Abstract
Background:
Direct sampling of arterial PaCO2 through an indwelling catheter to calculate ventilatory response and calculate physiologic dead space during cardiopulmonary exercise testing (CPET) had been the established standard at the UPMC Presbyterian Pulmonary Diagnostic Laboratory. Because arterial line insertion is a time consuming, invasive, and relatively low-volume procedure for the lab, we implemented a noninvasive method for measuring CO2 utilizing a transcutaneous monitor (TCM) to assess transcutaneous CO2 (PtcCO2). We assessed the impact of TCM on study visit length compared to prior in-dwelling catheter study time with the aim of justifying approval through finance for permanent purchase and implementation of the TCM for CPETs in our laboratory.
Methods:
We utilized a loaned TCM monitor for 3 months to compare transcutaneous measurements to resting arterial blood PCO2 measurements. We evaluated complete data on 18 subjects. We estimated 3 torr to be a clinically meaningful error between measurements. Based on these data comparisons, a proposal for justification was submitted to both administration and finance for purchase of the TCM.
Results:
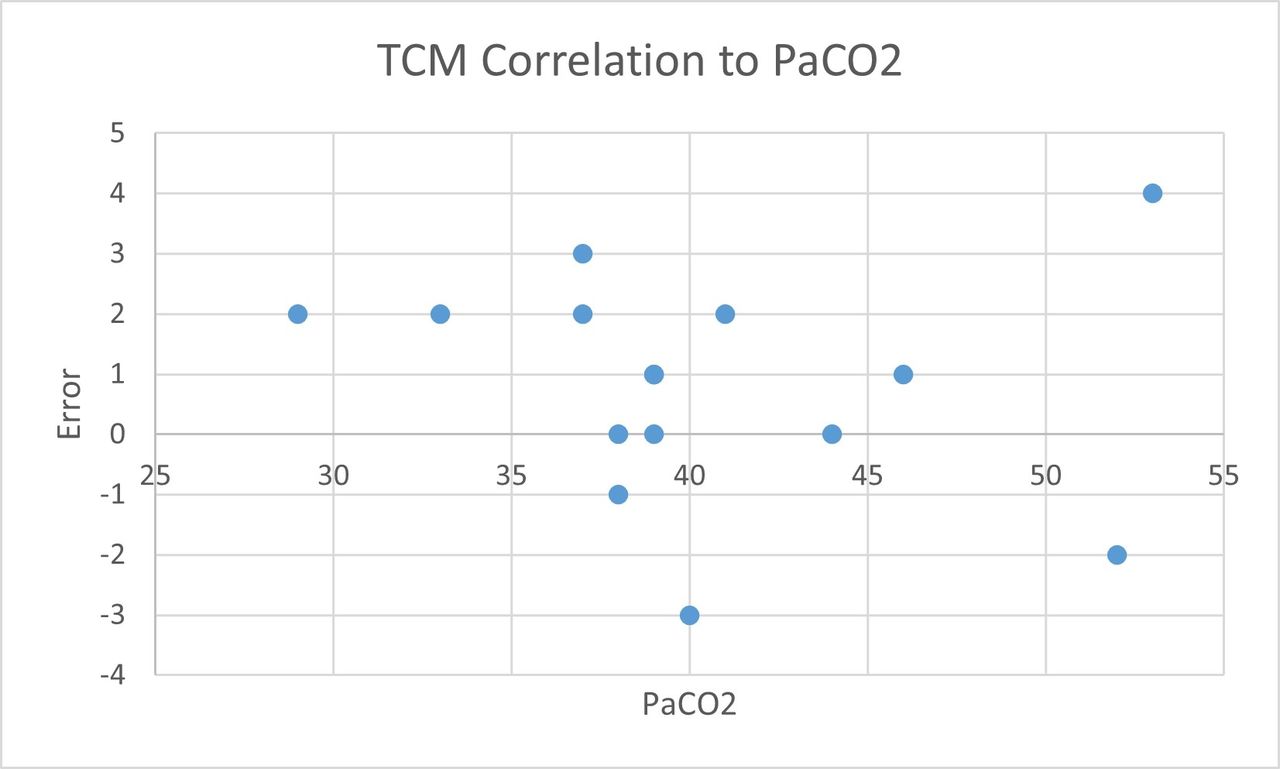
The difference between PtcCO2 and PaCO2 at rest was 0.3 torr ± 2.0 SD. Only 1 of 18 subjects had a difference of 4, exceeding the 3 Torr meaningful difference between the two approaches. After proposal for justification was accepted, the TCM was purchased. In-services were held to train staff on use of TCM. The PFT lab staff worked in conjunction with a representative from the metabolic cart company to integrate the analog signal into software. Use of TCM for PtcCO2 measurement was implemented into CPET policy and protocol. Additionally, the Pulmonary Diagnostic Laboratory was able to increase CPET capacity from 2 to 4 studies per week, allowing the potential for an extra 100 studies per year.
Conclusions:
The noninvasive TCM PtcCO2 accurately estimates resting arterial PCO2. Implementing TCM into our CPET protocol has increased CPET volume in the Pulmonary Diagnostic Lab, allowing patients to perform ordered testing without delaying care. The TCM maintained the accuracy of dead space calculation without the need for routine use of in-dwelling catheter. Confirmation of the dynamic accuracy of this measurement during incremental exercise is pending.
Get full access to this article
View all access options for this article.
