Abstract
Background:
A spontaneous breathing trial (SBT) is a test for critically ill patients in the ICU to assess their readiness to be liberated from mechanical ventilation and their capacity to sustain adequate ventilation and oxygenation before removal of the endotracheal tube. However, there are a variety of factors that lead to delays in extubation after a successful SBT. Therefore, we aimed to investigate the possible causes of delaying extubation after the patient has successfully passed SBT in the ICU from an interprofessional perspective.
Methods:
A cross-sectional study was used. A paper copy survey was distributed to physicians (consultants, fellows, and residents), respiratory therapists (RT), and nurses working in ICU from all Medina’s hospitals (secondary and tertiary), Saudi Arabia from March 2023 to April 2023. The survey questions focus mainly on the factors affecting timely extubation after a successful SBT trial.
Results:
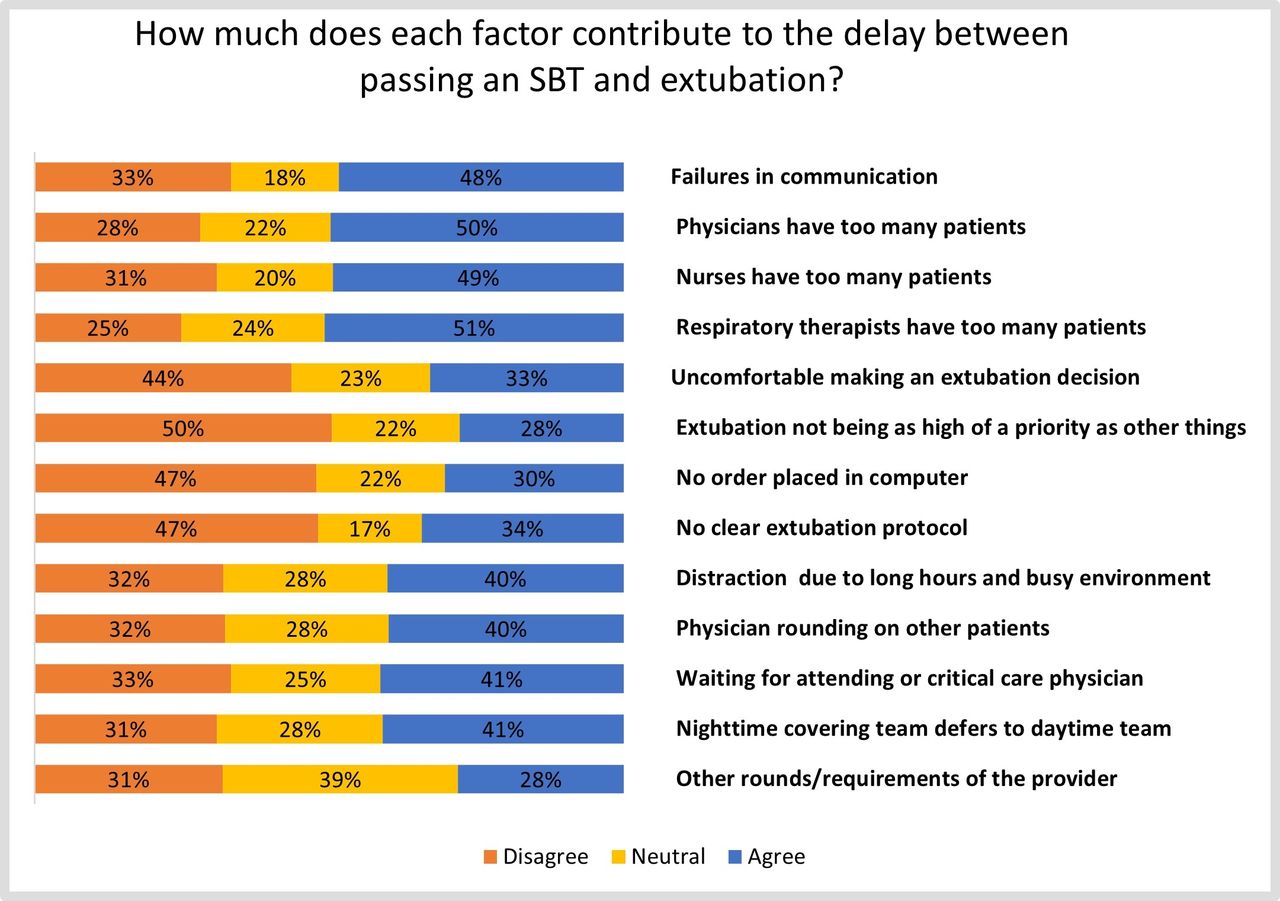
213 healthcare providers completed the survey, of which 53% were male, and 50% aged 20–29 years old. The study participants were 41% nurses, 34% RTs, and 24% physicians. Most participants (71%) consider that the adequate timing of liberation from mechanical ventilation after passing SBT trial is between 0-3 hours and 62% believe delaying extubation up to 3 hours is just about right. With regard to negative effect of delayed extubation, we found a lower proportion of nurses who were aware of the consequences of delayed liberation compared to physicians and RT (43%, 90%, and 78%, respectively P < .001). The most common factors that contribute to delaying extubation were physicians, nurses, and RT having too many patients, in addition to the failure of communication between physicians, nurses, and RTs (see Figure 1).
Conclusions:
Considerable proportion of the ICU workers reported delaying extubation to more than 3 hours that may have several drawbacks for critically ill patients. In addition, the barriers to timely extubated were mainly centered around poor communication between health practitioners and high workloads. These are modifiable factors that should be addressed by hospitals and policymakers in the ICUs to reduce the timing from passing SBT and extubation.
Get full access to this article
View all access options for this article.
