Abstract
Background:
While studies have investigated perceptions of various disciplines on incorporating artificial intelligence (AI) into clinical practice, there has been no exploration within respiratory care. As the role of AI expands, understanding clinicians’ perceptions and knowledge will be crucial for effective implementation. This study aims to assess the familiarity and comfort of undergraduate respiratory care students with AI and explore their perspectives on using AI as an adjunct assessment tool in the clinical setting.
Methods:
A 13-item mixed methods survey was administered via Qualtrics to a convenience sample of undergraduate respiratory care students at Boise State University via Canvas. This study received exempt approval from the Boise State University Institutional Review Board (#IRB24-285). The survey included 5 quantitative Likert-scale questions on familiarity, comfort, and receptivity to AI, 3 demographic questions, and 4 open-ended qualitative questions. Primary outcomes were students’ familiarity and comfort with AI in respiratory care. Secondary outcomes were their perspectives on AI as an adjunct assessment tool. The research team performed an inductive thematic analysis on the open-ended responses following Braun and Clarke’s framework. Theory triangulation was used to ensure data validity.
Results:
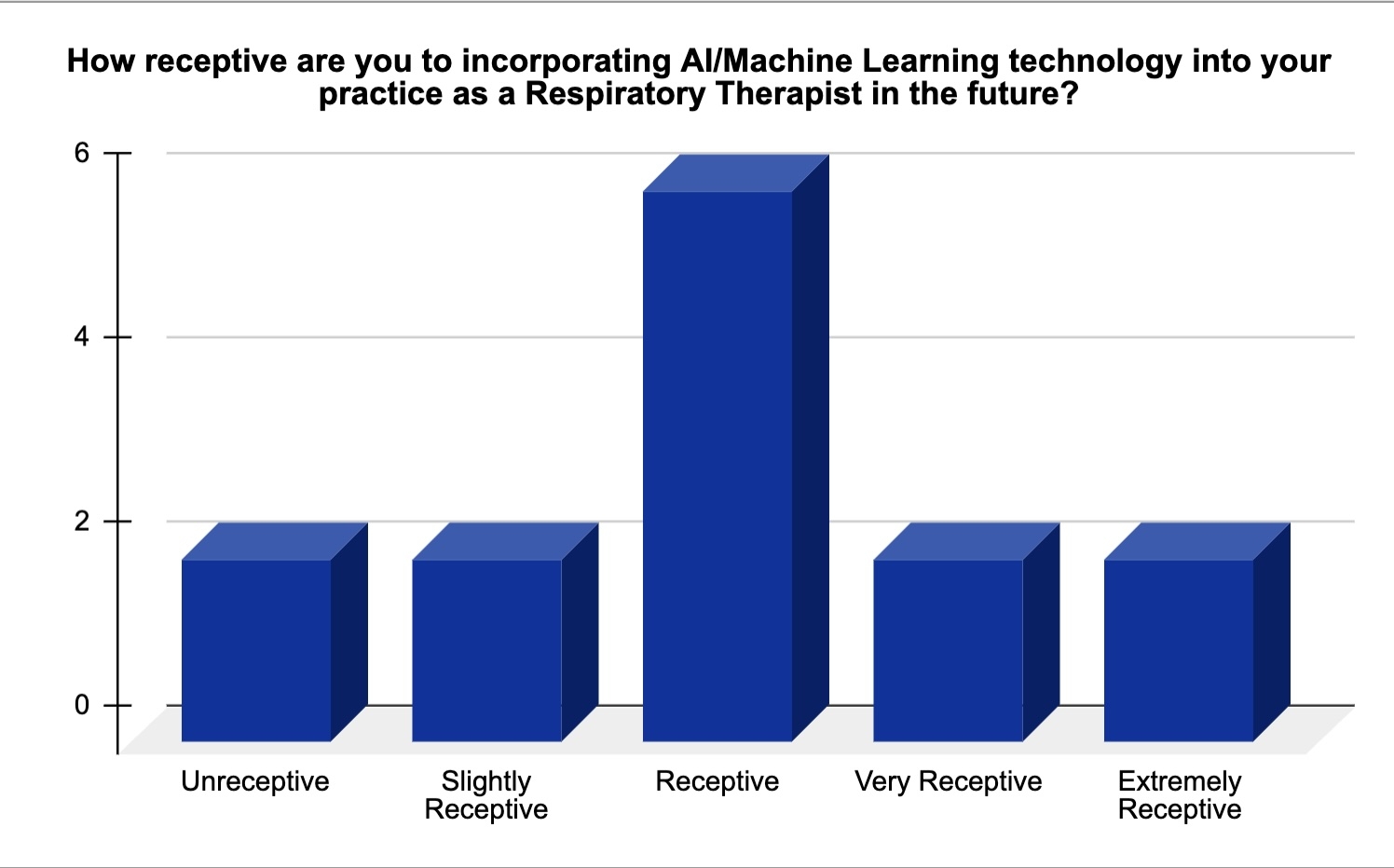
Of the 44 students contacted, 16 completed the survey, a 36% response rate. Incomplete responses were excluded from analysis. The study found that only two respondents were uninterested in incorporating AI into their future practice. Three themes were extracted from the qualitative data: potential, error, and clinical knowledge.
Conclusions:
The survey supports a general qualitative distrust of AI among students, particularly regarding bias, limitations, and safety. Despite this, the survey also supports a quantitative lack of knowledge but openness to further education and future integration. These findings suggest that while concerns about AI persist, there is a willingness among emerging respiratory therapists to learn more and potentially incorporate AI into their practice. Additionally, the students’ limited understanding of bias and ethics in AI highlights a significant opportunity for respiratory care education programs to address these critical issues. By incorporating comprehensive AI ethics and bias training into their curricula, these programs can better prepare students to navigate and implement AI technologies responsibly in the clinical setting.
Table 1 Perspectives of Respiratory Care Students on Use of AI
Emergent Themes
Theme Clusters
Formulated Meanings
Potential
Efficiency
Improves time management; Aids in formulating evidence-based care plans
Human Replacement/ Job Security
Loss of clinical autonomy; AI tools may replace portions of the RT’s role, reducing job security
Unfamiliarity
Benefits unclear; Unfamiliar with AI/ML; Not well covered in undergraduate academic programs
Error
Error
Technology isn’t infallible; Accountability for errors / misdiagnosis; Risk of diagnostic inaccuracy
Error Reduction
Reduces opportunity for human error; Consistent application of evidence-based medicine
Patient Safety
Promotes diagnostic accuracy; Mistakes may be dangerous or worsen outcomes; Implementation of AI-generated recommendations may cause harm to minoritized groups (global majority, LGBTQIA+, disabled, women, veterans, etc.)
Clinical Knowledge
Clinical Expertise
Overreliance on AI tools leading to loss of clinical skill; AI/ML tools don’t understand intricacies of respiratory care practice
Limitations of AI
Accuracy of information pulled from large language models is unknown; Needs strict oversight
Bias
AI perpetuates existing biases due to human-influenced data compilation; Ethical concerns about potential harm to underrecognized groups
Get full access to this article
View all access options for this article.
