Abstract
Background:
Pediatric acute respiratory distress syndrome (PARDS) frequently causes respiratory failure and carries high mortality in the pediatric intensive care unit (PICU) - 40% when oxygen index (OI) >16. OI is the gold standard for early diagnosis and evidence-based management of PARDS. Our primary goal was to improve OI documentation by respiratory therapists (RTs) via Plan-Do-Study-Act (PDSA) quality improvement (QI) techniques for intubated/tracheostomy PICU patients with arterial blood gases (ABGs). We hypothesized RT-targeted educational training and electronic health record (EHR) based QI interventions would achieve >75% OI documentation compliance.
Methods:
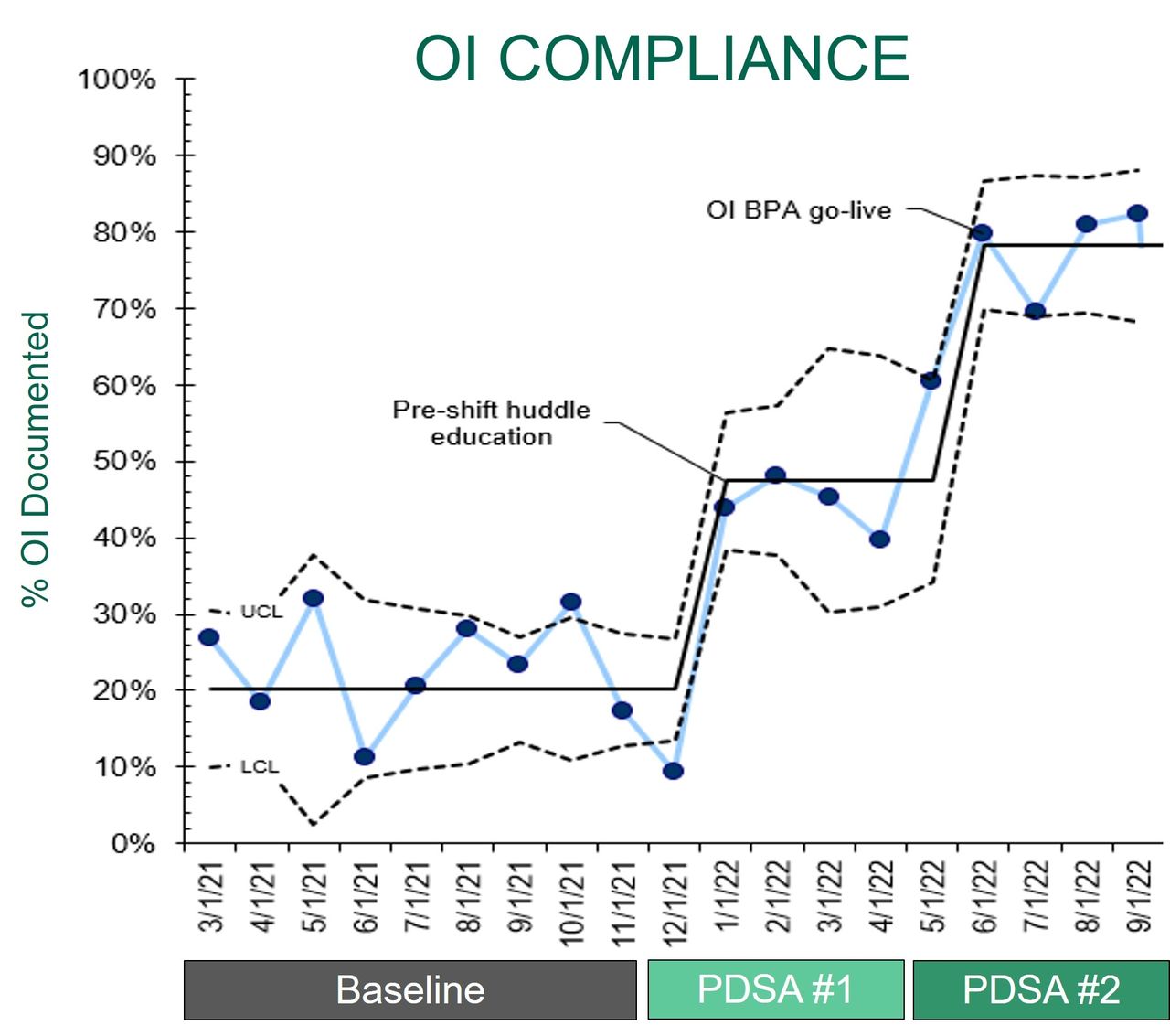
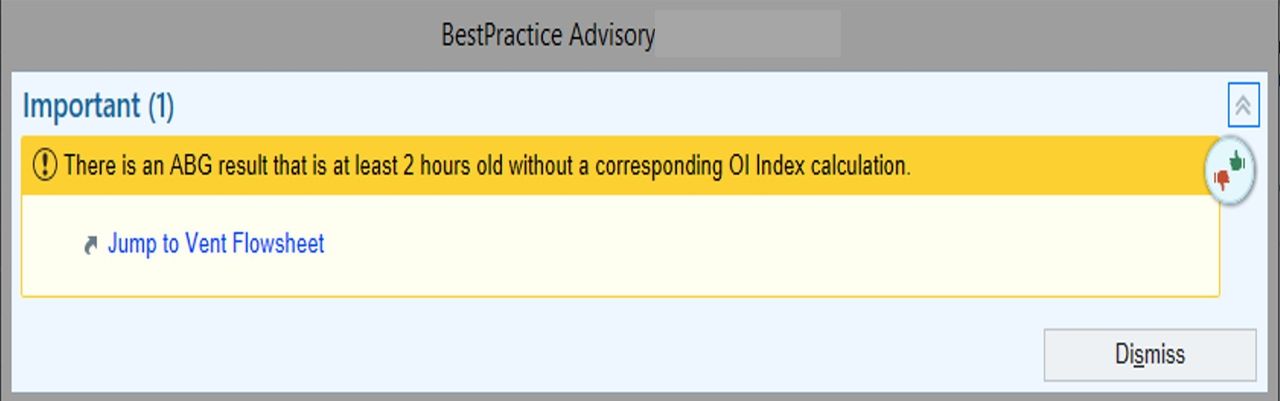
Inclusion criteria consisted of PICU admissions beginning March 2021 through September 2022. Patients must have an artificial airway and be mechanically ventilated with ABGs being monitored. We collected baseline and ongoing compliance data from Virtual Pediatric Systems and EHR. Techniques implemented included targeted education and the creation of OI Best Practice Advisory (BPA) in the EHR. PDSA 1 = implemented reminders at twice daily RT pre-shift huddles, emailed OI education to RTs, and training pamphlets on OI calculation. PDSA 2 = worked with EHR analyst to create BPA that is triggered by new ABG result and displays when RT opens patient’s chart. OI BPA acts as a reminder to document OI but allows for dismissal. Intervention effectiveness is tracked on a P Chart.
Results:
OI documentation compliance data: Baseline (March-November 2021): 23.2%, PDSA 1 (December 2021-April 2022): 39.2%, PDSA 2 (May-September 2022): 78.3%. At baseline, the RT department did not have a standard for OI documentation.
Conclusions:
A total of 297 patients over the course of March 2021 through September 2022 met the criteria for this OI project resulting in their EHR being reviewed and data collected. OI documentation by the RTs improved significantly following our interventions and we were able to achieve our target compliance rate. The EHR-based intervention (OI BPA) led to the largest and most sustained increase in documentation compliance. Limitations for this project included a lack of appropriate balancing measures, as well as increased new staff members – 14 RTs and 12 travel RTs. Once the level of new staff was recognized, proper education was given and became a new standard during the onboarding process.
Get full access to this article
View all access options for this article.
