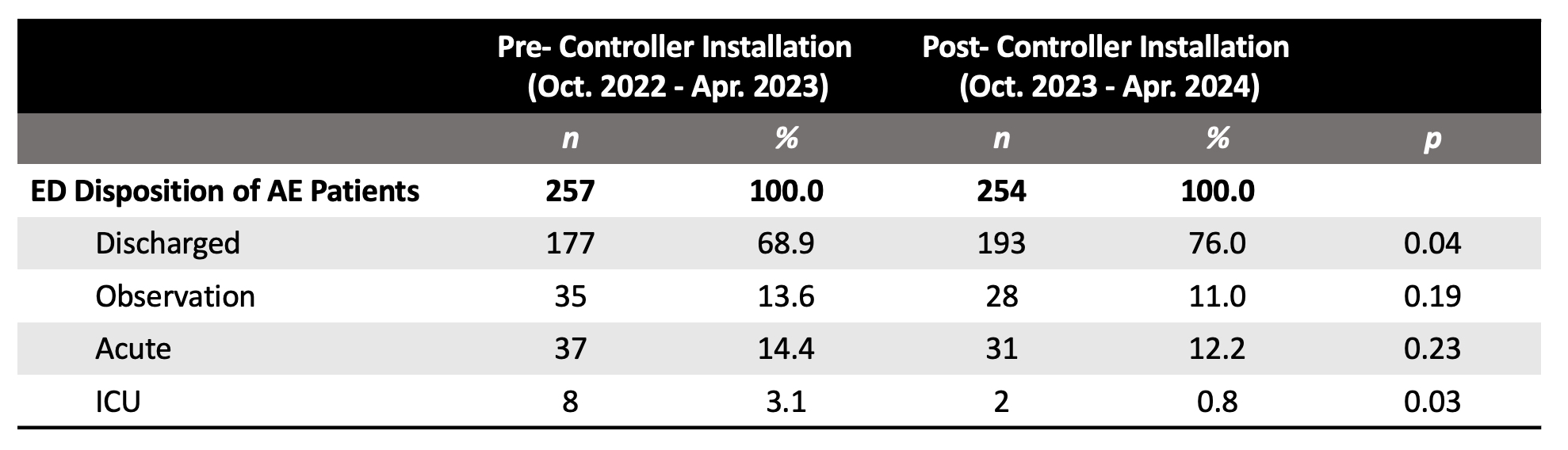
Figure 1 details the utilization rate of VMN for AE patients pre- and post-controller installation. Table 1 details the patient disposition and number of encounters for patients diagnosed with AE in the ED.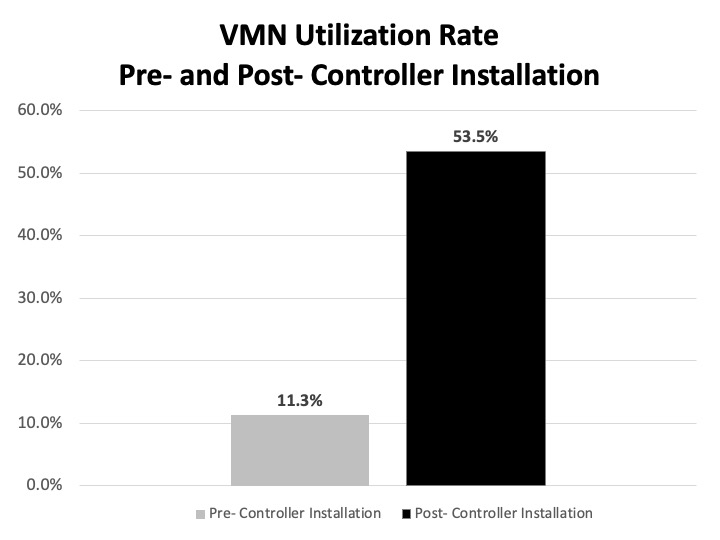
Get full access to this article
View all access options for this article.
