Abstract
Background:
In March 2020, the CDC implemented the diagnosis code of U07.1 COVID-19. Tracking reports of the condition was critical and many health centers submitted clinical data to national NIH-sponsored platforms like the National COVID Cohort Collaborative (N3C) and industry-focused Big Data EMR aggregators like TriNetX. TriNetX COVID-19 Research Network includes data from 87 healthcare organizations (HCO) from 11 countries. UTMB contributes data to both N3C and TriNetX platforms. Reports that illness from COVID-19 infection could persist or recur following the acute phase resulted in the CDC added the ICD-10 code, Post COVID-19 condition, unspecified (U09.9), in October 2021. UTMB opened an interdisciplinary Post-COVID clinic in August 2020 to address the needs of individuals with lingering symptoms. These symptoms contribute to decreased quality of life, increased morbidity, and disease burden. More than 900 patients visited our facilities between March 2020 and December 2022. Many who complained of dyspnea and fatigue were referred for pulmonary function testing (PFT) and rehabilitation. Data collected reveals that completing eight weeks of pulmonary rehabilitation (PR) significantly improves dyspnea and functional ability. We aimed to determine the incidence of U09.9 reported in TriNetX and if PR was utilized.
Methods:
The TriNetX database was queried to select patients diagnosed with a U09 diagnosis, who had charges for PR [CPT (94625, 94626, 1036835, or 1015099)] on or after the diagnosis.
Results:
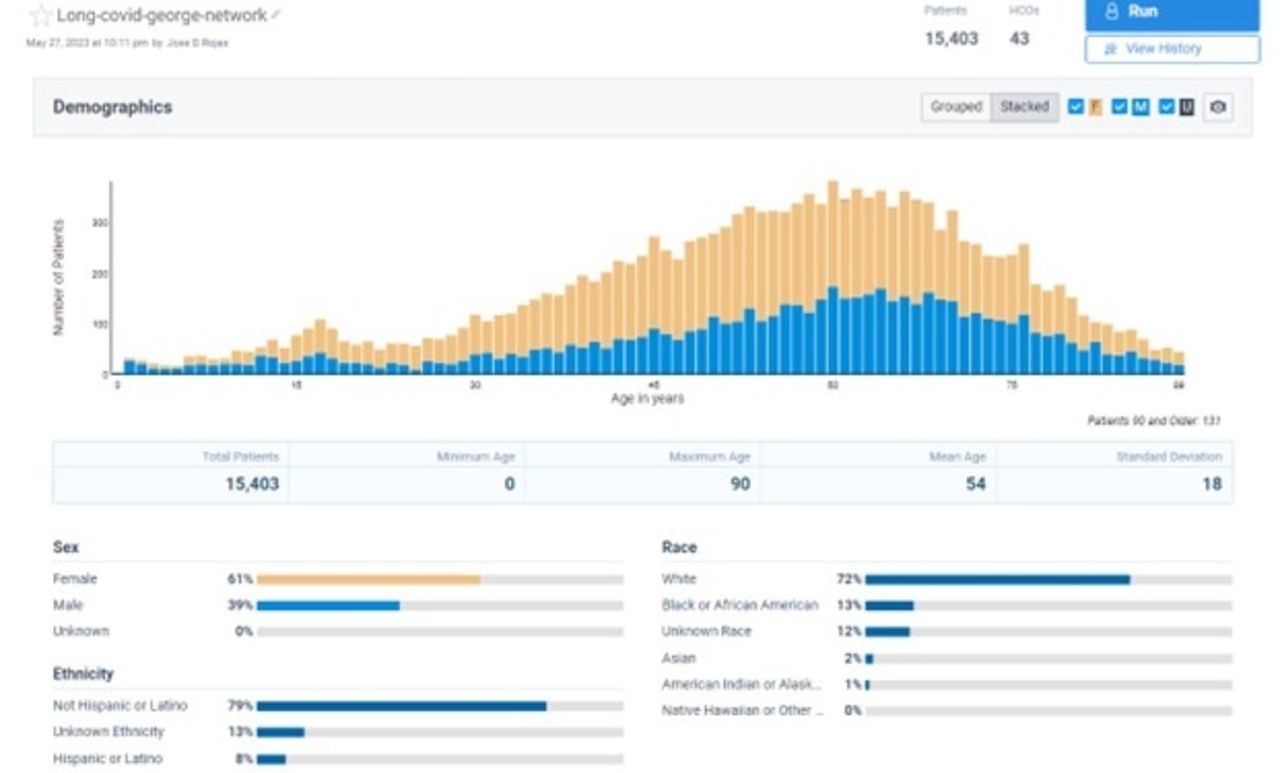
Forty-three of the HCO reported patient data for the above criteria. A total of 79,741 patients had an ICD-10 U09.9 diagnosis, and 15,403 had records for PR. Mean age was 54 ± 18yo at the time of diagnosis and 61% percent were female. Race/Ethnicity distributions were 72% white, 13% Black/African American, 8% Hispanic/Latino, and 8% unknown. Data reveals that within 3 months of the ICD-10 U09.9 diagnosis, 13% of the cohort also had a diagnosis for chronic lower respiratory diseases, with the majority being asthma (8%). Furthermore, 21% had records for bronchodilators and 12% for PFT or rehabilitation.
Conclusions:
Evidence shows that patients with post-acute sequela of SARS-CoV-2 have lingering respiratory symptoms and post-exertion fatigue/malaise, and PFTs and bronchodilators are frequently ordered. PR seems to be underutilized despite reported benefits. More studies are required to determine the barriers to the utilization of PR.
Get full access to this article
View all access options for this article.
